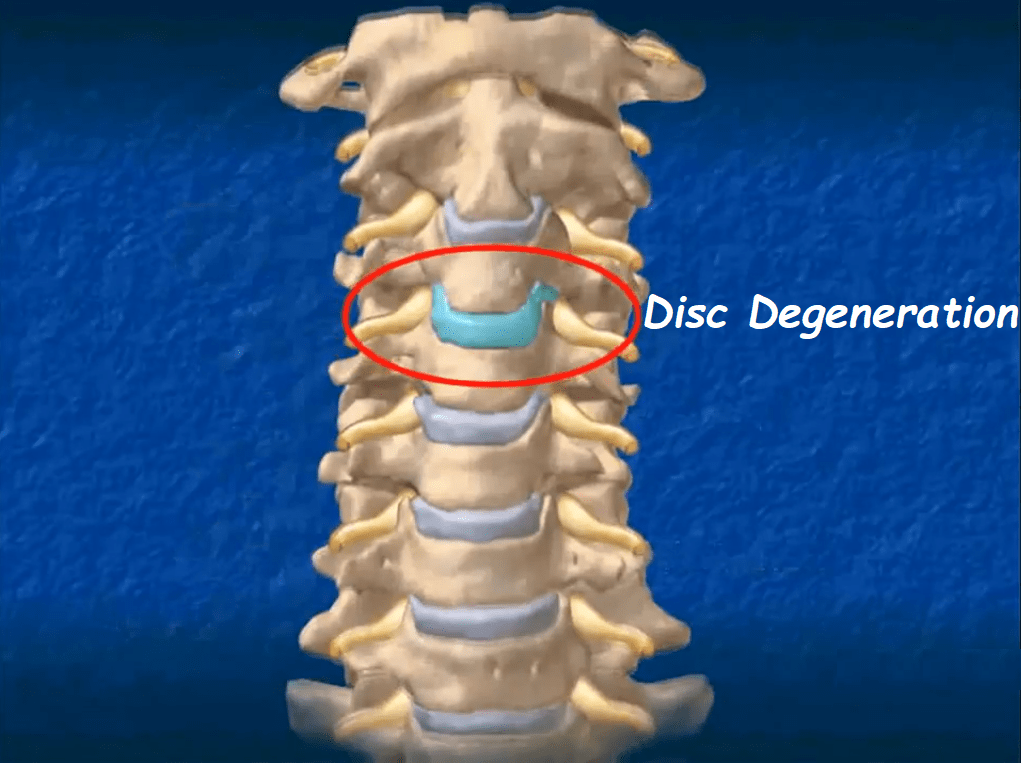
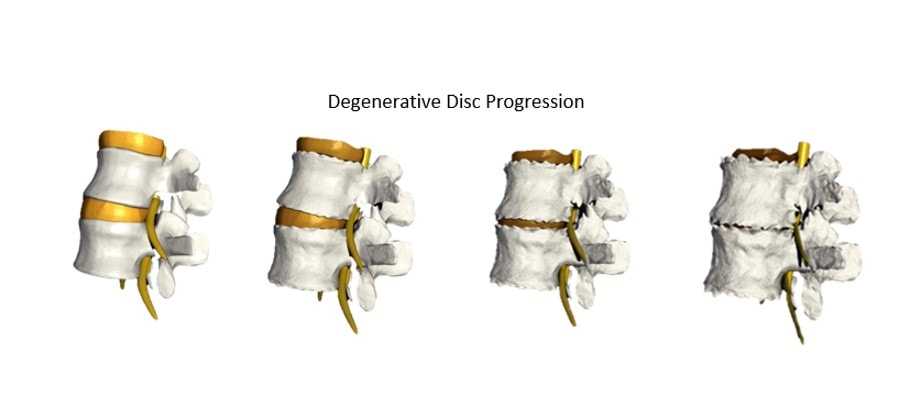
Lumbar Degenerative Disc Disease & Lumbar Spondylosis
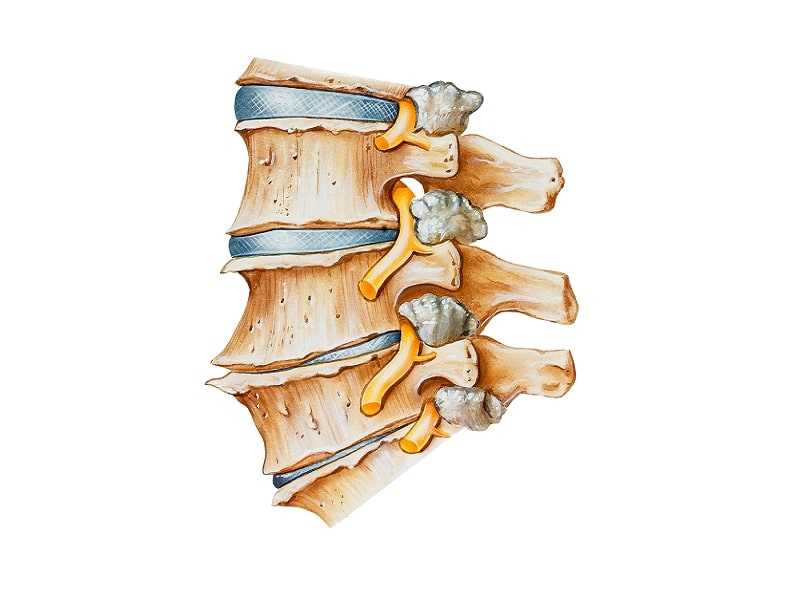
Clinical Presentation
Lumbar degenerative disc disease has no single, unifying presentation. A typical symptomatic patient has a clinical course of repeated bouts of low back pain, followed by long periods of pain relief. In this case scenario, a patient may describe a 10- or 20-year history in which he develops bouts of moderately severe low back pain, occurring once or twice yearly, sometimes severe enough to leave him bed bound, from which he gradually recovers to resume full activity. These bouts of pain may or may not be associated with radiating leg pain. The patient often is unaware of any particular inciting event to pain.

Although this may remain the pattern indefinitely, if the degenerative disc changes progress, then the patient can develop increasing symptoms. In some cases, a patient notes considerable morning stiffness or even severe pain on first standing in the morning. The morning pain may persist for a period of 30 to 60 minutes, until after he has fully showered and done some basic stretching exercises. Then, during the day, the patient feels relatively well. He may note that prolonged sitting, especially prolonged sitting in a car, is associated with an increase in symptoms, and getting in and out of the car may be particularly painful.

Morning stiffness and frequent bouts of pain also can be interspersed with more severe attacks of pain. This can manifest as a sudden, severe sense as if the back is locked; the patient becomes pitched forward or tilted to the side. If lumbar degenerative disc changes progress, then the patient may develop a pattern of more daily, situational pain, and may even develop a pattern of lumbar stenosis, which is described in this article.
The recurrence or increasing frequency of attacks generally leads a patient to seek medical help. This may be coupled with an increasing sense that the patient has become limited in certain activities, thereby diminishing quality of life.
Cause of Lumbar Degenerative Disc Disease
Degenerative disc disease primarily is caused by a genetically predetermined biochemical and metabolic alteration within the nucleus pulposus. The most notable changes occur between the ages of 30 and 50. Water content gradually diminishes as a result of the biochemical and metabolic shift, and the resultant drier and stiffer nucleus pulposus leads to fissures (tears). As a result, the entire disc complex begins to degenerate.
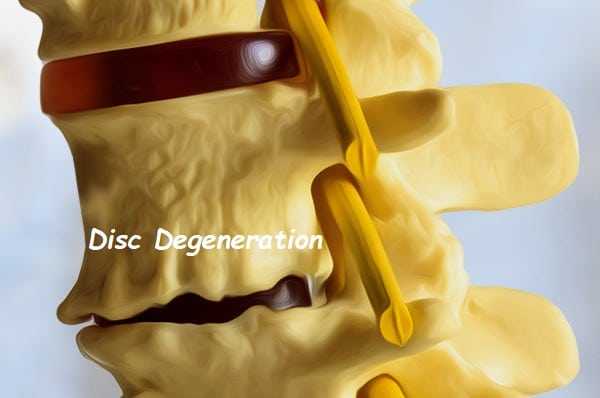
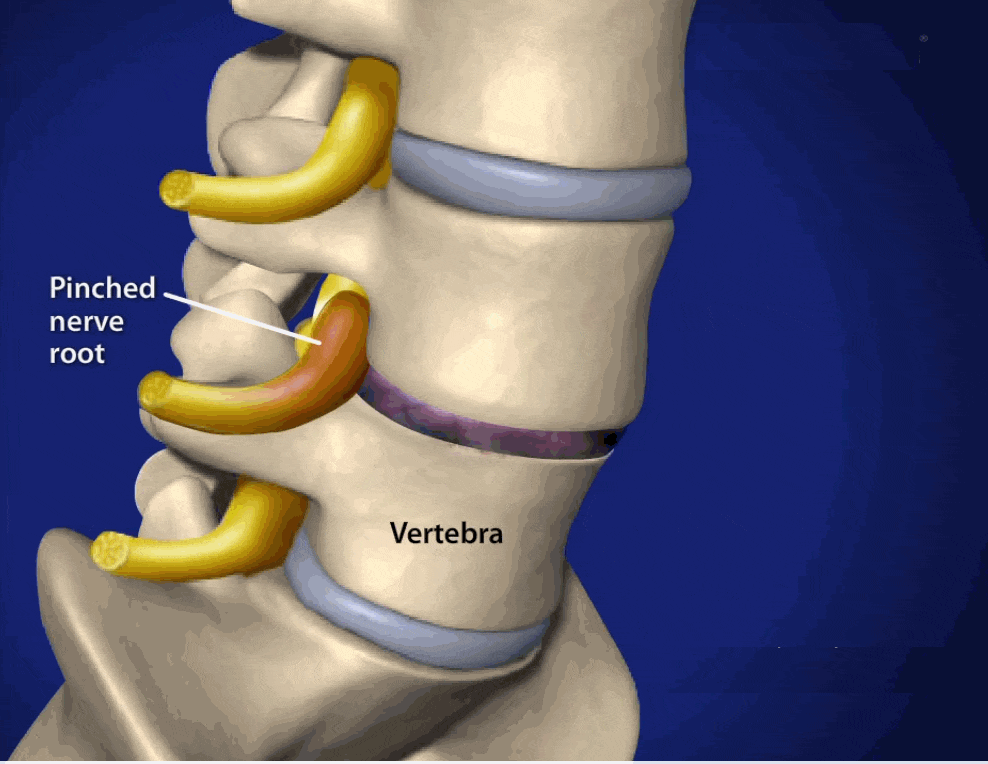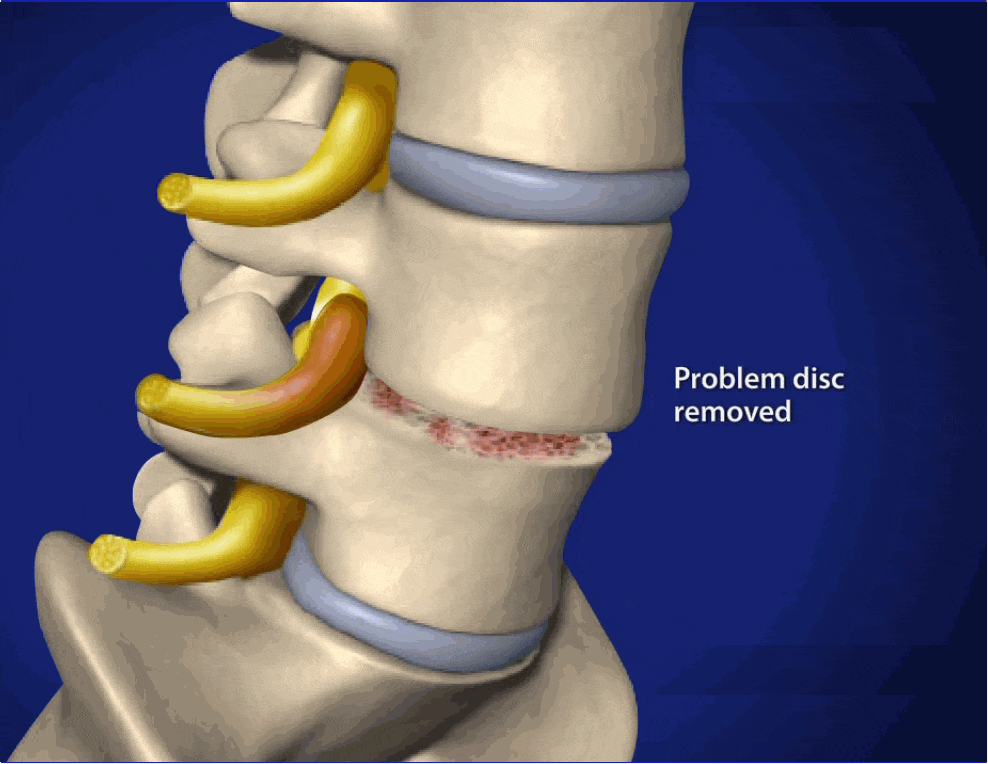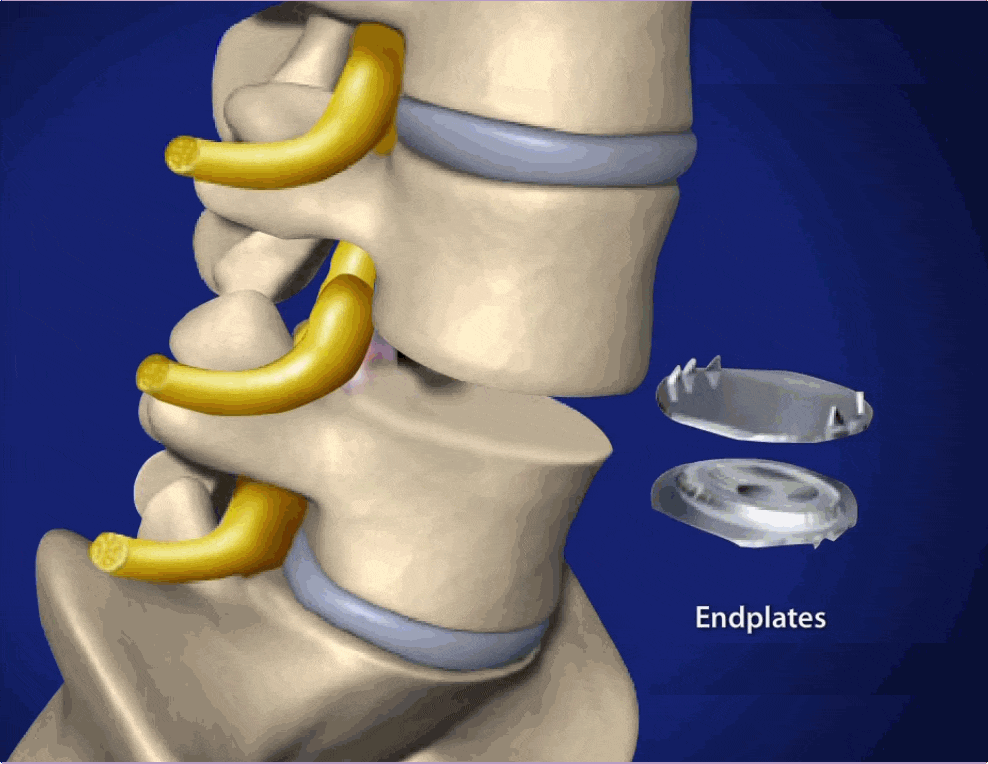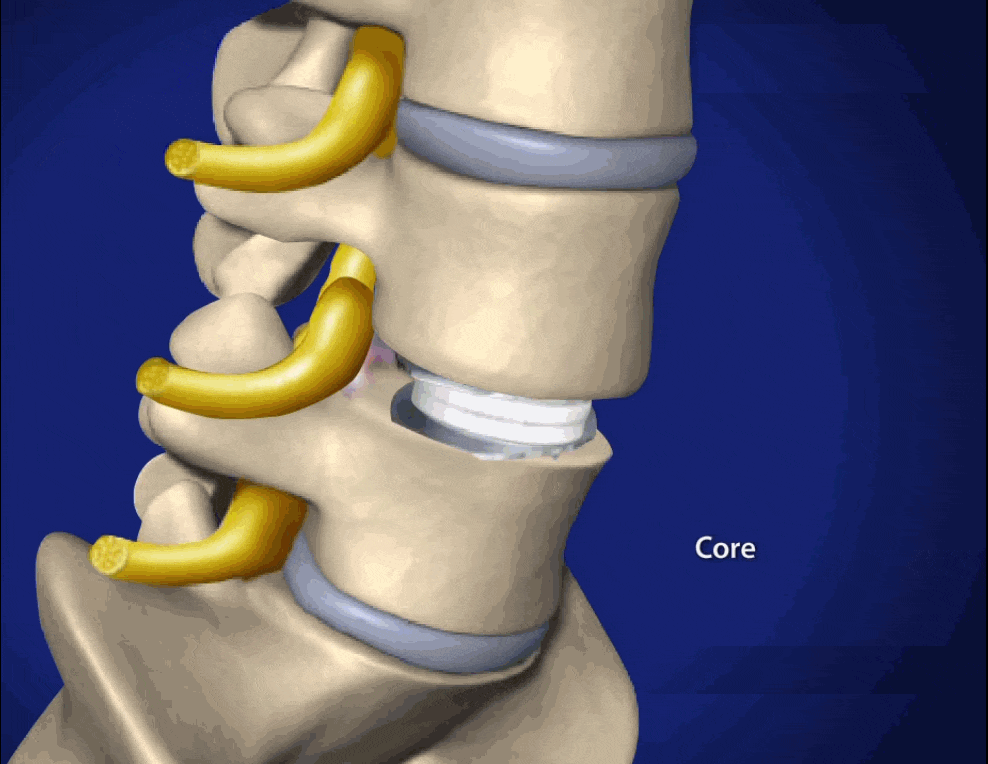
The sudden bouts of pain, which can develop intermittently, may be related to a sudden shift in the dynamic stability of the spinal joint. One explanation may be that a larger tear develops within the annulus, associated with a disc herniation. This ultimately resolves without more specific treatment. Another possibility is that, as the disc loses its water content, the vertebral bodies approach each other, and the facet joints assume a more weight-bearing role (Image 1). In this setting, the facet joints can suddenly become locked or irritated, causing sudden, severe, low back pain.
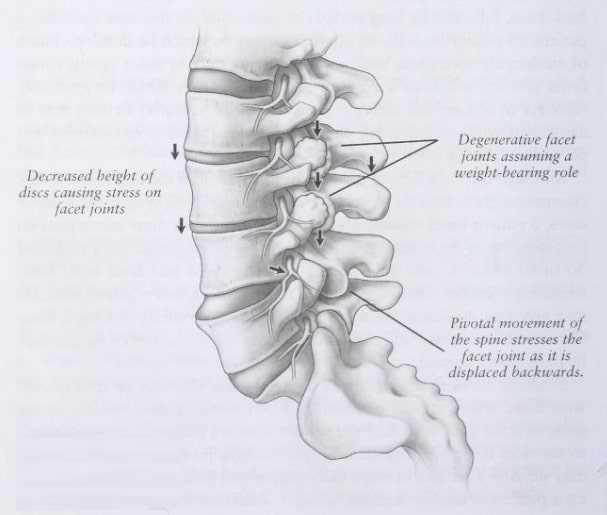
Another possibility is that, in the setting of degenerative disc changes, the spinal joint complex can become somewhat unstable and sudden, minor shifts can lead to irritation of pain-sensitive structures as well. When the lumbar disc is degenerative, the lumbar spine segments lose some stability. This means that bending forward or backward can be associated with abnormal movement of the lumbar vertebrae. The vertebrae may either rock back and forth or slide forward and backward (pivotal movement). In either case, pain-sensitive structures can become irritated. Lumbar degenerative disc disease also can be associated with spondylolisthesis, which is a fixed slippage of one vertebrae over another (Image 2). This condition not only is associated with facet jamming, but may also lead to nerve compromise and spinal instability (See here for details).
More progressive symptoms of degenerative disc changes are generally the result of minor instability of the lumbar spine coupled with facet irritation. The spine is no longer moving in a properly coordinated manner; in addition, the facet joints are becoming irritated because they are supporting the weight of the spine rather than acting as smooth, gliding joints. In addition, the lumbar musculature is generally poorly developed and cannot compensate for the lack of stabilizing forces of the lumbar disc. This cascade of events causes the patient to develop progressive symptoms.
Physical Examination
Patients with degenerative disc disease may reveal restriction of lumbar spinal flexion and extension. They also may develop pain at extremes of flexion and extension. Straightleg raising maneuvers are generally unremarkable. A flattening of the normal lumbar curvature may be noted, secondary to prolonged maladaptive changes in the spinal segment and the spinal musculature. The neurologic exam is unremarkable.
Imaging and Diagnostics Studies
Plain radiographs of the lumbar spine reveal evidence of degenerative changes. The space between the disc may be narrowed and evidence of calcium deposits or osteophytes may be seen, which are the natural result of long-term, degenerative changes.
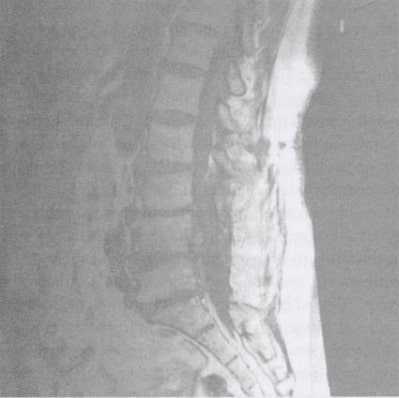
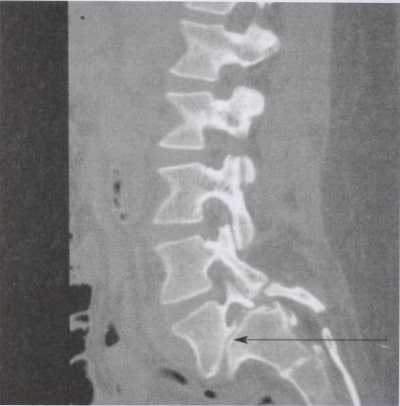
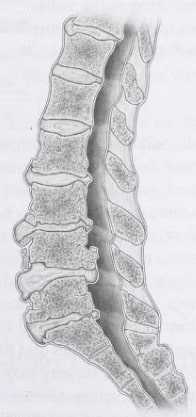
Magnetic resonance imaging (MRI) will reveal evidence of loss of water content of the disc, and associated degenerative changes will be noted in the facet joints (Image 3). Some narrowing of the spinal canal may be present, and there may be protruded disc material, which has become calcified over time. There may even be asymptomatic compression of nerve roots or evidence of spinal canal narrowing in the form of spinal | stenosis (Image 4). A computed tomography (CT) scan of the lumbar spine will reveal similar changes and | may be more useful if greater detail is required for analysis of the facet joint. Electromyography (EMG) and nerve conduction studies usually are not required, unless associated leg numbness or weakness is present. Occasionally, a bone scan is ordered as part of a general work-up for patients who have developed low back pain. A bone scan will reveal evidence of degenerative changes.
Treatment Considerations
Nonsurgical
In most cases, lumbar degenerative disc disease can be treated non-surgically. For acute exacerbations of pain, treatment with nonsteroidal anti-inflammatory drugs (NSAIDs) is appropriate. Such treatments generally last for 1 to 2 weeks. For a severe bout of pain, an oral course of corticosteroids may be indicated. Muscle relaxants may be helpful. Narcotic analgesics may be utilized to help with bouts of severe pain.
Spinal manipulation and acupuncture may be helpful for acute bouts of pain, but for the long term, the focus should be on manual physical therapy techniques and spine stabilization. In essence, patients generally develop a cascade of degenerative disc changes and muscular maladaptation; therapy must address the muscle imbalance and muscle weakness, then progress to spine stabilization. This is an attempt to allow the supporting musculature of the spine to help stabilize spinal movement.
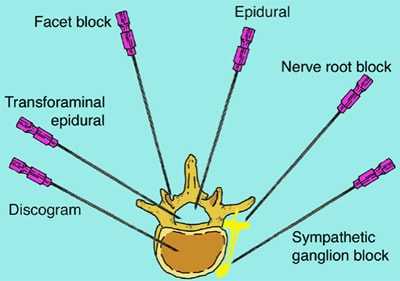
In some cases, injections are indicated and can provide substantial relief. Patients may have prolonged back pain as a result of facet jamming or facet irritation and, a facet block may alleviate symptoms. Facet injections can be followed up by physical therapy. In some cases, degenerative disc disease is associated with partial herniation of disc material, with associated compression of the nerve route. A lumbar epidural corticosteroid injection or selective nerve root injection can help to alleviate symptoms. In all cases of therapeutic injections, treatment should be followed by a progressive course of physical therapy, as tolerated.
Related Article
Spinal Injections For Back Pain
Surgical
Unless degenerative disc changes have progressed to the point of severe spinal stenosis (discussed in this article), or unless an associated neurologic compromise is present, most patients with lumbar degenerative disc disease can be managed nonsurgically. However, some patients develop multilevel degenerative changes and have associated spine instability. In this case, the spine will move repeatedly when the patient is in forward flexed or backward extended position, causing a sudden jamming or irritation of pain-sensitive structures. If nonsurgical measures and physical therapy have not led to substantial pain relief, and if a good clinical correlation exists between the degenerative changes and the type of back pain that one might expect from such changes, surgery may lead to beneficial results.
If lumbar degenerative disc disease is associated primarily with some degree of spinal instability, then surgery must consist either of lumbar disc replacement or spinal fusion. In cases of back pain from degenerative, faulty lumbar discs, laminectomy alone may render the spine even more unstable. The medical risks of surgery must be considered carefully.
The success of spinal surgery depends on both the surgeon and the patient. Some patients have chronic low back pain without any clear precipitating or palliative features to the pain, but show some degenerative changes on imaging studies. When surgery is performed on such patients, failure is likely.
In contrast, other patients have clear clinical evidence of spine instability from a faulty lumbar disc. Such patients frequently develop considerable pain with sudden positional changes, such as getting out of the bed in the morning, getting into and out of a car, or suddenly misstepping. They also can develop sudden pain with certain twisting and bending activities. Walking on level ground generally leads to pain relief in such patients. If a good clinical history of such pain exists, with associated advanced degenerative disc changes on imaging studies, then disc replacement or spinal fusion may well lead to a good clinical outcome.
The surgeon determines whether to perform lumbar disc replacement, posterior fusion, or circumferential fusion. In part, this decision is based on the surgeon’s experience with these procedures. The degree of spinal instability also influences the decision; patients with more severe instability will require spinal fusion.
Recovery from disc replacement surgery or spinal fusion surgery is more prolonged than it is from a simple laminectomy. The most prolonged recovery is from circumferential spinal fusion surgery. With any of these surgical techniques, patients may be required to wear a firm, plastic support brace for a period of 1 to 3 months following surgery. Physical therapy generally does not begin until at least 3 months following fusion, and it is extremely important to work with a skilled physical therapist. A modified program of spine stabilization should begin 3 to 6 months following surgery.
Mind-Body Considerations
For many patients, lumbar degenerative disc disease is simply a fact of life. Whenever we consider mind-body interactions, we consider our genetic predispositions, and both internal and external environmental influences can modify such predispositions. In the case of lumbar degenerative disc disease, there may be little one can do with regard to the development of lumbar degenerative changes. In some cases, these changes may progress to lumbar stenosis, regardless of any intervention. However, it is still worthwhile to take a mind-body approach in lumbar degenerative disc disease.
Frequently, patients develop bouts of severe pain in situations similar to lumbar strain and acute lumbar disc herniation. That is, the bouts of pain develop in the setting of physical or psychological imbalance. In addition, patients may develop maladaptive strategies from the fact that they are predisposed to developing lumbar degenerative changes. Sometimes a mind-body approach simply means that we understand that our body is moving in a certain direction, and we need to adapt accordingly. Mind-body does not mean mind over matter. Mind-body refers to a sense of mindfulness and mindful listening to the body.

Over the long term, many patients with lumbar degenerative disc disease respond favorably to a program of both spine stabilization and meditative exercises such as yoga, Pilates, or t’ai chi.
Summary Points
- Lumbar degenerative disc disease, also known as lumbar spondylosis, is primarily a genetically determined condition.
- Most patients with lumbar degenerative disc disease develop intermittent attacks of pain, followed by periods of complete pain remission.
- Most patients with lumbar degenerative disc disease can be managed nonsurgically. Such treatment should include a program of spine stabilization.
- Surgery is indicated for patients who develop spinal instability or progressive spinal stenosis.
- Lumbar degenerative disc disease does not necessarily cause low back pain; therefore, it is important to determine if low back pain is caused from degenerative discs or from another problem.