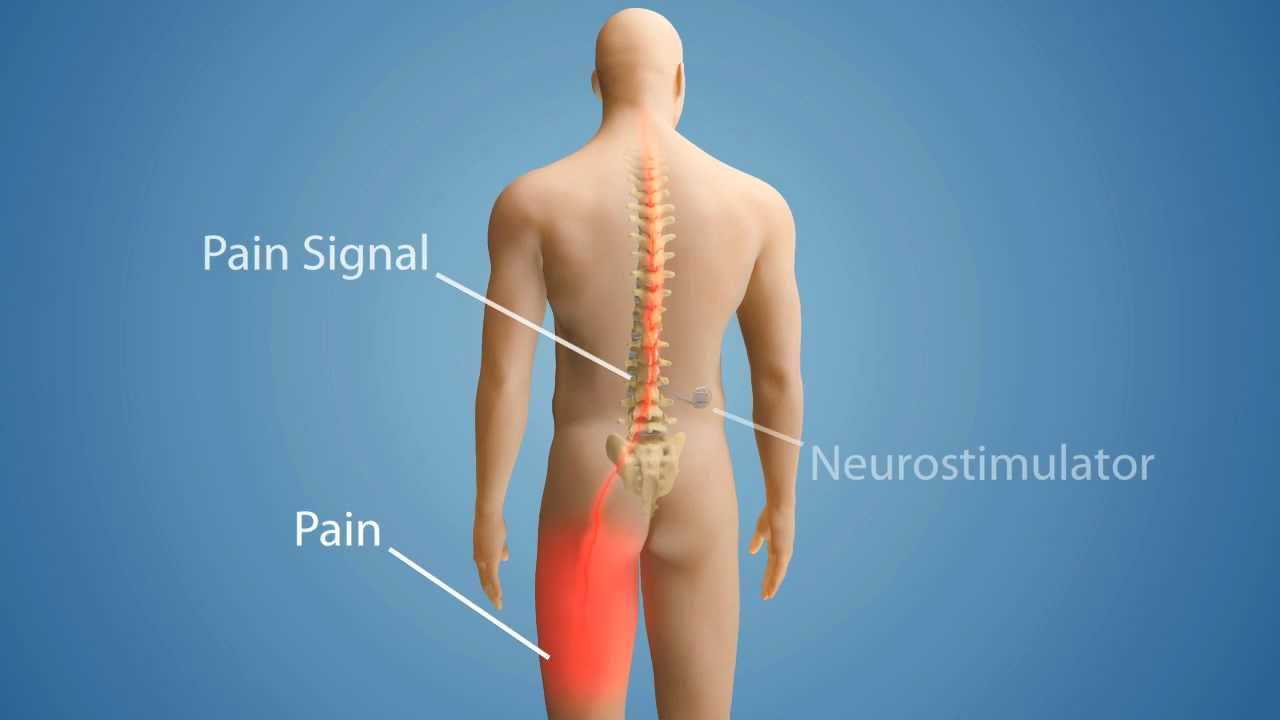
Recovering from back surgery

Overview
The recovering from back surgery can be lengthy and arduous, but in some cases patients may be able to return to work and normal activities within a few days or weeks rather than months. Minimally invasive back surgery that proceed without complication are often fairly swift to recover from, with microendoscopic discectomy and microlaminoforaminotomy two types of back surgery with a shorter operating time and a quicker recovery for most. In the majority of cases a brief period of rest followed by increasing gentle activity, such as walking, is encouraged after surgery to keep a patient healthy, get the blood flowing, and reduce stiffness. Patients are advised to stop any activity which leads to sharp or persistent pain and report unusual symptoms to their surgeon or physician for assessment.
The more involved the surgery the more protracted recovering from back surgery can be, in general. A laminotomy, for example, conducted to gain access to a herniated disc in neck or back which is then removed (discectomy) will usually take longer to recover from than a simple laminotomy to reduce pressure on the spine. If larger areas of tissue, ligament, or bone, have been removed during surgery then patients will usually be told to refrain from any twisting of the spine for at least six weeks after surgery to allow the tissue inflammation to go down and to avoid the development of fibrous scarring which may cause failed back surgery syndrome.
Support Devices
Most patients will require some kind of surgical collar, brace, or halo while recovering from back surgery such as laminectomy so as to keep the spine stable as it heals. The degree of rigidity of the support device will depend on the type of back surgery as operations involving spinal fusion of some kind are more likely to need stiffer support to avoid movements of the spine and potential shifting of the graft. Back surgery for scoliosis, kyphosis, or other major structural condition, is likely to require an extensive support device to maintain the new alignment of the spine and encourage fusion and healing. Other, more minimal surgeries are likely to require more gentle, short-term support. Patients should not use a stiff cervical collar or back corset for longer than is advised as this can inhibit the recovery of spinal muscles and cause weakness, hypo- or hyper-flexibility of the spine increasing the risk of further pain and disability.
While recovering from back surgery, patients should refrain from any heavy lifting, bending, or twisting of the spine until their follow-up appointment and should wear the supportive devices as directed by their surgeon for optimum recovery. Follow-up appointments are usually scheduled two weeks after back surgery where restrictions on activities may be lifted. After procedures such as laminoplasty or laminotomy the physician will usually perform an X-Ray at the follow-up appointment to determine the level of decompression achieved by the surgery. The presence of any anomalies can also be detected here and guidance given regarding activity resumption.
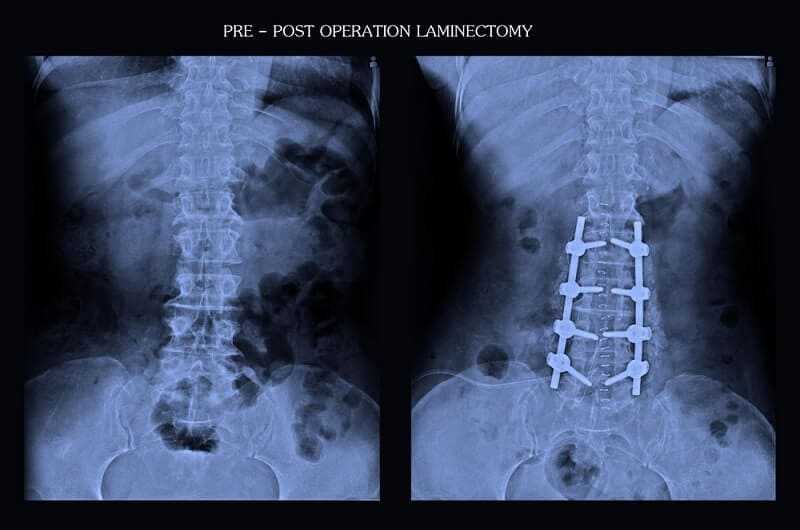
Long journeys as a passenger in a car are also commonly advised against while recovering from back surgery such as a laminectomy, corpectomy, or fusion, and braces or collars should be worn as recommended on any car journey. If non-dissolving sutures were used during the procedure then these will usually be removed at the two-week follow-up. Most surgical sutures are now the dissolvable type and require no appointment for removal.
Resumption of Activities
The correct time for resumption of activities such as driving, house work, exercise, or coitus should be discussed with the physician, ideally prior to surgery, to prevent undue spinal strain and optimize recovery. Driving is usually to be avoided for at least two weeks and support devices used for a little longer if driving or a passenger in a car. Heavy lifting, twisting, and bending can cause a greater amount of scar tissue to form in the spine and inhibit recovery or require further surgery to remove the fibrosis.
Most patients will be encouraged to undertake regular exercise in the form of walking while recovering from back surgery with a prompt resumption of gentle activity important in reducing the risk of thrombophlebitis. Ideally, patients will gradually build-up to two fifteen-minute walking sessions per day at two weeks post-surgery, and then 30-40 minutes twice a day at six weeks. Patients can walk for longer each day if they are comfortable but should take care not to rush their recovery as this may worsen their prognosis. Engaging in contact sports or high impact exercise is also frowned upon and swimming may not be suitable for those undergoing surgery on the cervical spine as it can strain the neck. If any activity leads to pain then the patient should cease that activity immediately and discuss their symptoms with their doctor or physical therapist.
Patients who have had spinal stenosis for a protracted period of time, or have incurred significant nerve impairment may find that their abdominal muscles and back muscles are weak and that a slower return to full activity is the preferred choice. It is wise to avoid sitting for a protracted period of time while recovering from back surgery as this can lead to stiffness and pain. House work, such as vacuuming, ironing, or carrying heavy laundry, and bending to load the machine is also likely to delay or compromise recovery and should be delegated until cleared by the surgeon. For more complex surgeries, such as a corpectomy, the recovery period will be longer than for less invasive back surgery, such as a microlaminoforaminotomy, and patients will usually not return to work for many weeks.
Post-Surgery Hygiene
Surgical incisions should be kept clean and dry, and care should be taken not to rub the area but to pat it dry instead. Dressings should be changed regularly according to the surgeon’s advice and, for some patients, this may mean engaging the help of a relative, friend, or health-care assistant as it is inadvisable to twist to change the dressing on your back. Any inflammation, fever, or leaking from the surgical incision should be investigated immediately to rule out infection or other complication. Patients are sometimes instructed to measure their temperature at the same time everyday (4pm or so) to monitor for any potentially problematic signs. If an infection does occur then antibiotics will usually be prescribed. In rare cases where the infection has spread to the spinal fluid, a further operation may be required to drain the infection and sew up the potential tear in the dura of the spinal canal.
It is usual for patients to experience some pain at the site of incision, and spasms of the muscles around the operated area also occur on occasion. Avoiding draughts or extreme cold, and wearing the prescribed surgical collar, corset, or brace can reduce these symptoms. After a laminectomy in the cervical spine care should be taken not to tilt the head back while shaving (for men) and it is wise to avoid washing your hair in the sink as this can also strain the neck. It is usual for patients undergoing back surgery to resume showering the day after surgery, although this should be discussed with the attending physician in order to maintain optimum healing conditions for the site of incision and prevent back strain.
Symptom Improvement
Patients who had numbness and weakness of the hands, arms, or lower limbs prior to their back surgery are likely to find that this continues for some time after the procedure as the damaged nerves work to repair themselves. Depending on the severity of damage the nerves can take six to eighteen months or so to heal, although in some cases the trauma will have permanently cut off nerve function. Pain can continue as the nerve heals and patients may also find that warm tingling sensations occur as the sensation returns. Gentle exercise can aid recovery although there are likely to be some movements which are to be avoided, such as raising the arms above the head for cervical laminectomy patients, so as to reduce spine strain.
After a foraminotomy operation to relieve pressure on the spinal nerves, most patients experience immediate improvements in the symptom of pins and needles in the arms and a reduction in pain relief occurs in 80-90% of cases. Weakness of the muscles and numbness usually take longer to correct, with six to twelve weeks a common recovery period, assuming no permanent damage has occurred. After this procedure most patients are up and about after a couple of hours and return home within the day. Similarly, as microlaminoforaminotomy is often performed using a local, rather than a general anaesthetic, some patients actually experience an immediate reduction in radicular pain during the surgery. This, as always, is affected by the level of trauma that has occurred and for most patients a period of several weeks is the more likely time-frame for recovery from pre-surgery symptoms. Fine-motor skills and strength are a little longer in returning as the innervation of muscles improves. Numbness can take a little longer to dissipate after a microlaminoforaminotomy.
In cases of minimally invasive laser spine surgery the recovery period is usually reduced in comparison to standard open surgery techniques. This is due to the reduced amount of tissue damage involved in this type of surgery and the shorter operation time. With more conventional surgery where a large region of the back is opened up, ligaments and nerves moved aside, and a greater degree of bleeding, a patient is more likely to suffer bruising, pain, tenderness, and a longer period of recovery. Minimal access discectomy can result in prompt recovery for patients and they will usually be able to return home on the same day as their surgery. Again, patients undergoing the more traditional procedure of open discectomy will suffer from a larger amount of tissue trauma and will usually stay in hospital for around four days.
Post-Surgery Medications
Narcotic medications may be used briefly after surgery to cope with pain, but should be discontinued after two to four weeks as they are addictive. Narcotic medication can cause constipation, so patients are advised to drink plenty of water and eat sufficient fiber. Tylenol (acetaminophen) is another option for managing pain. Patients should discuss the use of any nutritional or herbal supplements with their physician prior to use as these can react with other medications they may be taking or have an adverse effects on their immune system or blood coagulation. Some herbal anti-inflammatories for example may be problematic if a patient has received an implant due to potential immune system rejection of the device. Others, such as white willow, fish oils, or vitamin E may cause complications with regards to bleeding and haemorrhage after surgery.

Whilst not a medication, the nicotine in tobacco can significantly affect back surgery and smoking should be stopped well in advance of any surgery on the back. Patients may not be able to access spinal surgery if they refuse to quit smoking as the habit can seriously compromise recovery. Smokers undergoing spinal fusion have been shown to have a 40-50% failure rate in comparison to 8-20% of non-smokers. Continuing to avoid smoking after surgery is also wise as fracture rates are higher in smokers as is their usage of analgesic medications. Smoking also reduces the synthesis of collagen and can compromise the stability and flexibility of the spine and other joints in the body.
In cases where recovering from back surgery involves cervical spinal surgery it is possible that some swelling may occur in the neck which causes difficulties for a patient in swallowing food, liquids, or medications. In these cases an IV may be started to allow for proper delivery of fluids and medication. A hoarse throat can also occur in operations such as an anterior cervical discectomy due to the possible impact on the laryngeal nerve during this surgery. On rare occasions this may lead to a permanent change in the voice or even cause the loss of the voice but is usually only temporary and recovers after inflammation reduces.