Giant Cell Arteritis (GCA)
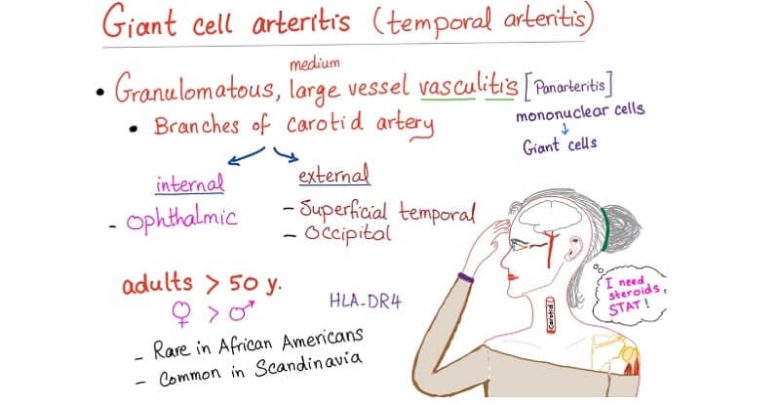
There’s a far more serious condition associated with Polymyalgia Rheumatica (PMR). In a typical study Dr. Gene Hunder conducted, 15 to 20 per cent of patients with PMR had a condition called giant cell or temporal arteritis; about 50 per cent of patients with GCA also have Polymyalgia Rheumatica. It affects the external carotid artery in and around the head and scalp, occasionally the branches of the arch of the aorta, and sometimes the bigger abdominal arteries. The walls of the arteries thicken and narrow, allowing clots to form or ruptures of the arterial wall, occasionally causing a stroke or heart attack.

The most characteristic effect, though, is clotting in the vessels supplying the retina of the eye, causing sudden and permanent blindness. At one time, says Hunder, “up to 50 per cent of patients with GCA became blind. Nowadays, it’s more like 10 per cent. That’s still scary, and it means that physicians should be aware and start treatment early, because prednisone will prevent blindness in most patients.”
Patients with Polymyalgia Rheumatica (PMR), though, should be their own first line of defence against GCA. Headache is the most important sign, says Dr. Bevra Hahn: “Headaches, visual symptoms, pain in the jaw while chewing, or very tender scalp—these are clues to inflamed blood vessels in the cranium. [Prednisone] doesn’t cause any of those symptoms, so it’s almost certainly the disease. Fortunately, most of the time you have time to get to the doctor and change your medicine.”
Despite the potential hazards, patients with PMR should feel optimistic, says Hunder. “PMR is diagnosable. We don’t understand it completely, but it’s treatable, and, if carefully followed, the side effects to prednisone can be minimized in most patients. The eventual outlook is good. They should recover.”






This is a really good article, I actually started with GCA first (biopsy positive) over 2 years ago, recently I have been diagnosed with PMR and was told by my Rheumatologist that because I’ve been on preds for so long and almost was able to finish them, they have already helped. I am still on course to finish but on a much slower taper.