Chronic Pain Medication and Addiction

I am going to try and do the impossible. In one short article I am going to explain the anatomy and physiology of addiction. I will also attempt to show the dynamic between chronic pain medication and addiction.
To put into perspective for you what I am trying to do, it would be like asking a theology student to define God and give 3 examples on an essay test question. The task would be daunting, to say the least.

But you see, everywhere I looked in my research for this monograph I found either too complicated a discussion on the topic of chronic pain medication and addiction, or too little information given, or a totally biased rendering of the facts.
There can be no doubt that there has been a substantial rise in the number of people overdosing from prescription pain medications over the past decade or more. However, there has also been a substantial improvement in the treatment of chronic pain over the same time period.
If you grew up in a small town like Kenmore, New York (where I grew up), you may have noticed that the number of car accidents was really few in your town. But when I moved to Philadelphia, Pennsylvania, I noticed there were car accidents all the time. Did the danger from automobiles change from Kenmore to Philadelphia?
Of course not…with more traffic you have more accidents…so it is with chronic pain medication and addiction. We are not planning on limiting the number of cars that people are allowed to drive in Philly are we…so why would we limit how much medicine a person can take who has chronic pain (within the parameters of acceptable side effects)?
Using the same metaphor, cars are more lethal the more irresponsibly you drive them. The over doses that are seen with prescription pain medications are mostly due to abuse of the medications…like driving too fast for the road conditions.
In the next section I am going to take you to medical school for a moment and teach you some neuroanatomy of addiction.
The Neuroanatomy Of Addiction
There is a brain signal equivalent to every behavior a human manifests. That means, there is a signal pattern to the neurons of your brain when you are in love, angry, creative, and even when a person is an addict.
That signal pattern occurs in unique areas of the brain. We can measure how the pattern is different when you compare a normal brain and a brain of someone with a substance abuse issue.
These areas of the brain connect with each other to create the condition of substance abuse. The brain actually learns to make the “hookup” under special conditions.
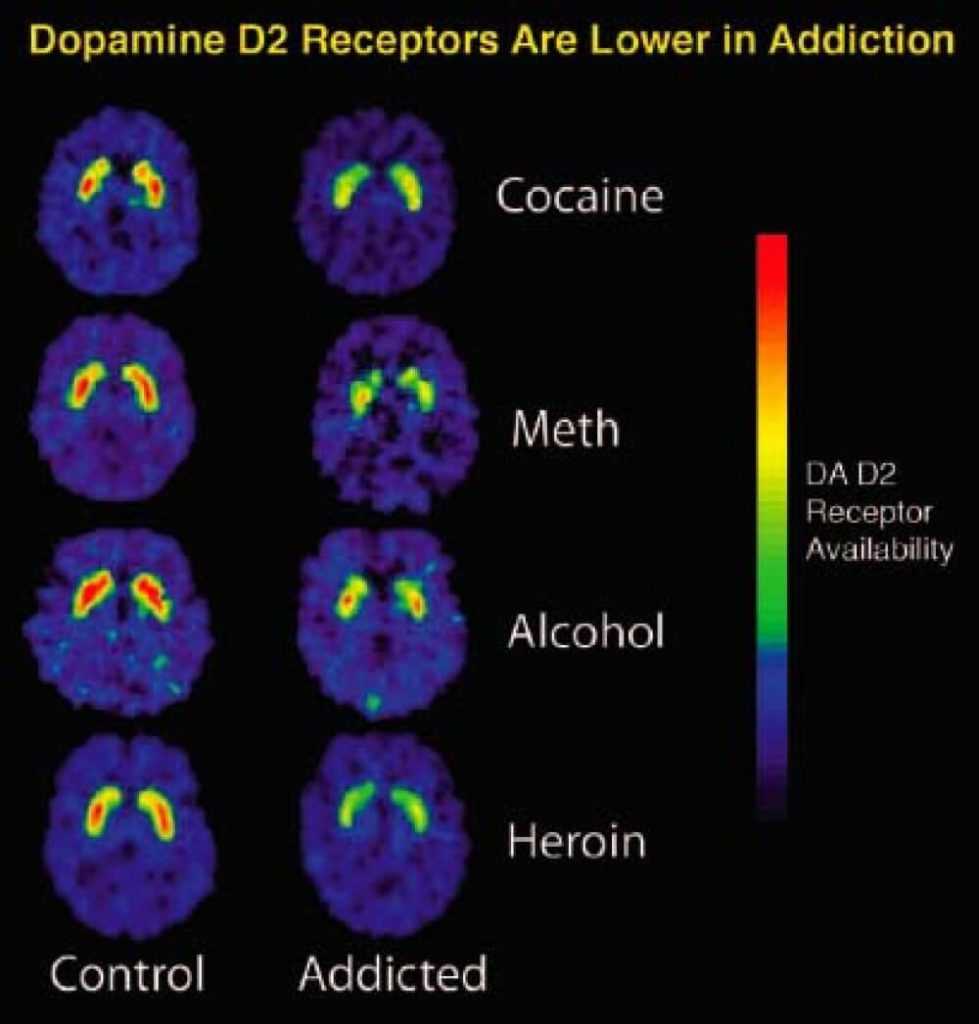
The “hookup” occurs differently for different people (though there are similarities). Your genetics, personal experiences, disposition, and intellect are just a few of the conditions that effect whether an “abusive hookup” is going to occur.
In reality, the brain of a person with a substance use disorder (previously known as an addiction) has a brain that is structurally different from others. That is the bad news.
The good news is that our brain structure can change through training it. That is called neuroplasticity (and unlike what you may have heard before…your brain never stops changing). The addicts brain can heal.
The Neurophysiology Of Addiction
Nerve cells are social. They really like to “talk” to each other and do so continuously. In fact, if a nerve cell does not have “conversation” it dies.
The nerve cells of your brain are continuously “talking” with electrical and chemical conversation. The chemical conversation is the favorite for nerve cells. This occurs at a place called the “synapse” (see the image).
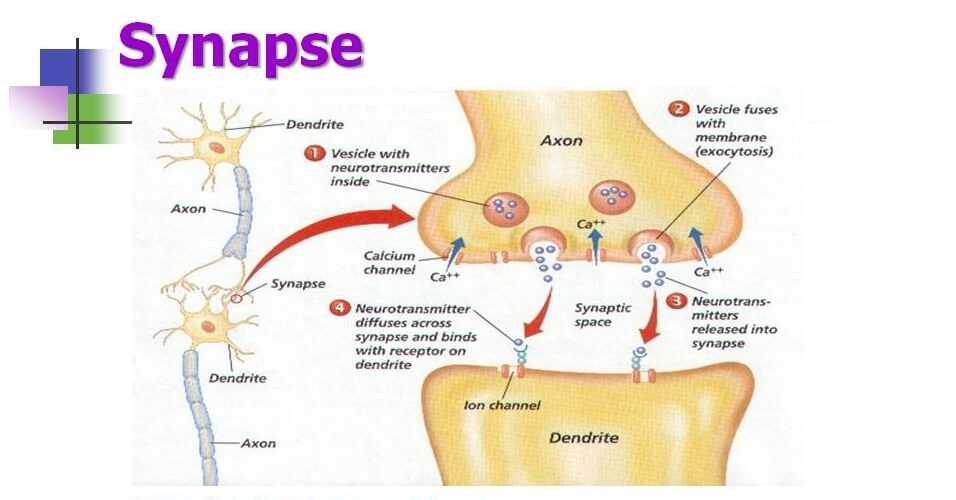
The “synapse” is a specialized space between 2 neighboring nerve cells (like 2 neighbors in a community with the homes close to each other speaking through an open side window). The space is really small between the 2 cells (making it easy to talk to your neighbor).
In substance abuse, the conversation becomes very one sided. The chemicals that the nerve cell uses to communicate (called neurotransmitters) are either too high or too low for the needed conversation. The drug has effected the synapse directly or indirectly.
The favorite chemical to disrupt in substance abuse is called Dopamine. It is used when the nerve cells want to have a conversation about pleasure. You can understand why it is their favorite..
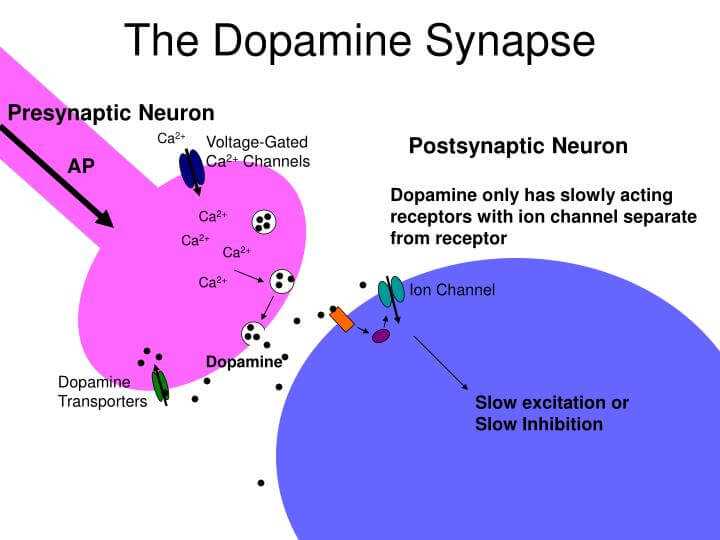
Of course, there are many other neurotransmitters that we could discuss. The process is just a “wee bit” more complicated than I am making it…but you get my point.
Substance abuse is not only a structural problem; it is also chemical. Until the structure and chemistry of the brain can be healed, the substance abuse behavior lingers
The Data Regarding Causing Addiction With Prescription Opiates
It is expected that people would believe that the problem with opiate overdoses is the opiates. Taken to the extreme, if you could remove all opiates you would never have another opiate overdose, right? Or remove all the cars and never have another traffic fatality.
Yeah, well, that is one of those hypotheticals that border on the absurd. The real issue with substance abuse is not the substance, it is the abuser (or maybe the driver).
Of course, opiates induce a host of neurochemical changes in human physiology. But those changes need to be understood and managed.
Did you know that most physicians in practice today had less than 10 total hours of pain management training during their medical education? Those are the same doctors who are being expected to understand how to treat chronic pain.
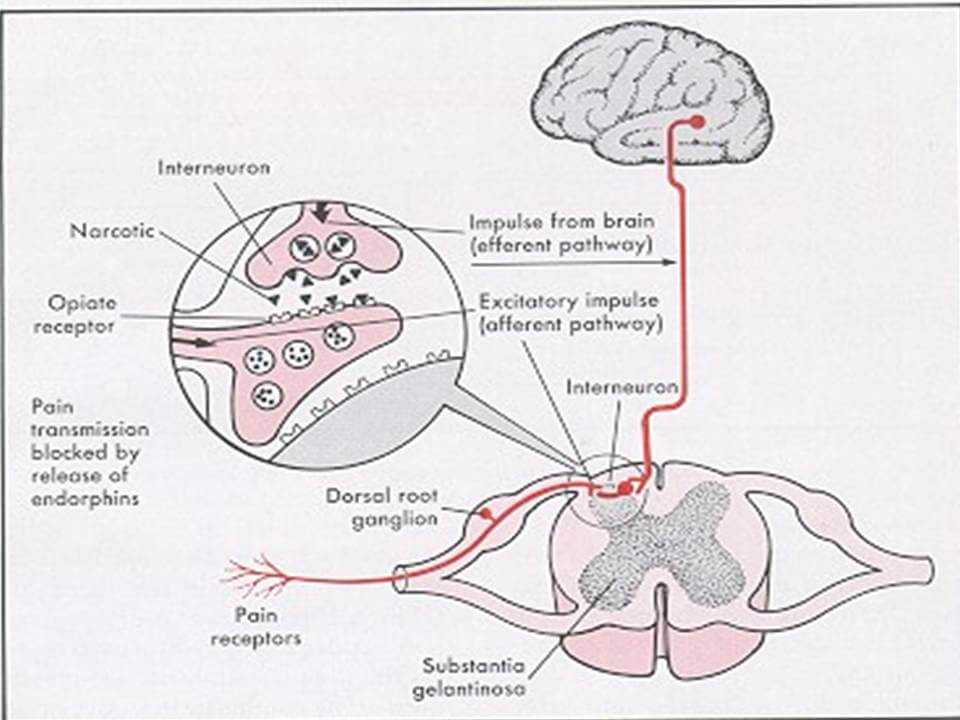
In 2007 Edlund et al. published a study which looked at 15,000 veterans who took opiates for pain. They noted a 2% incidence of conversion to substance abuse (98% did not become addicts…it is rare to have a 98% success rating in anything).
The actual incidence of opiate substance abuse in the U.S. is probably around 15% (and has been since the Civil War).
The Center For Disease Control (CDC) Recommendations Regarding Treating Chronic Pain With Opiates
In March 2016, the CDC published their long awaited guidelines for primary care practitioners. The recommendations sent a chill through the medical providers who are treating pain with opiates.
Essentially, there was a concerted effort on the part of the many opiophobic expert panel members for the CDC to limit and restrict the amount of opiate pain medicine that should be prescribed.
Though the panel consisted of no pro-opiate therapy experts, no pain patients successfully treated with opiates, and had a panel member who has profited substantially helping law firms litigate the drug companies that manufacture opiates, the recommendations were published anyway.
My belief is these recommendations will make it even more difficult for legitimate chronic pain patients to obtain the opiate pain medications they so readily deserve.
Does Being An Addict Disqualify a Person From Opiate Pain Medications?
What about the substance abuser who has chronic pain unrelieved with other therapies? Are they disqualified from opiate pain medications?
In the medical community that I practiced in they would be. Not only are most people with a history of substance abuse stigmatized but they are often excluded from any therapy that is potentially habituating.
Left with no other pain management alternatives, the addict in recovery will often relapse in their search for pain relief. Are they really to blame? This issue gets little attention in the main stream media.
My Recommendations Regarding Treating Chronic Pain With Opiates
I have reviewed with you some basic principles of anatomy, physiology, current literature, and current controversies in chronic pain medication and addiction. The following are several of my recommendations for addressing this issue:
- Reconvene the CDC panel and include a more balanced representation of opiate therapy prescribers and patients. Temporarily rescind the present recommendations (re-instate them if the more diverse panel comes to the same conclusions).
- Federally mandate all medical schools and residency training programs to include a comprehensive curriculum in pain management and substance abuse (consider doing so in all nursing and allied health professional schools too).
- Federally decriminalize all personal use of drugs in favor of pro-active law enforcement for referral to drug rehabilitation. Reserve incarceration for violent drug offenders and illegal distributors.
- Emphasize intensive screening for all people who require chronic opiate pain medicine as therapy. This would include teaching providers how to implement and interpret the screening methods (with established and published standards).
I believe these 4 changes would produce a gradual reduction in the number of people who are hurt or die from substance abuse issues.
This would also allow providers to treat the millions of Americans who suffer from chronic pain and have opiate pain therapy as their only reliable way of obtaining pain relief.
I hope you have found this monograph provocative. If you have any further questions, please comment. I would love to hear from you and will answer you promptly.
To your health.





Do you honestly believe the cdc is going to change there attitude towards chronic pain sufferers. I’ve said this before they are using addicts who did supposedly over dose on opoids. They need to realize addicts can and will find other meds like cocaine,meth, crank,and anything they can find. Taking the opoids away from them are not going to stop them from finding something else that will kill them. They will take whatever they can find. I have been hearing things about the drug dealers are making a pain pill that looks just like Vicodin or something similar only it has fenytal in it and is causing more deaths to whoever buys them off the street. This is going to cause chronic pain sufferers who have to live the rest of there lifes with horrible pain. They are taking away the one thing that gives some quality to there lifes. With out that there will a lot more suicides because we won’t be able to live with that kind of pain. Yes I’m one of the chronic pain sufferers. It should be taken into consideration that we all live with other chronic diseases besides. For example I was diagnosed with Fibro in 1998 since then I have gotten a very rare form of psoriasis that which is the only known skin disease that’s a emergency in can put you in the hospital and it can kill you it’s autoimmune disease,also I have had cancer twice in the last eight years,breast had mastectomy 2 years later I got lung cancer stage 3 in lympnodes. Had left upper love removed I turned down radiation i was told it would mess my esophagus up and I would have to be tube Fed and it would mess up my good lung. I took 6 months chemo I am now a six year cancer survivor and advocate I am also an advocate for chronic pain sufferers. Some thing has to change before there are a lot more people dying because they can’t live with the pain without an opiate to ease it so they have any quality of life. From a chronic pain sufferer an advocate.
Hello Susan…thanks for your comments. Can you imagine formulating recommendations that will literally effect millions of Americans and not including every point of view. Where is the intellectual honesty of the CDC? My respect for them has lessened considerably.
The people who are suffering needlessly with severe chronic pain every day, need someone who will represent us in a class action lawsuit against the CDC, DEA and the administration in the Whitehouse for what they have done to millions of people accross this country! The sheer ignorance of everyone of them is astounding! We need help and right away! There will certainly be a epidemic of suocide, as people will not be able to tolerate living in pain 24 hours a day, everyday! And who will we see about that?! It will take these corrupt government agencies, if ever, 10 years to see what they have caused and even then, they will not admit it on their own, or do anything about it! Why are the professionals in the medical community not sticking up for their patients and bringing these agencies to task? What happened to “do no harm”? You would think their Hippocratic oath would make them feel some sort of obligation to tell the truth about the situation we are in at this time! But no, they are just silent and jumping on this ridiculous bandwagon and are complicit in this outrageous act of torture! Shame on them all, and I hope either in this life or the next, they also will be held accountable for torture that is inhumane and unforgivable! PLEASE someone has to help us immediately as there is no time to waste.
I say the statistics are not accurate as far as patients of pm clinics are concerned. Treating physically dependantcy for pain management and comparing that to heroin and drug abusers is totally wrong unfair and unethical. Many medications can cause withdrawl symptoms like prednisone ,trazodone and antidepressants to name a few . Most medications have a list a mile long of side effects. Especially new meds. Some soon become subjected to lawsuits. Opiates have been used for several decades. Yes they can cause serious addiction but with physicians care and monitoring its no worse than some other options. You Dont want patients to have to self medicate! If you ever had an abcess tooth you know you would do anything to get that pain to stop! Dont put chronic pain sufferers in the same category as drug abusers. Its just wrong!