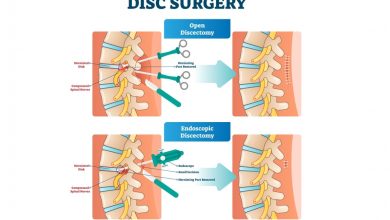
What is Endoscopic Discectomy ?
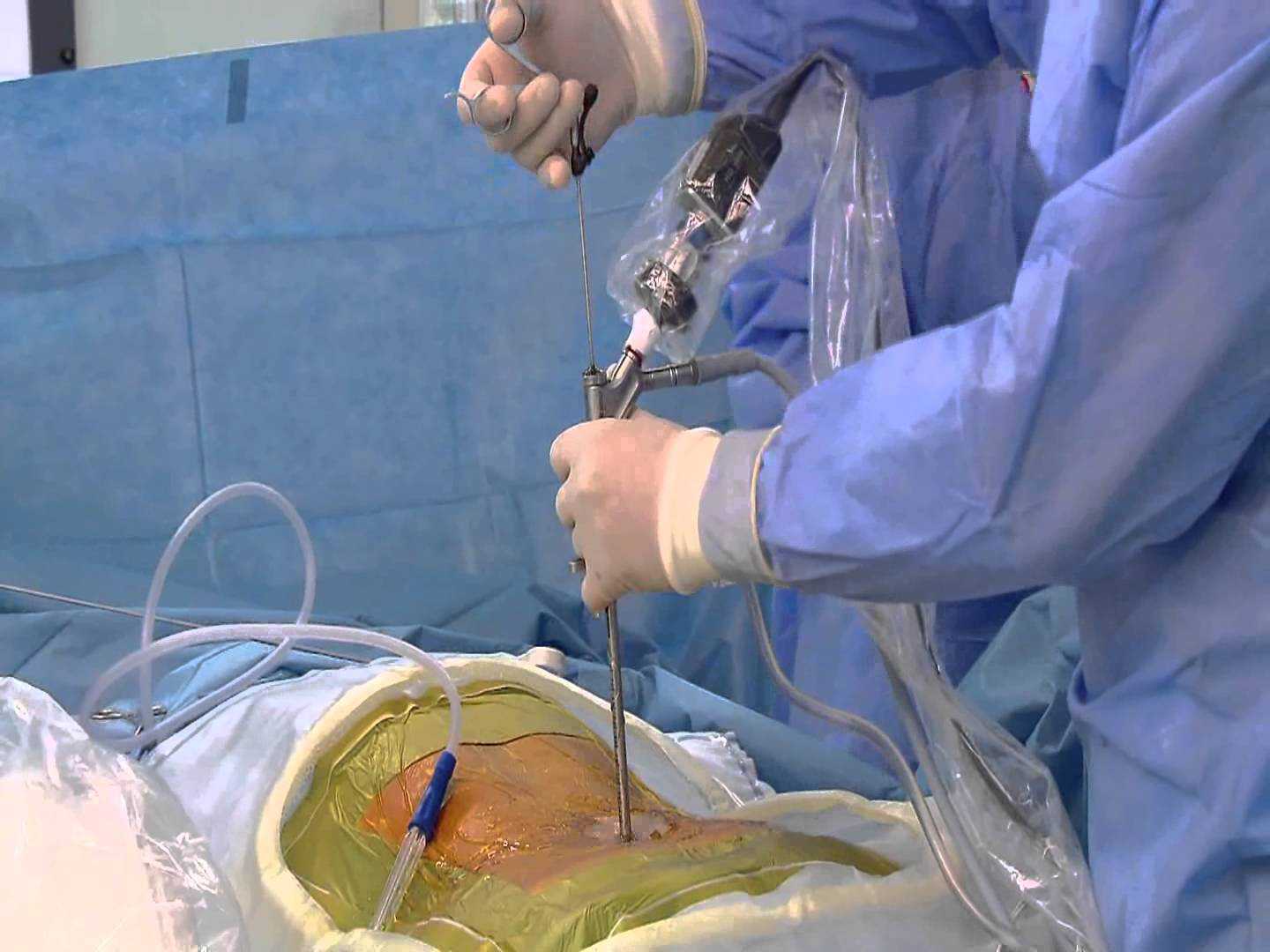
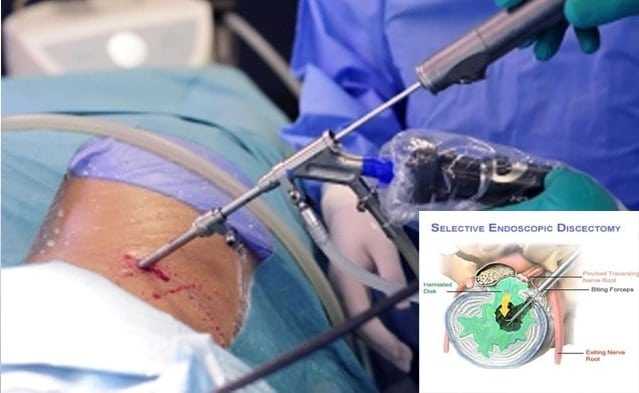
An endoscopic discectomy is the surgical removal of an intervertebral disk with an endoscope (a device consisting of a tube and optical system for observing the inside of a hollow organ or space. An endoscopic discectomy may be done through a small puncture opening).
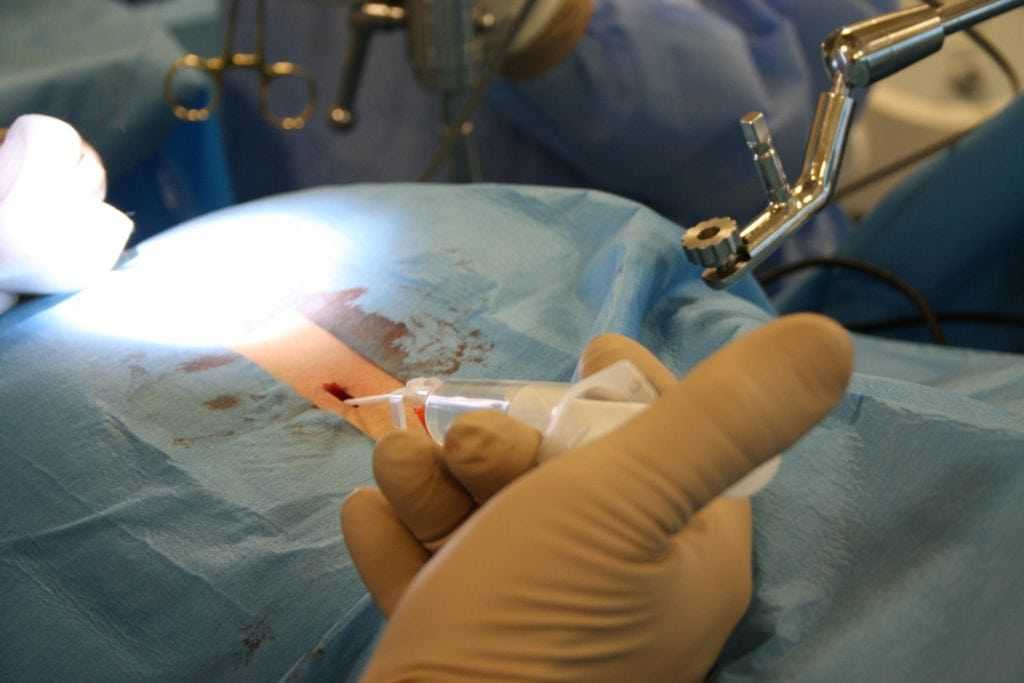
Endoscopic Discectomy is an outpatient surgical procedure to remove herniated disc material. Using local anesthesia with the help of x-ray fluoroscopy and a magnified video for guidance, a small specially designed endoscopic probe is inserted between the vertebrae and into the herniated disc space through the skin of the back. Tiny surgical attachments are then sent down the hollow center of the probe to remove a portion of the offending disc. Sometimes, the microsurgical attachments can be used to push the bulging disc back into place and be used for the removal of disc fragments and small bone spurs.
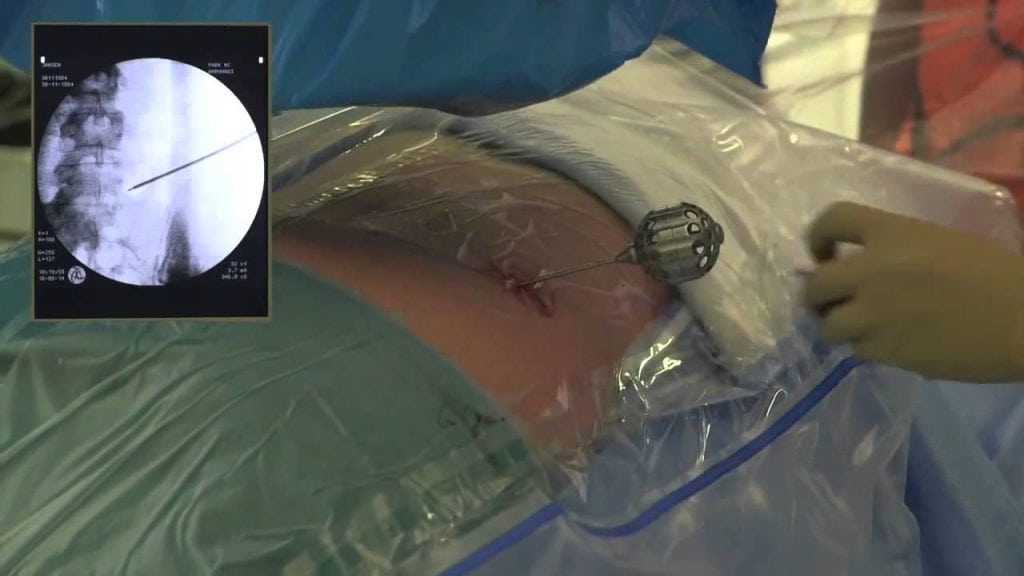
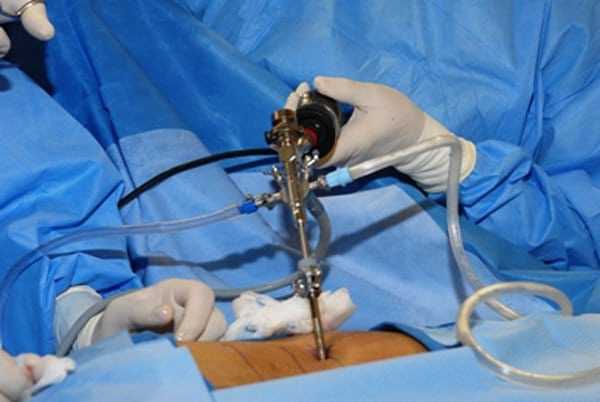
On average, the procedure takes about an hour. X-ray exposure is minimal. You normally will feel little, if any, pain or discomfort. There are no stitches. Upon completion, the probe is removed and a small Band-Aid is placed over the incision. The amount of nucleus tissue removed varies, and the supporting structure of the disc is not affected by the surgery. In comparison to large incisions required for open surgery, the access route to the disc in minimally invasive surgery consists of only the probe’s small puncture site, usually the size of a freckle.
An Endoscopic Discectomy is different from an open lumbar disc surgery because there is no traumatic back muscle dissection, no bone removal, and no large skin incision. The risk of complications from scarring, blood loss, infection, and anesthesia that may occur with conventional surgery are drastically reduced or eliminated with this procedure. Endoscopic Discectomy was invented to be an effective treatment for herniated discs while avoiding these risks.
Why Endoscopic Discectomy ?
- Major surgery is not the only alternative to living with back or leg pain, numbness or weakness.
- This procedure has provided relief for thousands, and it’s covered by most insurance
- NO STITCHES, NO GENERAL ANESTHESIA
- Most patients are discharged within three hours of the procedure with just a band-aid in place.
- Most patients who have the procedure on Friday return to work on Monday.