Tylenol Side Effects

Have You Considered This?
So if a medicine is over-the-counter (OTC) it must be safe, right? Well, when you consider Tylenol side effects with the potential liver toxicity, kidney toxicity, skin toxicity, toxicity to the fetus, overdoses, emergency room visits, and hospitalizations all related to this substance, you might wonder how it ever became legal.
The American generic name for Tylenol is acetaminophen. Canada, Japan and a few other countries with close ties to the U.S. also use the same generic name.
However, the predominately used international name is paracetamol. The chemical name “American style” is N-acetyl-p-aminophenol (also called APAP). The name acetaminophen is a shortened hybrid of the chemical name.

Tylenol is the number one used OTC pain medicine in the U.S. This article will concentrate on the potential Tylenol side effects. But first, some brief history…
What is The History Of Tylenol?
The development of this substance occurred in 1852 by Charles Gerhardt, a French chemist. It was called acetanilide.

In 1899 Karl Morner (a German scientist) discovered that acetanilide was metabolized in the liver to the active compound acetaminophen.

The actual production of the direct compound came years later. However, widespread use did not occur until McNeil Laboratories (headquartered in Philadelphia, Pennsylvania at the time) marketed APAP with butabarbital as a prescription pain relieving medicine in 1953.
Shortly thereafter, Children’s Tylenol was released on the market by the same company (in 1955). It was offered as a safer alternative to aspirin for children.
In 2005 over 28 billion doses of Tylenol (or Tylenol combined with another medicine) were used by Americans.

How Does Tylenol Work?
One would think that for the long period of time APAP has been around we would have a detailed understanding of how it works…we don’t. We do know that it works on a category of chemical messengers called prostaglandins.
These local hormones modulate the transmission of pain signally and the production of a fever response in illness or injury. By blocking the prostaglandins, pain and fever can be blocked. This puts APAP in a category of medicines called NSAIDs (or non-steroidal anti-inflammatory medicines).
Although it is in the same class as aspirin and ibuprofen (Motrin), APAP does not affect the prostaglandin system in the same way. A very big difference is that the formation of stomach ulcers is not seen with APAP.
Furthermore, the clotting problems seen with aspirin and ibuprofen do not occur with APAP. All good news for APAP (and McNeil Laboratories).
What Is Tylenol Good For?
Important Note
THE FOLLOWING INFORMATION IS NOT INTENDED TO REPLACE THE NEED FOR A THOROUGH HISTORY AND PHYSICAL BY A LICENSED PRIMARY CARE PRACTITIONER BEFORE BEGINNING APAP THERAPY.
APAP is a very good medicine for pain and fever relief. The following is a partial listing of the conditions APAP may be good for:
- Tension Headache
- Migraine Headache
- Toothache pain(click here for my post on this topic)
- Temporomandibular Joint Syndrome (click here for my post on this topic)
- Earache pain
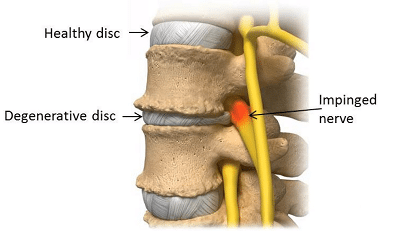
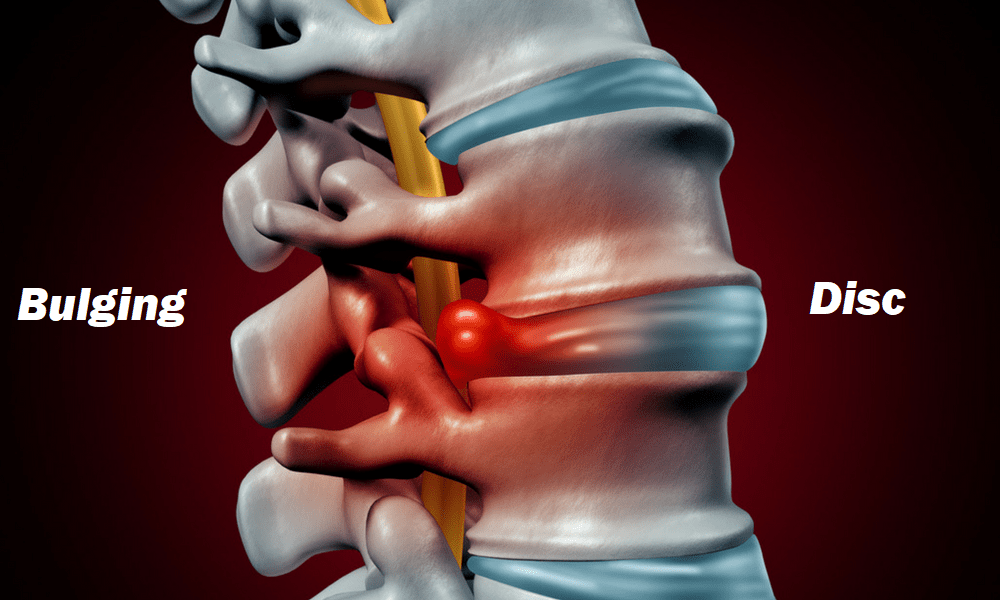
- Neck Pain
- Back Pain(click here for my post on this topic)
- Carpel Tunnel Syndrome (click here for my post on this topic)
- Degenerative Joint Disease(click here for my post on this topic)
- Rheumatoid Arthritis pain(click here for my post on this topic)
- Knee pain(click here for my post on this topic)
- Hip pain(click here for my post on this topic)
- Plantar Fasciitis pain (click here for my post on this topic)
- Ankle Sprain and Strain pain
- Menstrual pain
- Kidney Stone pain
- Costochondritis pain
- Pain Associated with Simple Bruises
- Fever
How Is Tylenol Dosed?
Here is a few table that outlines the proper Pediatric dosing for APAP:
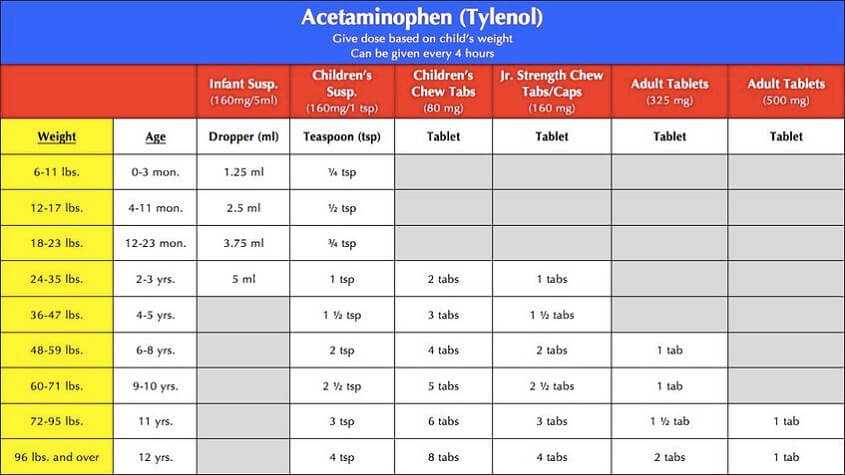
Remember that APAP is taken every 4 to 6 hours as needed.
What Are The Potential Side Effects Of Tylenol?
There are few acute side effects to APAP (other than what might be expected in an overdose). A good “rule of thumb” to follow with side effects is, “any negative change in condition after starting APAP requires immediate stopping of the medicine and evaluation by a licensed primary care practitioner or physician.”
People with pre-existing liver or kidney disease should only take APAP under the direct supervision of a licensed primary care practitioner or physician. That includes a history of alcoholism, drug abuse, and Hepatitis (any type).
You must also be very aware of the chronic medications you are be taking and any interaction that may occur with APAP. The supervision of your primary care practitioner or physician is essential to properly evaluate drug interactions.
APAP has over 160 different medications that it may interact with.
Special conditions such as pregnancy and nursing are also times to be very careful taking APAP. There have been reports of a higher incidence of Asthma in children of mothers having taken APAP during their pregnancy.
The following table reviews potential serious side effects:

To avoid a potential overdose or serious side effects consider the following:

Summary Remarks
I have reviewed Tylenol side effects as well as its history, mechanism of action, and indications. It is wisdom to remember that any medicine that has an effect will always have side effects.
There is no possible way to take a medicine without risk.
By following the basic information and dosing guidelines outlined in this monograph, Tylenol can be taken safely. It is a very effective pain reliever (4 regular strength 325 mg Tylenol tablets is equal to 4 mg of morphine in pain relief).
I trust this article has been informative and helpful. Please leave me a comment or question in the box below.
Wishing you joy and good health.