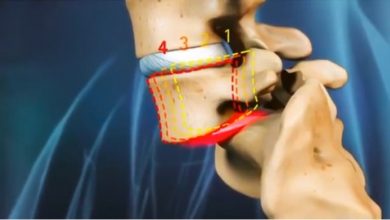
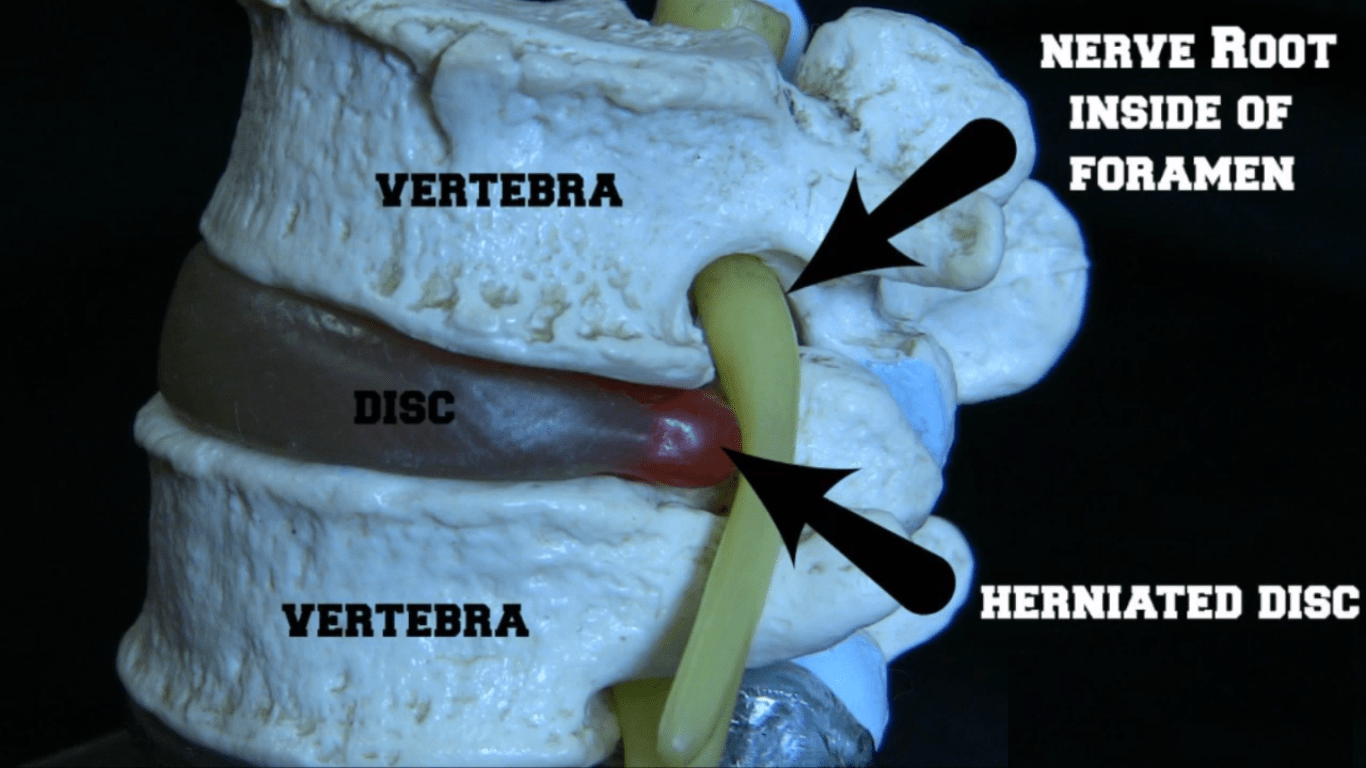
Degenerative spondylolisthesis
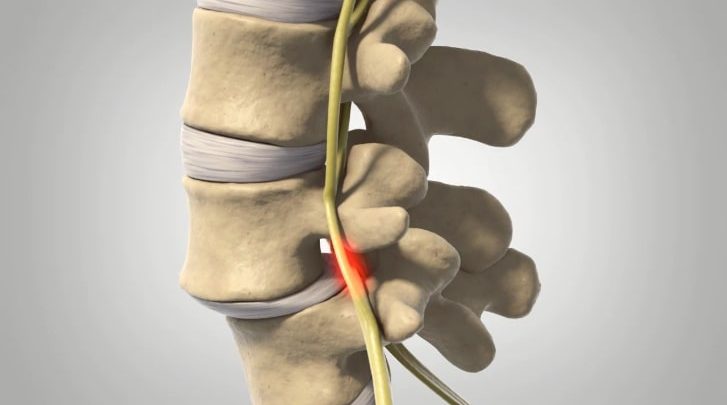
Degenerative spondylolisthesis is one of six types of this spinal condition. It occurs as a result of the general aging process; therefore, it is more often seen in the elderly than in young adults. While it is common for people over 50, it is even more likely to be seen in people over 65. Females will develop degenerative spondylolisthesis over males.
Degenerative Spondylolisthesis Definition
This is a spinal condition where a vertebra slips forward over the one below it. As your body ages, your bones, ligaments, and joints in the spine tend to become weak and are sometimes not able to support the spinal column in alignment.
This condition will usually occur in either the L4-L5 level of your lower spine, which is the most common location. It can also be present at the L3-L4 level. While it is a possibility that degenerative spondylolisthesis can be present in other levels, it is rare.
This version of spondylolisthesis can also occur in the cervical area (neck) of your spine; however, when this does happen, it is generally considered a secondary problem to arthritis in the facet joints.
Causes of Degenerative Spondylolisthesis
Your joints will undergo a degenerative process as you age. In each spinal vertebra, there are two joints that are composed of inferior and superior articular processes (facet joints). These facet joints are held in place by capsules (fibrous tissues). The capsules become thin as part of the normal aging process. They then weaken. This can cause the capsule to stretch and cause one vertebra to slide over another.
Two of the most common primary conditions that can lead to this version of spondylolisthesis are: osteoporosis and osteoarthritis. Osteoporosis can weaken your spinal bones, which can cause vertebral fractures that can cause the spinal bones to shift and then slip. Osteoarthritis can increase bone on bone contact. This can grind down the spinal bones causing them to slip.
Diagnosing Degenerative Spondylolisthesis
Your doctor will first review your medical history (symptoms). A physical examination will then be performed. You will be examined for physical symptoms, which include range of motion, flexibility, muscle weakness and/or neurological symptoms.
Diagnostic tests will be performed if the doctor suspects spondylolisthesis after the medical history and physical exam. The first diagnostic test will be an X-ray. If further tests are needed, it is possible an MRI scan may be ordered for a more in depth look.
Symptoms of Degenerative Spondylolisthesis
- Lower back pain
- Muscle spasms
- Pain with radiation to the buttocks and/or legs
- Lower extremity weakness or numbness – (RARE)
- Pain comes on with activity (example: during walking)
Treating Degenerative Spondylolisthesis
Prevention is the best way to treat this condition. Take steps early to prevent age related health conditions, such as osteoporosis and osteoarthritis that lead to degenerative spondylolisthesis. A treatment plan is based on your symptoms.
Bed rest for one to two days could help to relieve immediate discomfort. Your doctor may also prescribe an anti-inflammatory and/or pain medication to help alleviate symptoms. If needed, your doctor may also prescribe an epidural steroid injection to alleviate inflammation.
It is possible you will be given a brace to help stabilize your spine. It can be worn as needed for a short period of time. Physical therapy is also an option to increase back conditioning. Muscle strengthening helps to reduce the frequency and intensity of spasms.
Surgery is an option, but will not be considered unless there is an acute neurologic deficit, such as significant leg weakness or if the slippage is pulling on the nerves exiting the spinal canal causing pain, numbness, and/or weakness. Surgery is a last resort. If surgery is necessary for degenerative spondylolisthesis, it will require fusing the slipped vertebrae to the adjacent vertebrae.