Cymbalta As Pain Medication
Have You Considered This?
Did you know that chronic pain and depression are closely linked? People with chronic pain as their primary disorder often report the development of depression. Furthermore, people with depression as their primary disorder report more complaints of chronic pain. This article will be a review of Cymbalta as pain medication.
The neurochemistry of chronic pain and depression is closely related. Similar neurotransmitters (the brain chemicals responsible for nerve signal transmission) are utilized by the brain for chronic pain and depression. I like to think of chronic pain and depression as “first cousins.”
So when a doctor tells you that your pain “is all in your head” they are technically correct (though they are probably using this phraseology to keep you at “arm’s length” in preparation for a psychiatric referral).
Why certain people manifest their altered brain chemistry as chronic pain instead of depression is an area of active clinical research at the present time (as is the reverse). It seems that very creative people (with highly active associative cortex brain function) have a much greater likelihood of developing depression (think Vincent Van Gough).
Finally, people who are depressed, who develop a physical condition that results in chronic pain, report more intense levels of pain than those people who have a similar chronic pain condition without depression.
So you can see that depression and chronic pain are inextricably linked. By the way, this does not mean that chronic pain is ever imaginary nor that the chronic pain patient is a “head job” (demeaning descriptive phraseology that does not belong in the vocabulary of anyone involved in health care).
All this having been said, just what is Cymbalta?
What is Cymbalta?
Cymbalta (trade name) or Duloxetine (generic name) is an anti-depressant that works on the areas of the brain that modulate depression, anxiety, fibromyalgia, and neuropathic pain. It was originally developed and marketed by the Eli Lilly pharmaceutical company in 2004 (after some delay by the US FDA in regards to liver toxicity and possible cardiotoxicity).
It is a Serotonin and Norepinephrine reuptake inhibitor and is available by prescription only in most countries (definitely by prescription only in the US). It became available as generic Duloxetine in 2013.
How Does Cymbalta Actually Work?
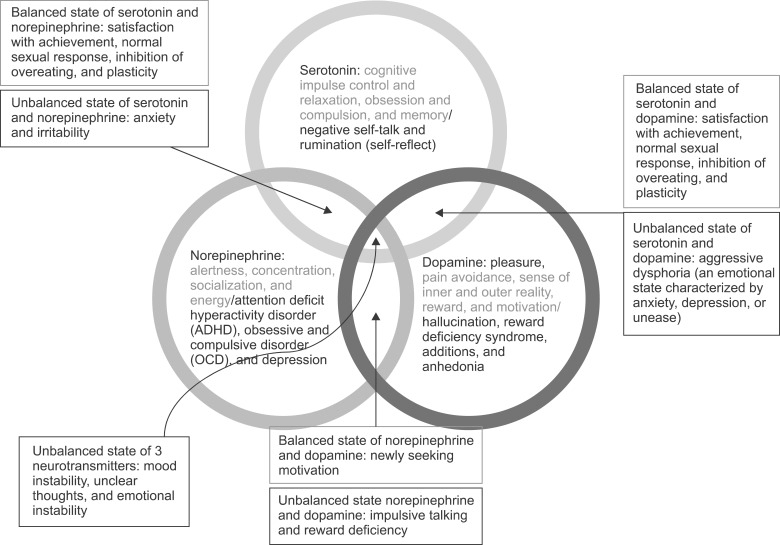
Depression is thought to occur due to an imbalance of the neurotransmitters Serotonin (ST) and Norepinephrine (NE). When either of these neurotransmitters reach critically low levels in the limbic system of the brain (the area where emotion is processed) depression can occur.
Chronic pain is also mediated in similar areas of the limbic system. Here again, low levels of ST and NE are seen in people with chronic pain. Medications that elevate these transmitters will often result in the reduction of certain types of chronic pain.
Not all chronic pain is processed in the same manner. In particular, neuropathic pain (pain that comes from the dysfunction of the nervous system) is processed in the brain using a sodium channel based mechanism. Cymbalta is particularly effective for pain relief in neuropathic conditions by blocking the sodium channel ions.
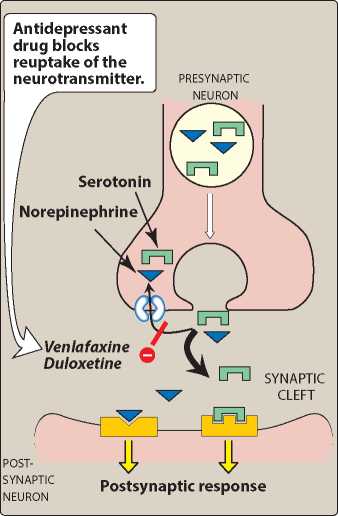
Cymbalta slows down the removal (“reuptake”) of NE, ST, and sodium ions from the synaptic cleft (space between nerve cells) that transmits the nerve impulse from nerve cell to nerve cell. By allowing these transmitters to “loiter” in the synaptic cleft the nerve impulse has a greater likelihood to be transmitted.
This general class of medication is called an SNRI (Serotonin and Norepinephrine Reuptake Inhibitor).
Anti-depressants that favor only blocking the reuptake of NE (TCAs-Tricyclic Antidepressants) or ST (SSRIs-Serotonin Reuptake Inhibitors) have not been found to be as effective for the reduction of neuropathic pain.
The TCA class of antidepressants tend to be very sedating (elevated levels of NE in the brain are sedating). Whereas in the SSRI class of antidepressants, elevated levels of ST are energizing with insomnia as a major side effect.
What Cymbalta is Used For?
Cymbalta has been approved by the US FDA (Food and Drug Administration) for the following uses:
- Chronic Pain from musculoskeletal conditions (in particular Osteoarthritis of the lower back).
- Diabetic Peripheral Neuropathy (the intense burning pain in the feet seen when blood sugar is poorly controlled).
Fibromyalgia (a chronic pain condition where there are “trigger points” of focused pain throughout the body).- Generalized Anxiety Disorder (a chronic state of heightened autonomic arousal with persistent anxiety).

It has also been approved for use, in other countries, for Urinary Stress Incontinence and the peripheral neuropathy that can occur with chemotherapy. Furthermore, Cymbalta is often used by doctors in an “off-label” format.
“Off-label” use of any medicine is where the medication has shown a benefit for patients but has not been officially recognized (by the FDA for instance) for such use. Many medications are used this way by physicians for their patients.
Official uses for a medication are the only uses that a drug company may market. They may vary from country to country (France limits the official indications for Cymbalta as compared to the US).
What Are The Potential Side Effects With Cymbalta?
You may expect that the dual mechanism of Cymbalta could “double” the chance of side effects. In fact, Cymbalta does have a rather impressive side effect profile. Here is a listing of the most common and severe side effects:
- Nausea/Vomiting
- Sedation
- Insomnia
- Dizziness
- Dry Mouth
- Withdrawal Syndrome: When Cymbalta is abruptly discontinued a very uncomfortable withdrawal syndrome can occur. It is characterized by “electric shock” sensations, agitation, confusion, nausea, vomiting, nightmares, and a host of other uncomfortable symptoms.
A gradual reduction in dose for this medication is recommended when discontinuing it. It can take weeks to gradually wean off of Cymbalta. There is no universally accepted weaning schedule for it.
Sexual Dysfunction: Cymbalta is well known to make it impossible to achieve orgasm in women who had no such difficulty before taking the medicine (and can also make the issue worse in women who already have a challenge in this area). Men can also be similarly affected.
Increased Suicidality: Curiously Cymbalta, a medicine to treat depression, can actually stimulate suicidal attempts. Though this can be seen with nearly any anti-depressant, Cymbalta has received a “black box” warning for this. The US FDA attaches a “black box” warning to medications that have a proclivity for potentially serious, if not lethal, side effects.
Important Note
THE ADMINISTRATION AND MONITORING OF CYMBALTA MUST BE UNDER THE SUPERVISION OF A LICENSED MEDICAL PRACTITIONER. THIS IS A POWERFUL MEDICINE THAT REQUIRES CLOSE FOLLOW-UP.
×
Dismiss alert
How is Cymbalta Dosed?
Cymbalta is generally begun at the lowest effective dose and gradually adjusted according to effect and side effects. The starting dose is generally 30mg per day (taken once daily). It is well absorbed from the gastro-intestinal tract and primarily metabolized in the liver.
On any given dose it takes 3 days for the blood level to stabilize. Therefore, dose adjustments should not be made any more frequently than every 72 hours (most doctors will wait weeks before adjusting the dose). Furthermore, the actual therapeutic effect may take weeks to show itself. Adjusting the dose of this medicine may only be justified in 2 to 4 week intervals because of this.
Doses over 120 mg per day are generally not recommended (the number of side effects at that dose counter-balances the benefit).
Finally
I have reviewed the history, mechanism, indications, side effects, and dosing for Cymbalta. This medication has been an important advance in the treatment of chronic pain (in particular neuropathic pain). Many people have had their pain significantly reduced by this medicine.
It carries with it a large responsibility for both patient and prescribing practitioner. As I have said in previous articles on pain management…the treatment of chronic pain always carries some risk. It is impossible to treat pain effectively without understanding this.
I hope you have found the information in this article valuable. Please contact me with your questions and comments.
Wishing you much joy and healing,
Oleg