Plantar Fasciitis FAQs and Answers

What is plantar fasciitis?
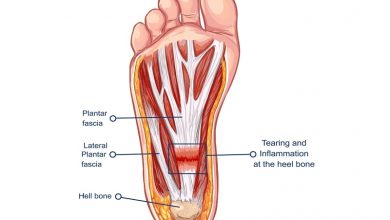
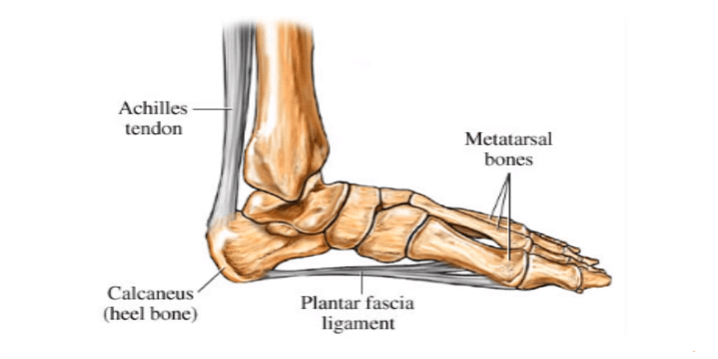
Plantar fasciitis is inflammation of the ligament that runs along the sole of the foot from the toes to the heel, called the plantar fascia. The inflammation usually occurs where the ligament attaches to the heel bone, causing pain in the heel area of the sole of the foot. The pain is worse when standing or walking; it is particular sharp and severe first thing in the morning, when the first steps are taken after getting out of bed.
What are the symptoms of plantar fasciitis?
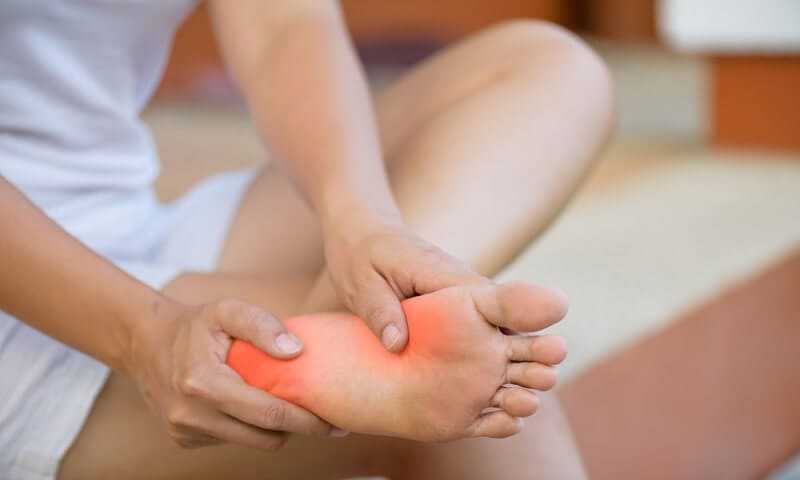
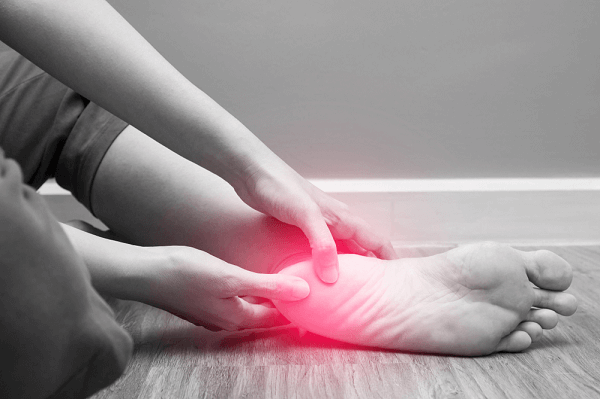
The main symptom is pain in the sole of the foot, near the heel bone. This is caused by the inflammation of the plantar fascia ligament. The pain starts off as a tender spot that feels like a stone bruise but becomes more severe and sharp as the condition worsens. The pain on taking the first few steps of the day has been likened to walking on shards of glass.
What causes plantar fasciitis?
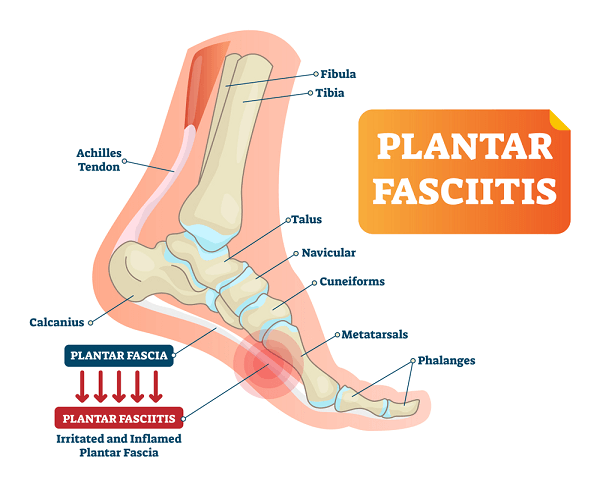
The plantar fascia ligament acts as a shock absorber for the feet; it supports the arch which flexes to absorb the impact of weight-bearing. By wearing shoes that are old or don’t fit properly, by regularly standing for long periods, especially on hard surfaces, by wearing the incorrect shoes for the exercise or sport you are doing or by being overweight, the tension on the ligament becomes too great and causes minute tears to occur. These become inflamed, causing pain. People with flat feet or overly-arched feet are especially prone to plantar fasciitis.
Can plantar fasciitis be prevented?
There are certain measures you can take to prevent plantar fasciitis occurring and to avoid it recurring. The following points are important:
- Wear shoes that support the foot and ankle properly.
- Shoes that have an arch support and cushioning at the heel are recommended.
- Avoid going bare foot or wearing slippers and flip-flops.
- If you need to stand for long periods on a hard surface, place a thick rubber mat under your feet for extra cushioning.
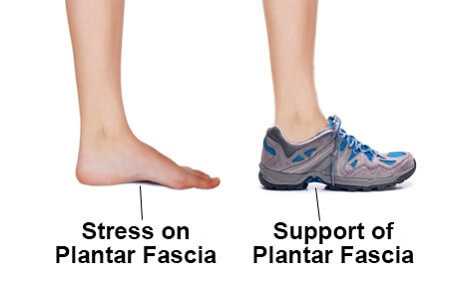
- Wear shoes that are designed for the activity or sport you are participating in.
- Avoid walking or running on hard surfaces all the time.
- Alternate exercise activities to prevent damage to the plantar fascia.
- Stretch the calf muscles, Achilles tendon and plantar fascia before exercise.
- Follow a short daily routine of specific exercises designed for plantar fasciitis patients to prevent the ligament becoming short and tense.
- Maintain a normal weight for your height
For more information about this, click “6 Ways to Help Prevent Plantar Fasciitis“.
How can I avoid plantar fasciitis coming back after I have successfully treated it?
Following the prevention strategies listed above is the best plan of action to prevent recurrences. Pay particular attention to establishing a daily routine of stretches, wearing the correct shoes and alternating exercise activities and surfaces.
Can plantar fasciitis be treated?
There are several treatment options that have been shown to be effective in the majority of plantar fasciitis cases. Effective treatment also helps to prevent a recurrence of the condition. The following conservative treatment methods are those that have been shown to be the most effective:
- Rest – it is important to get off your feet to allow the healing to take place and to ease the pain.
- Ice – applying ice to the area is most effective at easing the pain and reducing inflammation. Repeat the process regularly in the first days of the pain occurring.
- Anti-inflammatory medications, NSAIDS, including those with aspirin or ibuprofen, help to reduce inflammation and pain. Over-the-counter NSAIDS may be sufficient or your doctor can prescribe stronger ones.
- Specific plantar fasciitis exercises and stretches help to correct the tight ligament and prevent a recurrence. These need to be done daily, on an on-going basis.
- Night splints help to stretch the plantar fascia and calf muscles.
![]()
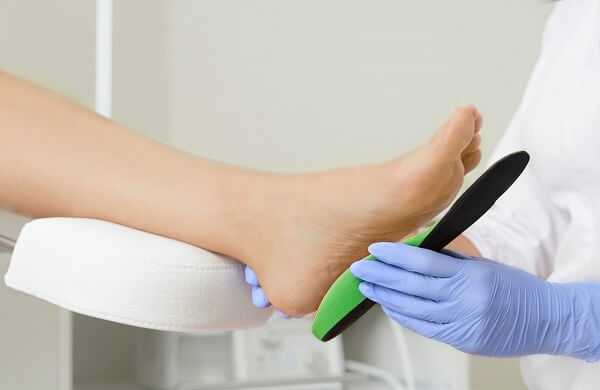
- Arch supports in all footwear give the necessary support and prevent strain and tension on the ligament. Custom-made orthotics are helpful for some people.
- Cortisone injections into the ligament may help to relieve pain.
For more information about this, click “Medications Used for Plantar Fasciitis“.
Surgery is a last treatment to be tried mainly because it has many potential complications and side effects and doesn’t have a high degree of success.
What are the risk factors for plantar fasciitis?
- Age and sex – plantar fasciitis is more common between 40 and 60 years of age and is more prevalent in women than men.
- Obesity – excess weight puts added strain on ligaments and muscles.
- Occupation – a job requires that you to stand or walk for long periods on hard surfaces puts you at greater risk.

- Certain activities and exercise – distance running, dance aerobics, ballet all place added strain on the heels and ligaments.
- Incorrect or badly fitting shoes – shoes that are loose, have no arch support or cushioning, have thin soles or are flat all have the potential to cause damage to the plantar fascia. Going bare foot can also cause problems.
- Foot mechanics – flat feet, high arches or abnormal walking patterns all affect the weight distribution of your feet, adding stress to the plantar fascia.
Is plantar fascia surgery worth the risks?
Plantar fascia surgery is only suggested after all other conservative treatment options have been tried and failed. Only patients who have been following a treatment plan for around 12 months, that includes a daily exercise regime, will be considered. Surgery is the very last treatment option and only 5% of all plantar fasciitis sufferers will have it. The prognosis is not good for the surgery and orthopedic surgeons cannot give a high likelihood of success. The best course of action is to discuss your case with a qualified surgeon and then make your own decision.