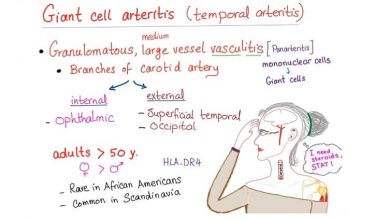
Polymyalgia Rheumatica (PMR)

Not long ago, most physicians probably knew polymyalgia rheumatica—if they knew of it at all—as the “surprise arthritis,” because its symptoms were said to strike so suddenly. Their colleague, the rheumatologist, probably characterized it as difficult to conclusively identify— so difficult, in fact, that a patient’s swift and satisfactory response to drug therapy was often taken as confirmation of the diagnosis.
It would be gratifying to say that time and science have put matters right, that PMR is known and completely understood, but the most that can be said is that PMR is better understood. It is now known that patients have good reason to be optimistic.

PMR rarely affects anyone under fifty, strikes twice as many women as men, demonstrates a mild family connection (though it doesn’t seem to be strongly hereditary), and—like some other rheumatic conditions—almost all reported individuals are Caucasian.
PMR is rarely life-threatening, says Dr. Bevra Hahn, professor of medicine and chief of rheumatology at UCLA in Los Angeles. Nor is there much likelihood of the sort of joint deformation common to other forms of arthritis. ‘That’s quite unusual,” says Hahn. And the really good news is that in some 50 to 60 per cent of patients, the disease goes into total remission after one to two years.
What is Polymyalgia rheumatica ?
“Polymyalgia rheumatica” is a good summary of the ailment, poly meaning many, myo meaning muscle, algia meaning pain, and rheumatica referring to an inflammation of connective tissue, such as muscles and ligaments. Patients complain of usually symmetrical pain and stiffness in the neck, shoulders, pelvic girdle, thighs, and buttocks.
Location is one of the reasons PMR can be difficult to identify, says Dr. Gene Hunder, chair of the division of rheumatology at the Mayo Clinic in Rochester, Minnesota, and professor of medicine at the Mayo Medical School: There’s often a mild synovitis (joint inflammation) associated with the disease—”mild in the sense that there’s not a lot of swelling”—but since it’s often the hips or shoulders that are involved, “there’s no way the hip joints, for instance, can be palpated [felt or examined by hand, because the joints are so deep beneath the tissues].”

Hunder estimates that about one in two hundred people over fifty are at risk, but there’s a marked difference in the symptoms patients experience. “Someone with the more severe disease could have a low- grade fever,” says Hunder, “marked fatigue, and anorexia weight loss.” Hunder describes one of his patients, who was confined to a wheelchair because of involvement in her hips and thighs, who was so stiff that she was having a hard time washing her face and combing her hair. “On the other hand,” he says, “PMR can be very mild. The patient limbers up in an hour in the morning and has few symptoms the rest of the day. They feel a little fatigue or stiffness after sitting for an hour, but they don’t have a systemic sickness. PMR covers a broad spectrum.”
Is it a “surprise arthritis”? “It’s highly variable,” says Hahn. “Some patients can tell you the time and date it started to hurt, others no. But the same is true with rheumatoid arthritis. You can wake up with rheumatism in every joint, or it can creep up over a period of months. It’s the same for most rheumatic diseases.”
Diagnosis and Treatment
Hunder claims that making an accurate diagnosis isn’t really all that difficult: “By taking a careful history of the patienf s symptoms, you can elicit the typical features of the syndrome. If a patient can sit in a comfortable position, for example, the symptoms would be less, and they might not even be present at times.” The morning stiffness is also very characteristic: ”We look for that. During the first easy movements— turning over in bed, pushing the covers down—that would accentuate the discomfort. Then, after one or two hours, the symptoms would tend to subside, only to return after another period of inactivity.”
There’s also a blood test that measures the sed rate (see the related article): Most people with PMR have a characteristically high rate. All of that— plus age over fifty, pain location, “and the absence of swelling in peripheral parts of the body,” says Hunder, “which might suggest RA”—contribute to a diagnosis of PMR.
Treatment Options
Then there’s patient response to drug treatment—usually the corticosteroid prednisone. “PMR responds abruptly and very well to it,” says Hunder, “so some people see it as a diagnostic test. But there are a number of types of rheumatic disease that respond to prednisone, so I think it should be seen as just one point in the diagnosis. I don’t usually use it as a diagnostic tool, because I hope to make an accurate diagnosis before starting the patient on prednisone.”

If a patient’s condition can be managed with NSAIDs or ASA, it should be. Prednisone is a powerful drug—”a two-edged sword,” says Hunder. Possible side effects of long-term use include fluid retension, hypertension, easy bruising, diabetes, psychological effects—anxiety, hyperactivity, stimulation, or depression—even osteoporosis. “The idea,” says Hunder, “is to use the least dose for the shortest period of time that satisfactorily suppresses the disease.”