Severe Chronic Arthritis

If you live long enough you are going to develop a form of severe chronic arthritis called Osteoarthritis. In this blog post I will be discussing this most common of all arthritic conditions in human beings.
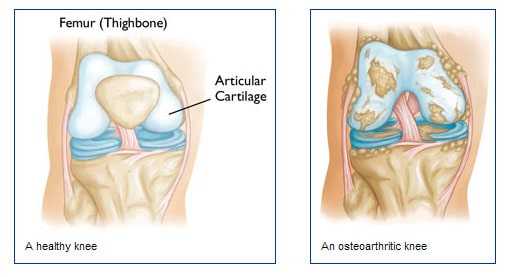
In fact, it is so common that I often explained to patients that Osteoarthritis is more a function of “wearing out” than really being a disease process. For instance, when the brakes of your car wear out through use it doesn’t usually mean they are defective (unless they wear out more quickly than expected). Osteoarthritis is like that…a “wearing out” of the joints.
27 million Americans have Osteoarthritis. Nearly everyone over the age of 60 years old have it. Women tend to develop it more than men.
There is a tendency for it to cluster in families (if a close relative has it you will have a higher likelihood of getting it). There is a form where it is developed at a considerably younger age than 60 years old. That type of Osteoarthritis would have a strong genetic connection.
There are risk factors besides genetics. Obesity, over use of your joints, injuries to the joints, and joint abnormalities from structural issues (ie. scoliosis) all increase the risk of developing Osteoarthritis.
What It Feels Like ?
Essentially, the severe chronic arthritis of Osteoarthritis is pain in the involved joints. The joints that are the most susceptible to it would be the joints that are enduring the most “wear and tear”.
In the usual course of events this would be what would be called “weight bearing” joints. However, if you use your hands excessively (not a weight bearing joint unless you walk on your hands all day:) you can develop it in your fingers.

The pain of Osteoarthritis worsens with over use or prolonged rest. It is almost as if the “joint lubrication” has dried up (actually it does). Imagine how the engine of your car would work without oil?
Eventually the engine would “seize up” and stop. Without oil in your automobile engine you would destroy the cylinders, valves, etc.. This is analogous to what happens in Osteoarthritis.
Osteoarthritis (OA) lacks the systemic immune reactions that are seen in Rheumatoid Arthritis and Systemic Lupus Erythematosis. There is usually no fever, weight loss, or blood abnormalities in OA.
What It Looks Like ?
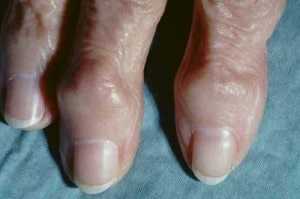
On physical examination, the joints may be swollen but not excessively red. The joints may make noise (crepitus is what medical people call it) when moved. Remember the joints at risk are the ones that undergo the most use so hands, knees, hips, and spine are favorite targets of OA.
On X-Rays of the involved joints, the joint space will appear to be narrowed (due to a loss of cartilage) and deformed. There will often times be excessive bone growth on the edges of the joint due to the bone reaction to cartilage loss. In time the joint deforms and may bend outwards (especially in OA of the knees).
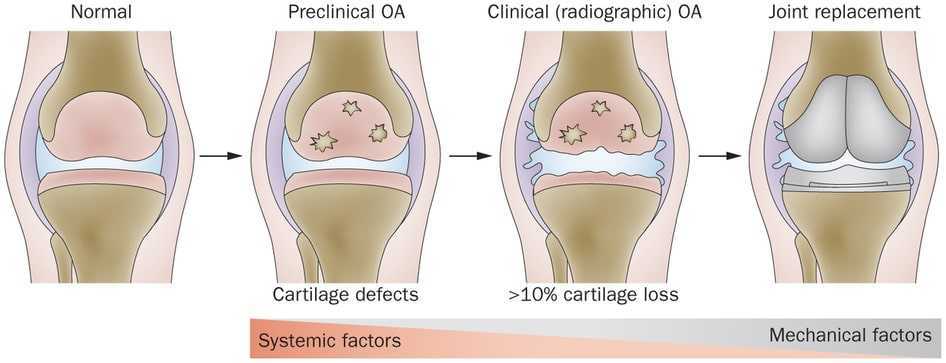
When viewed by MRI or CT Scanning of the joint there is an absolute loss of cartilage on the surface of the joint. The loss causes “pitting” which are actual plugs of cartilage lost.
How To Diagnose It ?
The diagnosis of OA is not mysterious. The history as previously enumerated, physical examination as we have said, and an absence of blood abnormalities is usually enough to make the diagnosis.
X-Rays, MRIs, and CT Scans are not usually necessary to make the diagnosis. Those studies are most useful for pre-operative evaluation so that the surgeon can plan his best strategy for the patient.
How It Can Be Treated ?
Fortunately, OA is a very treatable form of severe chronic arthritis. The following treatments would be considered standard for this disorder:
Weight Loss: obviously reducing the stress on the joints is essential to persevering function and healing.
Exercise: the beneficial effects of exercise are numerous. The best exercises are the ones that do not increase the stress on the joints too much. Aquatic exercise is an excellent alternative for OA as the water has a effect to “off-load” the stress on the joints.
Medications: natural anti-inflammatory supplements, skin applied over the counter medications, non-prescription medications, and prescription medications are all very helpful for OA. I refer you to review and search this website for the numerous articles on a variety of therapies that may be helpful to you.
Joint Injections: there are a variety of medications that can be directly injected into the joints. The most preferable is a class of medications that may help rejuvenate the cartilage in the joint (usually only the knee can receive these injections). The other injections are anti-inflammatory and provide excellent temporary relief.
Surgery: when the less invasive therapies don’t work a surgical consultation is a good idea. Orthopedic Surgeons are experts in their evaluation of OA. The least invasive procedure that relieves pain is usually the best surgical option. However, actual joint replacement may be the final result after all other therapies fail. Because a joint replacement has a fixed duration before it too wears out, most Orthopedic Surgeons prefer to replace joints as a last resort.
Finally
We have discussed the diagnosis and treatment of severe chronic arthritis caused by OA. This is the most common form of arthritis and is very treatable.
I would also like to hear from you. Please leave me a question or a comment in the space below and I will be sure to reply promptly.
Wishing you joy and healing.



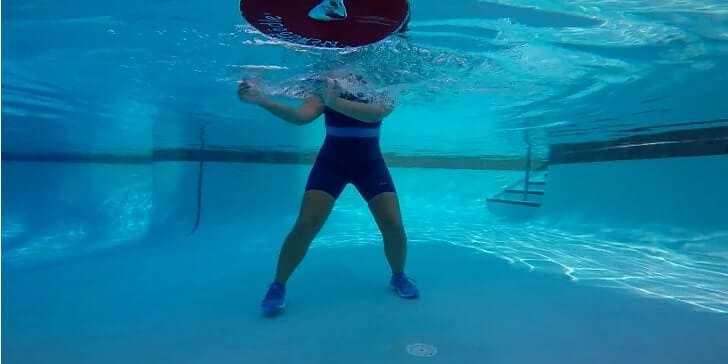
Thanks for been diagnosed with the great information I have OA,of my knees I have had 3 cortisone shots this last time my Orthpedic Dr said let’s try Gel shots and PT, all has been like at a 75% inprovement in pain relief although when it rains or it’s cold outside I feel it bad.