Chronic Pelvic Pain Syndrome In Women
A Real Case…
Marion and her husband (her name has been changed) were sitting patiently in the examining room when I walked in. “Hello Doctor,” Marion began, “I was referred to you by Pastor Focht who told us if you couldn’t figure out what was wrong with me no one could (I winced as I heard those words)”.
“Ever since I had my Hysterectomy I have had a searing pain in my vagina. I had the surgery because of the pain…it didn’t help. Doc, my life is unbearable.”

Marion has what would be termed “Chronic Pelvic Pain Syndrome in Women” (CPPSW). About 15% of all women in the U.S. suffer from this malady. Only a third of women seek medical care for this chronic pain syndrome (of which less than half ever receive a definitive diagnosis).
Chronic Pelvic Pain Syndrome in Women Is Complicated
Marion was understandably upset as she queried me, “What is causing all this pain? With all the tests I have had done and Doctors I have seen someone should have figured this out by now.” The diagnosis of CPPS in women is complicated. Let me put into perspective the difficulties in coming to a specific diagnosis about this condition:
1-) The first major challenge is that women have pain, hemorrhage internally, and generally feel less well on a monthly basis…this is called menstruation. The process is actually a monthly inflammatory process with hemorrhage.
2-) The second major challenge is that many women will have a growth that expands their uterus 400% or more, have a radical fluctuation in body chemistry, and end the process with a traumatic event to their pelvis…this is called pregnancy.

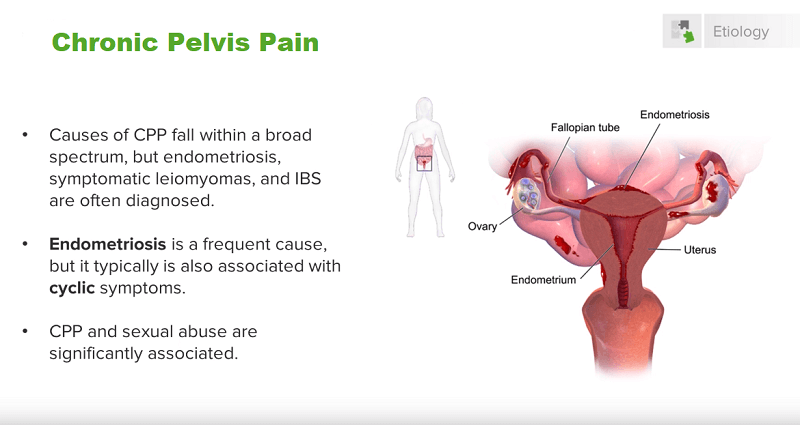
3-) A final challenge (there are probably more) is that women have a conduit from the outside to the inside that has a tendency to “hide stuff”…this is called the Female Reproductive Tract.
It is no wonder that women have chronic pelvic pain. It’s a “set-up”, of sorts. In the usual course of events women are regularly “traumatized” by their normal anatomy and physiology.
The list of possible causes for chronic pelvic pain in women is enormous. Before a woman can be said to have this syndrome the pain must be present for 6 months or more (a little longer than the usual 3 months for chronic pain in other areas of the body).

As I have stated in my previous blogs, a good history and physical is a starting point for any diagnostic workup. In this case, it was essential to have a very careful history taken with an emphasis on symptom fluctuations associated with menstruation (before Marion’s Hysterectomy).
Many Doctors would have skipped a menstrual history since Marion no longer had a uterus. However, it was important to ascertain the exact time that her pelvic pain began. In Marion’s case she had her Hysterectomy for persistent bleeding and pain due to Fibroids.
Naturally, a thorough pelvic examination must be performed by an experienced Doctor (with the emphasis on “experienced” in performing pelvic exams).
There are a multitude of technical studies that can be done to try and secure a diagnosis. The difficulty is that the anatomy of the pelvis is “tight” and “shielded” by the pelvic bones.
There is no single test that completely looks at the pelvis…not even a CT scan.
Chronic Pelvic Pain Syndrome in Women Can Cause Desperation
“I don’t want to live if I can’t get some relief,” was Marion’s attitude after having her pain for so long. In her case she previously had a work-up that was very adequate.
Unfortunately, it did not reveal any cause for her pain. When an adequate work-up has not yielded any specific findings the cause for the pain may be neurogenic or psychiatric in origin.
Human disease does not occur in a vacuum. There are patterns that will emerge when a person is repeatedly examined.
Dr. Charles Mayo (of the Mayo Clinic) once re-examined a patient every week, for months, before he was able to see a pattern of symptoms emerge in order to make a diagnosis.
In Marion’s case, I took a pragmatic approach to relieve her pain as soon as possible:
1) Her pain was treated aggressively and immediately. She was given a regimen of opiates (a sure fire way to get some pain relief quickly).
2) A second medication that could reduce the nerve impulses of pain (a medicine called Lyrica) was started.
3) A third medication was also begun (to restore neurotransmitter levels to normal)… a low dose anti-depressant that “recycles” both norepinephrine and serotonin (called Cymbalta).
The opiate pain medications gave her immediate relief (and hope), while the other medications would take weeks to work.
Many doctors would have just begun the Lyrica and Cymbalta because of the risk of addiction to the opiate. It is not more righteous to leave a patient in pain because ofan unwarranted fear of addiction. Many Doctors would argue otherwise.
Summary Remarks
On multiple re-visits Marion’s medications required adjustment. She was open and honest about how she was taking her opiate medications (the only way a Doctor can guard you from major side effects). She could not tolerate the Cymbalta side effects so it was discontinued.
In about a year her pain began to diminish. She was weaned down on her chronic dosing of opiates and remains on an as needed dose. Her last visit with me went something like this:
“Doctor, my pain has gotten as low as a “3” at times. If you hadn’t given me the relief I needed when I first met you… I think I would have taken my own life. What would I have done without you, Doc?”
Her husband sat next to her and wept.
If you have further questions please comment. I would love to be of service to you.I wish you much joy and good health.