Degenerative Disc in the Neck
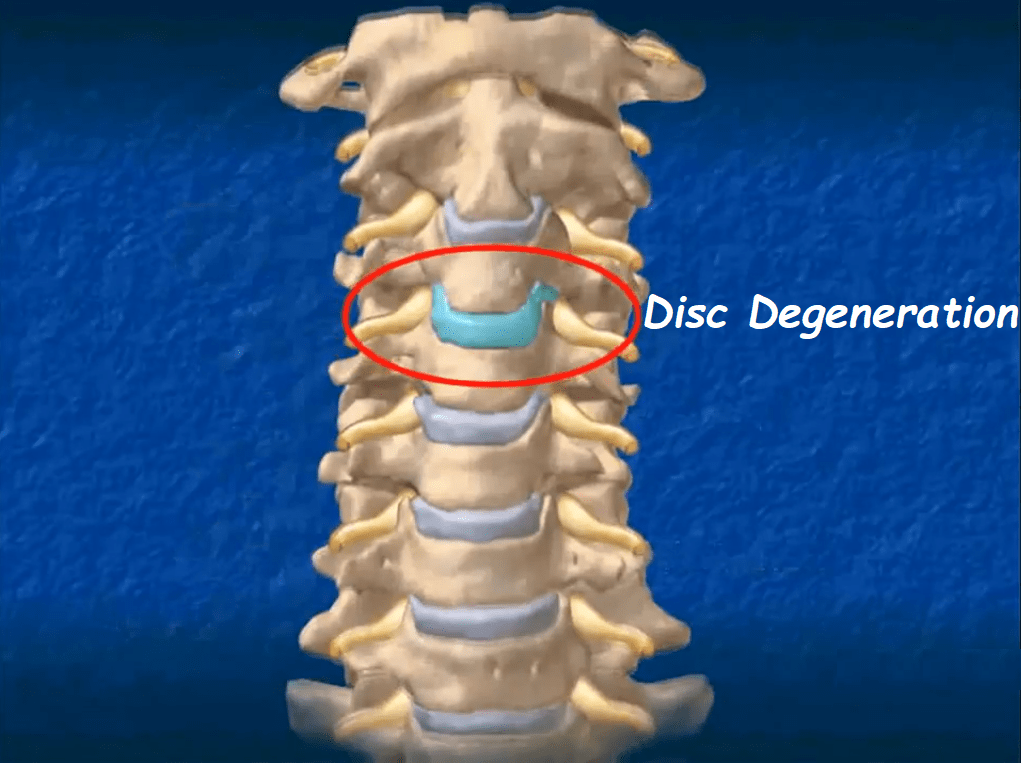
Cervical Degenerative Disc
A cervical degenerative disc is located in the C1-C7 area of the spine, which includes the neck and upper back. Although the lumbar spine is most at risk for degenerative disc disease due to its weight bearing role in everyday activities like lifting and twisting, the neck is also a common area in which this condition can present itself.
Degenerative disc disease is a term used to describe wear and tear on the spinal discs. Discs with this condition lose water and become more brittle, not only reducing the amount of cushion between vertebrae, but also making the sufferer more susceptible to developing other issues
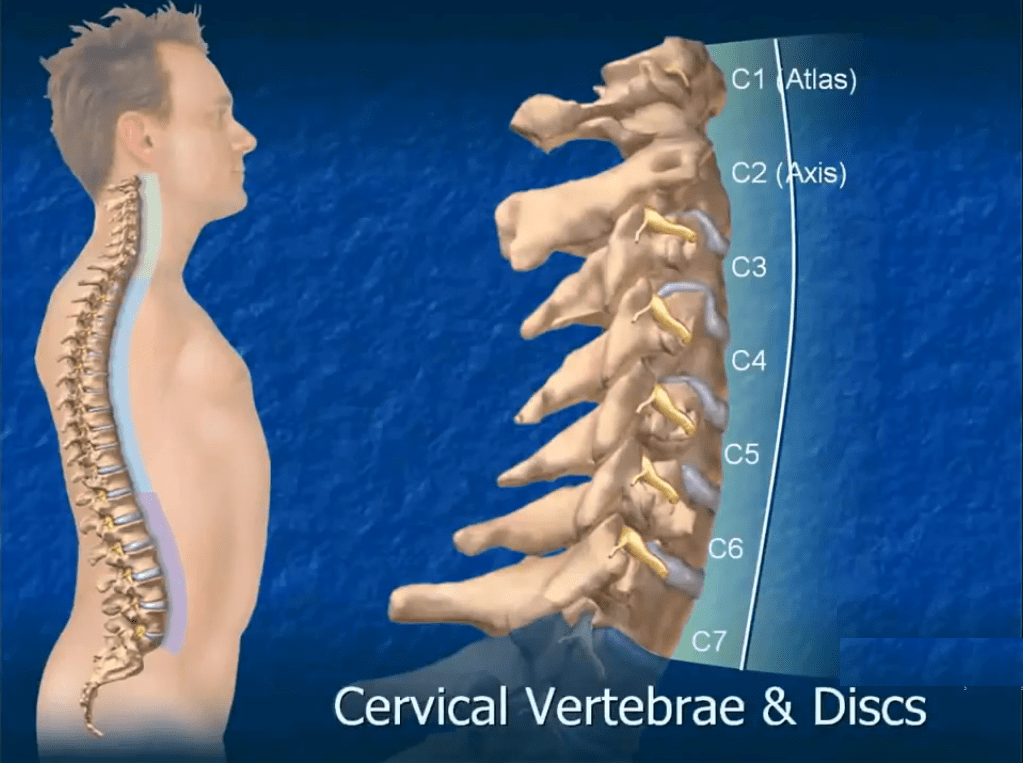
A cervical degenerative disc can lead to other spine conditions including:
- Bone spurs
- Herniated disc
- Bulging disc
- Spinal stenosis
- Pinched nerves
Degenerative Disc in the Neck
Degenerative disc disease is a process in which the spinal discs that cushion vertebrae in our back break down over time. Although it is usually age related, there are a number of possible causes of a degenerative disc in the neck, including:
Sports injuries
Repeated injuries, even on a small scale, make the discs weaker and more susceptible to degeneration.
Physically demanding jobs
Work that includes frequent heavy lifting and other strenuous activities puts more stress on the spinal discs and creates a greater chance of developing degenerative disc disease earlier in life.
Obesity
Although the effect is greater on the lower back than neck, carrying extra pounds on your body puts more pressure on your spinal discs, making them more likely to split or bulge.
Genetics/heredity
As with many diseases, some people are simply more prone to degenerative disc disease because of the genes passed down to them.
Degenerative Neck Disc Causes, Symptoms, and Treatments
Causes
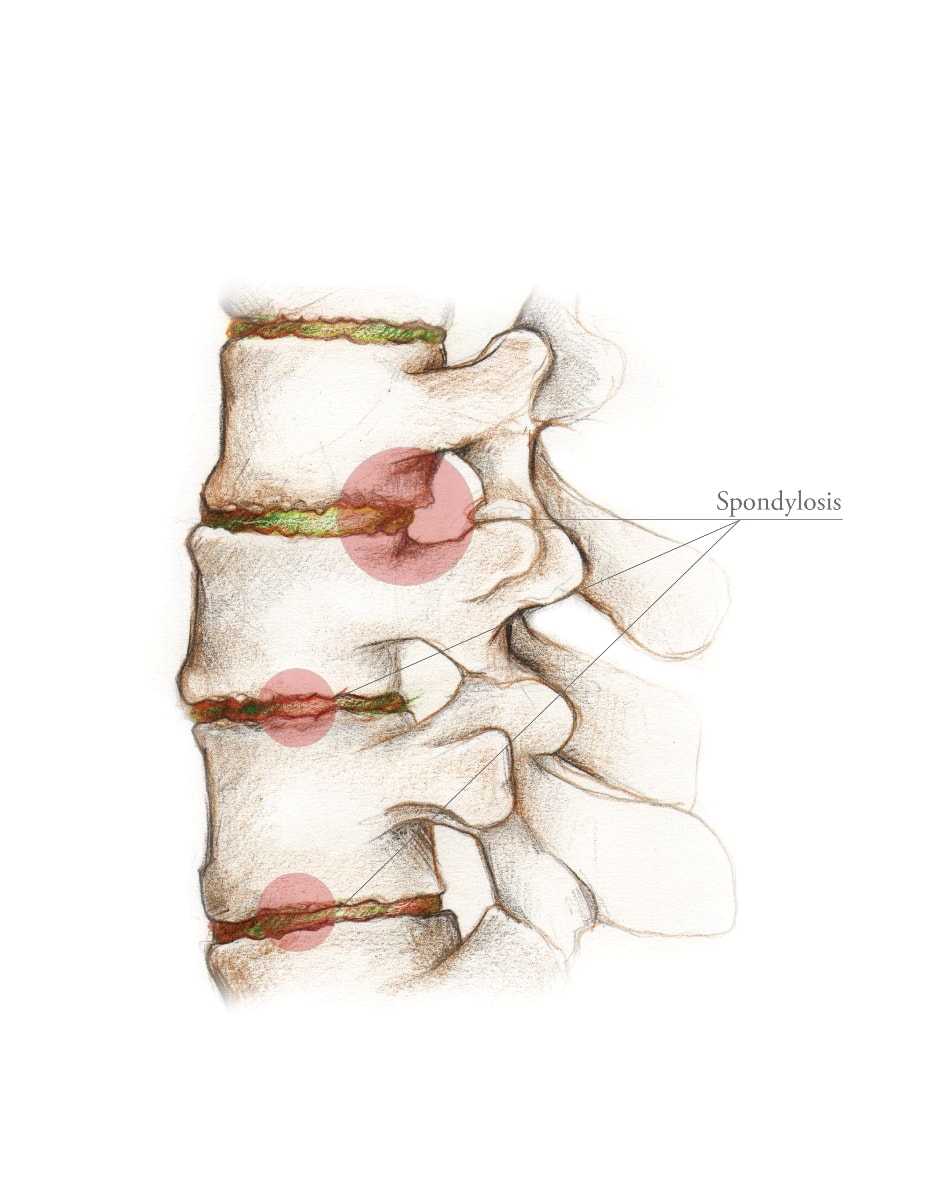
Disc degeneration is a natural side effect of aging in which the intervertebral discs lose volume, protein, and water content. The wear and tear of normal life causes a degenerative neck disc to become thinner and more prone to bulging and herniating. Disc degeneration can be hastened by trauma to the body such as from a car accident, but usually it just comes with age.
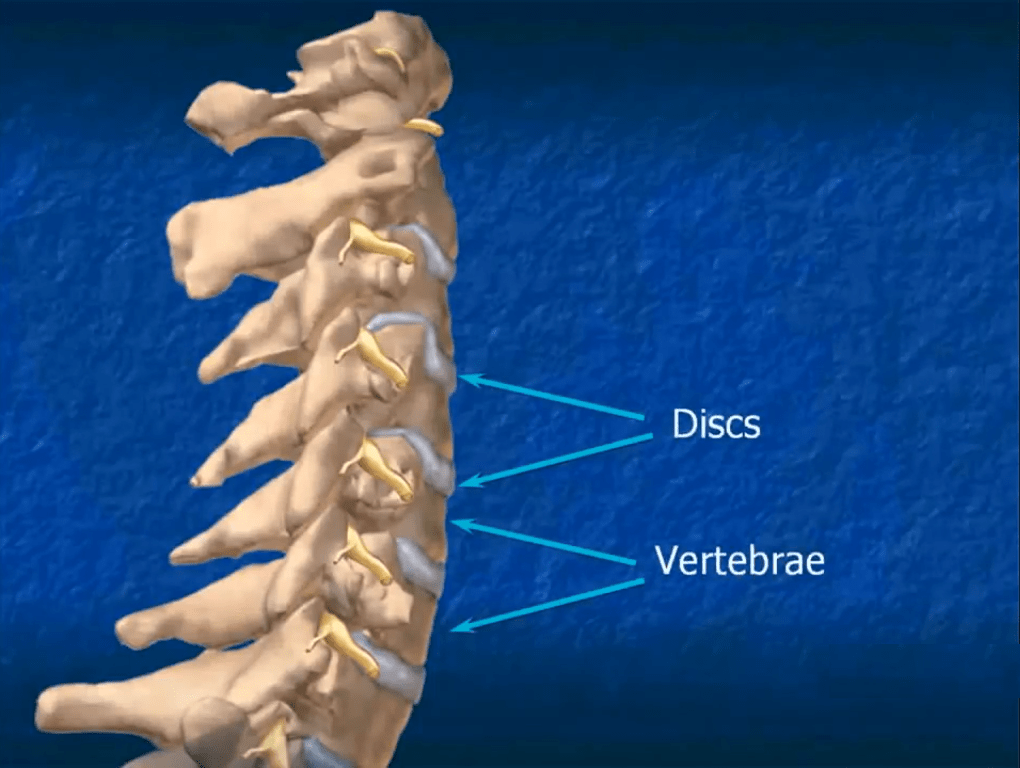
Symptoms
A degenerative disc in the cervical region of the spine will cause stiffness and pain in the neck, but it can also result in headaches, pain, tingling, numbness, and other symptoms in the shoulders, down the arms, and into the hands and fingers.

Treatments
Although disc degeneration can’t be stopped completely, there are many treatments that can help reduce the effects of a degenerative disc. These include:
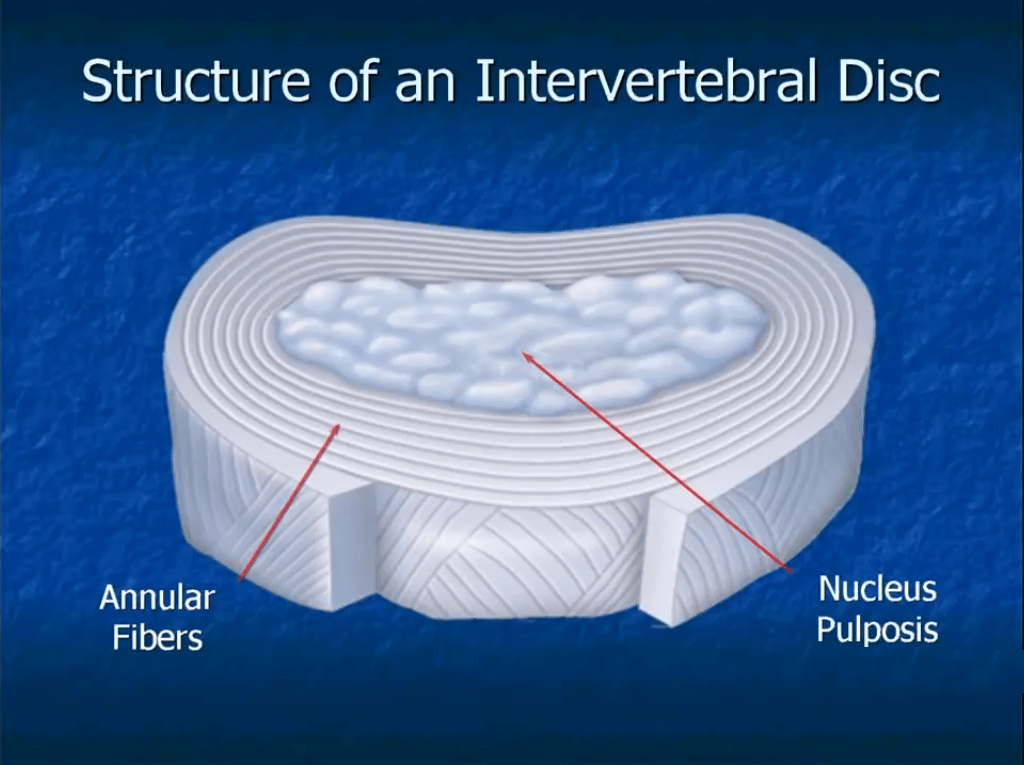
Chiropractic treatment
By decompressing the spine, a chiropractor can increase the space between vertebrae, creating a wider opening for nerve roots to pass through and allowing the spine to bend more. This treatment would need to be repeated regularly to maintain the effects.
Anti-inflammatory steroid injections
When a degenerative neck disc causes pain, it’s most likely because a nerve root nearby has been irritated and inflamed by pressure from the disc itself or from impinging bone. By injecting a steroid, your doctor can reduce inflammation, thereby minimizing symptoms.
Pain medicines
Many people find that their symptoms can be managed by taking pain medication. For mild pain, over-the-counter brands are sufficient, but for more severe symptoms, prescription pain medicines may be necessary.
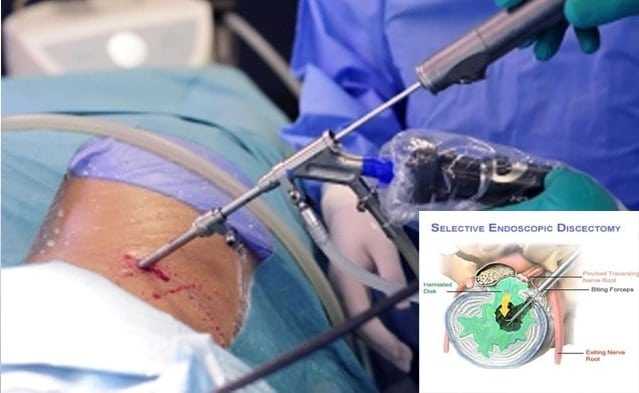
Degenerative Disc Surgery
These are just three possible treatments. If these and other conservative treatment options fail, then your doctor may recommend surgery. Open-neck surgical treatment usually includes a lengthy hospital stay, a long recovery, and permanent scarring.
Degenerative disc surgery comes in a variety of forms, and most recently, disc replacement has started to make headlines. This surgery involves removing any remaining portions of a damaged disc and replacing it with an artificial disc. The disc is attached to the vertebrae on either side, and the core is made of a flexible material like rubber or plastic. The artificial disc has proven successful for some patients, but—as with all artificial implants—there is potential for the body to reject it. Additionally, because it requires a highly invasive open back surgery, there are a variety of other complications it could create.
A more traditional degenerative disc surgery is spinal fusion. This procedure uses bone grafts and metal hardware to affix two adjacent vertebrae. This provides extra support and stability to vertebrae that are compromised by a deteriorated disc. Unfortunately, this procedure has only a moderate success rate, and—like disc replacement—it comes with the risk of rejection and the complications of an invasive surgery.



I have DDD from the neck all the way down my spine. And I’m 60 years old.