Pain Myths

Recent estimates in the U.S. are that over 100 million Americans suffer from chronic pain. The number of people with chronic pain exceeds the incidence of all other diseases combined. And yet, there are still many pain myths associated with chronic pain.
The latest reviews of medical school curricula show that chronic pain and the management of it is only given about 5 hours of class instruction, on average, in an entire medical school curriculum. Furthermore, few graduating medical students enroll in post-graduate residencies for pain management.

It is no surprise that so few graduating medical students enter the field when so little attention is given to the management of chronic pain in their curriculum. The students understand that the respect a discipline gets is proportional to the time devoted to teach it.
The Center for Disease Control (CDC) defines an epidemic as “the occurrence of more cases of a disease than can be expected in a given area or among a specific group of people over a particular period of time.” Wouldn’t you think chronic pain would qualify? And yet, there has been little media attention given to the epidemic of chronic pain.
Perhaps the reason for such under-emphasis of chronic pain in medical school curricula is due to most Doctors who teach in medical schools think the students will learn it in their residencies. The problem with that logic is that most residency training occurs in facilities that are designed for acute care. The Doctors learn acute pain management and then try to apply those principles to chronic pain management. It doesn’t work very well.
It seems that chronic pain management has become obscured by the media attention of the “epidemic” of prescription drug abuse. When the numbers of addicted patients are compared to those with chronic pain it becomes obvious that we have failed our public in America. The management of chronic pain in America is the greatest failure of modern medicine.
For all the reasons I have stated (and more) many myths abound regarding chronic pain. I have compiled 7 of the greatest pain myths for you to consider.
7 Pain Myths
1) Chronic pain is just a symptom.
Acute pain is an early warning system that the malfunction of an organ system(s) is occurring. It is helpful to the patient and Doctor as it gives clues to what might be happening. In chronic pain there is no benefit to the patient (or Doctor for that matter). Furthermore, chronic pain amplifies the negative consequences of many existing diseases. Chronic pain increases death from cancer, heart disease, and strokes.
The effect of ongoing chronic pain can even cause disease that didn’t exist before. Depression, Peptic Ulcer Disease, and Heart Disease (as well as other diseases) can actually develop in people who have poorly treated chronic pain.
Chronic pain is a disease all unto itself and not just a symptom.

2) If there is no positive diagnostic study, for a given chronic pain syndrome, the patient must be lying.
In the disease model of medicine, Doctors routinely perform tests that look for structural causes for chronic pain. The problem with this approach is that it uses a Cartesian approach to pain where tissue damage must be identified before a patient with chronic pain will be believed. This approach works fairly well with acute pain but falls short in chronic pain patients.
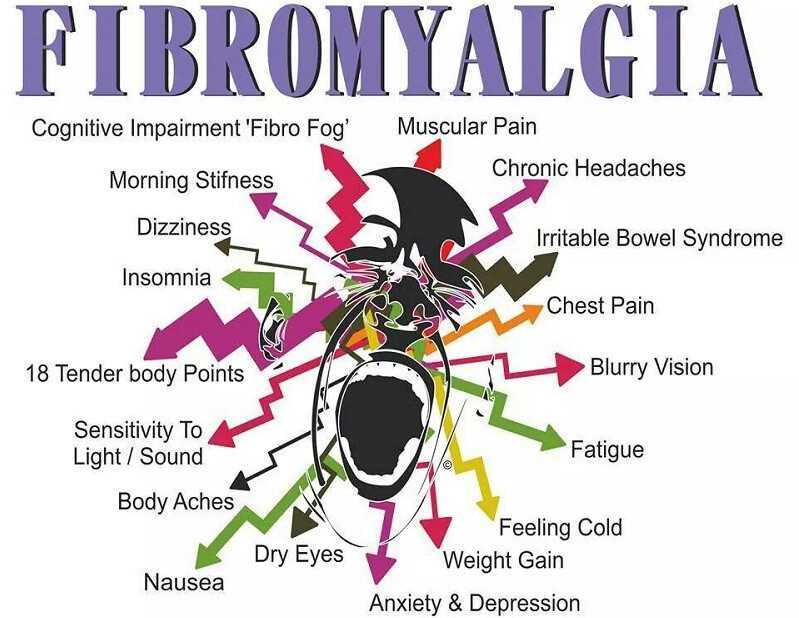
Pain is actually generated by the central nervous system where many disorders have no structural abnormality identifiable (such as in Fibromyalgia). Even cases of severe low back pain can have a “normal” MRI. Those patients are often treated with disrespect and told they are malingering.
A Doctor or nurse could no more tell the temperature of an oven by looking at it than they could estimate the amount of chronic pain a patient is in. Pain is physiologic not structural.
There is, to date, no diagnostic study that measures pain. Doctors must rely upon the honest reporting by their patients to gauge their pain.
3) Chronic pain is felt the same way by people who have the same disorder.
The perception of pain is very individualized. Syndromes that cause pain are neuro-processed differently in different people. Patients who grew up in emotionally traumatic environments will often have more extreme reports of pain from conditions that may only provoke mild pain in other people raised in a less traumatic environment.
Also, expectations and distractions effect how a person perceives their pain. There is a subset of people who benefit enormously from hypnotic therapy. In this type of person they are able to reduce their pain through “disattention.” Not all people have the same ability to use this form of therapy called “hypno-analgesia.”
Any given pain syndrome can have very diverse effects on different people.
4) All Doctors are taught how to diagnose and treat chronic pain.
I already covered this in the introductory section of this article. Most Doctors are resistant, if not embarrassed, to admit they do not understand chronic pain. Perhaps they subliminally sense their own inadequacies.
Most Doctors have inadequate training in chronic pain management.
5) Use of opiates for chronic pain relief usually leads to addiction.
There is a universal belief among Doctors that the use of opiates leads to addiction. A recent Cochran Review on the subject showed that people who have no genetic tendency for addiction have less than a 1% chance of becoming addicted taking opiates.
However, all people who take opiate pain medication on a regular basis become habituated. This is a physiologic phenomenon which requires gradual reduction of an opiate when desiring to change to another medicine inorder to avoid a serious abstinence syndrome (nausea, vomiting, body aches, diarrhea, etc.).
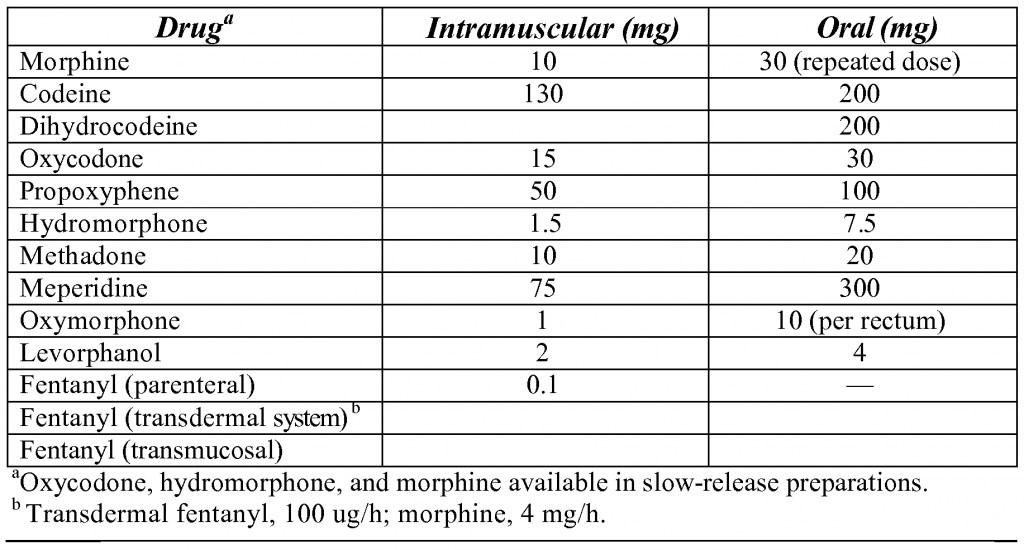
During the Vietnam War, 20% of the returning American veterans were using heroin during their military tour. When they returned home, greater than 95% of these veterans returned to their families without needing to go into drug rehabilitation. Having taken heroin for years in Vietnam did not automatically make them addicts.
Sociologists believe that the making of an addict depends on the “cage we live in.” That is, the family, neighborhood, and culture that we are reared in. Attributing addiction to a chemical substance is too simplistic. As you look around you, does this approach seem to be working?
The use of opiates does not make a person an addict.
6) Chronic pain can be so severe that it cannot be relieved.
I am aware of many patients who were told that their pain just couldn’t be relieved. They would have to learn to live with it (not a good idea for reasons that I previously mentioned). In all the cases of pain that I was acquainted with there was always some way to reduce pain to a tolerable level.
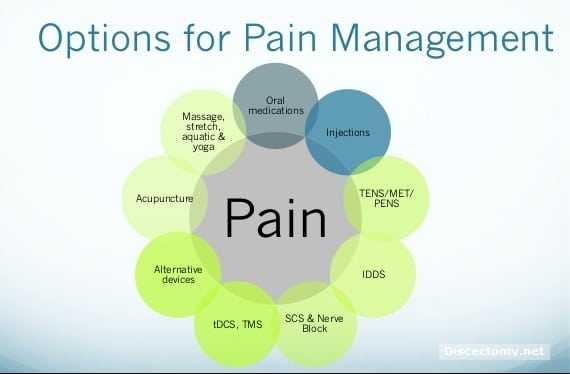
The relief of a patient’s pain is proportional to the treating Doctor’s motivation to do so. The “you have to live with it” comment by treating practitioners is an attempt to curtail any further involvement in a pain patient’s case. It is code language for not being interested or committed to the patient.
It is also good to remember that the more severe the pain the greater the risk that goes along with treating it. There are no “risk free” options when treating chronic pain.
There is no pain that is so severe that it cannot be treated.
7) Doctors all agree on the best way to treat chronic pain.
The field of pain management is where many other areas of medicine were before they were well understood and taught in medical school. Medicine is an evolving science. Pain management is still quite primitive and needs an objective way to detect pain in a person.
Pain management is an area of medicine where Doctors often disagree on the best way to treat a person’s pain.
Finally
There are more myths than the ones I have enumerated. These are the ones that seem to recur in the many conversations I have had with Doctors and patients alike. Perhaps the durability of these chronic pain myths give people a certain measure of comfort by keeping the pain patient at arms length and subjugating the importance of their pain?
Or perhaps it is that the pervasiveness of chronic pain and our inadequate response to it as Doctors, family, and friends is too disturbing for our psyche to handle? We find ourselves needing to project the blame somewhere other than ourselves for this modern day blight.

Nevertheless, these beliefs will change as they must change. The plight of the chronic pain patient must become the focus of a national repentance about how we are failing to address this epidemic. Doctors will need to become warriors to stand up to all the contrary forces that seek to limit effective treatment in lieu of the influence of legal, financial, and social pressures.
“I have a dream” that one day the chronic pain patient will be able to receive the treatment to relieve their pain as law enforcement, insurance companies, and the politics inside and outside of medicine unite with Doctors to quell this epidemic.
Imagine law enforcement working with Doctors to identify addicts and help place them in drug rehabilitation rather than the present adversarial relationship that exists.
Imagine Doctors working with law enforcement helping to identify the small neighborhood cartels that illegally distribute prescription medications.
Imagine insurance companies actually funding pain therapies that work instead of paying for ineffective, high cost procedures.
Imagine drug companies pricing their pain medications so that all people have access to the best medications available.
Imagine families, friends, health care workers, law enforcement, etc. pooling their resources to intervene on behalf of a person who has become an addict and help them transition into drug rehabilitation instead of stigmatizing the addict.
Imagine there being a diagnostic study that reliably measures chronic pain.
Imagine the medical profession actually teaching, integrating, and emphasizing the treatment of chronic pain in their medical school curriculum.
What we imagine can become a reality…
Wishing you joy and healing,
Facebook
Google+
Twitter
Pinterest
Reddit
Tumblr
Skype
StumbleUpon
WhatsApp
Email
Print
VK





Thank you doctor. It is reassuring that there are medical professionals who listen, try to understand, and who BELIEVE.
Thank you for your good wishes.