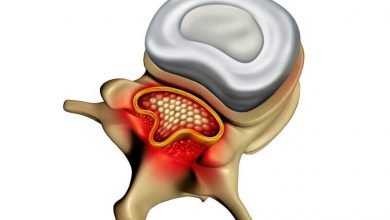
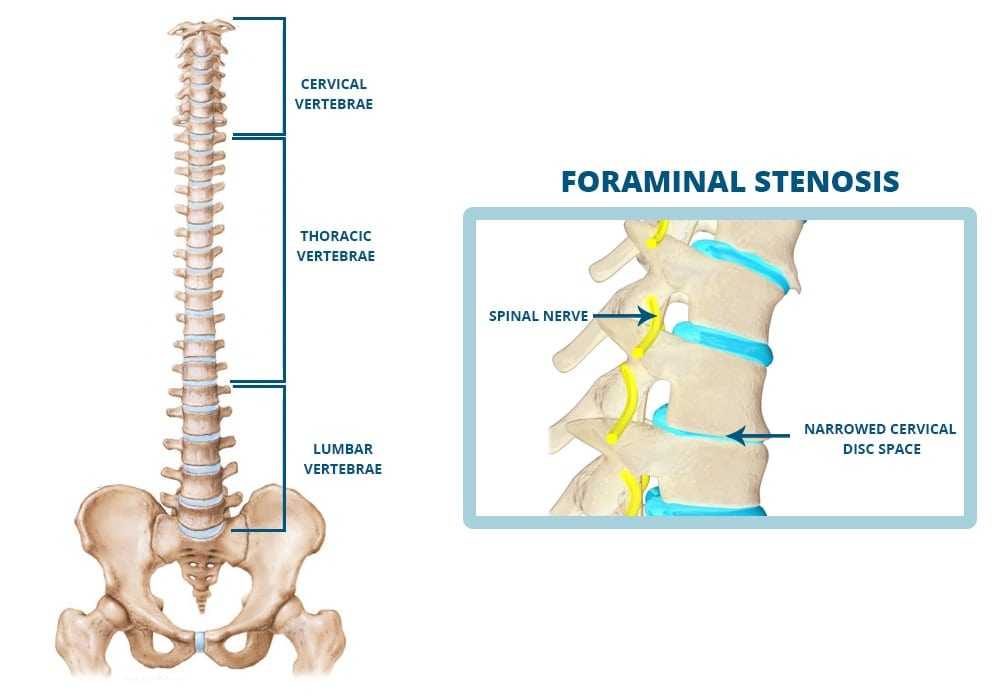
About Spinal Stenosis
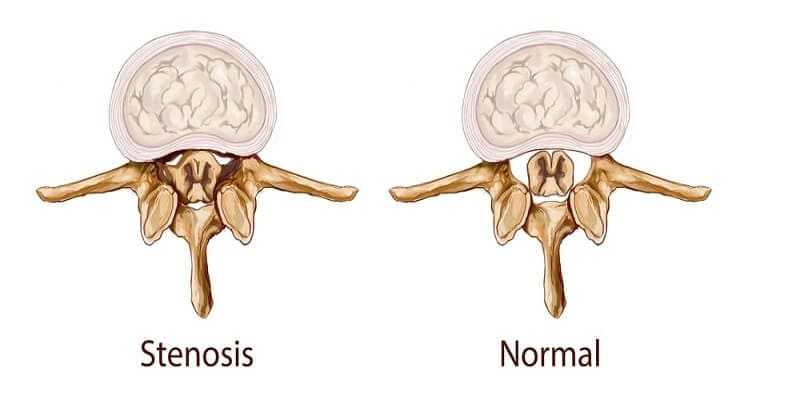
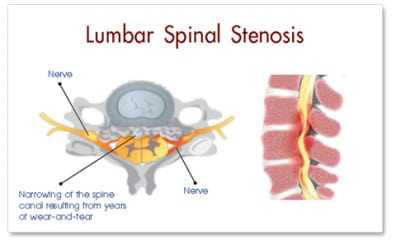
Lumbar spinal stenosis (or narrowing of the spinal canal) is a clinical syndrome because of pain in the lower back, buttock or leg. The term “stenosis” means a narrow constriction within a tubular structure.
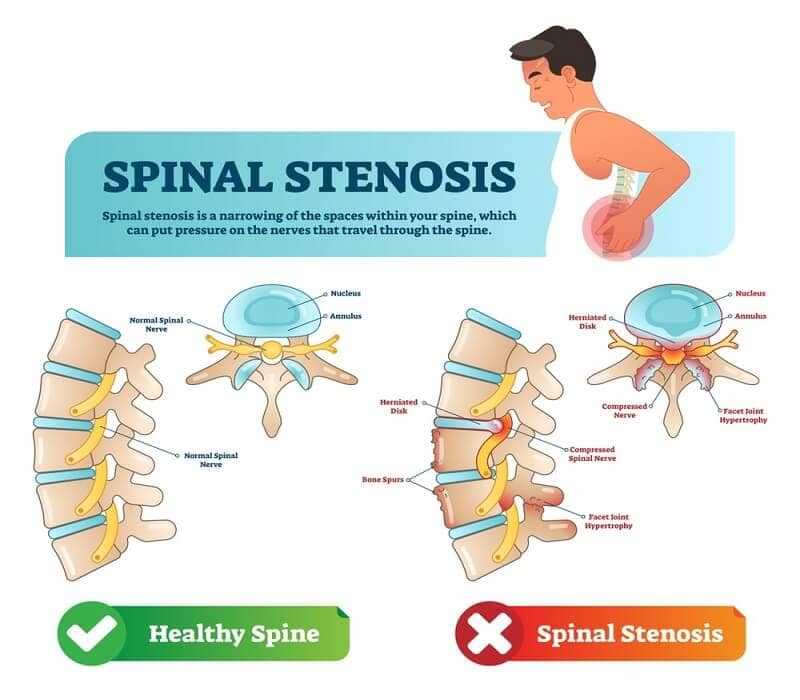
Sachs and Fraenkel (Fraenkel B and Sachs J, 1900) were among the first to link the symptoms of sciatic nerve compression in the Spinal Stenosis channel. Subsequently, descriptions of the condition report are: compression bone acquired called “degenerative” and/or constitutional narrowness or “defect” of the spinal canal.
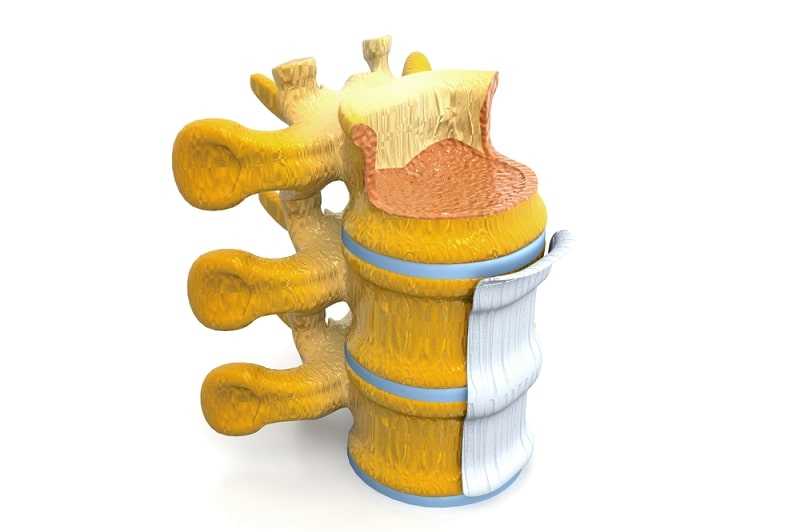
Van Gelderen (C. Van Gelderen, 1948) suggests that the hypertrophy of ligamentum flavum is a possible cause of spinal stenosis by publishing two cases of patients suffering from this condition. The clinical syndrome of spinal stenosis and their relationship to congenital narrowness are described in detail by the surgeon Holland Verbiest, which is also clearly demonstrated by the mechanical compression of neural elements in myelography (HA Verbiest, 1954).
Kirkaldy-Willis et al. clarify the pathologic anatomy of the spinal canal stenosis and contribute to the good correlation between anatomical lesions and pathological symptoms (Kirkaldy-Willis W, Paine K, Cauchoix J, et al., 1974).
Classification
The etiology of spinal stenosis is most commonly (Arnoldi C, Brodsky A, Cauchoix J, et al., 1976) or congenital, developmental, acquired, degenerative or a combination of all.
Most cases of spinal stenosis are acquired, because the degenerative changes of the complex consists of three joints of the intervertebral disc and two facet joints.
In some cases, these degenerative changes may be superimposed on stenosis. Variations in form, as in the dimensions of the vertebral canal, may predispose to stenosis of the spinal canal with canal clover more readily associated with lateral recess stenosis, more common in the case of round or oval canal.
Clinical examination
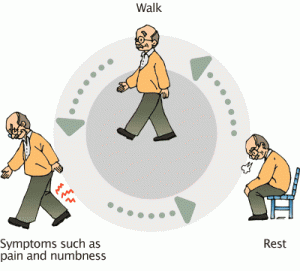
Patients may not suffer from lumbar spinal stenosis, while others may experience very severe pain. If the symptoms most frequently encountered are low back pain and intermittent claudication of the cauda equina, bilateral sciatica is accompanied by paresthesia of the lower limbs occurring after a certain distance of running.
Here is a summary list of features suggestive history in a case of lumbar spinal stenosis:
Demographics
*Adult middle-aged or older, except “congenital” …
*Ratio Male> Male (3 / 1 to 5 / 1)
*Leg Pain> bad lower back
*Gene in the limb
*Projection or root
*Pseudoclaudication (called neurogenic claudication)
*Caused by standing or walking
*Relieved by sitting position above station leaning forward (sign of the cart)
Differential Diagnosis
*Peripheral neuropathy (non-physical activity in type dysesthesias burns)
*Vascular claudication
*Affection of the hip (Hip-column syndrome)
Physical examination
Imaging
Radiology standard
Scanner and lumbar
MRI lumbar spine
Reviews can be stressful, expensive (and very irradiating for some) and should be achieved if the surgeon asks for a surgical indication (not before).
Cause
With the upright posture of humans, the lower lumbar spine is mechanically loaded high. Degenerative changes are age-and wide-spread on load and light forms. It is not so much the question of whether they develop, but more the question of how quickly the narrowing progresses, and whether it causes clinical symptoms.
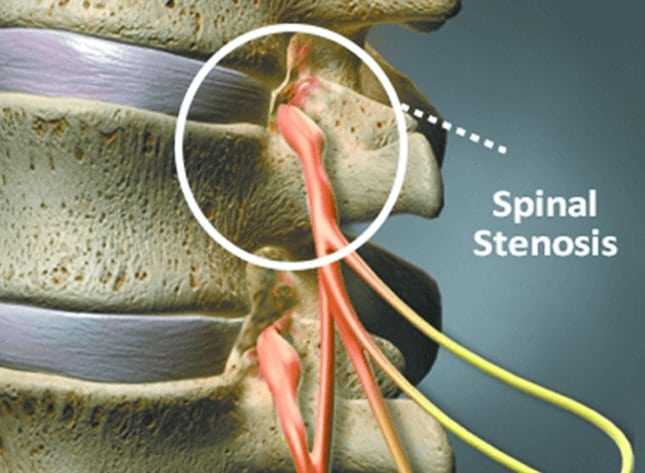
As part of the normal aging process, inter-vertebral discs lose height. Next is the creation of osteoarthritis of the facet joints arc (spondylarthritis). This combination creates an hourglass-shaped narrowing of the spinal canal. The stenosis may have different shapes. Occasionally, a relatively intact spinal disc space shifts and “slips” to the side.
Clinical features and diagnosis
The clinical findings are uncharacteristic. Dysfunction and pain or irritation of the sciatic nerve can be caused by very different pathological changes of the lumbar spine. Typical of the spinal stenosis is the symptom of spinal claudication. The patient complains of pain at the front or back of the legs.
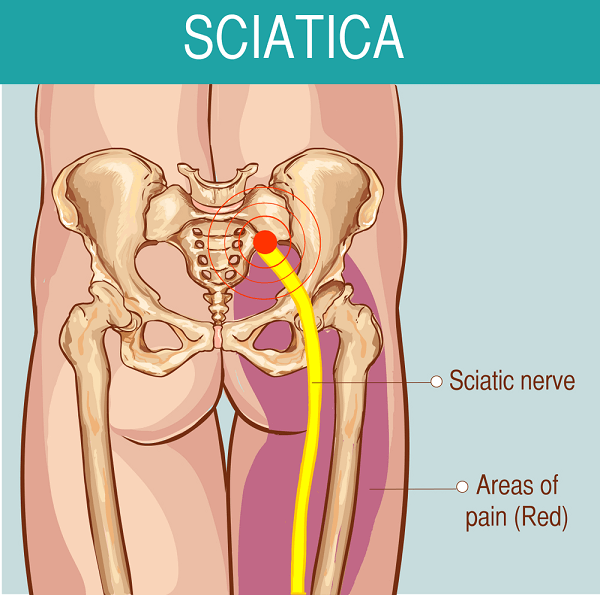
The pain is better when they sit down. The spinal canal through the bend reduces the irritation of the nerve structures. If the patient in extreme cases can only go no more than 100m, further diagnosis and treatment is necessary.
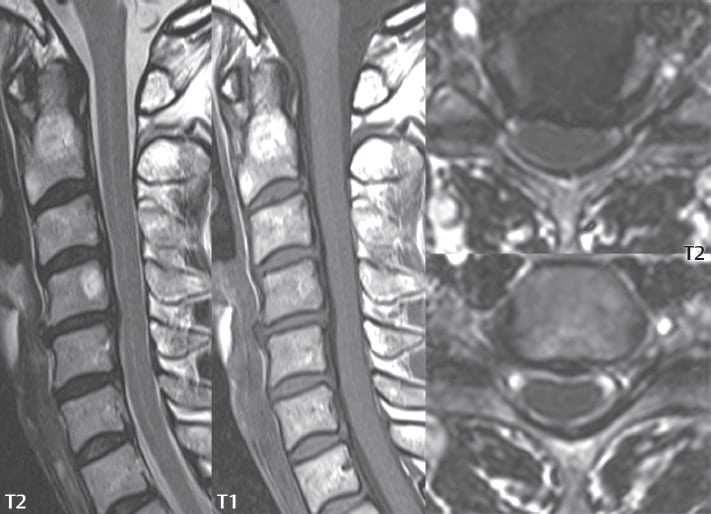
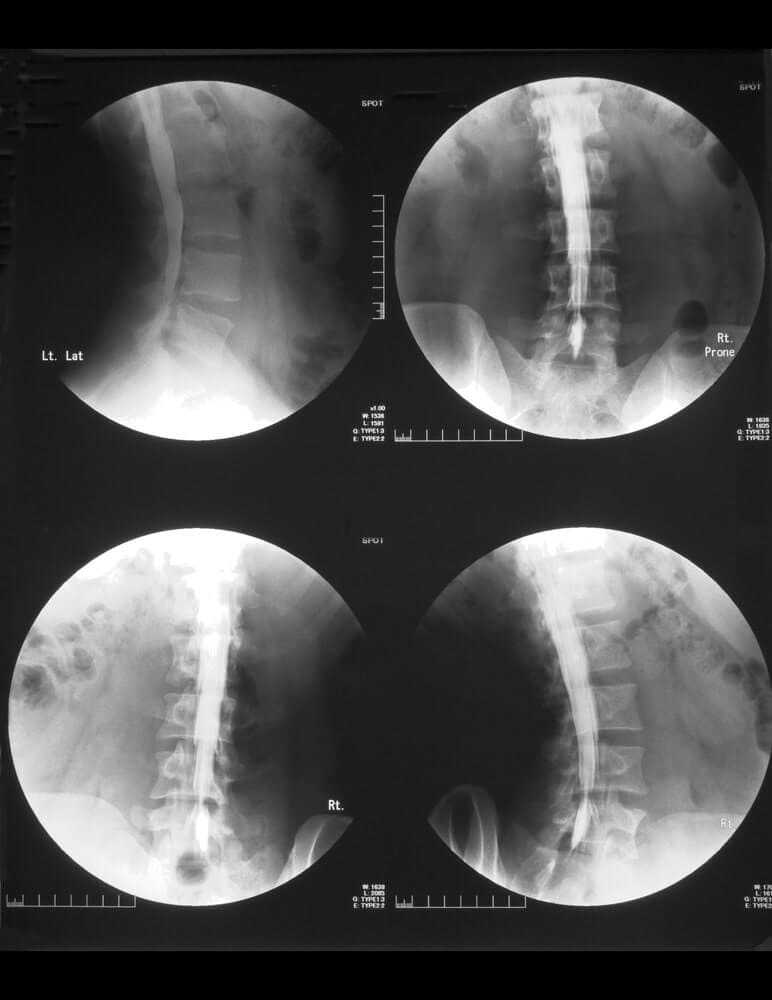
The normal X-ray diagnostics is already a first indication that may be proven by MRI examination. The stenosis is progressive and often progresses at different rates. After several years there is usually no more deterioration. Neurological deficits are rare.
Therapy
In many cases, the reason for such changes are in the mechanical instability. The muscles of the spine can be stabilized by appropriate exercises, thus increasing instability and its consequences.
The main emphasis of treatment is on physical activities, relaxation exercises, and electrotherapy and not on the use of analgesics. Immediate relief, especially in elderly patients is possible through exculpatory or stabilizing hull bandages/cloth corset. This disc can be relieved.
As part of surgical decompression of the spinal canal, it can be extended again, in mild cases, and even the placement of a stent between the spinous processes is possible (interspinous spacer).
Alternatively, reinforcement can be made using the respective discs which are removed and two small plates (Cage) are replaced, which act as placeholders. In addition, the affected segment is stiffened with screws and rods. In 4-6 months a sufficient ossification of the two vortices (bone bridges) can produce up to 95% of their normal capacity.
The two vertebrae are then bonded together, resulting in a few vertebrae having functional limitation. Tobacco use can delay this process, so at least several months of abstinence may be prescribed. Postoperatively, a physiotherapy treatment is appropriate, which is often used to settle by itself later and carried out with exercises.
Economic importance
The economic significance of the various diseases of the spine is very high. For most the spine is more or less directly the cause for retirement and it constitutes at the most job losses. Not least because of the economic importance of spinal stenosis and other back problems to this issue, a whole industry has arisen.
A variety of so-called rehabilitation hospitals, physical therapists and orthopaedic surgeons provide services which are partly financed by the cash registers. In addition, there is a large private market of “treatment” often with insufficient or no proven medical benefit.