Myths About Opioid Therapy
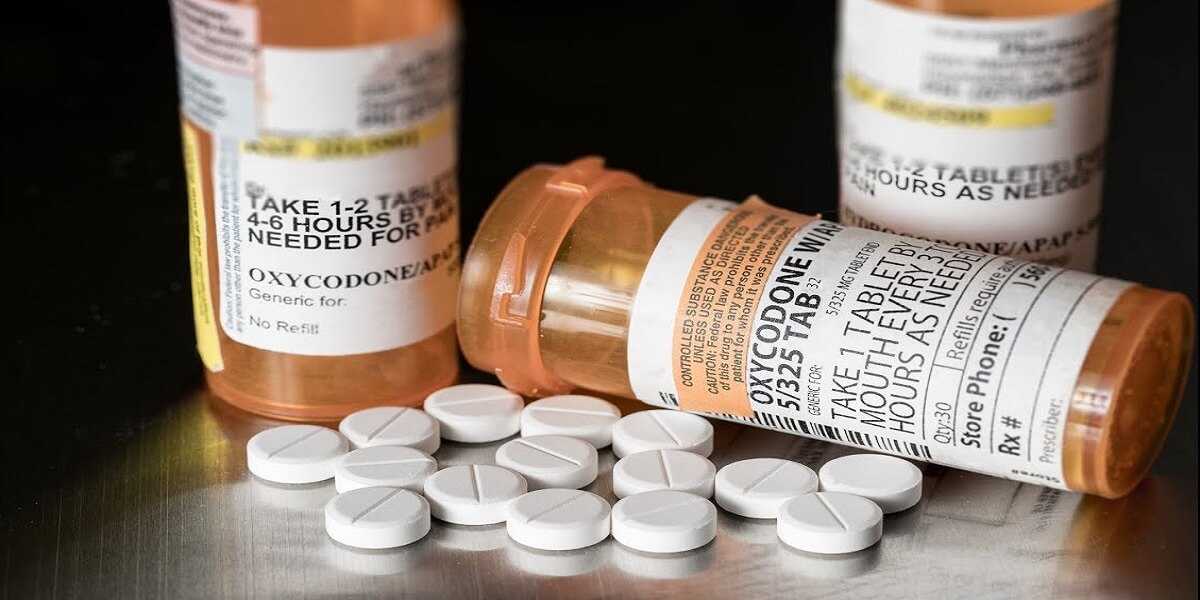
If you listen to the media bias you will have a very negative opinion of opioid therapy. Not surprising…negative news sells advertising time better that positive stories. I am here to tell you there are many myths about opioid therapy.
I have pondered long and hard why there are so many myths about opiod therapy. In my pain management practice, I saw largely positive outcomes in the people I selected to be treated with opioids (if they took the medicine as directed).
However, I did have my share of people that had bad outcomes. I am unaware of anyone who took the medications as directed who developed life threatening complications.
It would seem to me that the issue about opioid therapy is largely one of patient selection. Not all people who have chronic pain should have opioids as their primary therapy.
This is to be expected as no one therapy is best for all people. Many of my patients had a bad outcome with surgery for their chronic pain (in particular people who had back surgery for chronic pain).
And yet, we wouldn’t insist that surgery is always a bad idea would we? Again, selecting the right patient for surgery is essential. But you see, patients don’t come with a sign on them that states they will have a good result.
Therapy for chronic pain is always risky no matter what it is. And Doctors aren’t prophets. Given certain conditions there is usually a range of therapeutic options that can be taken. Choosing the right one each time would be impossible for Doctors.
So the practice of medicine is an imperfect science, practiced by imperfect people called Doctors, practiced on other imperfect people called patients. Perhaps that is why it is called “the practice” of medicine.
The result can be the dissemination of disinformation about certain therapies. Let me share with you 7 common myths about opioid therapy.
Seven Common Myths About Opioid Therapy
Myth Number 1: “If a person uses opioid therapy chronically, and drives a motor vehicle, they will be impaired.
It would seem to make sense that, if a given medicine can affect the central nervous system (CNS), it would impair one’s ability to drive. And we know that opioids affect the CNS.
But, there is a HUGE difference between the short term administration of opioids for pain and the long term administration. Chronic usage of opioids allows the brain to build up a tolerance to the “brain drain” of opioid therapy.
The brain adjusts to opioid therapy given chronically.
Studies done to measure the driving abilities of people on chronic opioid therapy have demonstrated that people on such medicine chronically have no greater risk of an accident than people not taking any medicine at all.
In fact, if you take over the counter Benadryl you are at greater risk of a car accident while driving than if you are on chronic opioid therapy. I don’t think anyone is suggesting that we make over the counter anti-histamines illegal are they?
Myth Number 2: “If a Doctor prescribes a long acting opioid therapy the person taking it will have less likelihood of habituation.”
There is a difference between habituation to an opioid and addiction. Habituation is a physiological phenomenon that occurs with many medicines (for instance anti-depressants, anti-hypertensives, and anti-seizure medications). Opioids are no different in that respect.
Addiction is an obsession and compulsion to abuse a substance despite physical harm.
This can only be diagnosed by watching a patient over time.
Nearly all people who take opioids chronically will become habituated. Very few will become addicted. Addiction is a person dependent occurrence.
Long acting opioids have no less likelihood of habituation than short acting. In fact, habituation may occur more quickly with long acting opioids as the opioid receptor (the place where the medicine attaches to give its effect) has no chance to “recover.”
Myth Number 3: “If a Doctor prescribes a short acting opioid the person taking it will have less likelihood of habituation.”
There is also a myth that short acting opioids are always less habituating than long acting. When the opiod for either the long or short acting preparation of a molecule is used, the risk of habituation is common with both. After all, in most cases, it is the delivery system that has been changed not the molecule.
The actual incidence of habituation with opiods is complicated. The studies done trying to prove this have been fraught with methodological problems.
Myth Number 4: “The recent opioid “epidemic” has been caused by Doctors “over-prescribing” pain medications.”
Did you know that there is no “top dose” on opioid pain medications? In medicine we would call this a “ceiling effect.”
A “ceiling effect” is where additional increases in the dose of a medicine do not result in additional therapeutic effect (but will usually increase the side effects).
Motrin has a “ceiling effect.”
Doses of Motrin higher than 1200 mg per day offer no additional pain relief and increase the risk of gastro-intestinal hemorrhage. Each year in the U.S. up to 15,000 people die from gastro-intestinal hemorrhage from anti-inflammatories (the category for the type of drug that Motrin is in).
And these statistics are for those anti-inflammatories that were prescribed. No one knows how much the taking of over the counter (OTC) Motrin would add to this number of 15,000 gastro-intestinal hemorrhage deaths.
This is because it is nearly impossible to track OTC medicines for research purposes. It is safe to say that the number of deaths from anti-inflammatories is probably much higher than reported because of OTC usage.
The actual deaths from the appropriate use of anti-inflammatories each year in the U.S. is more than the deaths from the inappropriate use of opioids (called over doses).
If the normal use of anti-inflammatories causes more deaths than the abuse of opiates, why do we have such a national obsession with opiate pain medications?
Myth Number 5: “The recent increase in opioid overdoses is the direct result of Doctors inappropriately prescribing pain medications.”
If a person commits a crime using a gun, is the gun charged with the crime? Of course not, only a person can be charged with a crime.
Well then, if a person takes their opioid medicine not as prescribed (or perhaps they weren’t even prescribed the medicine), why then is the medicine held responsible? Shouldn’t the person inappropriately taking the medicine be the issue?
Furthermore, if crime is more common in highly populated areas with a larger number of telephone poles (which it is), we wouldn’t say the telephone poles cause the crime would we? Association is not causation.
When the under treatment of chronic pain was recognized in the 1990’s, an emphasis for more effective treatment was made. The number of people with chronic pain in the U.S. is estimated at 100 million people.
When the number of opioid prescriptions increased, in response to the epidemic of under treated chronic pain, the number of complications would be expected to increase too.
More prescriptions were written, more people with chronic pain were treated effectively, and more complications occurred.
The ”over-prescribing” of opioid pain medicines is the result of attempting to treat the largest epidemic ever recorded in human history…the chronic pain epidemic (100 million people in the U.S. alone). The percentage incidence of over doses hasn’t changed. It is the number of people being effectively treated for their chronic pain that has.
Myth Number 6: “Opioid overdoses occur in people taking large doses of this type of medication on a chronic basis.”
This is a tricky myth. It is true that the larger the dose of opioid pain medicine any given person takes the greater the risk of overdose when followed over time. But this is not due to the dose of the medicine.
What is actually happening is a process of un-natural selection.
The higher any given dose for opioids the greater the likelihood is that the person is an undisclosed addict.
Addicts are reluctant to be honest with their Doctor when it comes to their opioid medications. The higher doses draw a higher percentage of addicts into any practice that is willing to prescribe this size dose.
Here again, it is a matter of patient selection and not the evils of opioid pain medication.
Myth Number 7: “The Urine Drug Screen is the best method for detecting when a person is abusing or diverting their opioid pain medication.”
The common practice of performing Urine Drug Screens (UDS) in pain management has become a standard of care (though the exact number per year, interpretation, and appropriate response to the findings have yet to be standardized). We did them frequently in my practice of chronic pain management.
However, the UDS is not a definitive diagnostic tool for compliance, addiction, and diversion (selling the medications).
The UDS is only one piece of information that a pain management physician uses when following a patient.
There are many false positives, false negatives, and all the variations in between. Furthermore, the interpretation of the UDS should always be in light of the clinical findings of the patient.
No single test can identify diversion, abuse, or compliance.
Summary Remarks
I have reviewed the need for careful patient selection when using opioid medications for chronic pain management and 7 common myths about opioid pain medications. The opinions contained in this article are all backed by research data from credible sources.
If you or a loved one have chronic pain you will want to consider opioid pain medication as one way in which your pain could be treated effectively and safely. There are, of course, many treatments for chronic pain other than opioids.
Do not be swayed by the preponderance of media attention to opioid over doses. Few people over dose taking their opioid pain medications as prescribed.
If you have further questions or comments, please leave it below. I would love to hear from you (even if you disagree with this article).
Wishing you joy and healing,