Frequently Asked Questions about Vertebroplasty

Who gets vertebral fractures?
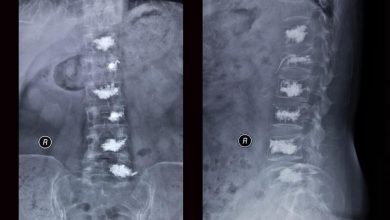
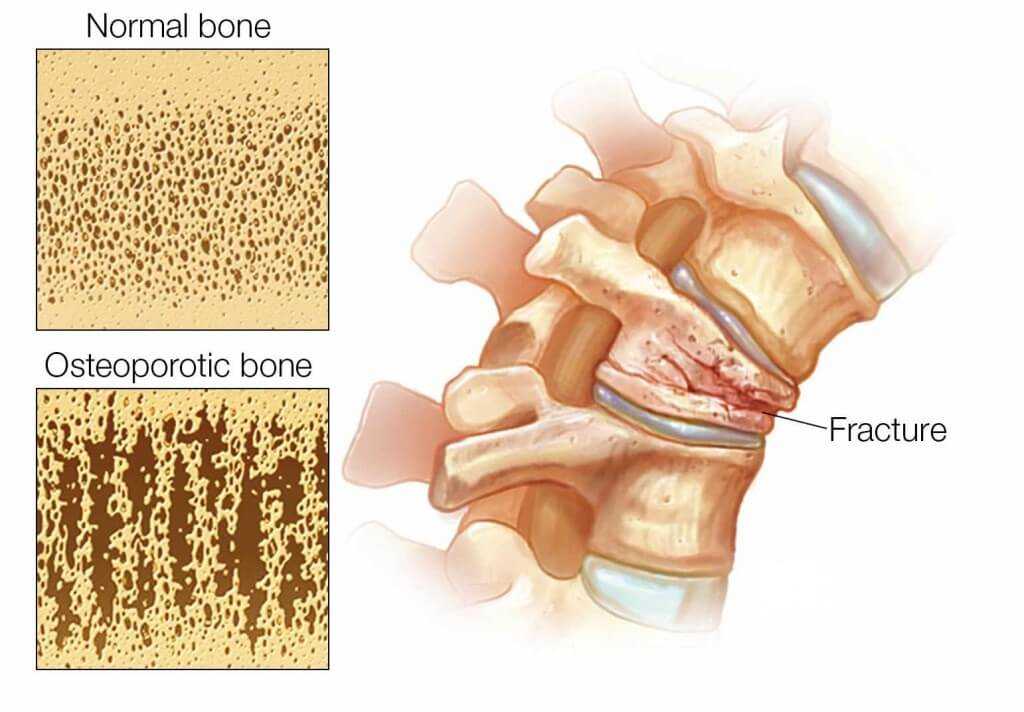
Osteoporosis is the leading cause of vertebral fracture. In osteoporosis, there is progressive bone loss, creating structural weakness and skeletal fragility. After menopause, women become especially susceptible to bone loss and the development of fracture. Osteoporotic fractures most commonly involve the hip, wrist and spine. Lifetime risk of any symptomatic fracture is 40% in women, and 13% for men. Lifetime risk of symptomatic vertebral fracture is 16% in women and 5% in men. Eighteen per cent of women over 50 years old and 27% over 65 years old will suffer one or more symptomatic vertebral fractures due to osteoporosis. Approximately 700,000 vertebral fractures occur annually in the United States.
For more information about “Osteoporotic Fracture”, click here.
What is vertebroplasty?
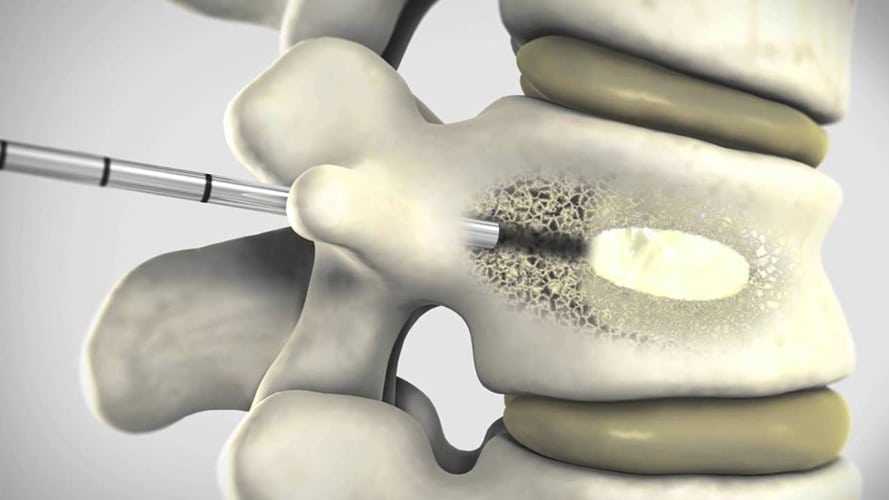
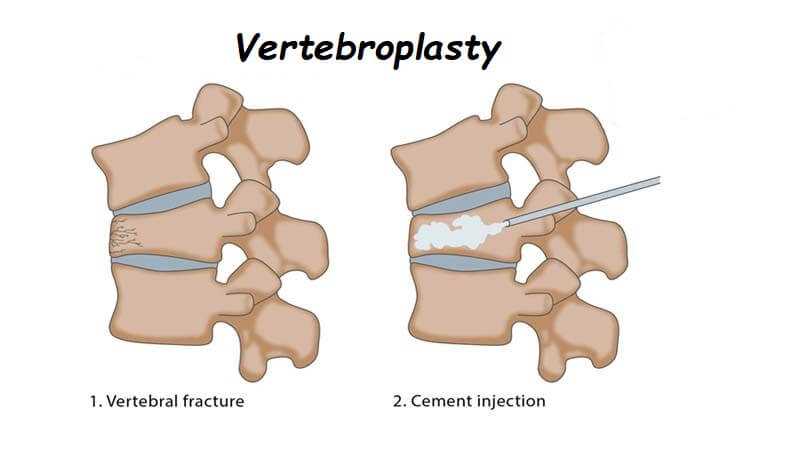
Vertebroplasty is the injection of cement-like material (bone mineral substitute) into a collapsing vertebral body. The procedure is performed to reinforce the fractured bone, alleviate chronic back pain and prevent further vertebral collapse. The cement-like material stabilizes and strengthens the crushed bone. Vertebroplasty was developed in France in the 1980’s, but is relatively new in the United States. It is currently available in only some hospitals.
What are the results of vertebroplasty?
Vertebroplasty is a non-surgical procedure that usually provides pain relief and increased mobility within 48 hours. Over several weeks, two-thirds of patients can expect a marked decrease in their doses of pain medications. Many patients become symptom-free. Three-quarters of patients can expect to increase their mobility and activity levels. Vertebroplasty cannot correct curvature of the spine caused by osteoporosis, but may help to prevent worsening curvature. The procedure treats only the fractured vertebra. It does not prevent future compression fracture at other levels.
Until vertebroplasty, treatment options for vertebral compression fracture were limited to bed rest, pain management with strong oral or intravenous medications, reduced activity, back bracing or invasive spine surgery. Vertebroplasty may prevent the need for placement of rods and screws to support the spine.
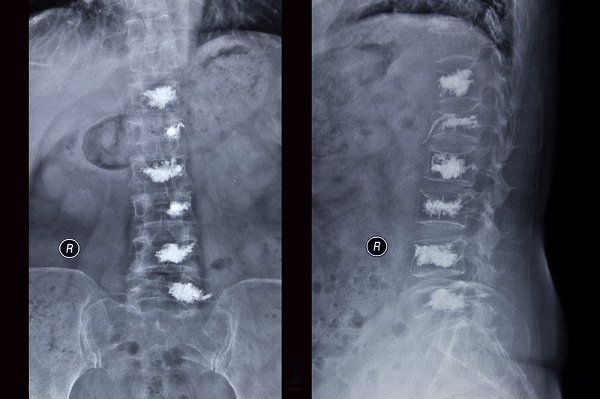
How is vertebroplasty performed?
Vertebroplasty is a non-surgical procedure that is performed using state-of-the-art imaging (fluoroscopic) guidance. The procedure is usually performed in the morning. Patients must be able to lie face down for 1-2 hours. Some patients with severe emphysema or other lung diseases may have difficulty lying in this position. Our team of professionals will make you as comfortable as possible. An intravenous line is placed in the arm to decrease anxiety and control pain. Intravenous antibiotics are also administered to prevent infection.
https://www.youtube.com/watch?v=8XOHsNkjdS8
After using a local anesthetic to numb the skin and muscle, a needle is positioned in the collapsed vertebral body. We inject a radiology contrast agent (contains iodine) to confirm proper needle placement, followed by the cement-like material. The longest part of the procedure is setting up the equipment and positioning the needle in the collapsed vertebral body. The actual injection of cement takes only 10 minutes. Medical-grade cement is similar to epoxy or glue. It is injected in a liquid form that quickly hardens over 10-20 minutes. We usually obtain a CT scan after vertebroplasty to evaluate the distribution of cement.
What are the risks of vertebroplasty?
Although vertebroplasty is safe and effective in most cases, the procedure should be performed only if a patient has back pain that significantly impairs mobility and quality of life. Potential complications include bleeding, infection, and worsening of pain. In patients with severe osteoporosis, rib or vertebral fracture can occur. Since the cement is injected as a liquid, it can leak out of the vertebral body into surrounding tissues and veins. Surgery is rarely required to remove the cement that has leaked, although it is a possibility.
Who is eligible for vertebroplasty?
Candidates for the procedure include men and women who have chronic back pain (at least 6 weeks) and debilitation due to vertebral body fracture. Patients often have limited mobility and cannot perform routine daily activities, such as bathing, dressing and walking. Vertebroplasty is usually performed after conservative treatments (bed rest, back brace, oral pain medications) have failed. Most patients are elderly (average age 70 years), but younger patients with osteoporosis, due to metabolic disorders or long-term steroid treatment, may also benefit from vertebroplasty. Some patients with vertebral destruction from malignant tumors are also candidates for the procedure.
Who is not eligible for vertebroplasty?
Not all patients with vertebral fracture are appropriate candidates for vertebroplasty. Careful screening is critical to ensure that symptoms are due to the vertebral fracture, rather than another problem. It is not enough that patients have a vertebral fracture, since a healed fracture should not cause pain. Thus, it is necessary to exclude other potential explanations for back pain, such as disc herniation, severe arthritis and compression of the spinal cord or nerve roots.
What is the pre-procedure evaluation?
All patients must be evaluated by one of our staff prior to vertebroplasty. Sometimes a telephone interview is sufficient, but usually patients must be seen in person. The evaluation includes a directed history and physical examination and blood tests. Often, patients can point to a single painful spot. If the location of pain matches the level of fracture seen on standard radiographs (x-rays), then there is a good chance that vertebroplasty will be successful.
If a patient is receiving anti-coagulation treatment (coumadin), it is necessary to stop the medication until coagulation returns to normal. In patients who cannot discontinue their coumadin, it may be necessary for brief hospitalization and intravenous treatment (heparin).
At our initial evaluation, patients should bring any imaging studies that were not performed at MGH. It is essential that all patients have recent plain radiographs and MRI. If MRI cannot be performed (due to a cardiac pacemaker, for example), CT scan is necessary. Some patients may need examination under fluoroscopy or bone scan.
Post-procedure care:
Patients usually recover after a few hours and can go home with an adult if the trip is short. Otherwise, patients should plan on staying overnight in a local hotel. Hospitalization is not required unless the patient is extremely frail or requires additional monitoring after the procedure.
There may be dull aching at the needle puncture sites during the first 24 hours following the procedure. An ice-pack can help with this discomfort. Tylenol or non-steroidal anti-inflammatory medication is usually sufficient. Narcotic pain medications should be minimized. You should call your doctor if you develop severe or increasing chest or back pain, fever, or neurological symptoms.
Patients are called at home approximately 48 hours and 7 days following vertebroplasty. Otherwise, patients receive follow-up care from their referring or primary care physicians. To hasten recovery and regain satisfactory levels of activity, patients may benefit from physical therapy or short-term back bracing. Osteoporosis should be treated if medical therapy has not already been instituted.
Facebook
Google+
Twitter
Pinterest
Reddit
StumbleUpon