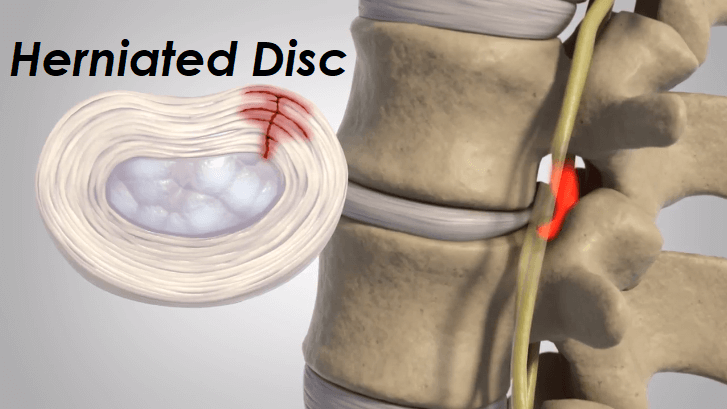
A brief description of a Herniated Disc

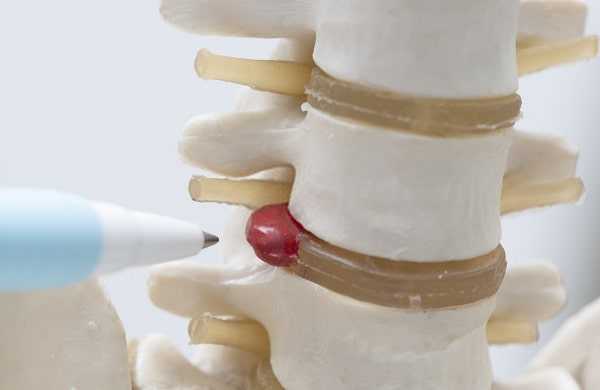
A herniated disc (also known as a “slipped,” or “ruptured,” disc) is a common cause of neck, lower back, arm, or leg pain. Although a herniated disc can result from a single traumatic event, it is more often the result of a gradual degeneration of the spine.
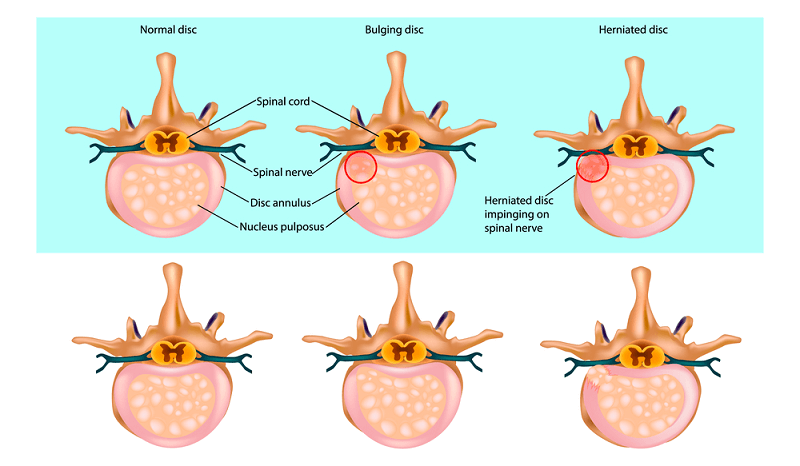
Causes
As you age, your discs lose water and become more stiff and brittle. Sometimes the discs can also gradually swell and bulge out of the spine without losing fluid, a condition that does not necessarily cause pain. But when the tough outer covering of the disc tears, whatever the cause, the center of the disc may extrude, or herniate. And when the disc substance pokes out far enough to irritate a spinal nerve, you will almost certainly feel pain in your legs as well as in your back. This is called a slipped disc, although the disc actually remains attached firmly between the vertebrae and does not move.
Symptoms
Symptoms felt in the back include:
• Sciatica —a sharp, often shooting pain extending from the buttock down the back of one leg
• Weakness in one leg
• Tingling (“pins-and-needles”) or numbness in one leg or buttock
• Loss of bladder or bowel control
• A burning pain centered in the back
Common symptoms felt in the neck include:
• Muscular pain between the neck and shoulder, possibly shooting down the arm
• Headache near the back of the head
• Arm weakness
• Arm tingling or numbness
• Loss of bladder or bowel control
• Burning pain in the shoulders, neck, or arm
Among the conditions that can weaken the disc are improper lifting techniques; obesity, which places extra stress on the discs; repetitive strenuous activities; smoking; trauma; and poor conditioning. In addition, you may have a genetic predisposition for herniated discs, which can make you more likely to experience a rupture.
The following symptoms require an urgent trip to your physician’s office or an emergency room:
- Severe or worsening weakness of your muscles. For instance, if you were able to lift up your foot or stand on your toes after your injury but now you can’t, injury to your nerve may be worsening and may require immediate surgery.
- Loss of bowel or bladder control. If you have lost the ability to control your urine, stool, or both (incontinence), there is too much pressure on the nerves that control your intestines or bladder, and surgery may be needed.
- Pain that is steadily worsening.
- Back pain with a fever.
- Pain that is worse at night or at rest.
Diagnosis
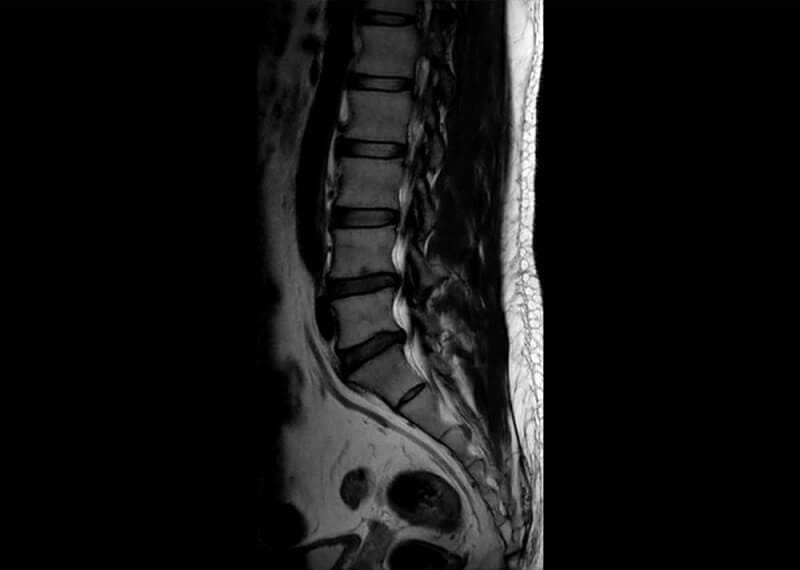
After obtaining a thorough medical history and carefully examining you, your doctor may order radiographic imaging of your spine. A traditional X-ray may pick up degenerative spine changes, but an MRI/CT scan or an EMG will be needed to determine whether there is any nerve damage.
Nonsurgical Treatments
Although pain from a herniated disc may feel like an emergency, most herniated discs do not result in permanent damage to your spine. Moreover, conservative therapy will relieve herniated disc symptoms in more than 90 percent of patients. This typically involves a regimen of bed rest and over-the-counter pain relievers; muscle relaxants, as well as analgesic and anti-inflammatory medications; cold compresses; and heat.
If conservative treatment fails, epidural injections of a cortisonelike drug may lessen nerve irritation and can be given on an outpatient basis.
Physical activity such as bending forward and lifting should be minimized; sitting for long periods should be avoided. The lower back exercises detailed earlier in the chapter may help strengthen your back and stomach muscles.
Surgical Treatments
Surgery is aimed at stopping the herniated disc from pressuring and irritating the spinal nerves; it should also relieve pain. But such remedies should be considered only if nonsurgical therapy does not lessen your symptoms after a period of at least six to twelve weeks, given the inherent risks of these invasive, open-surgery techniques:
• Laminotomy: In this procedure, only a portion of the lamina is removed to relieve pressure on a nerve or to allow the surgeon access to the disc that is pressing on a nerve.
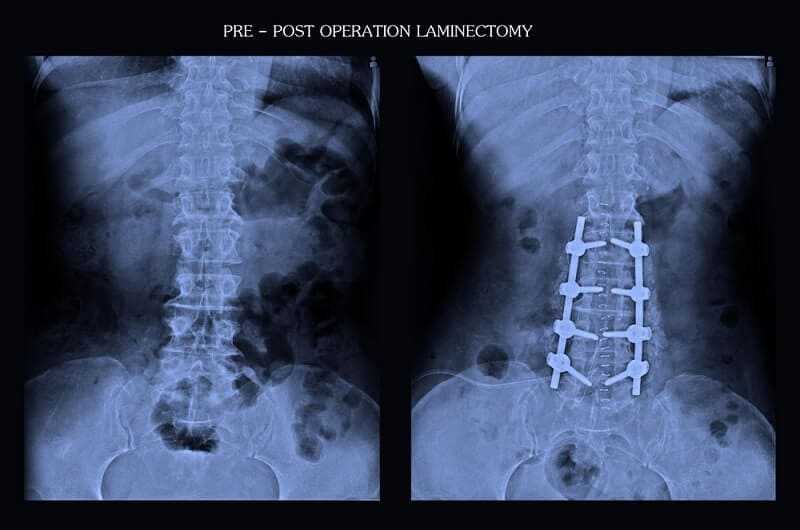
• Laminectomy: The entire lamina is removed in a laminectomy, with your surgeon determining how much bone to remove by reviewing the MRI or CT scan.
Check out here for more information.
• Discectomy– This technique involves removing part of a disc to relieve pressure on a nerve. In the case of a herniated disc, either a laminotomy or a laminectomy is usually performed along with a discectomy.
• Micro discectomy: Some surgeons are performing micro discectomies, which involve smaller incisions and the use of a microscope. The success rate for these operations is similar to standard discectomy (80 to 90 percent), and the recovery time is somewhat shorter. Not all cases are suitable for this approach, however.
Alternative Therapies
Like sufferers of lower back pain, those patients who are searching for relief from pain resulting from a herniated disc often seek alternative treatments such as acupuncture, chiropractic care, interventional therapy, traction, TENS, and ultrasound. Be sure to consult with your doctor before beginning an alternative course of treatment.
Possible Future Treatments
Open discectomy and micro discectomy are the gold standards for surgically treating a herniated disc. But researchers are working on less invasive treatments, including:
• Nucleoplasty: With heat-producing (bipolar radiofrequency) technology, an energy field is created that lessens the pressure within the disc, providing pain relief.
• Oxygen-ozone therapy: This therapy involves injecting a combination of oxygen and ozone gases into a herniated disc to reduce the disc’s volume and limit pain. This treatment can enhance the effects of simultaneously administered steroid injections.
• Disc and nucleus replacement: Metal and plastic prostheses are being used experimentally as replacements for discs and nuclei.
• Biological repair: Although biological repair techniques are not yet considered safe enough for human use, there have been attempts to repair or regenerate a disc by injecting proteins that promote regeneration (for example, growth factor).
Related Article
Herniated Disc – Artificial Disc Replacement Surgery
Note that because these procedures are still new (or in development), there are few long-term studies documenting their efficacy or safety. But it still may be worth asking your doctor whether any of these may be useful for your situation — either now or down the road.
Exercises for Prevention and Healing
Core strengthening builds the muscles that support your entire body. Pilates, yoga, and martial arts all provide well-rounded core strengthening programs. Other core strengthening exercises include:
• Transverse core strengthening exrcise: This exercise strengthens the muscles that extend from your ribs across your waist and help support you in an upright position. Stand with your feet shoulder-width apart and toes turned in slightly while holding a ball directly in front of you. While keeping your abdominal muscles tight and your feet flat on the floor, turn your body from side to side. Repeat five to ten times; you may use progressively heavier balls.
• Sagittal core strengthening: This exercise stretches and strengthens the low back muscles that help you stand and lift. With your feet shoulder-width apart and your arms by your side, stand about a foot from a wall, facing away from it. Tighten your abdominal muscles and, while keeping your hips and knees bent, lean back until your buttocks touch the wall. Using your hips, push your body back to an upright position, then extend your arms, reaching over your head. Repeat five to ten times.
• Abdominal crunch: Inhale and draw in your stomach while lying on your back; exhale as you lift your chest off of the floor. Repeat ten to fifteen times.
Resistance training is exercise done against something that provides resistance, such as a weight (handheld weights or training machines) or isometric techniques (muscle-against-muscle resistance). The following exercises use resistance to strengthen the neck and back areas:
• Neck press: Press your palm against your forehead and use your neck muscles to push against your palm; hold for ten seconds and repeat ten times. Next, press your palm against one of your temples and use your neck muscles to push against your palm, holding for ten seconds and repeating ten times on each side. Finally, cup both hands behind your head and use your neck muscles to press backward.
• Side bridge: While lying on your side, with knees bent at 90 degrees, prop your head up on your elbow, elongate your neck away from your shoulders, and draw in your stomach. Lift your hips away from the floor, keeping your head, shoulders, and hips in a straight line; hold this position for as long as thirty seconds (less if you feel too uncomfortable). Repeat five to ten times.
• Prone bridge: Facing the floor, prop yourself up on your elbows and toes, keeping your shoulders, hips, and knees in a straight line. Hold this position for as long as thirty seconds. Repeat five to ten times.