Treating Sjogren’s Syndrome – Dry Eye

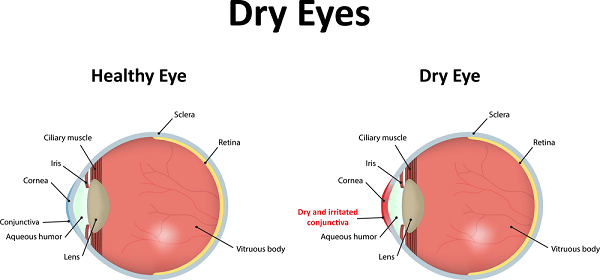
For some women, over-the-counter “artificial tears” can temporarily soothe dry eyes. However, these lubricating drops don’t have lasting effects and, in severe cases, must be used frequently, increasing the risk of problems from preservatives, says Janine Smith, MD, deputy clinical director of the National Eye Institute (NEI). Ocular lubricant ointments can be helpful if used before bedtime but can blur vision, causing problems during the day.
There are preservative-free and preservative-releasing drops available, including Refresh Tears (multidose), Bion Tears, and TheraTears. “TheraTears has also been shown to increase production of mucin in a rabbit model,” adds Dr. Smith. Some products provide the staying power of an ointment without blurring vision. “Lacrisert is a very tiny pellet, kind of like ointment in a pellet, that is placed between the eye and the lower lid, and it dissolves over a twenty-four-hour period. It’s only effective in patients who have some tears, because it needs tears to dissolve,” explains Dr. Smith. Several new gels have a consistency somewhere between eyedrops and ointment. GenTeal is a water-based gel and is among lubricants that contain “disappearing preservatives,” which break down once the product is exposed to air.

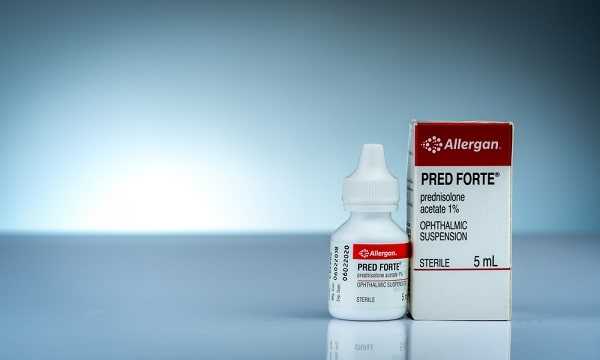
Corticosteroid eyedrops (such as Pred Forte and PredMild ) can also reduce inflammation. However, they can cause glaucoma and cataracts and are not safe to use for long periods. They are generally used as a short-term therapy for people who have not responded to other treatments. “If the eye is extremely inflamed, other measures won’t work. If you can bring down the inflammation, other treatments may have a better chance of helping,” says Dr. Smith.
Tiny silicone plugs (called punctalplugs) can be placed in your tear ducts near the corner of the eyes and can help tears stay around longer. “In women with Sjogren’s who have very low tear flow, punctal plugs may make things worse. If you have no outflow of tears, as the tears evaporate, inflammatory proteins can concentrate on the surface of the eye and cause discomfort. So you need to use other measures to keep the surface of the eye lubricated and flushed,” says Dr. Smith. In rare cases, the plugs can become contaminated and cause infections, and ducts may become damaged.
Special goggles for outdoor use decrease tear evaporation or slow it, adds Dr. Smith. Some goggles have special inserts or patches that increase the humidity around the eye. There are also plastic side shields for glasses and wraparound sunglasses. Humidifiers can make a big difference in the bedroom and elsewhere.
New therapies aimed at treating the underlying causes of dry eye are in the pipeline, including androgen eyedrops. “Animal data suggest that topical androgens may suppress lacrimal gland inflammation and correct the meibomian gland dysfunction in Sjogren’s syndrome, aiding tear formation and production of a lasting tear film,” explains Dr. Smith. “It’s also thought that androgens have anti-inflammatory properties, and that there’s a relative androgen deficiency locally in the eye that may allow inflammation to progress on the surface of the eye.”
There are also receptors for androgens and estrogens in the eyelid, the conjunctiva, the cornea, the lacrimal gland, and even in the retinal pigment epithelium. “We’re learning more about how complex the ocular surface is, and it’s not something that you can just rewet with a lot of water. Really what’s needed is something that will produce physiologic tears,” comments Dr. Smith.
Tests are under way of an experimental eyedrop preparation (INS365) that acts on receptors in the eye (P2Y2, purinergic receptors) that regulate and stimulate secretion of tears and mucin. “It causes an increase in fluid on the surface of the eye. It’s not tear fluid, but transudate, fluid that comes from underneath the conjunctiva that moves onto the surface of the eye. It results in an increase in tear volume on the surface of the eye by that mechanism. It’s the only drug that works that way,” says Dr. Smith. So far, the tests have not produced changes in outcomes.
The National Eye Institute at NIH and others have conducted a study of the antiinflammatory drug cyclosporine in eyedrop form (Restasis). Restasis may prevent T-cell activation on the ocular surface and in the lacrimal gland. The drops, being studied in Sjogren’s and in postmenopausal women with dry eye, increase tear production (seen in a Schirmer test). If approved by the FDA, Restasis would be the first therapy aimed at dampening the underlying inflammation of dry eye.
“Sjogren’s probably needs to be attacked from several fronts. Androgens would attack evaporative dry eye and lacrimal gland inflammation. Theoretically, if you increase the tear flow, you will increase the clearance of pro-inflammatory cytokines,” remarks Dr. Sullivan. “Using topical antiinflammatory agents, such as cyclosporine, you can decrease some of the inflammation on the ocular surface that exists because of the disease. It’s likely that some combination of therapies would be needed.”