Women And Back Pain
Women can develop chronic back pain for several unique reasons that are different from men. There are a few obvious causes and some not so obvious. This article will attempt to explain 3 unique causes for women and back pain.

A case of chronic upper back pain:
Wendy (her name has been changed to protect her identity) came to my office with a complaint of upper back pain. She was an active person with no chronic medical conditions. A stay-at-home mother of 5 boys, ranging in age from 2 years old to 10 years old, she was busy. She described the pain as burning, daily, and excruciating at times.
The pain radiated into her arms making it difficult to hold a cup of water. She found herself dropping things without warning. She noted her grip strength had diminished. I asked her whether she was engaging in any activity that could be causing her pain…she adamantly denied any activity that was contributing to her chronic pain syndrome.
She denied any other changes in her health: there were no other joint issues, rashes, shortness of breath, or skin/nail changes. There was no recent history of any trauma and no family history of a similar syndrome in the female members of her family.
Her physical exam was remarkable for exquisite tenderness over the muscles and vertebrae from the 1st thoracic vertebra to the 5th thoracic vertebra. She refused any strong medicines and only wanted Tylenol.
I ordered X-Rays of the involved area which revealed nothing abnormal. A CT scan of the area was also unrevealing. By the 3rd visit she was very frustrated with me. She queried, “Doctor, you seem to be able to help everyone else with chronic pain…why can’t you figure out what is wrong with me?” I was stymied. Then something happened…
While we talked her 2 year old repeatedly climbed up in her lap, and slid down her legs as she held him. Over and over (perhaps 20 times in 10 minutes) Wendy repeated the action almost reflexively. I realized at that moment that Wendy had a syndrome called Thoracic Myofasciitis. She would have to change the way she picked up her son (and other boys).
I gave Wendy some advice about changing her activity with her son and some therapeutic exercises. Within several weeks her pain syndrome diminished and she was grateful (I was relieved).
I think it is safe to say most men would never suffer from Wendy’s syndrome (at least not for her reason). So let me describe for you 3 separate causes of chronic back pain that are unique for women.
3 Unique Causes Of Back Pain In Women
Disuse Myofasciitis Of The Upper Back
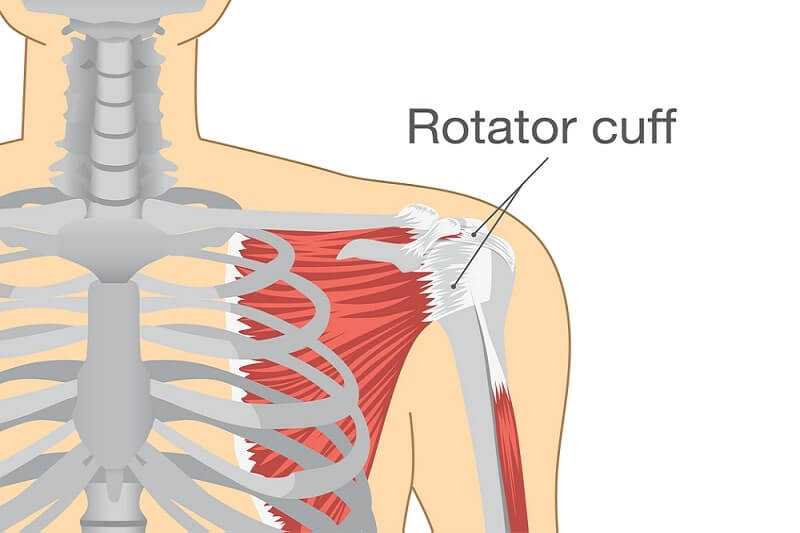
The spine is a very tightly arranged matrix of the spinal cord, muscles, nerves, ligaments, tendons, blood vessels, bones, and joints. Under usual wear and tear the matrix handles its work load quite well distributing the force over a large surface area.
However, in cases where excessive traction is applied (or repeatedly applied) the matrix can become inflamed. The inflammation can be quite painful and even irritate the nerves coming out of the spinal cord causing arm or leg weakness and a burning type of pain.

Once the myofasciitis is well established the pain can be constant. If the mechanical trauma causing the inflammation is not discontinued, the condition can be found to be very resistant to treatment. The actual mechanism for the excessive load must be changed. In Wendy’s case she didn’t even realize how her son’s activity was provoking the symptoms.
Many women experience variations of what Wendy experienced. In some cultures women carry their children all day while they work (I noticed that when I was traveling in Nepal.
…the women carried their infants while they worked in the rice patties). It is rare for men to have the same burden to carry their children.
In most cultures, the men have it easy when it comes to raising the children…

Myofasciitis of the Neck and Upper Back Due to Macromastia:
Most people admire the beauty of the female breast. Most women have at least a portion of their mystique attached to their breasts. Breast augmentation has become a billion dollar industry in the field of Plastic and Cosmetic Surgery. We have become a “breast obsessed” culture.

Some women have a genetic tendency to develop very large breasts called macromastia. Even women without the genetic tendency can find their breasts enlarging substantially in response to weight gain, pregnancy, and certain medications (the anti-depressant Paxil can do this).
The breasts are attached to the chest wall predominately with ligaments and skin. The real support for a woman’s breast comes from a series of ligaments called Cooper’s ligaments. Mostly due to the cumulative effect of gravity over time, a woman’s breast will stretch and “droop” over time. The heavier the breast the more likely this is to happen.

The ligamentous attachments of the breast to the chest wall cause the muscles, tendons, and ligaments of the upper thoracic spine to provide a counter-traction to the weight of the breasts. Persistent traction to the upper back can cause chronic pain (a myofasciitis). If this goes untreated a woman may even develop early arthritic changes (a form of degenerative joint and disc disease).
How much breast is too much (bigger isn’t always better)? The pathologic changes that cause pain and arthritis are most apparent when the combined breast weight reaches 3% or more of the total body weight of the person. The actual definition of macromastia can vary due to the body size and shape of any given person. In general, 1.3 pounds of breast tissue to 5.5 pounds of breast tissue is the starting weight for a breast where macromastia begins.
Most physicians would consider any breast weight above 3.3 pounds to be considered macromastia. Lower weights for macromastia would be considered in people who have symptoms related to excessive breast size even if they did not meet the 3.3 pound criteria.
The Lumbar Myofasciitis of Pregnancy:
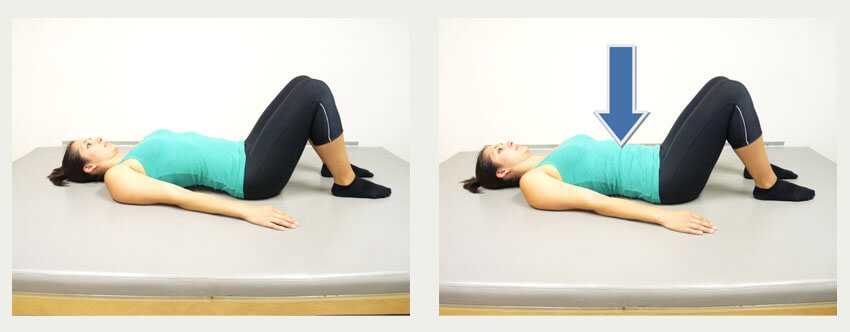
In pregnancy, the lower back curve (called the lumbar lordosis) is particularly strained on a woman’s body. In the normal state the lumbar curve sweeps forward and acts as a shock absorber during walking, running, and lifting.

With pregnancy, the enlarging uterus moves the center of gravity of a woman’s abdomen and pelvis forward causing the lumbar curve to become more accentuated. As the weight of the uterus becomes very substantial (in later pregnancy) the curve is dramatically increased. The large increase in the lumbar lordosis requires significant counter-traction by the muscles, ligaments, and tendons of the lower back.
This anatomical change in late pregnancy can induce a very severe myofasciitis of the lower lumbar area. Given the reluctance to give medicines in the pregnant state, doctors will often under treat the condition in favor of not inducing any side effects in the developing baby. The pregnant woman is often left in excruciating pain until she delivers.
Excessive weight gain, general deconditioning before pregnancy, and underlying medical conditions can make the myofasciitis even worse.
The good news is that the 3 aforementioned conditions are very treatable…so let’s discuss some options.
What Is The Therapy For The Three Unique Causes?
Disuse Myofasciitis of the Upper Back is treated by discontinuing the causative mechanism. Relief will not come immediately, however. The inflammatory process will take time to heal…as long as 4 to 6 weeks.
Anti-inflammatory medications and other medications can be helpful in the immediate treatment but, the cornerstone of therapy is mechanism reversal. I have previously written an article on exercises for back pain and would recommend you take a look at it to see some important exercise options (click here to see my post on back exercises).

As you read in the short case history about Wendy, some women may not even realize that their child rearing activities may be causing the pain. After all, that’s what mothers do naturally.
Macromastia is a surgical problem. Tight fitting support garments can reduce the traction effect of large breasts temporarily. However, real treatment will require breast reduction by a board certified Plastic Surgeon.
Plastic Surgeons differ in their abilities. There is a certain “artistic” quality to their results. As a rule I recommend plastic surgeons who have a long track record of good work in pleasing their patients. The technical know-how is not enough when it comes to Plastic Surgery…there is an artistic element that is hard to define.
The Lumbar Myofasciitis of Pregnancy is best treated with lumbar exercises, supportive garments (that pull the center of gravity backwards and support the pregnant abdomen), chiropractic manipulation, massage, and occasionally injections

Tylenol and Anti-inflammatories are actually quite dangerous for mother and baby. Recent studies have shown a significant increase in autism in the children given these medications. Medications that are usually safe in the non-pregnant state can have serious consequences if given during pregnancy.
Each medication is given a pregnancy rating (A, B, C, D, X) with “A” the least dangerous. Prior to administration, the prescribing practitioner should evaluate the medicine chosen for the pregnant woman for its pregnancy rating. Most clinicians will not choose a rating any higher than a “C” when used during pregnancy.
Note
The low back pain can be expected to persist for some time after delivery of the baby (you guessed it…around 6 weeks).
Finally
I have reviewed 3 common causes of back pain in women: Disuse Myofasciitis, Macromastia, and the Myofasciitis of Pregnancy. Though none of these maladies are life threatening they can be very uncomfortable.
In most cases, the treatments for these maladies are quite effective. Mechanism reversal is the primary treatment (as it is in most disease entities).
I hope you have found this article interesting and helpful. If you have any questions please send comment.
Wishing you much joy and good health.