About Osteoarthritis
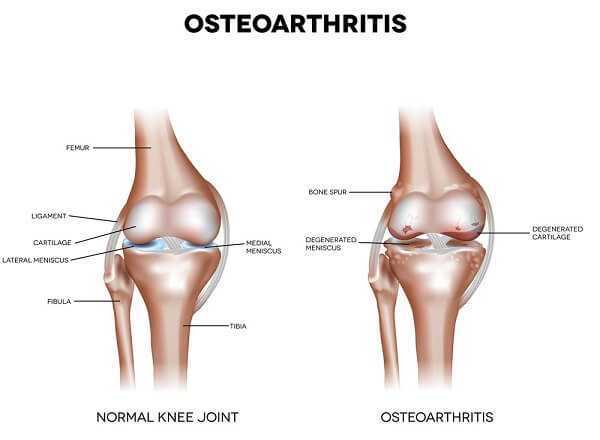
What is Osteoarthritis?
It is a degenerative joint disease. Here the healthy cartilage breaks down and wears away. This causes bone to rub against bone, leading to pain, swelling and loss of motion. Bony spurs and loose bodies, also form in the joint, leading to a feeling of grinding and crunching in the knee. All these symptoms may lead to disability and loss of quality of life.

Osteoarthritis Symptoms
Local symptoms are those of pain, stiffness, swelling and creaking. Some patients may exhibit symptoms like locking or giving way of the joint. Related problems are those of fatigue, disability, depression, anxiety.

How does it affect an individual’s life-style?
Though it is not a serious life-threatening disorder, it can affect the various aspects of one’s life.
At home
Simple activities of daily living like getting up from a chair or bed, walking stairs, using the toilet may be affected.
Social life
Hobbies, Family duties and having to change lifestyle expectations.
Occupational
Ability to do one’s job in the short and the long term.
Mood
May lead to depression and cause stress in life.
Sleep – quality of sleep may also be affected.
Carer – may affect the care giver, in many ways.
What happens to Osteoarthritic knees?
When a patient gets Osteoarthritis, there is a presumption that it invariably leads to severe progression. Though this can happen in a third of the patients, in many patients the symptoms may be static or even get better, as a result of the reparative response of the body.
Principles of Treatment
The doctor treating a patient with Osteoarthritis should take a holistic approach, in terms of assessing the effect of osteoarthritis on the individual’s function, quality of life, occupation, mood, relationships and leisure activities.
Patients should be educated on the disorder, its natural history and various management options available. The appropriate treatment option is instituted on an individual basis and reviewed on a regular basis, and if necessary, changes made accordingly.
Step 1
CORE – TREATMENT (Most Important)
The three options of Exercise, Physiotherapy and weight loss, form the most important aspect of management of Osteoarthritis. They should be part of any treatment that is being instituted towards osteoarthritis.
Exercise
Aerobic exercise – low impact exercise like cycling, walking, swimming Strength and resistance training. (Quadriceps strengthening)

Physiotherapy
*Quadriceps strengthening exercises
*Range of motion exercises
*Manual therapy like stretching
It is important that the exercise and physiotherapy are specific and prescribed, taking into account the patient’s interest, practicality and limitations. There should be a gradual increase to reach the desired level of activity. If at any point, pain of the joint is encountered, the intensity can be decreased to an acceptable level, rather than completely stopping it. Appropriate painkillers and other measures can be used to aid in the performance of exercise.

Weight loss
Increased body weight leads to increased transmission of load to the joints, leading to increased pain. It makes sense to keep the body weight to the optimum. This can be done by a healthy diet and regular exercise.
Step 2
If symptoms are not improving, your doctor may consider going to the next stage of simple medical interventions, in addition to Step 1 (Core-treatment).
Paracetamol
This has been shown to be an effective and a commonly used pain killer, in numerous studies. Due to its minimal side-effect profile, compared to other painkillers, this should be considered ahead of the others.
Topical Gels and Ointments (external application)
Anti-inflammatory and Capsaicin gels have been shown to be effective in early osteoarthritis. Capsaicin, extracted from chilli peppers, acts as a counter irritant on the skin. The local burning is said to block the pain pathways in the nerves, providing relief from the deep pain.
Step 3
There are various options in step 3, which should be used in conjunction with Step1 and may be Step 2.
Heat or Cold massage
Heat can be applied in the form of having a warm bath or by applying a hot water bag. Again cold can be applied in form of ice massage or ‘ice in a bag’ or frozen peas etc. Patients vary in terms of whether they respond better to heat or cold. Since it is cheap, easily accessible and with hardly any side effects, it can be definitely recommended as an adjunct to core treatment.
TENS
TENS produces selected pulsed currents which are delivered to the skin via electrode placement on the skin. These currents can activate specific nerve fibres potentially producing pain relief in some patients. Patients are advised to try it, and if they feel benefited, they could have more sessions. Though, it is generally offered by the physiotherapists, in some countries patients are encouraged to use them at home after appropriate training and supervision.
The following article may be of help.
AIDS and DEVICES
In-soles and shock absorbing footwear can aid patients in improving their symptoms due to arthritis.
Certain knee braces, can aid in off-loading the affected knee and help with symptoms.
Walking sticks, have been shown to improve pain and efficiency of walking. They act by distributing body weight through another point of contact on the ground. Walking frames are helpful, if the disability is significant.
There are modifications that can be done to one’s house, depending on their disability. These are things like raising your toilet level, having chairs that are high and having a banister (support) attached to your stairs etc.
SUPPLEMENTS
Glucosamine Sulphate and Chondroitin Sulphate are commonly prescribed in the management of arthritis. They are said to help in the synthesis of cartilage. There have been some studies done, where these have been found to be beneficial. They need to be taken for a period of 3 months, before evaluating their benefit.

Anti-inflammatory tablets
Your doctor may wish to start you on anti-inflammatory tablets along with or instead of paracetamol, for adequate pain relief. They should be prescribed at the lowest effective dose and for the shortest period of time. It is important to discuss about their possible side-effects. Most doctors will prescribe an additional tablet (proton pump inhibitor), for preventing gastric side effects.
Intra-articular Injections
Cortico-steroids
Synthetic cortico-steroids can be injected directly into the knee, to reduce the inflammation in the joint. They can be useful to settle symptoms in an acute flare up of osteoarthritis and buy the patient some time before other treatment modalities can take effect. But they should be used very sparingly, as repeated injections increase the risk of development of knee infection.
What is the best injection for knee pain ?
Hyaluranons
Hyaluranon in the normal joint, is found in the cartilage and the joint fluid. It aids in the maintainence of lubrication of the joint. Artificial hyaluranons have been manufactured and have been used in the osteoarthritic knee, with good benefit in some groups of patients. Again, the pros and cons should be discussed with the doctor.
ARTHROSCOPY
It is a surgical procedure, where a fibre optic camera is inserted into the knee and the anatomy is visualized in detail. It is very helpful, if there are mechanical symptoms like locking due to a torn meniscus or loose bodies in the knee.
TOTAL JOINT (KNEE) REPLACEMENT
If your symptoms continue to be bad and you have had no relief from the above mentioned options, your doctor may offer you a Total Knee Replacement. This is a surgical procedure, where the joint surfaces that are worn out are replaced with metal implants and an intervening polyethylene insert. You would need a General or a Regional Anaesthesia for this procedure.
In the appropriately selected patient, Total Knee Replacement offers excellent pain relief and great improvement in their quality of life. It is one of the most successful of operations, performed through out the world. Most people are extremely happy with the outcome.
https://www.youtube.com/watch?v=tKji04oFGdU
But as this is a surgical procedure, you have to familiarize yourself with the Pros and Cons, as well as the Dos and Don’ts, before embarking on one.