Endoscopically Assisted Spinal Decompression
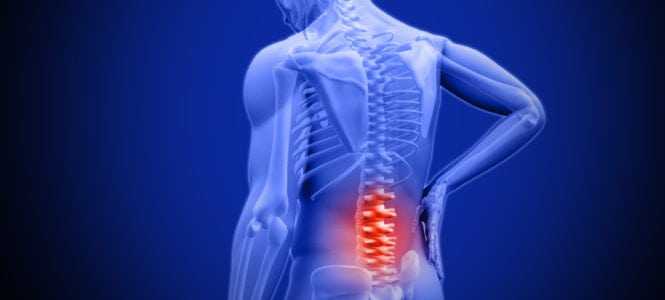
INTRODUCTION
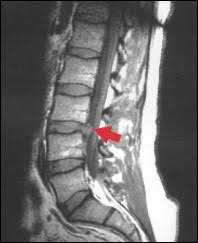
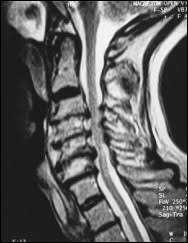
Cervical Disc Herniation
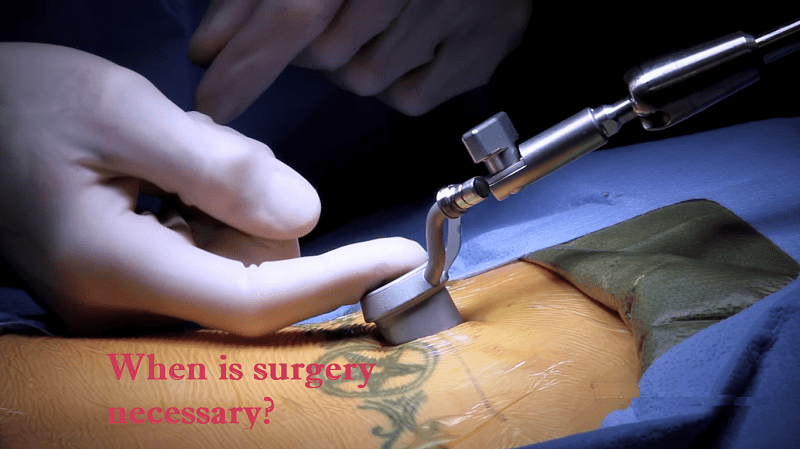
Minimally invasive, endoscopically assisted spinal decompression is a revolutionary procedure that was invented in the early 1950′s. Using a needle guide with an endoscope under local anesthesia, the internal structures are visualized under magnification and repaired from the inside using Laser and Radiofrequency (RF). One of the main benefits of the endoscopic decompression, unlike in traditional open spine surgery, is the fact that the adjacent muscle and tissue damage is minimized, which allows for faster recovery, reduced bleeding, and a small incision.
PATIENT INFORMATION
Endoscopically Assisted Spinal Decompression is the selective removal of targeted portions of a bulging disc, bone or other fragments that cause stenosis (narrowing of the spinal canal) and pressure on your spinal nerves and spinal cord.
It can be achieved by shrinking the inner or outer portions of the intervertebral disc, bone, or other fragments that cause pain using various techniques such as radiofrequency, coblation, ultrasound, heat (electro-thermal energy), or laser. This shrinks the disc or other structures, which in turn reduces compression of the nerve and spinal cord. If annular tear is present this also starts the healing process of an annular tear.
Procedure
Time in the operating room is about 90 minutes per level. Intravenous sedation and local anesthetic will be provided. Using fluoroscopy (an advanced form of x-ray that takes still as well as moving x-ray pictures), an entry is made approximately 10 centimeters from the spine. An arthroscope (also called an endoscope) is passed through the incision, subcutaneous tissue and muscle.
Careful entry is made into the interior of the disc, and disc material is manually removed at the site of the herniation. A radio frequency electrode and YAG: Holmium laser is used to control any bleeding, shrink the inner disc tissue, and shrink the annulus (outside rim of the disc). Occasionally, entry is made from both sides of the spine if indicated.
Expected Results:
The ultimate goal is relief from back, neck, leg, or arm pain, as well as from numbness or weakness of the extremities. After surgery there will be some discomfort in the surgical area. You will be released to home after about an hour of recovery, and will follow up within 2 weeks with your surgeon in the office for suture removal and wound care (For out of state patients, you may follow up with your primary care provider for suture removal). Please remain on bed rest until that time unless otherwise indicated by your surgeon. Please discuss before beginning physical therapy or chiropractic. Return to work varies according to patient response and the type of job they do. Occasionally, you will be placed on ‘light duty’ for the initial return to work and increased to ‘full duty’ as tolerated. Your disc begins to heal at about six weeks. Don’t rush getting back into the swing of things!

Back/leg or neck/arm pain may disappear immediately, but may also take up to several months to quiet down. The pain may change in character or increase in severity. This is a normal reaction. Please be patient and remind your family/friends to hang in there as you heal from your procedure.
Risks include infection, injury to the local nerves, unusual nerve sensations, continued pain, disc tears and local muscle bruising. Segmental instability (unstable backbone) may require additional surgery to repair.