Cognitive Behavioral Therapy

Chronic pain has been at epidemic levels for years in the United States. One can only imagine what the political response would be if HIV Infection, or Breast Cancer, or Ebola had shredded this many American lives. The response by nearly all agencies responsible for the health and welfare of American citizens has been woefully inadequate.
Opiate pain therapy is under assault by law enforcement, the medical profession has no structured plan to address this epidemic, and government is paralyzed by a lack of will to address the issue as a national catastrophe. Practitioners are usually left to address the issue themselves at great risk to their careers.

The search for creative ways to treat chronic pain is ongoing. Any practitioner hoping to treat chronic pain will have to negotiate a quagmire of regulation, political stagnation, and general misinformation about pain. Is there any hope?

The answer to that question is a resounding yes. As the field of Neuroscience begins to unravel the intricacies of central nervous pain modulation, the hope for definitive therapies modulating pain at the central nervous system level begin to appear.
Cognitive Behavioral Therapy (CBT) is a form of psychotherapy that has been shown to be effective in reducing many forms of pain (as well as several psychiatric disorders). Originally created by Drs. Beck and Ellis, the premise is that maladaptive conditions contribute to emotional distress and the maintenance of behavioral problems.

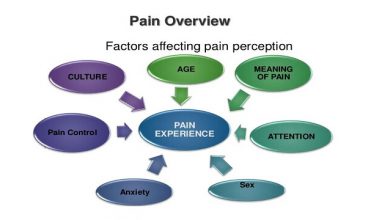
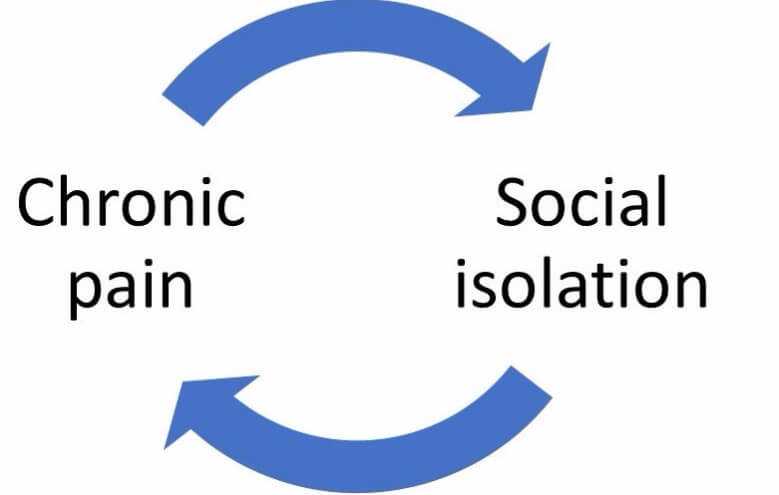
In that anxiety, depression, and insomnia significantly amplify the perception of chronic pain, CBT is a logical adjunct to any chronic pain regimen. This post will review the anatomy, physiology, and general mediation of pain by the brain as we discuss the positive effects of Cognitive Behavioral Therapy for chronic pain.
How Is Pain Mediated In The Brain?
Although the brain has certain modularity (for instance, vision is processed by the occipital lobe of the cortex-located in the back of the brain), the brain is really a vast, interconnected network. There is an emotional response to every conscious function of the brain. The limbic system (located in the center of the brain) acts as a neural intermediary for our brain network and reliably connects an emotional experience to every conscious event (and some unconscious…such as sleep).
Even certain unconscious functions can activate the Limbic system as the neural signaling traverses the brain from one region to the other. The notion that the human brain is only used 10% of the time is a drastic misrepresentation of the truth. Indeed, the brain is never inactive and is networked at all times.
Both internal (as simple as thoughts) and external stimuli (anything that provokes the senses) cause the brain to respond. Repeated stimulation of pain pathways cause them to change in structure and function (yes, chronic pain actually changes the anatomy of the brain). Repeated stimulation causes “wind up” which intensifies pain transmission.
With this increase in function, the same pain stimulus causes more pain over time. Pain patients often report worsening of their pain despite there not being any worsening of their disease that is demonstrable with diagnostic studies (such as an MRI). These patients are often accused of simply wanting more pain medication or of being addicts.
The automatic neural signaling of the brain is significantly affected by the frontal cortex of the brain (the area for thought – a particularly unique quality of being human). The frontal cortex exerts its influence over many automatic functions of the brain. Because of this, the thoughts and imagination of a person can affect the function of the brain and change it.
The entire process we are talking about is called “neuroplasticity.” The stimuli applied to a human being actually change the structure and the function of the brain. Consider identical twins…a misnomer really. You see identical twins do not have identical neural networks because their different life experiences modify their neural signaling. There are never 2 identical people for that reason…ever.
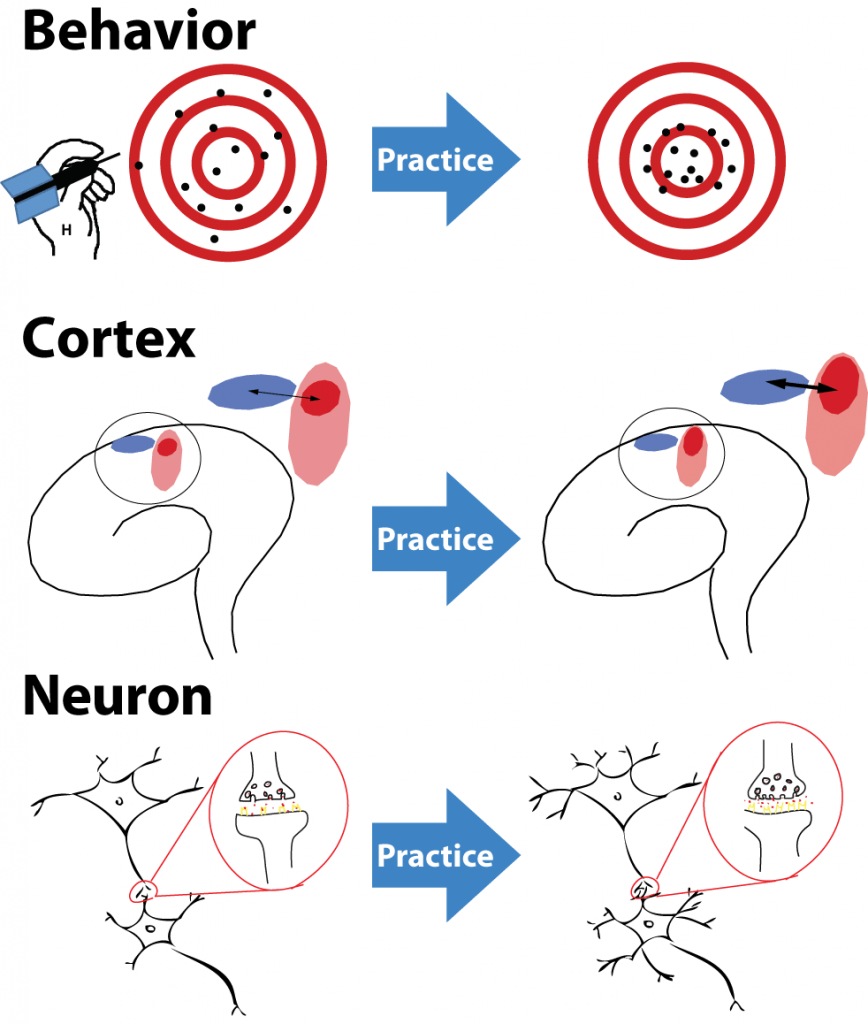
What Are The CBT Effects On The Brain?
t stands to reason that CBT could influence the processing of pain signaling since CBT effects how one thinks. Recent Neuroscience studies have disclosed that the chemical substances used for one nerve cell to “speak” to another, called neurotransmitters, are actually changed by CBT.
Serotonin, Norepinephrine, Dopamine, and many other neurotransmitters can actually be raised or lowered through CBT. The CBT exerts its effect through frontal lobe activation (remember this is where thought occurs) and modifies the effect of the neurotransmitter. Do this enough and permanent changes occur in the anatomy and physiology of the brain.
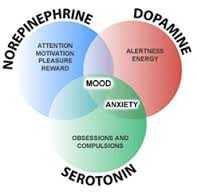
This process is much more precise than using medications, or electrical stimulation, or surgery as the exact pathways for the chronic pain are being effected. Furthermore, the unique “connectome” or neural network that has been established through years of experiences is precisely effected by CBT.
With continued CBT the “neuroplasticity” that occurs (it generally takes 6 weeks for this to begin to happen) will result in a significant clinical improvement. Most patients report a reduction in pain, anxiety, insomnia, and depression. Many patients end up taking less medication (and some even wean off their medications).
What Can CBT Be Used For?
The following disorders have all been shown to be improved with CBT:
- Nearly all forms and types of chronic pain
- Fibromyalgia
- Chronic Fatigue
- Chronic Anxiety
- Chronic Depression
In addition to the above disorders CBT has also shown great usefulness in the following disorders:
- Schizophrenia
- Substance Abuse
- Bipolar Disorder
- Eating Disorders
- Criminal Behavior
- Anger and Aggression
The Classic CBT Program Looks Like This
The classical structure of a CBT program always includes a certified CBT therapist, 30 to 60 minute counseling sessions, weekly or biweekly sessions, and homework. The person being counseled will be expected to continue their therapy by performing a series of cognitive exercises between sessions at home. The “homework” extends the therapy session and advances the process of neuroplasticity.
CBT is not structured to be a lifetime of counseling. The goal is to teach a person how to interrupt maladaptive thinking. Once taught, the need for continued counseling is finished. The individual becomes their own counselor and may only need occasional “refresher” sessions.
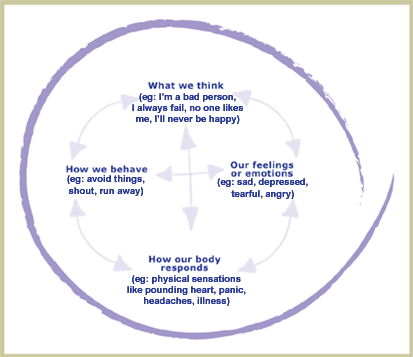
The sessions continue until the goal of retraining has been met. As was mentioned earlier in this article, CBT invokes “neuroplasticity.” The process takes time (demonstrable neuroplasticity has been shown on functional MRI testing as early as 6 weeks). The patient will need to be patient…and do their homework for the neuroplasticity to occur.
You Must Find a Genuine CBT Counselor
Not all counselors that market themselves as a “CBT Therapist” are actually trained in the modality. When CBT was first developed there were few therapists. Today most Americans will have access to this very effective form of therapy.
There are some on-line programs available too. When attempting to find the right therapist remember to inquire about their training in CBT and see how the “personality fit” is with them. When it comes to a psychotherapist, the emotional bond that you develop is essential for the therapy to be effective.
Summary
I have discussed the anatomy, physiology, effectiveness, and structure of Cognitive Behavioral Therapy. This therapy is an effective way to reduce pain and treat a variety of disorders.
My hope is that you have enjoyed this article. If you have further questions, please comment. I would love to hear from you.
Wishing you good health and much joy.