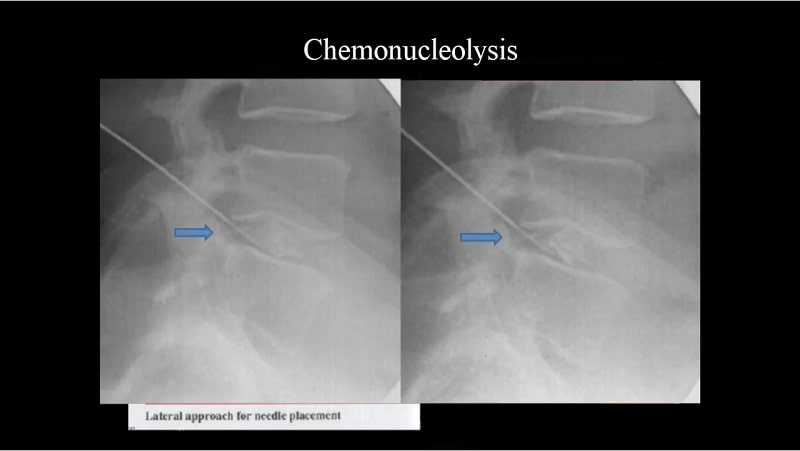
Is surgery necessary for spinal stenosis?

Spinal stenosis refers to an abnormality in a section of the body. The human bone channel is occupied by many spinal nerves, and as people age, they eventually experience pain, weakness, or numbness in their spine. Some people are born with a congenital form, but most tend to develop this condition later in life and turn to spinal stenosis surgery.
Let’s take a look at the symptoms first.
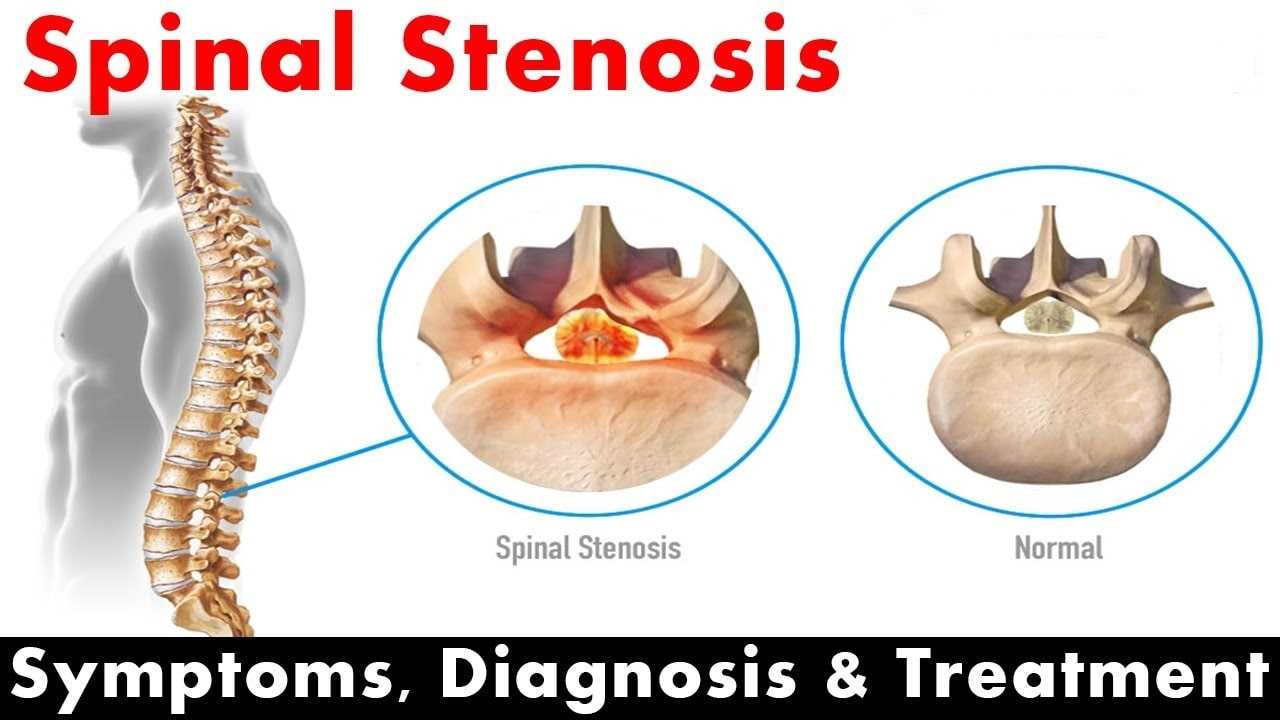
Spinal Stenosis Symptoms
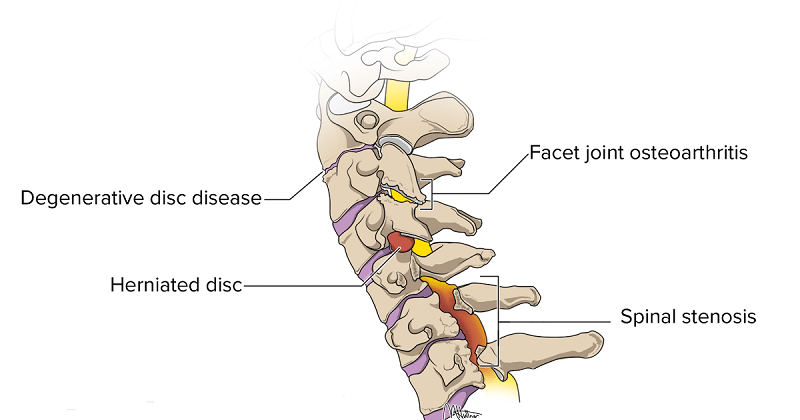
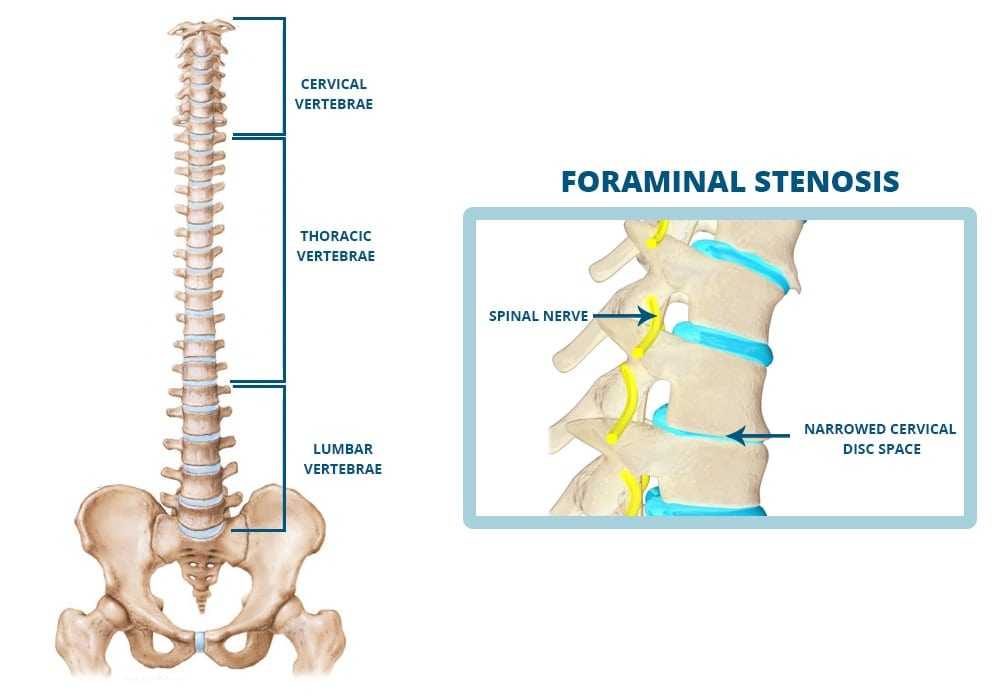
Spinal stenosis is defined as an abnormal narrowing of the bone channel within the spine that houses large numbers of nerves and the spinal cord itself. Although it is possible to be born with a congenital defect that will cause this condition, the majority of cases develop as a result of degenerative issues over time. There are two main types of spinal stenosis. Lumbar spinal stenosis affects the vertebrates of the lower and middle back. Cervical spinal stenosis impacts the vertebrates located in the neck. The latter type can be more severe and invasive treatments could be required in order to avoid very serious complications. Let us take a look at some of the primary symptoms of spinal stenosis.
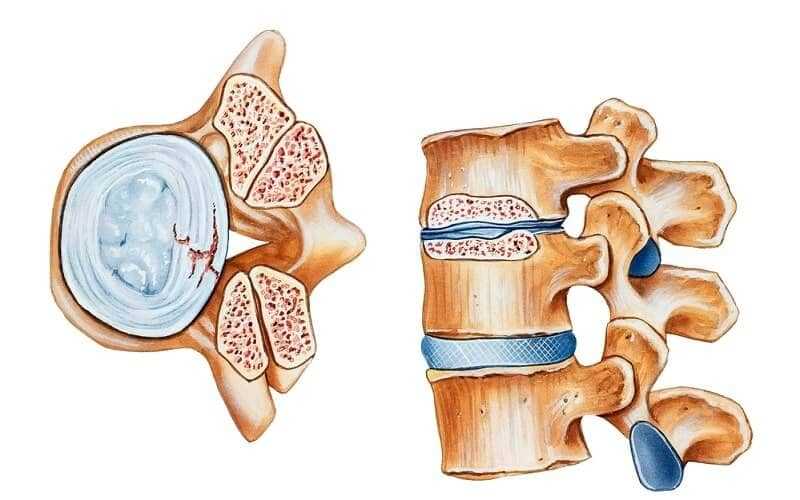
Main Symptoms
As mentioned previously, there are two different types of spinal stenosis. It therefore stands to reason that the symptoms can very depending upon where the spinal canal has narrowed. Nonetheless, a host of symptoms which tend to be common with either type can include:
- Symptoms which develop over time as opposed to presenting themselves acutely.
- Pain which increases and then subsides.
- Pain that occurs during specific activities (such as walking or tilting the head in an upward fashion).
- Pain that is relieved with physical rest.
Now that we can appreciate some of the symptoms that may be common with both types, let us examine the discrete indicators for both cervical and lumbar stenosis in greater detail.
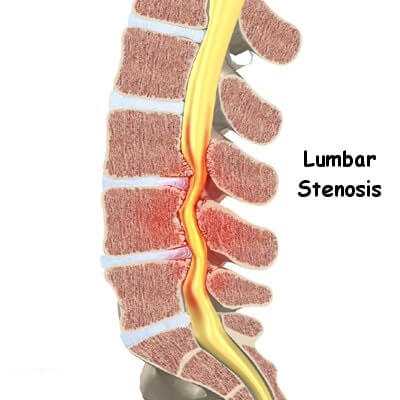
Lumbar Spinal Stenosis Symptoms
The most predominant symptom of lumbar spinal stenosis is pronounced leg pain (referred to medically as claudication). This pain may be dull or may feel as if it is sharply radiating down from one side of the spine. Sciatica is often a feature, as a compression of the spinal nerve root in the lower back could be present. Numbness and/or tingling can also occur in intervals along with pain.
In the majority of cases, this pain will cease after the patient stops walking and sits down. It is interesting to note here that a condition known as vascular claudication can appear to be quite similar. The primary difference is that any pain is relieved immediately. Another indicator that lumbar spinal stenosis may be present is if the patient finds relief when bending over. This will help to open up the spinal canal. However, pain will once again return when standing in the upright position.
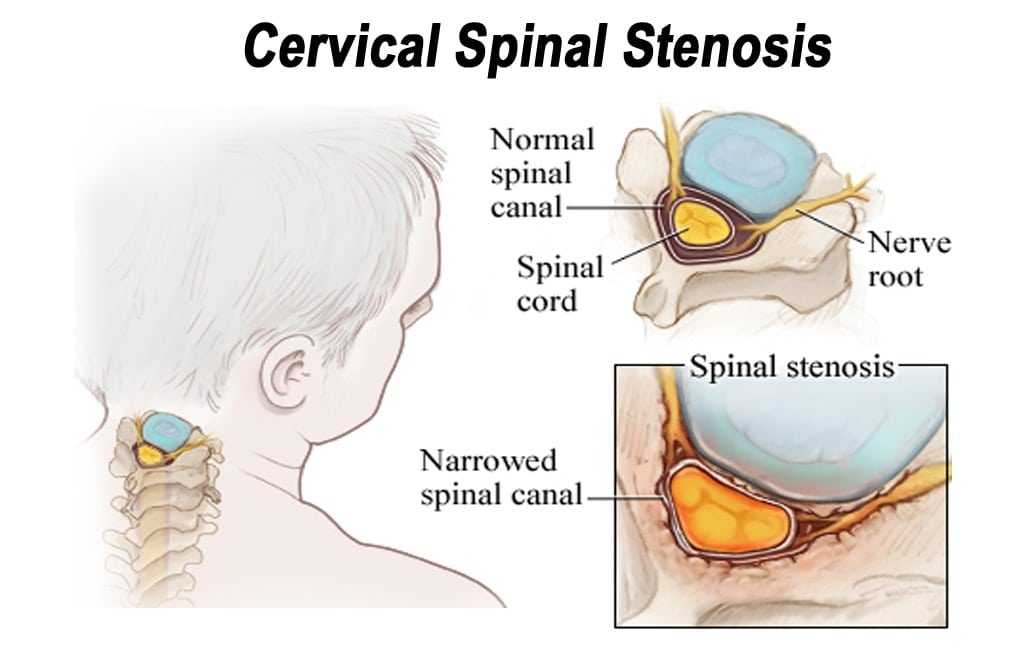
Cervical Spinal Stenosis Symptoms
As opposed to lumbar spinal stenosis, cervical stenosis is associated with a relatively different set of symptoms. Once again, these tend to occur gradually as opposed to immediately. The most predominant include (but may not be limited to):
- Numbness or pain in the neck, arms, legs or shoulders.
- Incontinence (loss of bowel or bladder control).
- Issues with walking and general coordination problems (such as tripping or a lack of balance).
The major difference with cervical spinal stenosis is that if the condition becomes too severe, paralysis can be the end result. This is why it is critical to seek the diagnosis of a trained professional if any of these symptoms occur.
Confusion with Other Conditions
There are times when the symptoms of spinal stenosis can be confused with other diseases and illnesses. For example, cervical stenosis may be misinterpreted as a herniated disc in the neck or peripheral arterial disease. Nervous system illnesses such as multiple sclerosis may also mimic cervical stenosis. Finally, other issues such as a deficiency of vitamin B12 or even a tumour may be causal factors.
Lumbar stenosis may be misdiagnosed as infections or tumours in the lower back area, changes in the nervous system such as those (once again) caused by multiple sclerosis, an abdominal aortic aneurysm or simple lower back pain due to a sudden injury.
As we can see, the symptoms of spinal stenosis can vary widely depending upon where the narrowing of the spinal canal occurs. As the condition can also be confused with other potentially serious situations, it is critical to seek the advice of a medical professional as soon as possible.
Treatment for Spinal Stenosis
Spinal stenosis is an ailment that develops gradually as we get older. It usually occurs after the age of 50, but in some cases, younger individuals can be diagnosed with scoliosis that may lead to spinal stenosis. In majority of cases, this condition occurs in the lumbar spine. Slipped or misaligned vertebrae can be the cause of spinal stenosis and the most common symptom is aching in the calves. Once this condition progresses further, the patient will find it increasingly difficult to walk or stand due to the extreme pain on their leg.
There are many different types of treatment for spinal stenosis, depending on its exact location and severity. Before you consider your treatment options, your doctor may prescribe medications to control your pain. Such medications include non-steroidal anti-inflammatory drugs to reduce inflammation. To calm muscle spasms, muscle relaxants such as Amrix and Fexmid can also help ease chronic pain.
Medications are only a temporary solution to chronic pain. In an effort to reduce your spinal discomfort, you should consider seeing a physical therapist. This professional can teach you many exercises that help build endurance and maintain your flexibility. By attending two or three sessions a week, you can help ease your symptoms.
There are also many non-surgical options for patients suffering from spinal stenosis. Some of these treatments are explained below:
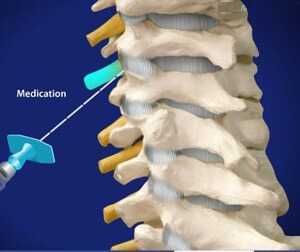
Epidural nerve block
This corticosteroid injection is applied into the space located between the nerve roots and the dura. After the doctor has applied some local skin anesthetic to the subject area, a special spinal needle is then inserted into the space in order to reduce the swelling around the nerve roots. For utmost accuracy, the physician performs this procedure under x-ray. You will typically need up to 3 injections within a 6-month time frame to feel completely relieved from pressure and pain.
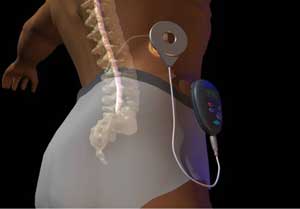
SCS (Spinal Cord Stimulation)
This treatment is an innovative technology that targets the most difficult-to-reach spinal area. Most chiropractors and doctors have identified SCS as an effective treatment option for chronic sufferers and it’s also used for diabetic patients or those suffering from neuropathic pain. To seek relief, you should refer to a qualified pain specialist who can determine the length of the treatment sessions. Some patients may need to undergo SCS treatment for a few days or at most, 1 week. During your first session, the practitioner will know how well you have responded to stimulation and can advise on whether you will need further treatments or not.
MILD
This safe and effective treatment is an outpatient procedure that’s performed in less than one hour. Many patients who have undergone MILD treatment have been able to stand longer and walk farther as they experienced significantly less discomfort. MILD is an FDA-approved procedure that involves the use of specialised tools inserted in your back through a very small incision. The small pieces of excess bones that cause obstruction in the spinal canal are removed with the help of an imaging device to guide the doctor through the entire procedure. This treatment will decrease the compression of the nerves and restores the spinal canal’s space so that the patient can walk or stand without feeling any pain.
Radiofrequency
This procedure is a long-term solution for pain relief. It is only performed when the exact facet joints have been fully identified as the sources of discomfort. These joints are located between each vertebra and provide stability to the spine. Once they become inflamed or irritated, facet syndrome can occur. Radiofrequency neurotomy uses thermal denervation to interrupt the sensory nerve. The doctor carries out this procedure through a local skin anesthetic. After the needles are placed in the correct position, the doctor applies thermal energy to deaden the nerve. This procedure is performed within half an hour on an outpatient basis. It is then followed by a further half an hour of recovery time.
Diagnosis of Spinal Stenosis
The symptoms of this condition tend to develop slowly over time. The pain that you experience in your spine area comes and goes, or it can occur during physical activities such as walking, cycling, or heavy lifting. You may also feel leg pain whenever you’re standing in an upright position. This can be due to lack of arterial circulation but the pain will soon subside when you sit down for a few minutes to rest your leg.
If your doctor has diagnosed your condition as lumbar stenosis, then you should flex your legs forward to open up the spinal canal and relieve your leg pain. The most common symptom that patients experience is numbness whenever they get back into an upright posture.
Spinal Stenosis Surgery
To minimise the pain and protect the surrounding tissues, most doctors advise patients to undergo spinal stenosis surgery. The surgeon tries to preserve the ligaments in an attempt to reduce the chance of developing adjacent-level degeneration in the future. Thanks to the advancement of medicine, spinal stenosis surgery has now more of a successful outcome than before; however, just like any other type of surgery, it’s not without risks.
The outcomes for spinal stenosis surgery have been most rewarding thanks to the latest surgical methods used on the spine. Decompressive laminectomy is one such surgery that treats low back pain. This procedure is carried out on the spinal nerve roots to relieve herniated discs, spinal injuries, and other related conditions. Patients generally recover quickly after decompression surgery and are able to increase their physical activity upon recovery. Some patients experience a better walking tolerance soon after recovering from their spinal stenosis surgery. This is due to pressure reduction on the nerve roots, which allows you to resume your normal daily activities.
There are also many other specialised techniques that can be used on the spine, although the actual procedure remains the same. These techniques depend on what types of metal implants are used and whether they are placed on the back or front of the body. Before you undergo surgery, your age, health condition, and the severity of your symptoms are assessed by the surgeon before he or she advises you on the most suitable course of treatment.
What to expect after surgery?
Depending on your state of health and the type of surgery you underwent, it can take up to 1 month or more before you’re able to return to your normal activities.
Why should you consider spinal stenosis surgery?
Patients who experience severe symptoms should consider surgery, especially if their symptoms restrict their normal day-to-day activities. Although non-operative treatments relieve pain, the effects are only temporary. If you find that you can no longer control your bladder or notice sudden changes in your walking ability, you should consider opting for surgery.
Imaging test results alone should not be the main deciding factor for having surgery. Even if your test results show increased pressure on spinal nerve roots, your walking ability and severity of your symptoms are the main deciding factors. In some cases, the surgeon may advise spinal infusion as the most stabilising option. This procedure will make it easier for the patient to move around and suffer from less pain. Spinal infusion also helps keep the bones in a healthy position without pressurising the spinal canal and the surrounding nerve roots.
What are the risks associated with spinal stenosis surgery?
Every surgery has its own risks and complications, especially when combined with other existing medical problems and the severity of the spinal pain. These risks may be higher in older adult patients. The possible complications can be anything from surgical wound infection, blood clots, anaesthesia problems, to nerve injury and paralysis.
Some patients may also have trouble passing urine shortly after their surgery, and in more severe cases, the fibrous tissue that covers the nerve near the spine can tear and require a second surgery. In some cases, chronic pain can develop right after the operation.
Before you decide to have surgery, make sure you discuss this with an experienced surgeon who can give you detailed information about the pros and cons of spinal stenosis surgery. Bear in mind that approximately 80 per cent of patients who undergo this type of surgery have significant improvement in their function.