Genes May Predispose You to IBD

There are several reasons for believing that IBD has a genetic component. It is important to realize that most IBD patients do not have any relatives at all with IBD. But if a person has ulcerative colitis, there is about a 10 percent chance of IBD in other members of the extended family, with ulcerative colitis more likely than Crohn’s disease. On the other hand, if a person has Crohn’s disease, there is about a 15 to 25 percent chance of IBD in the extended family, with Crohn’s disease more likely than ulcerative colitis. If a person has IBD, the risk of that person’s child developing IBD is thought to be about 5 percent. Remember that this means the child has about a 95 percent chance of not developing IBD. However, if both parents have IBD, the risk of IBD occurring in the children seems to be at least 50 percent.

Studies of identical twins have shown that if one twin develops Crohn’s disease, the chance of the other twin developing it is 44 to 58 percent, usually within a few years. If one twin develops ulcerative colitis, however, the probability that the other member will develop ulcerative colitis is much less. There are no reports of one identical twin having ulcerative colitis and the other having Crohn’s disease. This tells us that these disorders have a similar but not identical genetic basis.
Within the last few years, human gene research has provided us with some of the most exciting developments in medicine. While little has been accomplished so far in ulcerative colitis, mutations (genetic changes) in a gene known as NOD2 (also known as CARD 15), located on chromosome 16, have been shown to predispose some people to Crohn’s in the ileum, especially the form of the disease that causes a lot of scarring and narrowing. But NOD2 mutations have been found in only one-quarter to one-third of patients. Interestingly, NOD2 is a member of a family of cell proteins associated with diseaseresistance genes in plants.
As well, researchers have identified a group of antibodies known as antineutrophil cytoplasmic antibodies (ANCA), which are present in high levels in many people with ulcerative colitis, and in a significant number of their relatives, even when those relatives do not have IBD. These antibodies are found in low levels in some people with Crohn’s disease and a small proportion of their relatives, and are not found at all in healthy families. Another group of antibodies, known as anti-Saccharomyces cerevisiae antibodies (ASCA), are present in high levels in some people with Crohn’s disease and in some of their relatives.
Another factor that may be inherited is increased permeability (leakiness) of the intestinal lining in people with Crohn’s disease (see “abnormal immunity,” below).
Certain diseases occur more commonly in people with IBD. One of the best-known examples is the arthritic disease ankylosing spondylitis. Several years ago, Canadian researchers showed an association between multiple sclerosis and Crohn’s disease, and it has been known for some time that people with Crohn’s disease have a greater chance of having psoriasis. Recent studies suggest that left-handed people are twice as likely to get IBD (either form) as right-handers. Associations such as these support the concept that there is a genetic predisposition to IBD.
While this genetic information is important, we mustn’t forget that it’s widely accepted that there are environmental risk factors for IBD as well. Genetic research has begun to reveal some of the secrets of IBD, and we can expect more positive results in the future.
Abnormal Immunity May Be a Factor
In Here, the digestive functions of the GI channel are outlined. A second function, less well understood, is that of protecting the body against potentially harmful infectious agents or chemical substances.
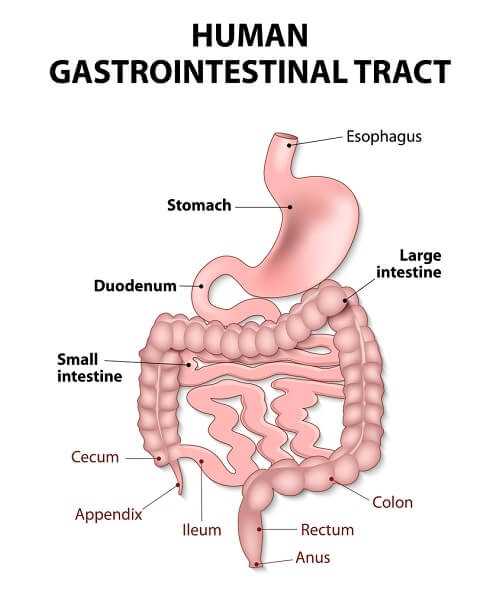
The inner lining of the intestine (the mucosa) contains many types of immune cells that act as defenders in recognizing foreign substances, known as antigens. These cells prevent such substances from passing through the mucosa and entering the body. Some of these cells, called macrophages, engulf the potentially harmful substances. Other cells, called lymphocytes, produce antibodies — chemical products that bind to and inactivate foreign substances and infectious agents. Sometimes, however, this immune response in the mucosa breaks down, and harmful agents or chemicals penetrate into the deeper layers of the intestine. This produces inflammation. This type of process may be important in IBD.
Lymphocytes also produce chemicals known as cytokines. Some lymphocytes produce Thl cytokines while others make Th2 cytokines. Normally the production of these two types of cytokines is balanced, but research shows that there is an imbalance in IBD: Thl cytokines are over-produced and Th2 cytokines are under-produced. Many treatments for IBD attempt to rebalance their production. The immunosuppressive drugs used to treat IBD (see here for details) suppress the Thl lymphocytes. Although this is frequently beneficial, suppressing any part of the immune system can have undesirable side effects. Recent work has focused on stimulating the Th2 system instead.
Research also shows that healthy people have an invisible intestinal “barrier” that can prevent various substances from being absorbed. Canadian researchers have demonstrated that this barrier is “leaky” in people with Crohn’s disease, so that substances that would not normally be absorbed may be able to enter the intestinal tissues and trigger inflammation.
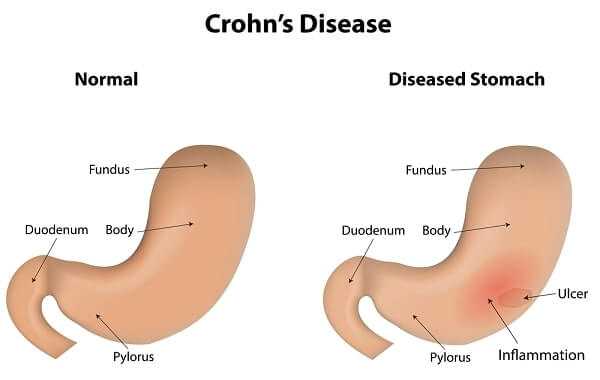
Numerous researchers have tried to show that IBD is an “autoimmune” disease, meaning that the disease occurs because the body attacks itself. Multiple abnormalities of the immune system have in fact been detected in people with IBD, but many researchers think these abnormalities are a result of the disease, not the cause. Even if these abnormalities perpetuate the disease, the factor that set off the disease in the first place remains the vital unknown.
What about Stress?
The issue of stress and the gut is an important one. Many people in the general population (i.e., people who do not have IBD) have gastrointestinal problems when they are under stress, and this has led to an assumption that stress has a role to play in IBD as well. The condition known as irritable bowel syndrome (IBS) is a disorder in which people tend to have abdominal pain and irregular bowel movements without any intestinal inflammation. Many people with IBS have a considerable increase in their symptoms when they are mentally stressed. Everyone is familiar with the term “tension headaches,” and people are not embarrassed to talk about them. But you don’t hear a lot of people talking about their “tension vomiting” or “tension diarrhea” or “tension bellyaches,” although these are every bit as common. As with tension headaches, tension gut symptoms can occur in any pattern, from occasionally to daily.
Doctors used to think that IBD was caused by stress. There is no evidence for this, and it is no longer believed by experts in the field. Controversy still exists, however, about the possible role of stress as a precipitating factor in flare-ups in a person with pre-existing IBD. Even if stress is a factor, it generally cannot be avoided, and the thought that a particular stress may cause a flare-up of the disease is in itself stressful.
People with IBD can also have IBS, and no doubt the occurrence of both conditions in the same person helps to perpetuate the idea that stress causes IBD. The experienced doctor and the experienced IBD patient know that IBD can begin when things are going well or when they are going badly. Saying that IBD is a psychological illness suggests that, because of the kind of person you are, you are in some way responsible for the disease. This is likely to make you feel guilty, which can make you feel even worse. Remember, it’s not your fault!





