Ruptured Disc – A Cervical Herniated Disc
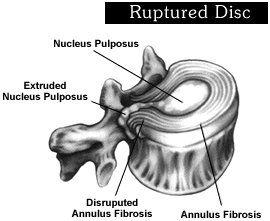
Ruptured Disc
A ruptured disc can be considered as the end stage in the developmental process of a disc herniation. Unlike bulging or protruding discs which are contained disc disorders (where in the nucleus pulposus is still confined within the annulus pulposus), a ruptured disc involves the creation of a tear in the outer fibrous ring that causes disc material to protrude further into the spinal canal or there is actual leakage.
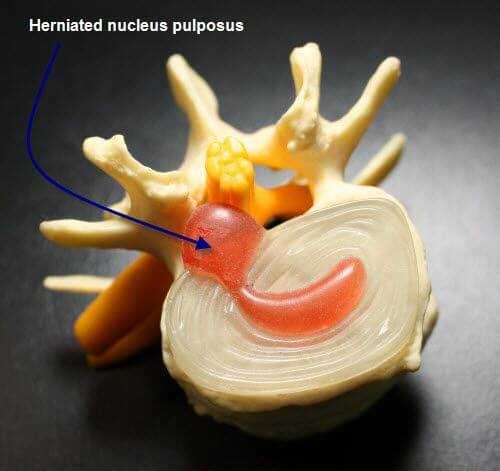
Thankfully, research on disc herniation has shown that bulging and protruding discs occur more often than ruptured discs. However, there is a greater propensity for severe pain in patients with ruptured discs.
Although ruptured discs could develop in any part of the spine, it is more commonly seen in the lower back (lumbar) region than in the neck (cervical region). Disc herniations of all types are rarely found in the upper/middle back.
Ruptured Disc Symptoms
Ruptured disc symptoms occur as a result of two factors…
- Compression of the nerve; and/or
- Irritation of the nerve roots or nerve by the extruded disc materials and inflammatory mediator substances.
Nerve compression leads to pain that follow the nerve that is affected. In the case of a ruptured cervical disc, the prominent symptom is neck pain. In a cervical ruptured disc, neck pain travels down to the shoulder and arm, descending further to the hand and fingers. The pain of a ruptured lumbar disc follows the path of the sciatic nerve, starting from the lower back and buttocks, going down to the leg and foot.
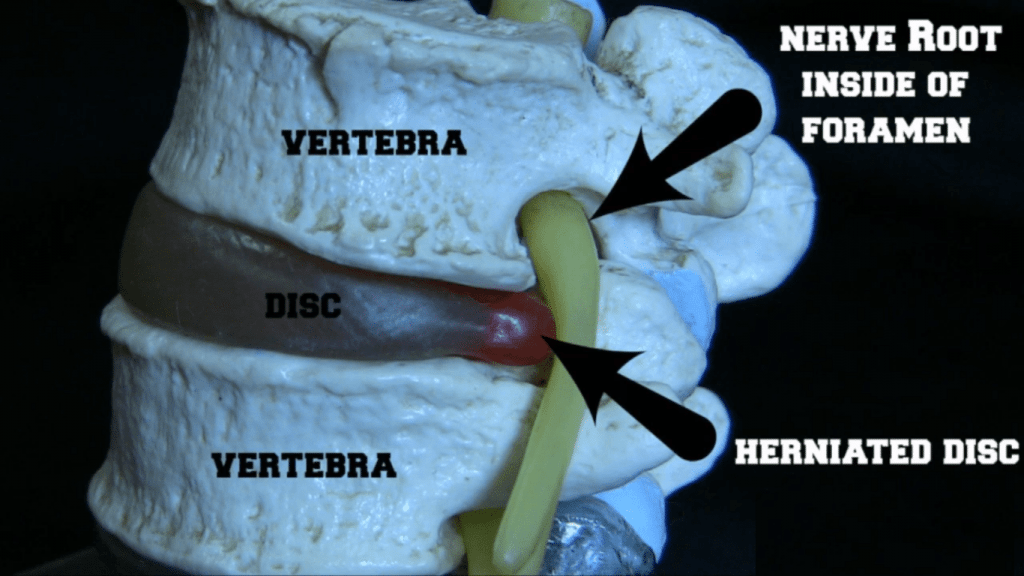
Irritation of the affected nerve by inflammatory chemical mediators increases the severity of pain. In some patients, pain or numbness can be so bad that moving the affected limb is very difficult. In others, walking is affected, so that a patient needs to be aided by a loved one or a caregiver.
Ruptured Disc Treatment
Most cases of ruptured discs resolve on their own, although healing takes a much longer period of time in comparison with bulging and protruding discs. Healing of ruptured discs usually take 1 to 6 months. Bed rest with a firm mattress is strongly advised for a ruptured disc, with a gradual increase in activity as supervised by a doctor or a physical therapist. To help reduce tension on the back while lying down, one could lay a pillow under the feet.
Exercises are very effective in relieving pain. Like bulging and protruding discs, the best exercises are gentle muscle stretches and back strengthening exercises, while avoiding twisting or jerking movements.
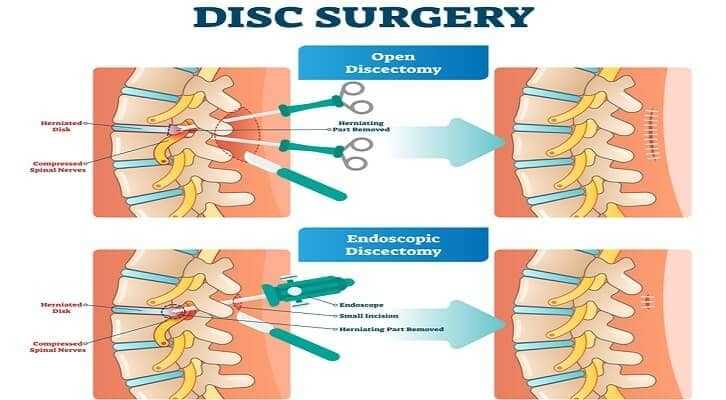
Ruptured disc treatment includes intake of NSAIDs to relieve pain and inflammation. Epidural injections of corticosteroids and cortisone are helpful in patients with severe pain. Surgery may be indicated as there is a greater risk of deteriorating neurological function. The surgery of choice for ruptured disc is discectomy, which involves removing the extruded disc material to relieve nerve compression and pain. Depending upon the affected site, discectomy can be performed via endoscopy or as a major open operation.
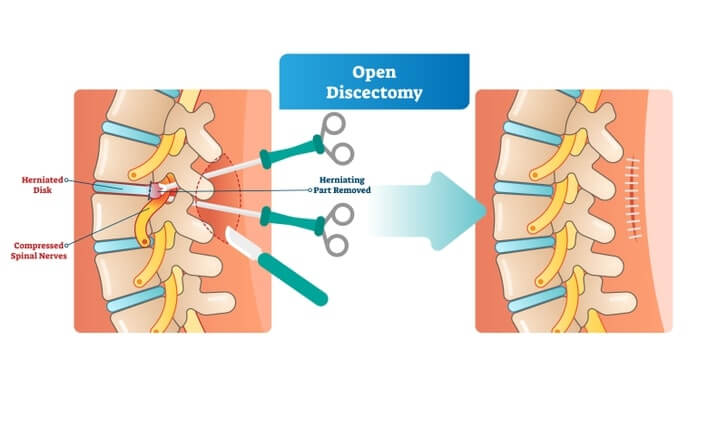
Although there are many treatment options for a ruptured disc, it is very important for patients to promote healing and not aggravate the condition by creating stability in their spines through the observation of good posture and regular exercise.