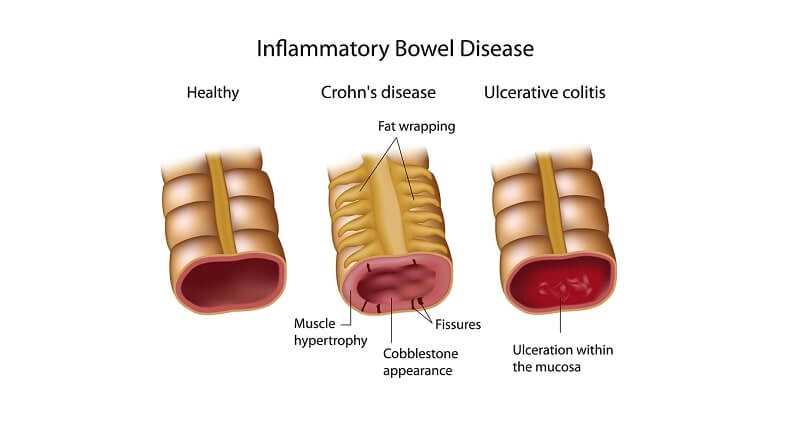
Complications of Crohn’s Disease

Bleeding
It can be pretty scary to look down into the toilet and see blood, especially if there’s a lot of it. Rectal bleeding is a common symptom of Crohn’s disease and the amounts of bright red blood that can appear in the stool are sometimes quite alarming.
This symptom of Crohn’s disease is the cause of many other complications associated with the condition, including lack of nutrients and low red blood cell count leading to iron deficiency and anemia.
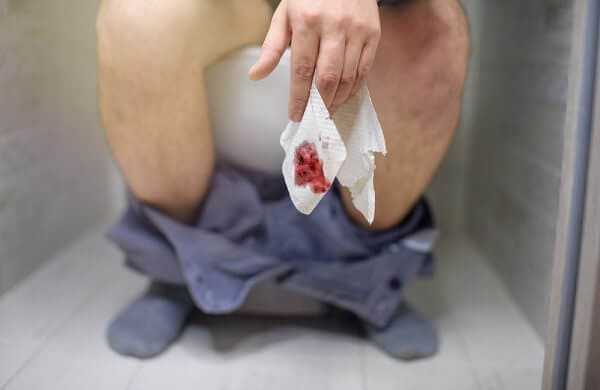
Bleeding may occur sporadically or seem to have no rhyme or reason, but its presence signals the effects of inflammation in the gut. Amount and frequency of blood may be related to the ingestion of foods high in fiber, but there are also some who believe that foods with high amounts of sugar and complex carbohydrates can play a role as well.
Eating foods that are not on the normal diet of the individual, such as going out to eat at a restaurant and trying something not commonly eaten, may have an effect on the bowel and thus result in rectal bleeding.
Anemia
Anemia is a condition where a low red blood cell count results in the cells of the body not receiving the proper amount of oxygen. It can cause tiredness and a feeling of lethargy, even after a full night’s sleep.
In Crohn’s disease, the body commonly loses blood through the digestive tract, where bleeding caused by inflammation can be significant enough to lower the patient’s red blood cell count.
This specific condition is called pernicious anemia, and is characterized by vitamin B-12 deficiency caused by gastritis, or inflammation of the gastrointestinal tract.

Someone suffering from any type of anemia is said to be anemic.
Severe anemia can bring on other complications, including heart palpitations and irregular heartbeat, among others.
Anemia can be treated with iron, which promotes the formation of new red blood cells in the body. Amounts of iron in the body must be brought up to normal levels within the body, which can be done with supplements or by eating foods high in iron.
Consumption of foods high in iron is the most natural way to receive the nutrient, so eating foods like beef, liver, and spinach can help to immediately boost levels.
Iron pill supplements may work as well, but they are believed by some to be harsh on the system and somewhat difficult to absorb, so for a Crohn’s patient who may already be having difficulty digesting certain things, these supplements might be less effective than simply eating high-iron foods.
Diverticulitis
Since Crohn’s disease affects all layers of the bowel, a condition can occur where inflammation causes pouches to develop on the exterior of the colon. This precursor to diverticulitis is known as diverticulosis; it develops into the former when one or more of these pouches becomes infected.
Diverticulitis is thought to be caused by a lack of fiber in the diet, and since low-fiber diets are a commonly recommended treatment for Crohn’s patients, the risk of diverticular disease can be heightened.
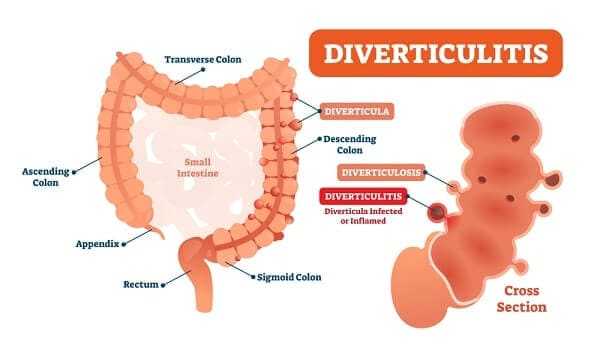
Surgery may be necessary to remove the infected pouch(es), but in many cases diverticulitis is treated similarly to Crohn’s itself, with low-fiber diets or limited food taken by mouth to rest the gut and allow it time to heal.
After the condition is believed to have been relieved, the usual course of action is to put the patient on a high-fiber diet as this is believed to be a measure of prevention against recurrence. A Crohn’s sufferer, however, does not always have so straightforward a solution.
A good way for Crohn’s patients to avoid diverticular disease is to keep a limited amount of fiber in their diet by eating cooked vegetables and fruits, although the benefits of this course of action varies from patient to patient and should of course be discussed with your doctor first.
Malabsorption
When the body cannot efficiently take in nutrients from the food you digest, you don’t receive the nourishment you need from eating. Minor to severe malabsorption can occur in patients with Crohn’s disease because the intestinal tissue normally responsible for absorbing nutrients is inflamed and doesn’t do its job effectively.
Malabsorption leads to malnourishment, which can cause a host of other complications of which weight loss is only the beginning. Malnourishment opens up the doors for endless problems.

Think of your body as a business, with food as its customers. It opens its doors and lets in customers that fuel the business.
Malabsorption is like having lots of customers who never buy anything. They go into the business, look around, and then leave. When the body doesn’t get the fuel it needs to keep going it has no choice but to shut down!
No matter how much you eat, if you’re suffering from extreme malnourishment it’s almost like you’ve eaten nothing at all.
The only way to treat malabsorption is to get the digestive tract back into a healthy enough state that it can start digesting food again. This is most commonly done with medicinal treatment – corticosteroids to quickly reduce inflammation and then some type of maintenance drug to keep the inflammation down.
Strictures
Healing in the body is usually a good thing. When the body heals itself, it covers its wounds with scar tissue to strengthen the areas that were previously damaged.
The human body has limits and thus a scar is never a perfect replication of the tissue that used to be there before the injury. It’s often a somewhat hard, rough area where the body fuses its flesh back together.
The digestive tract is designed to expand and contract in a process known as peristalsis, which pushes the food through your system. Scar tissue is hard and not flexible like normal tissue, so it can’t do the job as easily.
Since Crohn’s disease affects every layer of the digestive tract, inflammation that heals within the ‘tubes’ of your intestines can form rings of hard scar tissue that tighten and limit the passage of food matter. As these rings form additional layers of scarring, the pathways constrict and make Crohn’s sufferers prone to intestinal blockages.
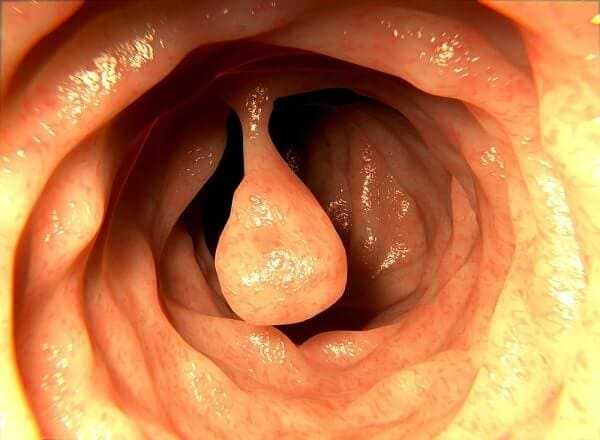
Strictures can be treated with the normal means of medication, through surgery, or other procedures like balloon dilation.
Strictures are named and specified by their location in the body – an esophageal stricture occurs before the stomach, a duodenal stricture in the first portion of the small intestine, an ileocecal stricture between the connection of the small bowel to the large bowel, etc.
Bowel Obstructions
A bowel obstruction occurs when particles of food are caught in the twists and turns of the intestinal tract. This can happen if you have any type of blockage, if a section of bowel is improperly twisted and closed off, if severe inflammation closes off the passage, or if a stricture has become so narrow that it stops food at that point.
High-fiber foods are more likely to cause obstructions than low-fiber foods, because of the rough residue that accompanies undigestible fibrous material.
When the body cannot expel food out the bottom end as it should, it is left with only one other choice. A bowel obstruction is accompanied by a feeling of tightness or pressure in the abdomen, and if not remedied will most likely result in severe nausea and vomiting.
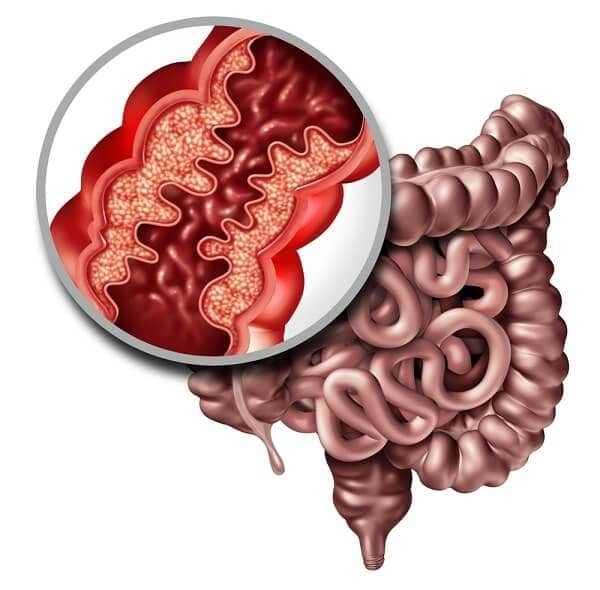
The pressure associated with an obstruction may soon become very painful and begin to throb or pulsate every few seconds or minutes as food builds up and the bowel attempts to push the food through the tight space. If left untreated, a severe obstruction could cause rupturing, which you do NOT want to mess with.
I’ve been to the hospital because of bowel obstructions several times and believe me, if there was an actual fun scale, it would rate in the negatives. Don’t let that deter you, though; it’s much easier to get over an obstruction if you act early and get the proper treatment.
Often with an obstruction, the pressure that builds up behind it must be relieved before the blockage can naturally clear itself. Doctors will usually resort to surgery only if the blockage doesn’t clear itself with treatment.
A common treatment for intestinal obstructions (and one that I’ve undergone too many times) is the placement of a nasogastric tube, called an NG tube for short. Basically, they insert a flexible tube that resembles a fish tank line up your nose and down into your stomach.
They connect the tube to a suction pump that slowly pulls stomach fluids and air up from your stomach and relieves the pressure over the course of several hours or days. The worst part is going in – after that, you get used to it and coming up it feels SO good getting that thing out of you!
Here’s a tip if you’re worried about a bowel obstruction. I’m not recommending that you use this instead of a visit to the doctor or the hospital if you need it, but since the pressure needs to be reduced to help the blockage clear itself you can try this remedy:
Lie down on your back, on the floor or on your bed. Make sure you have enough room between you and the ceiling to extend your legs upward, then curl into a ball and slowly lift your legs up and support your lower back with your hands, resting your elbows against the ground or bed. What you’re doing is turning your bowels upside down to let any trapped matter move around and shift itself so that air can escape.
Stay like this for several minutes, and if you can maintain your balance try swiveling your hips or swaying from side to side to loosen things up. Sometimes this can be really helpful if you have gas associated with Crohn’s, but I’ve also found that if I start to feel that pressure in my abdomen this can help out a lot.
Again, this might help, but don’t use this tip in place of medical advice! See your doctor or get to a hospital if you think something is seriously wrong!
Colon Cancer
Patients with Crohn’s disease have an increased risk for development of colon cancer. While this risk is greater than that of the average population, it is nonetheless believed in some medical circles to be slightly smaller than that in patients with crohn’s counterpart, ulcerative colitis.
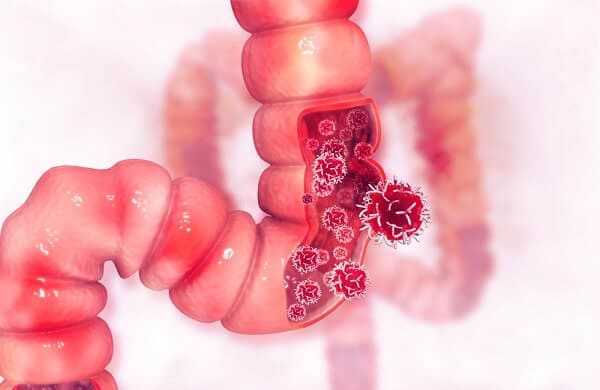
Statistically speaking, Crohn’s patients are estimated to be between ten and twenty times more likely to get colon cancer at some point in their lifetime than the general population.
Colon cancer in Crohn’s patients does not always appear in the areas of the bowel that are most damaged; in some cases, cancer develops in sections of bowel that were minimally affected by the disease prior to its appearance.
Fistulas
Ok, can I just say something? Fistulas are disgusting. They make me shudder. There. Sorry, had to get that out of the way. I’ve had this condition in the course of my disease so I think I have the right to say it.
A fistula is a passageway from one organ in the body to another. Fistulas are fairly common in Crohn’s because the inflammation associated with the disease can cause tissue within the body to literally deteriorate or wear away.
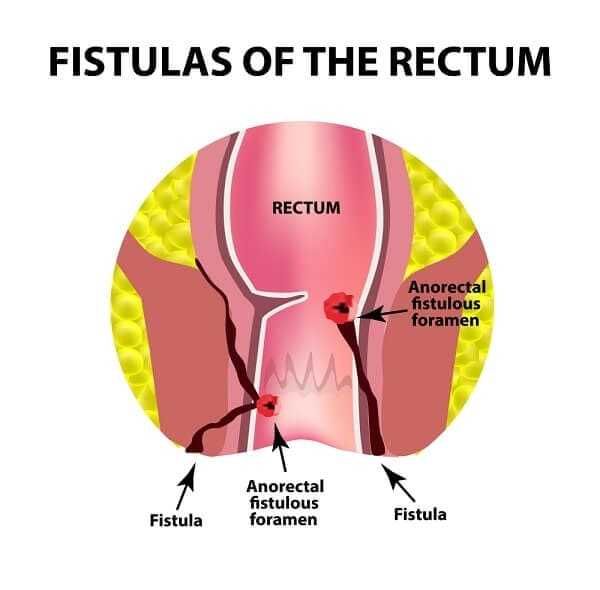
If two organs are adjacent or pressing up against one another, the continued damage and re-healing of tissue can cause the two organs to fuse together, creating a fistula between them.
Fistulas can also be tunnel-like, and may form either from one internal organ to another or from an internal organ to the surface of the skin. For example, I had one fistula from an area of damaged large intestine that ran to my duodenum, the first portion of the small intestine just after the stomach.
In my particular case the fistula was remedied surgically, as I was already undergoing a resection and the doctor took care of both problems at once. But it is possible for a fistula to heal, so don’t be afraid that just because you have a fistula it automatically means you have to have surgery.
Fissures
A fissure is – get ready for the cringe-factor – a tear in the skin of the anus. It may be caused by inflammation of the area from frequent bowel movements or continued wiping.
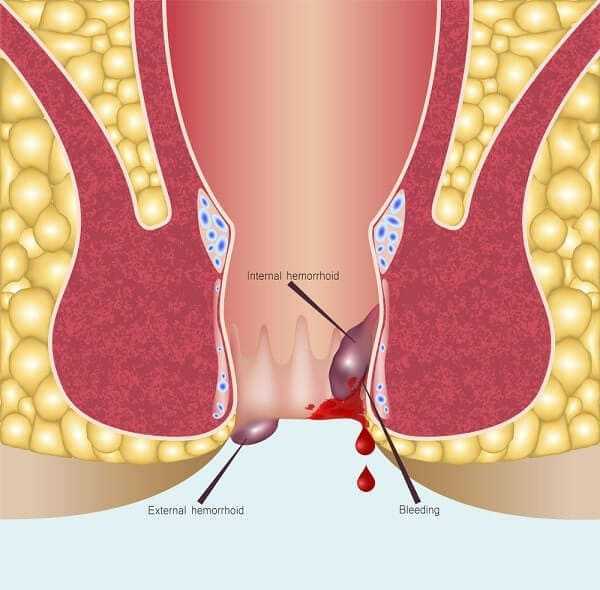
Since the area of the body in which fissures can occur is frequently exposed to high levels of bacteria and germs – and even more so in patients living with Crohns disease – they can take longer to heal than the average cut or abrasion.
Treatment usually involves a topical medication and the recommendation that you use caution and act gently upon the affected area to avoid infection. They may last for a long time, but can usually be healed by taking the proper precautions.
Abscesses
An abscess can happen in any part of the body, but in those with Crohns they typically appear in the affected areas of the digestive tract and are due to damage caused by diseased portions of the bowel.
If you’re as squeamish as I am, then it’ll be just as bad for you to read this as it is for me to write it. An abscess is an infected cavity in the body that fills with pus. This reaction is the body’s defense mechanism against the spread of the infection.
Abscesses can be drained if they appear on an external location in the body, but in the case of an internal abscess, such as along the lining of the bowel, they may be biopsied or surgically removed. Normally treatment is not so severe as to warrant surgery unless no other alternative, such as treatment with antibiotics, exists.
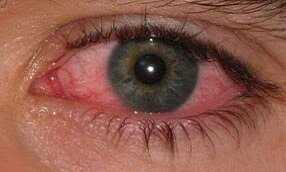
Eye Inflammation
This is one of those secondary, long-term effects of living with Crohns disease that can happen as one of a subset of problems related to malnutrition and/or general inflammation within the body.
The overall health of the body is thought by some to be linked to the health of the gut, so when things begin to go wrong with the system that absorbs our nutrients and a false reaction is triggered, this can have severe implications for other parts of the body over time.
Inflammation of the eyes for people with Crohns can start with only the inability to focus. Vision may become blurred or the patient may have difficulty maintaining focus for long periods of time. Blindness can occur in severe cases, but as mentioned above this can be primarily due to the continued lack of sufficient vitamins and minerals to keep the eyes in good health and working order.
Polyps
In Crohn’s disease, part of the body’s defense to the inflammation present in the gut is to secrete high amounts of mucous membrane as an agent to help sooth the affected areas. Abnormal tissue growth extending from these areas are called polyps. Polyps may be benign, but in all cases they pose the threat of becoming cancerous and therefore increase that risk in patients affected by them.
Polyps often appear around the most diseased areas of the small or large intestine in Crohn’s patients, and are characterized by severe pain whenever stool passes through those specific areas. Those present in the large intestine can sometimes be biopsied (removed for laboratory tissue sampling) during colonoscopy, and thus symptoms can be alleviated if there is little risk of perforating the bowel in doing so.
Polyps may protrude from the intestinal lining as a lump; this type of polyp is said to be a sessile polyp. They may also extend from the surface at the end of a thin stalk. A polyp with a thinner stalk is known as a pedunculated polyp.
Ulcers
An open sore in the digestive tract, primarily occurring in the lower esophagus, stomach, or duodenum (the first part of the small intestine) is called an ulcer. In those living with Crohns disease, this problem occurs when inflammation in any of these areas causes the lining of the tract to become damaged.
Normally, the stomach acts upon food that is eaten by breaking it down using acids that are secreted. The muscles of the stomach toss the food around and essentially mix it with these acids to cause this process to happen within a matter of hours.
The lining of each area that is usually exposed to stomach acid forms a protective barrier against the corrosive matter itself. When the lining is damaged, however, the effectiveness of this shield is also reduced, and therefore can cause acids to begin to digest the exposed flesh itself. In some cases, a bacteria called H. pylori acts on this area by working its way through the weakened protective lining and attaching itself to the wall of the stomach.
I realize this sounds like a pretty gruesome picture, but the fact is that this can happen in Crohn’s affecting the stomach because the body triggers this inflammatory reaction on its own. Ulcers can be caused by several other factors outside of Crohn’s disease, including the use of painkillers like NSAIDs including aspirin and ibuprofen, consuming excessive amounts of caffeine, and smoking.
Ulcers may induce symptoms of burning pain in the lower middle chest, including nausea, weight loss, loss of appetite, and vomiting – sometimes with blood present in the vomit. Recommended treatment for ulcers includes lifestyle changes, antibiotics, mucosal protective agents (antacids like Tums, Rolaids, and Pepto Bismol), and acid suppression methods including acid reducer medications (Zantac, Pepcid, etc.) and proton-pump inhibitors like Prilosec.
Spleen Enlargement
The spleen is located beneath the left side of your rib cage, between where the ribs stop and your navel. It can become larger than normal without any symptoms occurring whatsoever, but a severely large or inflamed spleen may begin to cause pain, discomfort, and a slight feeling of pressure on the right side of the abdomen.
Pain from spleen enlargement can also spread up to the shoulder and left arm as well.
The spleen performs several functions in the body related to the blood. It manufactures white blood cells to fight infection, stores platelet cells that help the blood clot, and acts as a filter by removing bad blood cells.
It is possible to live without a spleen, and in fact spleen removal through surgery is fairly common. Without a spleen to create enough cells that guard against disease, a person assumes a greater risk of serious infection occurring in the body.
In Crohn’s patients, an enlarged spleen is associated with the anemia and blood loss that also occur in sufferers of the disease. Irregular amounts of the different types of blood cells in the body are further skewed because once the organ becomes inflamed it cannot process or produce the cells in sufficient amounts.
Some drugs used in the treatment of Crohn’s disease, such as Remicade, are said to help reduce enlargement of the spleen. Other drugs that reduce general inflammation in the body may also be prescribed.
Surgery is an option, but one which carries some possible complications with it, including post-surgical infection. If left unchecked, however, an enlarged spleen could rupture, resulting in lethal levels of toxicity in the abdomen.