Chronic Pelvic Pain Syndrome In Men
A Real Case…
Bill was standing in the exam room when I came in. “I am sorry Doc but I need to go to the bathroom. Do you want a urine sample because, Doc, it hurts to pee. I have been like this for over a year.”
I handed Bill a urine cup to check for infection. A dipstick analysis showed no signs of any abnormality in the urine. Bill’s problem was likely chronic.
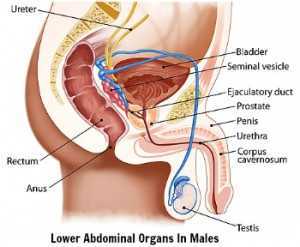
Chronic Pelvic Pain Syndrome (CPPS) in men is defined as pelvic pain for 3 months or more that is not due to a urinary tract infection. The old term for this was “prostatodynia” or painful prostate.
In the U.S.A., CPPS is the most common reason for men 50 years old and over to see a urologist.
As it turned out, Bill had previously had an extensive work-up by an excellent local urologist and was told that “his prostate was fine.” He had been given some medicine by the urologist but couldn’t remember the name of it.
Processing A Case Of Chronic Pelvic Pain Syndrome…
Bill told me that when he sits down it hurts behind his testicles (that’s why he was standing when I entered the exam room). He said it felt like he had to urinate all the time. However, when he goes there is just a small amount of urine.
There was no real burning when he urinated…he just has the pain behind his testicles “all the time.” “My last Doctor told me it was all in my head,” Bill complained. His primary care physician had referred him to a psychiatrist.
Bill has the usual non-specific symptoms of CPPS. He did notice the pain seems to get worse if he ejaculates. He is a truck driver by occupation.
There are several key considerations when working up a man with Chronic Pelvic Pain Syndrome:
1) A thorough work-up by a urologist is essential. If this has already been done, have a copy of the results of all the tests e-mailed to your Doctor’s office. You may be surprised when you find out that certain key studies had never been done.
2) There are no definitive historical facts, physical findings, or diagnostic studies to diagnose Chronic Pelvic Pain Syndrome in men. The diagnosis of Chronic Pelvic Pain Syndrome is essentially to rule out other causes for the symptoms a person is complaining about. Since the most common cause would usually be a prostate abnormality, diseases of the prostate remain a consideration in nearly all cases of Chronic Pelvic Pain Syndrome.
3) Recent research has suggested that even negative cultures of the prostatic fluid, prostate biopsy tissue, and urine does not exclude the possibility of a prostate infection. Some forms of bacteria require specialized testing to detect them.
4) There is recent evidence that in CPPS the prostate can become injured by a previous infection and give way to symptoms that masquerade as an infection.
5) The absence of “objective” findings on physical exam or diagnostic testing does not necessarily infer a psychiatric reason for the symptoms.
Chronic pelvic pain syndrome physical therapy

Remember…a thorough History and Physical, as well as a consultation with a urologist is essential in the evaluation of CPPS in men.
The mainstay of therapy in CPPS is a class of medications called Alpha-Adrenergic Blockers. They work by relaxing the smooth muscle in vital areas in the male genito-urinary tract (one of the mechanisms for chronic pelvic pain in men). The names are Hytrin, Cardura, and Flomax. Each has benefits and limitations.
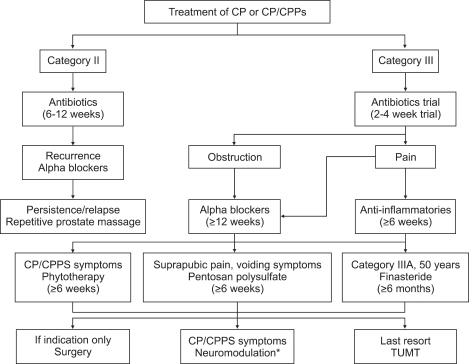
In CPPS a trial of antibiotics is often attempted (the duration of which may be more than a month). Theoretically, CPPS is a non-infectious disorder. However, given the limitations to perform specialized bacterial testing (cost, availability, etc), a 1 month trial of antibiotics is usually attempted.
Other less effective treatments are thoroughly reviewed by several on-line medical resource sites (ie. WebMD or Medscape). You can click on the highlighed links for more information. The table below lists some practical advice for primary care practitioners .
The Outcome Of The Case…
Bill was started on an alpha-adrenergic blocker with relief of his symptoms within 24 hours. His pain and urinary urgency improved and he had minimal side effects from the medications. On his last office visit with me Bill stated, “Doc, you’re a life saver. I didn’t tell you before, I guess I was embarassed, but I was having trouble being intimate with my girlfriend. This new medicine has changed everything.” A relatively simple answer to a problem that had plagued Bill for over a year.
If you have any further questions please comment. I would love to be of service to you.
Wishing you joy and healing,