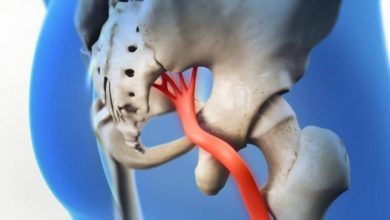
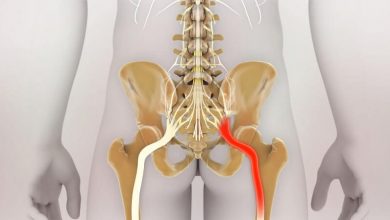
Brief and easy to understand information on Sciatica
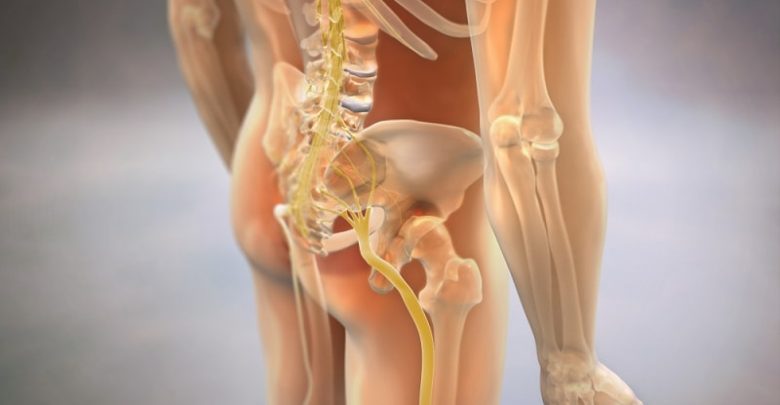
Pressure on a nerve, leading to backache and pain in the leg.
Causes
Sciatica in younger people probably follows partial slippage of a vertebral disc. The intervertebral discs are made up of a jelly-like core within a fibrous ring; a tear in this ring allows the contents to leak out and impinge upon the nerve roots. These coalesce to form the sciatic nerve, which runs down the back of the thigh into the calf and the foot.
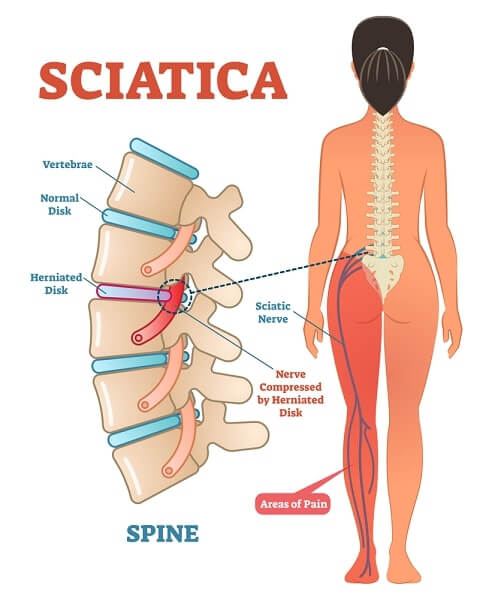
In older people the cause appears to be osteoarthritic outgrowths of bone that similarly irritate the nerves (see Osteoarthritis). The sciatic nerve is particularly affected because the vertebrae at the base of the spine – the lumbo-sacral region – are curved to a degree that increases the chances of a disc slipping. Sometimes there is a clear episode that precipitates sciatica; more often a minor exertion seems to bring it on or it appears out of the blue.
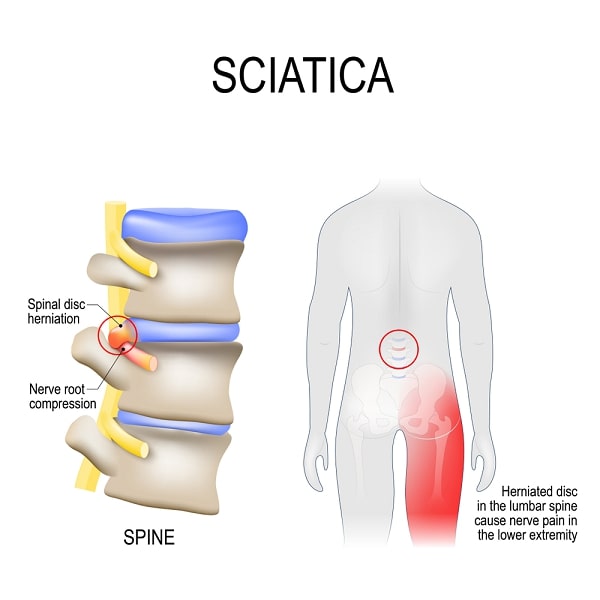
Symptoms
The onset is usually acute with sudden severe low back pain, worse on coughing or straining and flexing the back. The pain radiates down the back of the thigh and calf and ends in the sole of the foot. This is classic sciatica but there are variations depending on exactly which nerves are being affected. For example, pain may radiate more over the side and back of the foot. Along with the pain there may be muscular weakness in a pattern that again reflects which nerves are irritated, for example weakness in pressing the foot down or extending the knee. The ritual of tapping out knee and ankle reflexes further determines which nerves are affected.

Your doctor will check your straight leg raising, which means lifting your leg to see how high it can go without severe pain. Anything less than about 45° suggests significant pressure on the sciatic nerve.
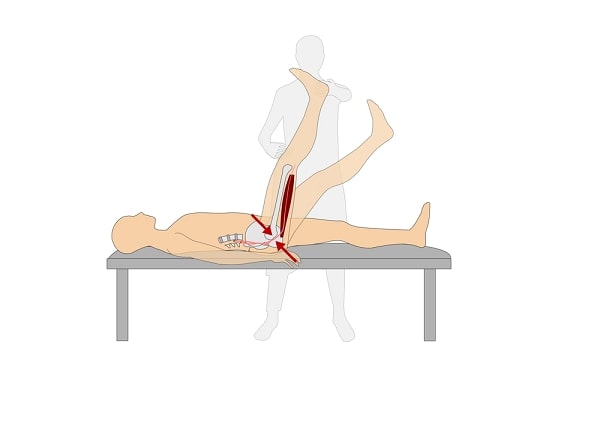
Investigations are of little benefit at this stage unless examination suggests a serious disc slippage that might need surgery, or any other worrying symptoms of backache.
Treatment
Treatment overlaps with that of backache. Rest for a few days, then attempt as much movement as you can. Use painkillers, and muscle relaxants if muscle spasms are a problem. Doctors are reluctant to prescribe the most powerful and possibly addictive painkillers for what they know may be a chronic condition. Physiotherapy helps to mobilize the spine aid it is also good for boosting confidence.
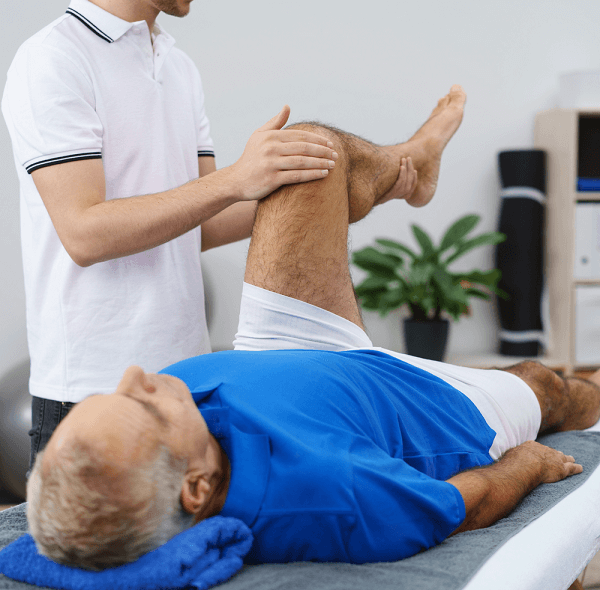
On this basis most episodes of sciatica will settle, many within a few weeks, but be prepared for full recovery to take three to twelve months. Persistent pain might be helped by a steroid injection into the spinal canal; this requires a general anaesthetic and the effects are often temporary.
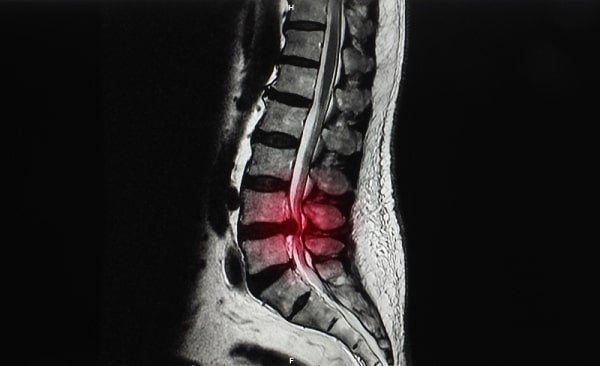
In less than one in a hundred cases, symptoms point to a persistently slipped disc: constant pressure on nerves, paralysis of foot movements, interference with urinary control and unremitting pain. Here investigations with an mri scan may confirm a seriously slipped disc and surgery might be appropriate. This aims to remove the slipped disc by surgically exposing the vertebrae or, as is increasingly done, by guided microdiscectomy, where fine instruments are guided to the disc through a small cut in the back.
Why do doctors ask about bladder control?
What investigations are available?
Why is surgery done so infrequently?
Complementary Treatment
Acupuncture is a very powerful treatment. Alexander Technique is also useful – see this. Chiropractic manipulation is an effective and speedy treatment. Yoga can be helpful, but must be undertaken only under the guidance of a suitably qualified teacher. Osteopathy can help if the cause is a prolapsed intervertebral disc or other spinal condition. Hellerwork see this. Rolfing corrects imbalances which can compress the sciatic nerve. Other therapies to try: chakra balancing; shiatsu-do; naturopathy; cymatics; auricular therapy; Ayurveda.