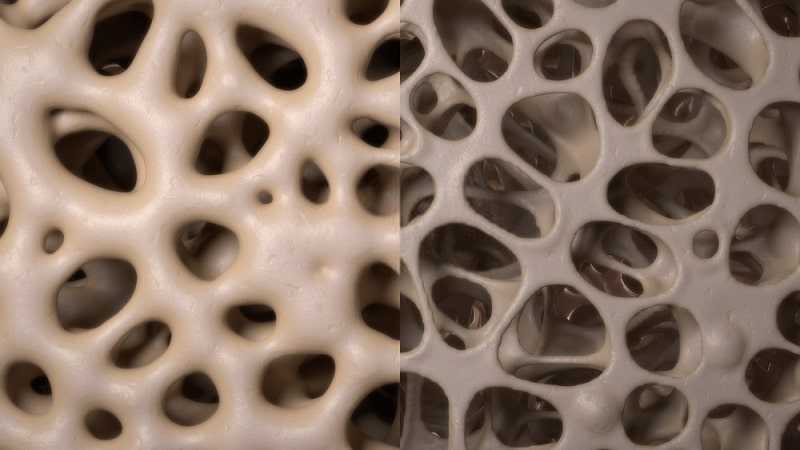
Osteoporosis – Understanding Aging

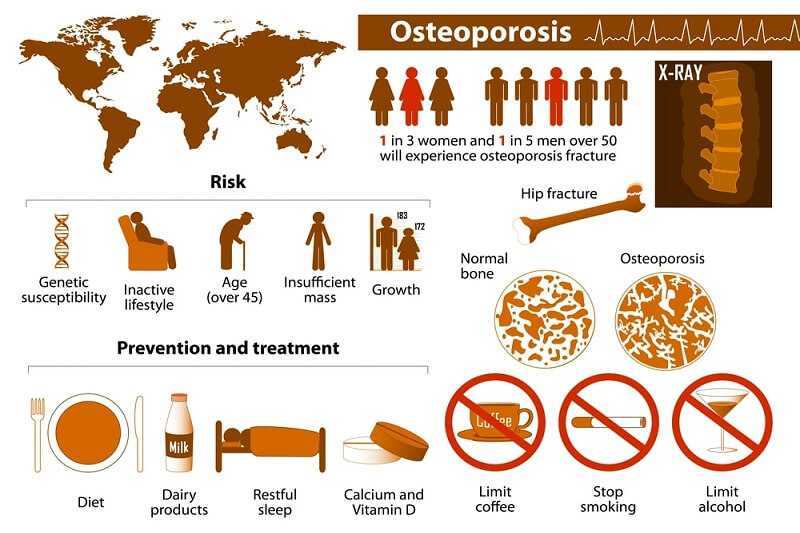
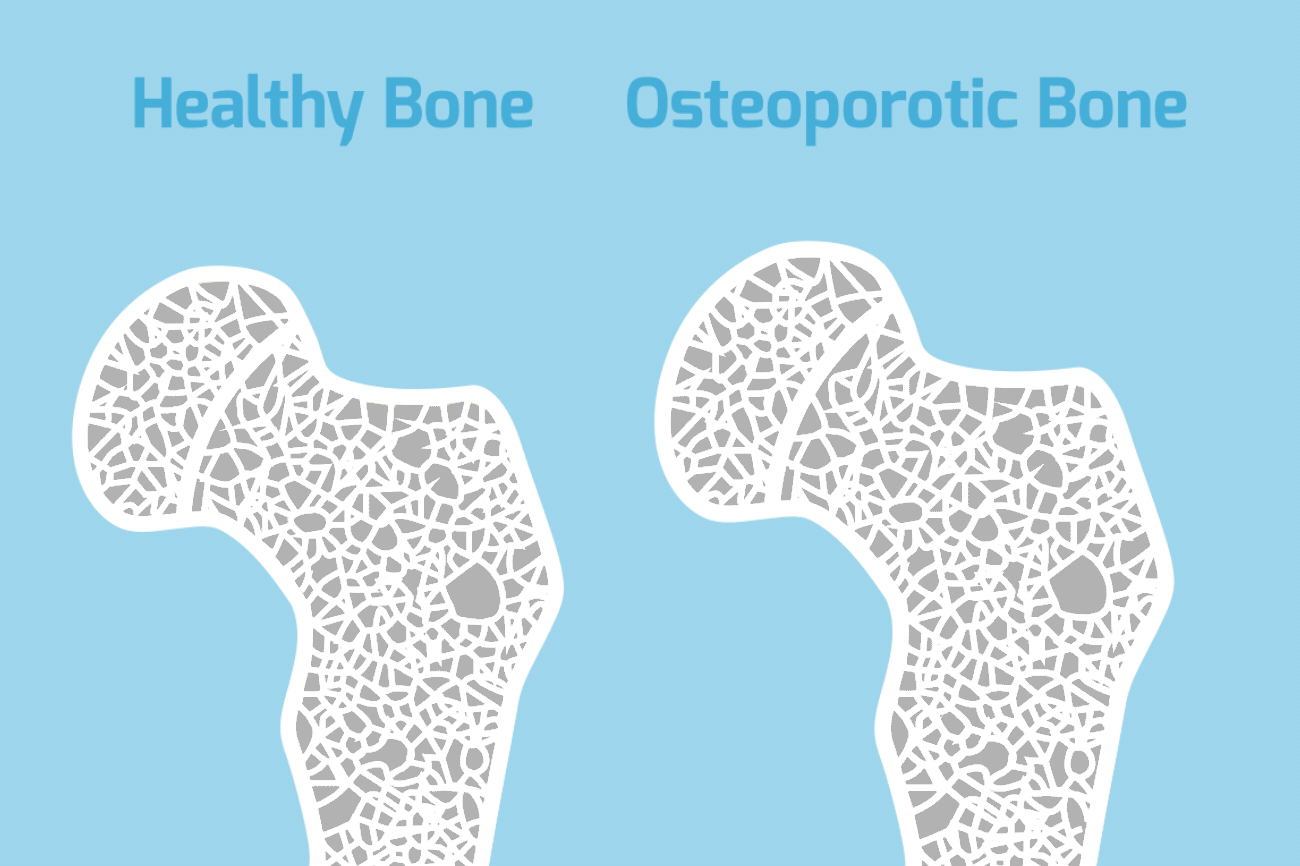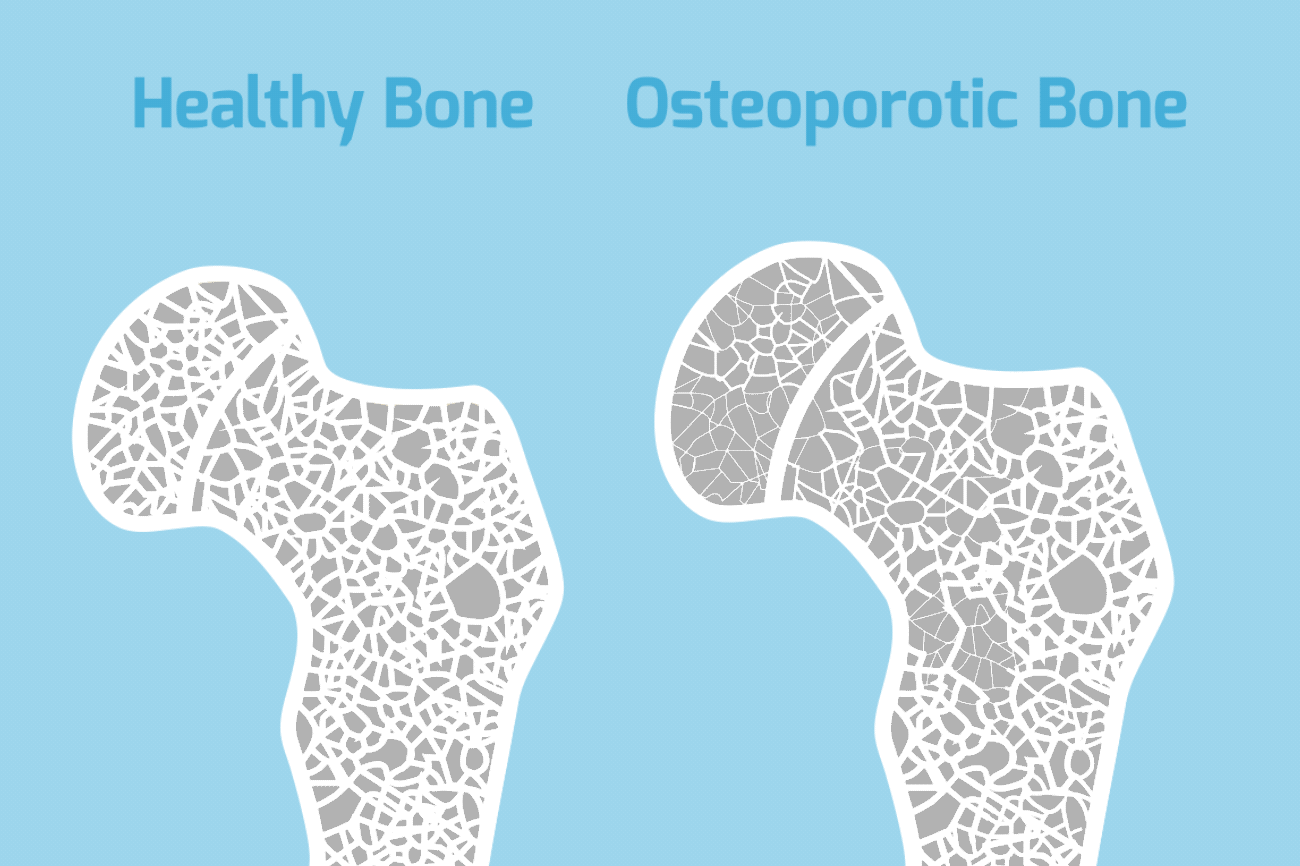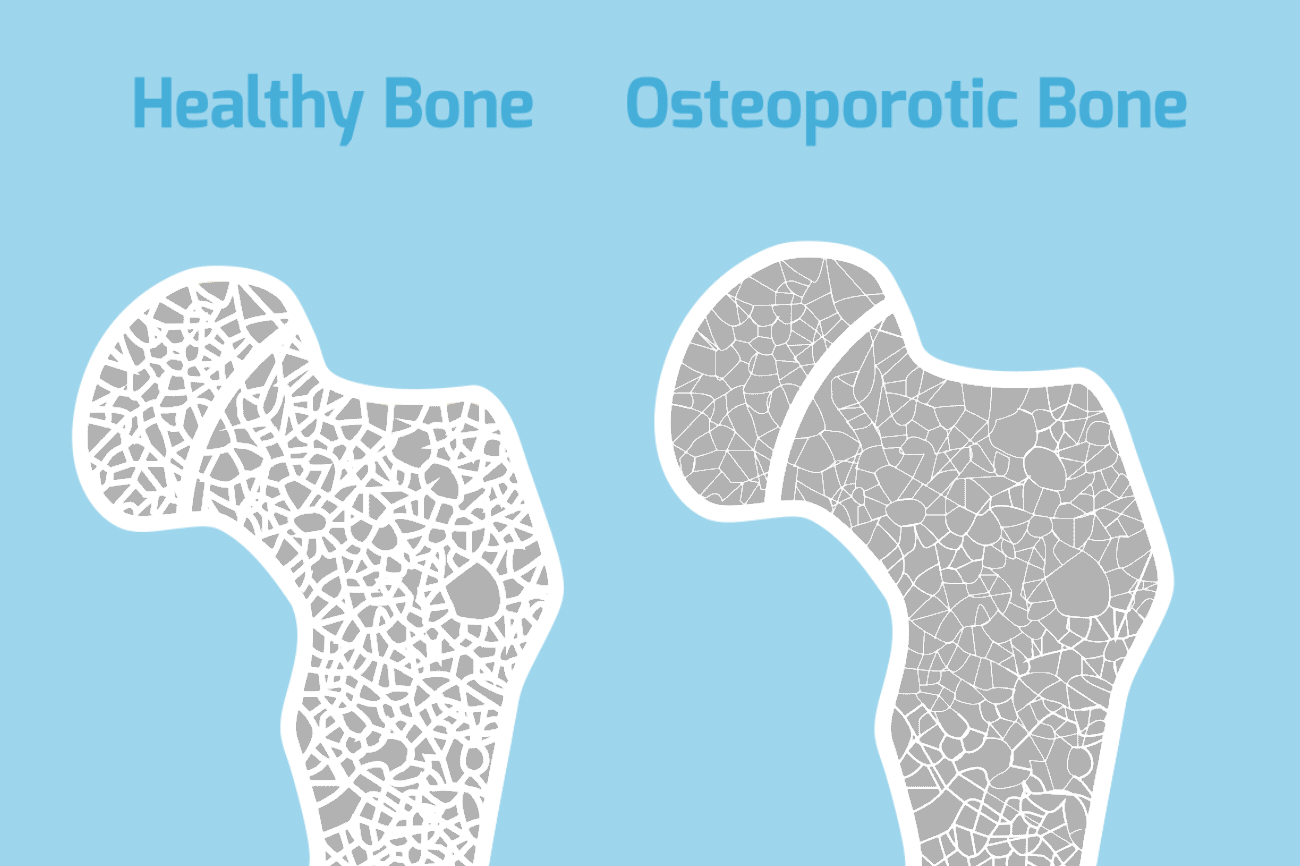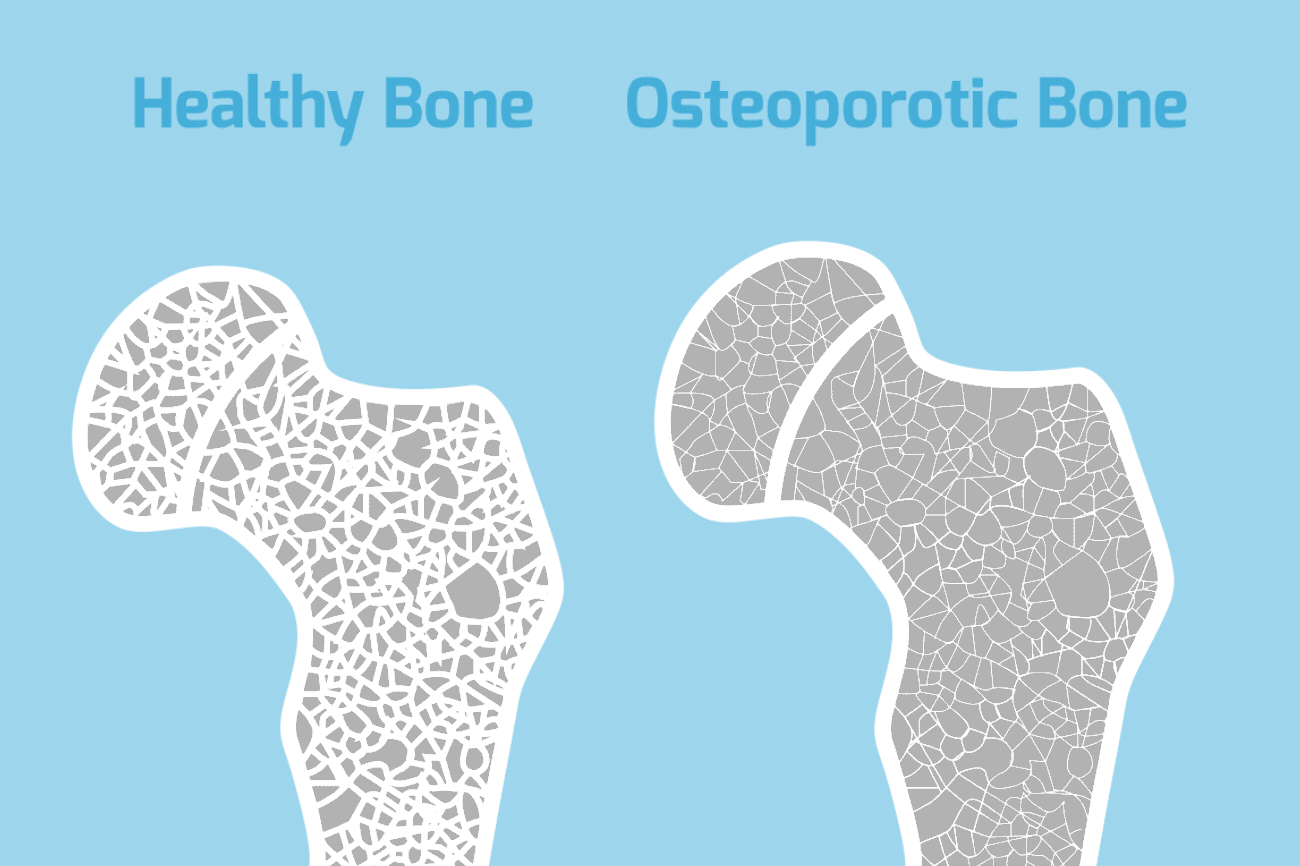
In osteoporosis, bones lose mass and density, becoming brittle, fragile, and more likely to break, even after a minor fall. Almost everyone’s bones become less dense as they get older because the body becomes less efficient at absorbing and using calcium, which is a vital component of bone. When a persons bone density falls below a certain level, they are said to have osteoporosis.
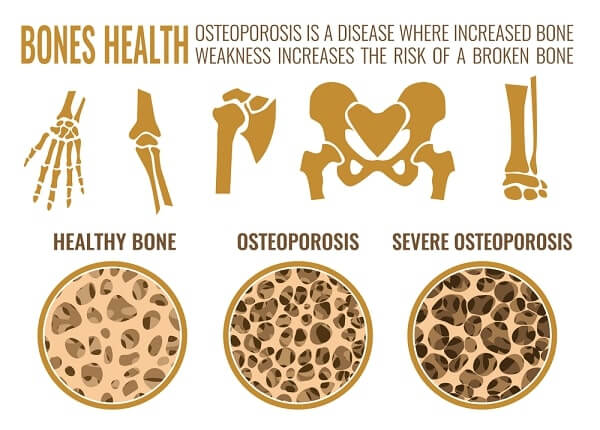
Understanding osteoporosis
A woman’s risk of osteoporosis increases dramatically during and after the menopause because the fall in estrogen levels during this time causes bone loss to accelerate; estrogen helps the body to absorb and use calcium. Men tend not to be affected until in their seventies. Taking oral corticosteroids, particularly for a long time, can also cause osteoporosis. Other risk factors include smoking, excessive alcohol and caffeine intake, a sedentary lifestyle, a diet low in calcium, low exposure to sunlight, family history, and being white or Asian. Osteoporosis is hard to detect and is usually discovered after a bone has broken. Reduced bone density can be screened using X- ray densiometry. Biochemical urine tests can be done, but they have limitations and are expensive. The bones most likely to be affected by osteoporosis are the spine, hip, and wrist bones. If left untreated, osteoporosis can lead to collapsing of the bones in the spine, which can cause pain, disability, and significant loss of height.
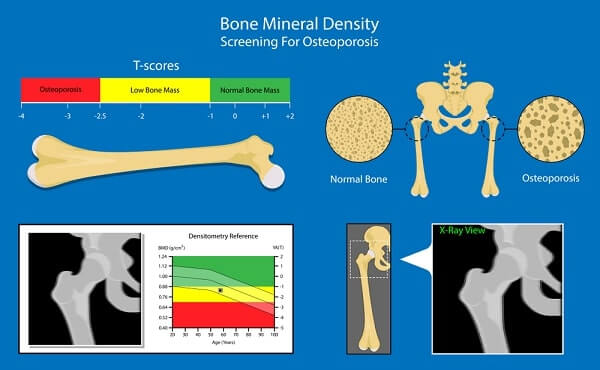
Preventing and treating osteoporosis

The best way to prevent osteoporosis is to make sure you have enough calcium and vitamin D in your diet. Dairy products like milk and cheese are an important source of calcium. Low-fat and nonfat milk and other low-fat dairy products are good choices because they are a good source of minerals and they are low in fat. Other good sources are tofu, sardines, watercress, dried figs, almonds, dried apricots, green leafy vegetables, and oatmeal. It may be a good idea for postmenopausal women to take a calcium supplement. Vitamin K, magnesium, boron, possibly silica, and other trace elements may also help. Sunlight is important, because the body needs it to make vitamin D, so older people who are housebound are at risk for osteoporosis because they rarely go outside. Weightbearing exercises (such as weight lifting, walking, and running) also increase bone density for as long as you keep doing them, so it is important to exercise regularly throughout your life.
In conventional medicine, osteoporosis is prevented and treated with drugs that increase bone mass. Hormone replacement therapy may be given—and it does treat osteoporosis—although there is no evidence that it lowers the incidence of fractures beyond age 60. Other drugs include raloxifene, calcitonin, and bisphosphonates such as alendronic acid.
Exercise is limited to how severe your condition is and how much pain you’re in. Don’t do too much too quickly, and stop if you feel any pain. People with severe osteoporosis should try to prevent falls and wear a hip protector, to reduce the risk of hip fractures after a fall.

Nutritional therapy advises eating foods high in calcium, little data exists on the effects of complementary therapies on osteoporosis. Herbs that may help include those rich in calcium (such as parsley, sesame seeds, nettle, horsetail, and dandelion leaf) and those that may have a hormonal action (such as sage, black cohosh, and wild yam).

Tai chi and yoga may help by increasing strength, flexibility, and balance, which may help prevent falls. It is claimed that homeopathic treatment can reduces bone loss, but this is unproven.