Microendoscopic Discectomy for Lumbar Disc Herniation: Systematic Review
Microendoscopic Discectomy for Lumbar Disc Herniation: Systematic Review
Lumbar disc herniation is a condition that can cause pain in the lower back and legs. A herniated disc occurs when the inner, soft tissue of the disc bulges out through a tear in the outer, tough layer of the disc. This can put pressure on nearby nerves, causing pain.
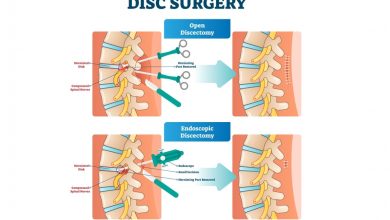
Microendoscopic discectomy is a minimally invasive surgical procedure used to treat lumbar disc herniation. In this procedure, a small camera called an endoscope is inserted into the affected area through a small incision. The surgeon then removes the herniated disc using special instruments.
A systematic review is a type of research that looks at all of the available evidence on a particular topic. In this case, the authors of the systematic review looked at all of the available evidence on microendoscopic discectomy for lumbar disc herniation.
The authors of the systematic review found that microendoscopic discectomy is an effective treatment for lumbar disc herniation. The procedure has a low rate of complications and a high rate of success in relieving pain.
Clinical Outcomes Following Microendoscopic Discectomy
It is estimated that up to 80% of people will experience at least one episode of low back pain in their lifetime. For many, the pain is acute and resolves on its own. However, for some, the pain becomes chronic and debilitating. If conservative measures fail to provide relief, surgery may be considered.
Microendoscopic discectomy is a minimally invasive surgical procedure that is used to treat herniated discs and other conditions that cause chronic back pain. The procedure is performed using a small microscope and specialized instruments.
The goal of microendoscopic discectomy is to relieve pain by removing the herniated disc material that is pressing on the nerve. The procedure is typically performed on an outpatient basis, and most people go home the same day.
There are several potential benefits of microendoscopic discectomy, including a shorter hospital stay, less pain, and a quicker return to normal activities. In addition, this procedure can be performed using local anesthesia, which eliminates the need for general anesthesia and the associated risks.
A review of the literature suggests that microendoscopic discectomy is associated with good clinical outcomes. One study showed that 94% of patients who underwent the procedure reported significant pain relief at their one-year follow-up visit.
Other studies have shown similar results, with patients reporting significant pain relief and improved function at their one-year follow-up visit. In addition, microendoscopic discectomy has been shown to be a safe and effective procedure, with a low risk of complications.
If you are considering microendoscopic discectomy for the treatment of your chronic back pain, be sure to discuss the risks and benefits of the procedure with your surgeon.
Risk of Complications Following Microendoscopic Discectomy
Microendoscopic discectomy is a minimally invasive alternative to conventional open back surgery. It is typically performed as an outpatient procedure and involves a small incision in the back. A microscope and special instruments are used to access and remove the herniated disc material.
The minimally invasive nature of microendoscopic discectomy results in less tissue damage, blood loss, and scarring. It also typically has a shorter hospital stay and quicker recovery time compared to open back surgery.
There are potential risks and complications associated with any type of surgery, however, and microendoscopic discectomy is no exception. The most common complications following this procedure are infection, bleeding, and nerve damage.
While the risk of complications is relatively low, it’s important to be aware of the potential risks before undergoing any surgery. Be sure to discuss all potential risks and complications with your surgeon prior to having microendoscopic discectomy.
Lumbar Disc Herniation: Overview
A lumbar disc herniation is a condition that affects the discs in your lower back. These discs act as cushions between the vertebrae in your spine, and they can become herniated when they are damaged or torn. This can cause a number of different symptoms, ranging from mild to severe.
Most lumbar disc herniations occur in the lower back, but they can also occur in the middle or upper back. The most common symptom of a lumbar disc herniation is pain. This pain can be mild or severe, and it may radiate into your legs or arms. Other symptoms can include numbness, tingling, weakness, and muscle spasms.
If you have any of these symptoms, it’s important to see a doctor right away. They can diagnose your condition with a physical exam and imaging tests, such as an MRI. Once you’ve been diagnosed, your doctor will work with you to develop a treatment plan.
Microendoscopic discectomy is a minimally invasive surgery for lumbar disc herniation. In this procedure, a small incision is made in the back, and a microscope is used to guide the surgeon to the herniated disc. Once the disc is located, a portion of it is removed. This relieves pressure on the nerves and can help to improve symptoms.
If you have a lumbar disc herniation, there are a number of treatment options available. Talk to your doctor to find out what’s right for you.
Parameters of Microendoscopic Discectomy
There are many factors that go into microendoscopic discectomy, and the procedure itself is very delicate. The surgeon must have a great deal of experience in order to ensure that the patient receives the best possible care.
The first factor is the size of the herniated disc. If the disc is too large, it may not be possible to remove it without damaging the surrounding tissue. The second factor is the location of the herniated disc. If it is located in a difficult-to-reach area, it may be necessary to use a microscope to see the disc and surrounding tissue.
Once the surgeon has determined that the herniated disc can be safely removed, he or she will make a small incision in the patient’s back. Through this incision, the surgeon will insert a small camera, called a microendoscope. This camera will allow the surgeon to see the herniated disc and the surrounding tissue.
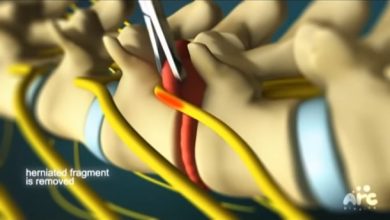
Once the herniated disc has been located, the surgeon will carefully remove it. In some cases, the surgeon may also need to remove some of the surrounding tissue. This tissue is called the annulus.
After the herniated disc has been removed, the surgeon will close the incision with sutures. The patient will then be taken to a recovery room where he or she will be monitored for a short time.
Microendoscopic discectomy is a safe and effective way to treat herniated discs. The procedure has a very high success rate and most patients are able to return to their normal activities within a few days.
Advantages of Microendoscopic Discectomy
Microendoscopic discectomy is a minimally invasive surgical procedure used to treat herniated discs. The method involves making a small incision in the back and insert a tiny camera called an endoscope. This allows the surgeon to see the disc and surrounding structures without having to make a large incision.
There are several advantages of microendoscopic discectomy over traditional open surgery. One advantage is that it is less invasive. This means that there is less risk of infection and a shorter hospital stay. There is also less pain and scarring following the surgery.
Another advantage of microendoscopic discectomy is that it is less disruptive to the surrounding tissues. This results in a quicker recovery time and less risk of exacerbating other conditions such as spinal stenosis.
Microendoscopic discectomy has shown to be effective in treating herniated discs. In most cases, patients are able to return to their normal activities within a few weeks. The procedure is also associated with a low recurrence rate.
If you are considering surgery for a herniated disc, talk to your surgeon about the benefits of microendoscopic discectomy.
Limitations of Microendoscopic Discectomy
Microendoscopic discectomy (MED) is a new surgical technique for the treatment of herniated discs. The main advantage of this technique is that it allows for a minimally invasive surgery with a small incision. Studies have shown that this technique is as effective as the conventional open discectomy technique and has a lower complication rate.
However, there are some limitations to this technique. One of the main limitations is that it can only be used for certain types of herniated discs. This technique is not suitable for patients with very large herniated discs or those who have disc herniations that are difficult to access. In addition, this technique is not recommended for patients who have had previous disc surgery.
Another limitation of this technique is that it is not available at all hospitals. This technique requires special equipment and training, which means that not all hospitals are able to offer this treatment. This can make it difficult for patients to find a hospital that offers this treatment.
Despite these limitations, microendoscopic discectomy is a promising new technique that offers a minimally invasive option for the treatment of herniated discs.
Overview of Related Studies
A herniated disc can occur anywhere along the spine, but most commonly affects the lower back. The discs act as shock absorbers for the spine, absorbing the impact of body movement. A herniated disc occurs when the outer layer of the disc ruptures and the inner jelly-like material leaks out. This can put pressure on nearby nerves and cause pain.
Microendoscopic discectomy is a minimally invasive surgical procedure used to treat herniated discs. The surgery is performed through a small incision in the back and does not require the removal of any bone or muscle. A tiny camera called an endoscope is inserted through the incision and used to visualize the herniated disc. A small probe is then inserted and used to remove the herniated disc material.
The majority of patients who undergo microendoscopic discectomy experience a significant reduction in pain and a quick return to normal activity. The surgery is considered very safe, with a low risk of complications.
If you are experiencing pain caused by a herniated disc, talk to your doctor about whether microendoscopic discectomy might be right for you.
Evaluation of Study Quality
The quality of a study is important to consider when trying to determine the validity of its results. There are many factors that can affect the quality of a study, and it is important to take all of them into account when judging the credibility of its findings.
One of the most important things to consider is the study design. Different designs have different strengths and weaknesses, and some are more likely to produce valid results than others. For example, randomized controlled trials are generally considered to be the gold standard when it comes to scientific research, as they are the best at ruling out confounding factors. Observational studies, on the other hand, can be useful for generating hypotheses but are not as good at providing definitive proof.
Another important factor to consider is the sample size. Generally speaking, the larger the sample size, the more reliable the results. This is because a larger sample size provides a more representative sample of the population and is therefore more likely to be accurate.
The quality of the data is also important. Studies that use data that has been collected in a well-designed and reliable manner are more likely to be accurate than those that do not. This is why it is important to use reputable sources when collecting data for a study.
Finally, the statistical methods used to analyze the data can also impact the quality of a study. Studies that use more sophisticated methods are usually more reliable than those that use simpler methods. This is because more sophisticated methods are better able to control for confounding factors and eliminate bias.
When evaluating the quality of a study, it is important to consider all of these factors. The overall quality of a study can be judged by how well it meets all of these standards.
Discussion of Findings
A “Discussion of Findings” is a chance for your surgeon to go over what they found during your microendoscopic discectomy. This is an important step in the process because it allows you to understand what was going on with your spine and what the surgeon did to correct the problem. It also gives you an opportunity to ask any questions that you may have about the surgery or your recovery.
During a microendoscopic discectomy, the surgeon will make a small incision in your back and insert a tiny camera called a microendoscope. This camera will give the surgeon a clear view of your spine and the surrounding structures. The surgeon will then remove the herniated disc material that is pressing on your nerve root. Once the material is removed, the surgeon will place a small piece of bone or a synthetic graft to replace the disc material.
The “Discussion of Findings” is an important step in the microendoscopic discectomy process because it allows you to understand what was going on with your spine and what the surgeon did to correct the problem. It also gives you an opportunity to ask any questions that you may have about the surgery or your recovery.
Conclusion
There are many ways to remove a herniated disc. The most common and most successful method is microendoscopic discectomy. This is a minimally invasive surgical procedure that is performed through a small incision in the back. The surgeon inserts a tiny camera, called a microendoscope, into the incision. The microendoscope gives the surgeon a clear view of the herniated disc and the surrounding area. The surgeon then uses small surgical instruments to remove the herniated disc.
Microendoscopic discectomy is a very effective procedure for herniated disc surgery. The vast majority of people who have the procedure done experience a substantial reduction in pain. In addition, the procedure has a very low risk of complications.
If you are considering herniated disc surgery, microendoscopic discectomy is definitely worth considering. It is a minimally invasive procedure with a very high success rate.