Endoscopic Spinal Surgery
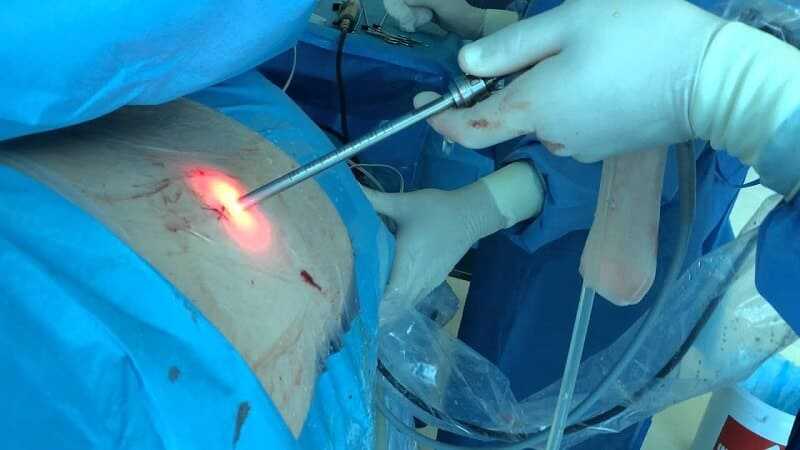
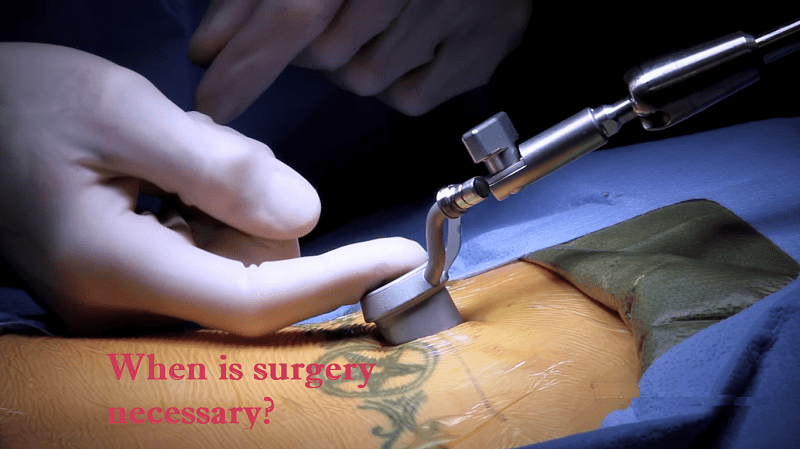
Endoscopic spinal surgery is a type of minimally invasive back surgery. Traditional back surgery involves making a large incision down the back or neck, retracting the muscles away from the surgical area, and inserting instruments into the trouble spot. Endoscopic spinal surgery is much different, as it uses a special tool that only requires a 1 inch incision to complete the procedure.
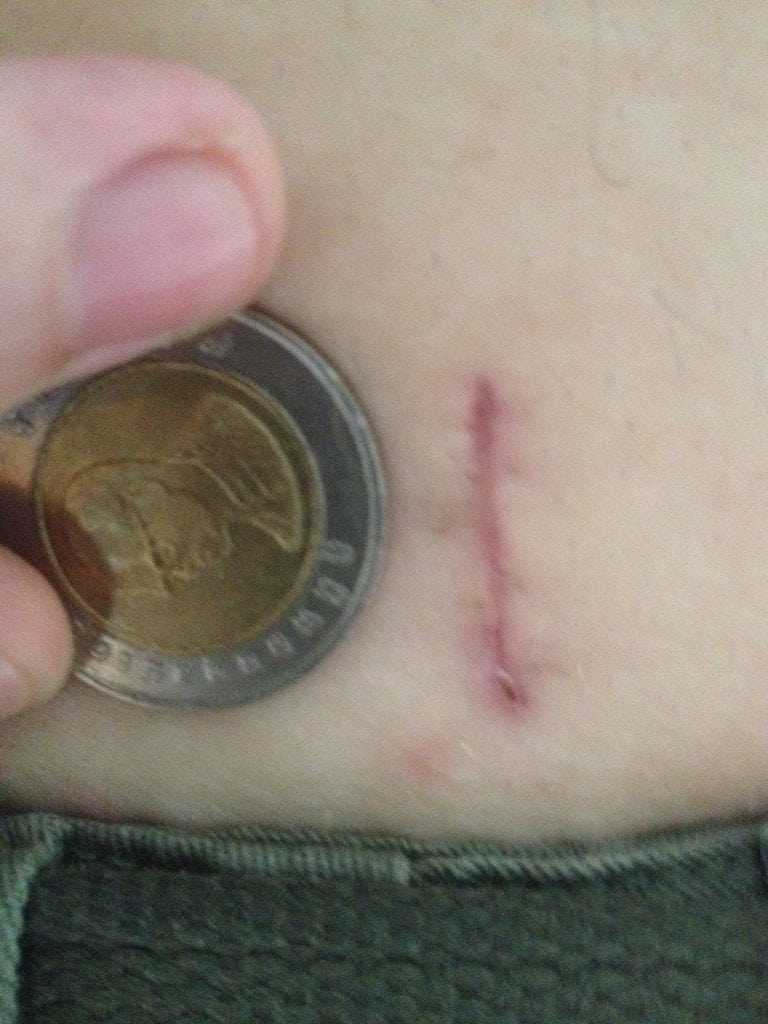
The surgeon makes small incisions in the back, usually no more than an inch, at various places. Through these incisions, he inserts small, fiber optic cameras and instruments. These endoscopes are usually no wider than a pencil, and they are able to manipulate the structures of the back without opening the skin wide. With the smaller instruments and high tech cameras, a surgeon can easily perform surgeries that would have caused pain, infection, and scarring just a decade before.
Conditions Treated with Endoscopic Spinal Surgery
Many conditions that were traditionally treated by open back surgery can be performed with endoscopic spinal surgery. For instance, the curvature of the spine, such as side to side scoliosis or front to back kyphosis, can be treated with an endoscope rather than traditional surgery. Tumors that occur in the spinal column can also be treated with a minimally invasive approach, and fractures of the vertebrae can be stabilized using this procedure.
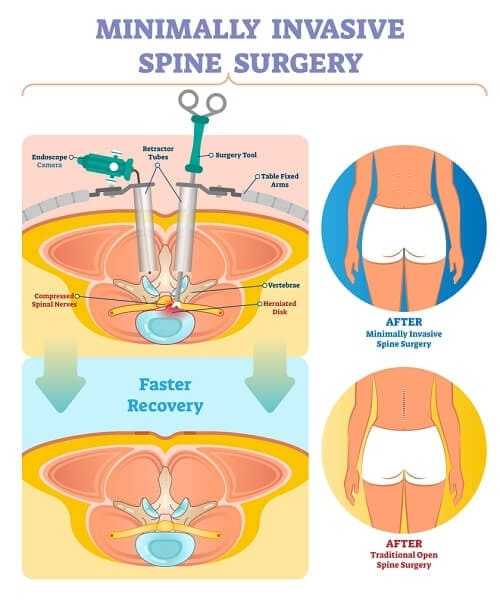
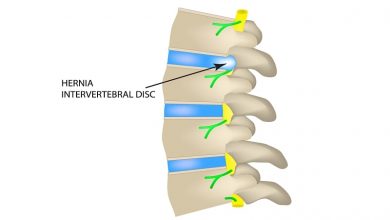
One of the most important applications of endoscopic spinal surgery is the treatment of degenerated discs. Surgeons can now repair and remove slipped and herniated discs that are pressing on nerve roots and causing pain. This means it can be used for such conditions as sciatica and degenerative disc disease. A surgeon can easily remove a disc and fuse the vertebrae together for a spinal fusion. This type of surgery usually involved a great deal of pain, a large scar, and a risk of infection. With this new technology, patients can be up and walking the same day — and with less pain than before.
Risks and Benefits
The most obvious benefit of endoscopic spinal surgery is smaller incisions. This means that you have less pain, less likelihood of infection, and less blood loss in surgery. Since muscle retractors are not used, the pain associated with moving tissue out of the way is lessened. You will also not have the risks of damaging muscle tissue and nerves that are near the site of surgery. You will not need to be in the hospital as long, and your post-operative recovery course is usually much less than with traditional surgery. Instead of rehabbing your back for a year, it can sometimes conclude within a month or so.
Even though the risks of surgery are lessened with minimally invasive surgery, the still do exist. You run the risk of infection to the incisions, but this is far less than with traditional surgery. You may even experience damage to surrounding tissue, and the effects of anesthesia can sometimes cause a reaction. One common risk associated with this procedure is the formation of blood clots in the legs that can go to the heart or lungs. This can cause death if the clots are not caught soon enough. However, with post-operative exercises and machinery, the risk for this side effect is also very low.
If you have a back problem that traditional surgeons want to fix with a long incision, you don’t have to allow it.