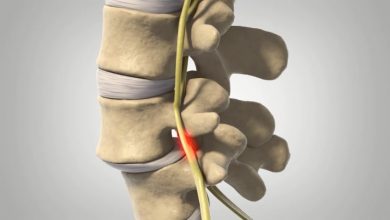
Back Surgery for Spondylolisthesis
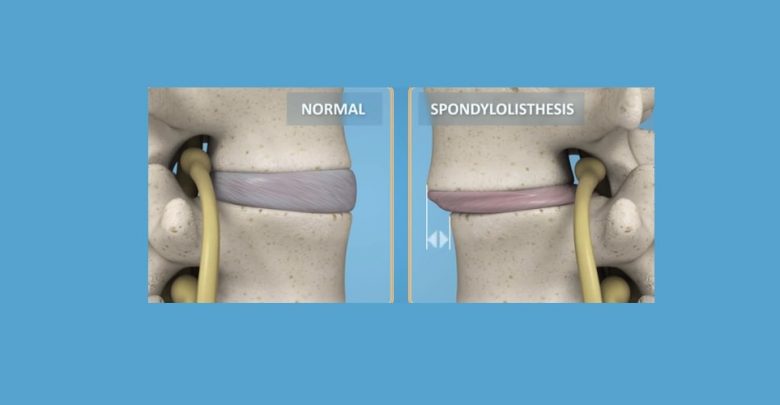
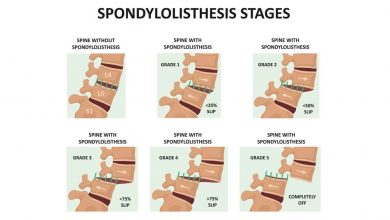
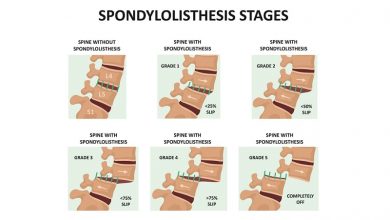
Spondylolisthesis is a condition where vertebrae ‘slip’ out of position in the spine, causing the normal structure of the spinal column to become dysfunctional and often leading to spinal stenosis when degenerative spondylolisthesis remains unaddressed (Kalichman, 2008). This displacement can occur when there is significant acute damage to the area, from a contact sports injury say, or as a result of more chronic issues such as cervical degenerative disc disease, osteoarthritis, and other cervical spinal issues.
The most common cause of spondylolisthesis is wear and tear on the spine leading to degeneration of the tissues of the spinal column. Chronic degenerative changes in the ligaments, facet joints, bones, and cartilage that hold the spinal/vertebral column in position affect the stability of the vertebral column and the vertebrae can slip out of position. Another category of spondylolisthesis is called isthmic spondylolisthesis and is the result of spondylolysis; a defect in the pars interarticularis. This pars defect in part of the vertebrae is most commonly caused by repetitive microtrauma in childhood through activities such as gymnastics, diving, soccer, football, and wrestling (Standaert, 2000).
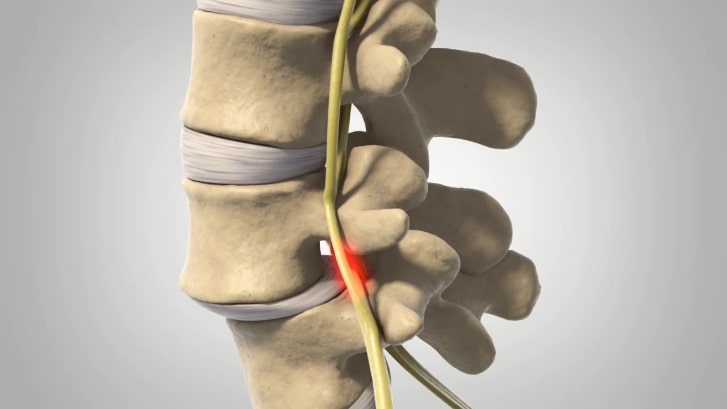
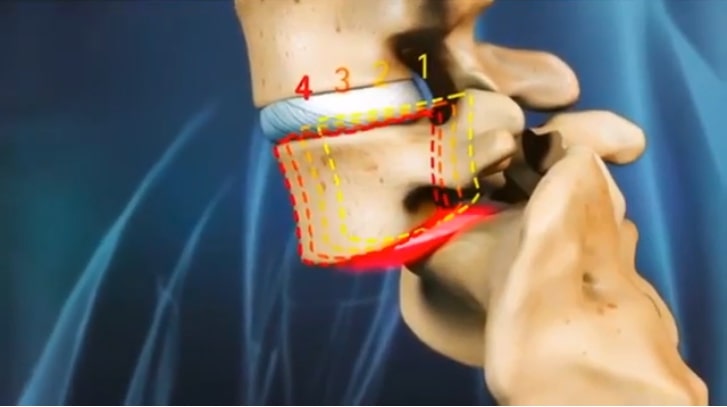
Who is Affected by Spondylolisthesis?
It is rare for children under five to be diagnosed with the condition, unless there is a congenital abnormality that predisposes them to spondylolisthesis. Children are more likely to start developing spondylolisthesis between the ages of seven and ten as increased physical activity and the rapid growth of adolescence begins. Wear and tear may not cause symptoms however, until later in the teenage years or into adulthood with around 5-6% of men and 2-3% of women thought to have spondylolisthesis. Those engaging in very physical activities, either professionally or recreationally, are more likely to suffer from the condition, with gymnasts, weightlifters, and football players at increased risk.
Traumatic spondylolisthesis can also occur if the vertebrae are subject to direct trauma resulting in fracture of the pedicles, or facet joints, or dysfunction of the lamina at the back of the spine. Congenital abnormalities of the facet joints can lead to spondylolisthesis, as the vertebrae are allowed to slip out of place. The condition is referred to as dysplastic spondylolisthesis. A further classification is pathological spondylolisthesis, where a defect of the bone, or a tumour causes the slip to occur.
Spondylolisthesis Treatments
Ascertaining the cause of the spondylolisthesis is key to providing appropriate treatment. Where isthmic spondylolisthesis is suspected, the patient will usually be advised to avoid the cause of the microtrauma, and to make use of alternatives to back surgery such as analgesics, anti-inflammatories, and physical therapy in the first instance. Where significant acute damage has occurred, or where conservative treatment has failed to provide relief, back surgery for spondylolisthesis may be recommended, although there is considerable debate over the merits of surgery for spondylolisthesis that has occurred gradually or is congenital. Spondylolysis normally does not require surgical intervention, unless it progresses into spondylolisthesis. Dysplastic and pathological spondylolisthesis are more likely to require back surgery to remove the defective tissue or correct the abnormal spinal structure and reduce stenosis symptoms. The use of a brace or corset may be helpful in reducing neck or back pain in the meantime. Correct posture, and core muscle strengthening, along with neck and back strengthening exercises are important parts of the treatment plan for spondylolisthesis.