Spinal Cord Injury Nerve Pain

Injury to the spinal cord (SCI) was usually a lethal event up until World War II. The poor soul that survived was subjected to a world confined to a wheelchair (at best), little social helps (such as graded curbs), and recurrent infections (urinary and pressure sores).
The irony of war caused advances to occur that improved the survival of people with spinal cord injuries. Improvements in antibiotics, treatment of pressure sores, and advancements in the surgical stabilization of a traumatized spine radically improved survival.
The lethal complications of SCI…urinary sepsis, pulmonary embolism, pneumonia, and pressure sore infections have become more manageable. Early intervention for these complications have substantially improved the life expectancy of people with SCI.
The most recent statistics on spinal cord injuries are as follows:
- There are at least 12,000 spinal cord injuries per year in the US (that is new injuries).
- 250,000 to 450,000 Americans live with the results of a SCI (65% in chronic pain).
- The estimated cost is 9.7 billion dollars per year (I always cringe at cost disclosures).
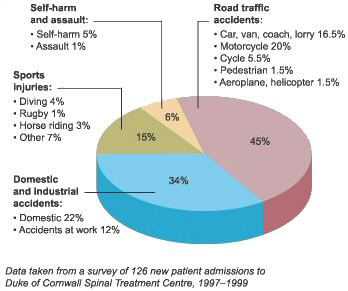
- The largest proportion of SCI is due to car accidents (followed by falls and violence).
- The average age at injury is 42.6 years (implying decades of supportive care will be needed).
- 80% of SCI patients are men (implying a significant restructuring of family’s that have a member with a SCI).
These statistics do not include the war injuries that our brave men and women are suffering defending our liberty against terrorism.
Today, improved emergency room care with high dose steroids, spinal protocols, immediate transfer to a neuro-intensive care unit, immediate neuro-surgical intervention, and a host of treatment improvements have markedly improved the SCI patient’s survival.
What remains a major management issue is spinal cord injury nerve pain. With improved survival in SCI the long term management of chronic pain remains challenging and frustrating. The rehabilitation of people with SCI and chronic pain is markedly reduced.

How Does It Happen?
The exact mechanism of pain in SCI is still incompletely understood. It would appear that spinal pain after SCI often worsens as healing occurs. People who have had a gunshot SCI seem to be at a greater risk for developing chronic spinal pain.
SCI is divided into Complete and Incomplete spinal cord injuries. The Complete Type results in total malfunction below the level of injury. The Incomplete Type has some residual function below the level of spinal injury (whether it be sensory function, motor function, or both).
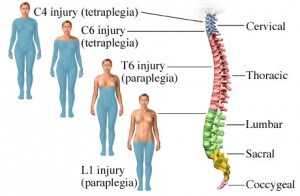
Curiously, people with the Incomplete Type are at greater risk for developing chronic spinal pain.
The possible mechanisms for chronic spinal pain are as follows:
- Nerve cells make new connections in the brain in response to SCI (called neuroplasticity).
- Nerve cells create new relationships with supportive cells (called Glial cells).
- Nerve cells become more easily excited.
- Nerve cells are less inhibited.
All in all, there are so many changes that occur it is difficult to sort out which ones cause the spinal pain syndrome. Also, there are many people with the identical injury that do not develop spinal pain.
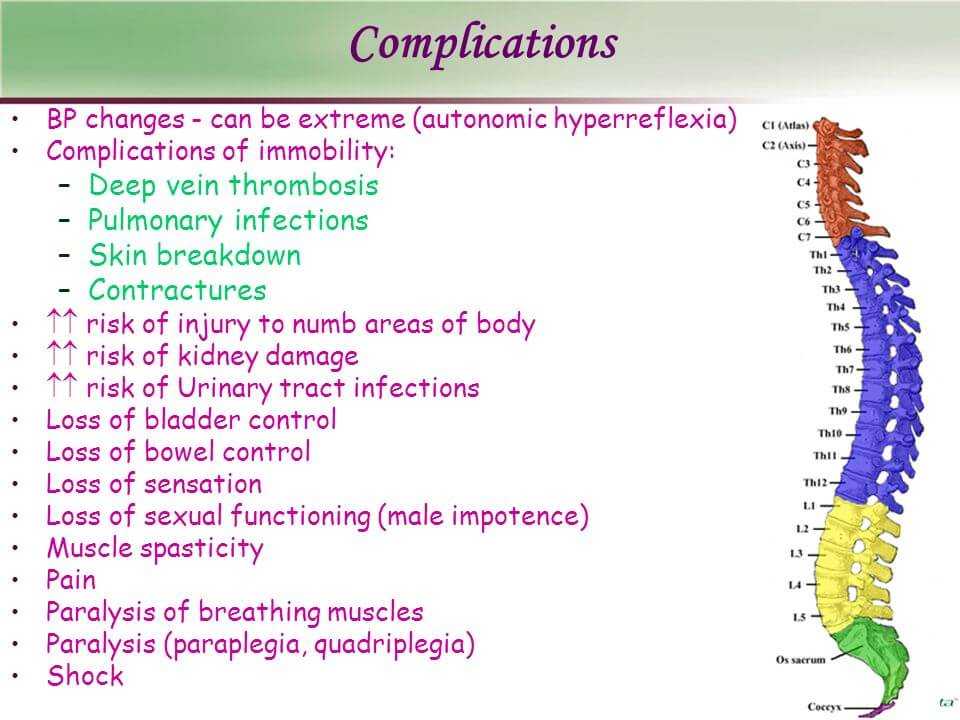
Why Does It Happen?
You might think that having a SCI would leave a person painless and paralyzed from the level of the spinal cord injury downward. As I said before, about 65% of people can have “pain” above or below the level where the spinal cord is injured.
The central nervous system is effected by many factors. It is the single most reactive organ system of your body to environmental stimuli. That re-activity has a certain amount of pre-programming genetically.
But it is not restricted to genetics. It will also change in response to the variations of stimuli from the environment. Imagine if your computer could “rewire” itself in response to the way you used it.
It could come with a built-in structure but, within a short time, it could adjust its structure according to the programs you used, or the internet searches you did, or even the way you interacted with it. Well…that’s what your central nervous system does.
And the number of combinations of changes possible? With 100 billion nerve cells, each with thousands of connections, each changing according to the environmental stimulus…the number and types of connections exceed the number of known stars and planets in the universe (no exaggeration).
What Can Be Done?
In order to intelligently treat the pain of SCI, it is subcategorized into 9 types. I will briefly describe each and its’ treatment:
1) Spinal pain: this is pain that arises from the bones, ligaments, and tendons of the spine. It is essentially musculo-skeletal pain. It responds to all the treatments that would work for a muscle pain and degenerative joint disease. Acetominophen, anti-inflammatories, and opiates all help this type of pain (click here to see my post on chronic back pain from degenerative disc disease).
2) Muscle spasm pain: this is pain that results from the prolonged contraction of a muscle. Though it will respond to the treatments for spinal pain, the most effective treatment is Baclofen. Baclofen is a muscle relaxer that is particularly well suited to treat muscular spasticity.
3) Overuse pain: this is pain that occurs in areas that sustain extra “wear and tear” due to the SCI. For instance, the shoulders and wrists are often injured in paraplegics (people with an SCI that results in leg paralysis). The therapies described in #1 would be useful for this type of pain.
4) Internal Organ pain: the person with a SCI can have a dysregulation of internal organ function. This is a vague but discomforting syndrome where the person may feel cramping or bloating. There is no specific treatment for this disorder. The episodes usually remit on their own.
5) Nerve entrapment pain: SCI patients can develop “pinched nerves” just as any other person. Their description of the pain will depend on the level of their spinal cord injury. The symptoms and treatment would be according to the nerve trapped.
6) Spinal Cord swelling pain (called syringomyelia): in this type of pain the spinal cord has swollen due to a blockage of spinal fluid flow. The patients will usually describe a burning pain. This syndrome develops years after the initial injury. Surgical treatment is the only effective option…the blockage has to be relieved.

7) Transitional Zone pain: this is a burning sensation that occurs on the border of the skin at the level of the SCI. It is treated with the medications that relieve other types of neuropathic pain.
8) Psychological pain: it goes without saying that depression, anxiety, etc. can be manifested as pain or worsen existing pain (click here to see my post on depression and chronic pain).
9) Central pain (called the central dysesthesia syndrome): I leave the most difficult of all the pain syndromes associated with SCI to the last. The mechanism for this pain syndrome is poorly understood and treated.
The SCI patient will complain of pain in the areas of anesthesia…below the level of the SCI. It is variously described as tingling, aching, squeezing, throbbing, etc.. The descriptions can be rather bizarre.
Other problems can make it worse…infections, anxiety, depression, weather changes, etc.. It is thought to be generated deep within the brain. It usually starts soon after the SCI and is found in about 33% of all SCI patients.
There is no currently reliable treatment for this formidable pain syndrome. The treating physician will have to be persistent in trying to find a combination of medications that may work.
Finally
Spinal cord injury nerve pain is a challenge to treat. I have reviewed the mechanisms and treatments at the present time. Much research is ongoing to improve the treatment of this mysterious malady. In most cases some relief can be achieved.
If you would like to ask me a question or comment, please below comment. I would love to hear from you.