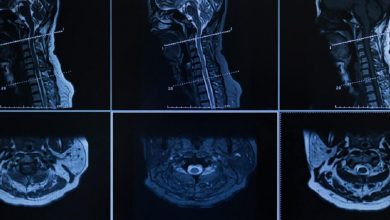
Options For Lumbar Spinal Stenosis
Over 75% of all Americans will experience back pain at some point in their lives. This results in billions of dollars in direct health care costs, lost wages, and collateral costs (ie. nursing home admissions, home care, etc.). A subset of people with chronic back pain will have lumbar spinal stenosis.
So just what are the options for lumbar spinal stenosis? This monograph will answer that question.
Most back pain in the United States is caused by a weakening or wearing of the structures of the low back. In some cases there is a genetic tendency. While, in other cases, we just “beat up” our back with the activities in our life.
Smoking, obesity, occupations that involve operating machinery that vibrates your body, genetics, and sports activities that stress the spine all contribute in developing lumbar spinal stenosis. Your spine and the structures that support it (ligaments, tendons, discs, and muscles) have a limited capacity to heal after being damaged.
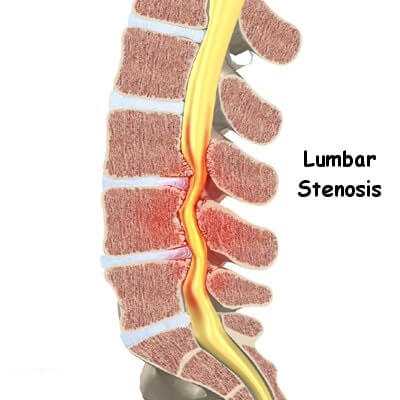
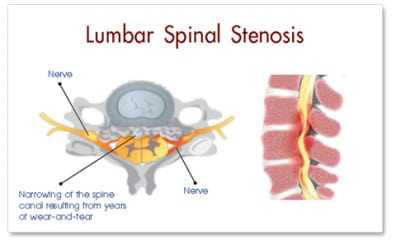
What Is Lumbar Spinal Stenosis?
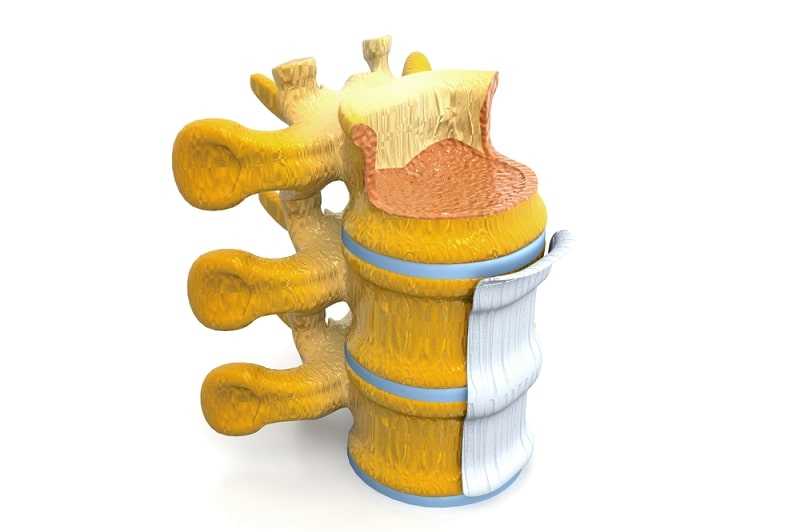
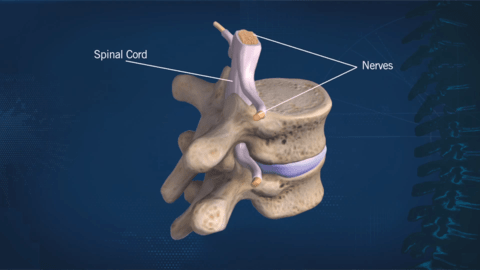
In the interior of your back is a canal called the spinal canal. It is a “bony tube” that runs from your neck to your lower back. It is the home for your spinal cord and spinal nerves.
The spinal canal provides protection for your spinal cord (a very fragile structure indeed). Each segment of your spine has the spinal canal within it. As the spine bends so does the canal and your spinal cord.
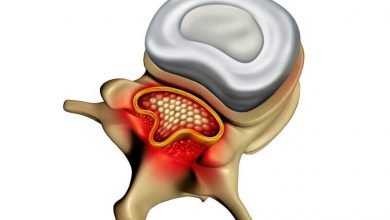
Any structure that “pinches into” the canal will potentially cause narrowing or “stenosis” (the medical term for narrowing). So you can see that bone overgrowth, disc bulging, tumors, blood, etc. can all cause stenosis.
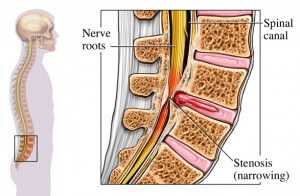
To make matters more complicated, some people are born with a congenitally small spinal canal. In people born so it takes much less intrusion to narrow the canal and cause symptoms.
How Does Spinal Stenosis Cause Pain?
The mechanisms for the pain are many. Here is a brief summary of how the pain is generated:
1) Compression of the spinal cord: Nerves do not appreciate being squeezed, cut, torn, frozen, burned, “starved” (deprived of blood or oxygen), poisoned, or stretched. The spinal cord is like a cable with thousands of wires in it. Compression “kinks” the wires.
2) Stretch of the spinal cord: As the spinal canal narrows the spinal cord and spinal nerves are “teathered” and stretched.
3) Ischemia of the spinal cord: Though a rare complication in spinal stenosis, it is possible to reduce blood flow to the spinal cord as the structural damage pinches the blood vessels that supply the spinal cord.
4) Associated inflammation and degeneration: As the muscles, ligaments, tendons, discs, and bony elements are all close neighbors, injury to any of these structures can cause pain. Also, the existence of spinal stenosis may adversely effect the function of the associated back structures that are not directly injured (such as the vertebral facets).
How Does Spinal Stenosis Feel?
The symptoms of Lumbar Spinal Stenosis are mostly what you would expect: low back pain, radiating leg pain, numbness in the legs and feet, and weakness of the legs.
There are 2 symptoms that are more predictive of lumbar spinal stenosis than other causes of low back pain:
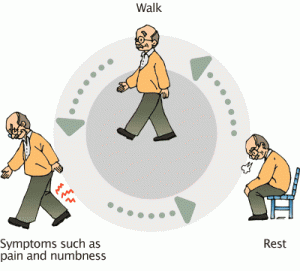
1) Spinal Claudication (claudication is impairment in walking): This is a curious finding that as people walk they develop leg pain. If they stop walking the pain will often diminish. This must be differentiated from arterial vascular claudication.

2) “Shopping Cart” Claudication: You have probably seen this when you are at the supermarket…people pushing their carts by leaning on them bent at the waist. This is a position of comfort for people with spinal stenosis.
The physical examination will show the usual muscle spasm in the lower back (a general finding in people with back pain), reduced strength in the legs, reduced range of motion of the lumbar spine, and pain when the lumbar spine is forcefully palpated (or touched).
What Are The Tests For Lumbar Spinal Stenosis?
The diagnosis of lumbar spinal stenosis requires a thorough history and physical by a licensed primary care practitioner. There is no definitive symptom, or physical finding that makes the diagnosis.
CT Scanning and MRI scanning can diagnose causes for spinal canal narrowing but there are many cases missed by these tests. The symptoms and position of relief along with a CT scan or MRI of the lumbar spine will usually provide enough information to make the diagnosis of lumbar spinal stenosis.
What Are The Best Therapies For Lumbar Spinal Stenosis?
The treatments for lumbar spinal stenosis can be broken down into 2 basic categories:
Non-invasive Therapies:
1) Low Back Exercises: This is the best and most effective therapy for lumbar spinal stenosis. For a good introduction to exercises for low back pain see my post on the topic (click here for a link to low back exercises).
2) Traction: If the cause for the lumbar spinal stenosis is disc herniation, this form of therapy may be very effective. The portable traction device called the Disc Doctor WG30 has been found very effective for people with a disc herniation in the L-5/S-1 position.
3) Bracing: Supporting the lower back with a lumbar corset has been found to relieve pain in lumbar spinal stenosis. This is especially helpful when the distance to be walked is more than 100 feet.
4) Massage Therapy: This form of therapy enhances healing of damaged back structures and releases endorphines in the brain. The pain relief may be very temporary.
5) Manipulative Therapy: Both Chiropractic and Osteopathic Manual Therapies have been shown to give relief in lumbar spinal stenosis through aligning the vertebrae of the spine.
6) Ultrasound, Cool Laser, Muscle Stimulation, Hot Packs, Cold Packs, Acupuncture, Trigger Point Injections etc. are all helpful adjuncts to a good low back exercise regimen.
7) Medications: The use of non-prescription and prescription medication can be very helpful in reducing pain and allowing an exercise regimen to be started.
Important Note
DESPITE ALL THE THERAPY AVAILABLE TO A PERSON WITH LUMBAR SPINAL STENOSIS, MANY WILL CONTINUE IN PAIN. FURTHERMORE, SOME PEOPLE DEVELOP SPINAL INSTABILITY AND/OR SPINAL CORD COMPROMISE AND MUST BE REFERRED FOR INVASIVE THERAPY.
Invasive Therapies:
The general mechanism of pain relief with the invasive approach is to reduce the compression or stretch of the spinal cord.
1) Epidural Injections: This procedure injects corticosteroids (and perhaps a local anesthetic) into a space around the spinal cord called the epidural space, hence they are called epidural injections. The intent is to decrease inflammation around the spinal cord and decrease the pressure on it. Epidural injections work best with acute disc herniation.(click here for a link to Epidural injections)
2) Facet Injections: In this procedure, corticosteroids (and perhaps a local anesthetic) are injected into the small joints on the top and bottom of the vertebrae called facet joints. The intent is to decrease inflammation as in the above. Lumbar facet injections work best when acute facet inflammation is the mechanism for the spinal stenosis.(click here for a link to spinal injections for back pain)
3) Spinal Laser therapy: In this procedure, the spinal canal is entered by way of a small incision in the low back. A cannula is used to give the laser access to the area of compression and simultaneously visualize the spinal cord and spinal nerves.
Laser therapy is best used when the compression tissue has a high water content (such as a herniated disc) as the laser is able to vaporize the tissue. Laser therapy will not vaporize bone compression.
4) Spinal Decompression: There are many surgical procedures that fall under this category…from a micro-discectomy to an open spinal laminectomy with spinal fusion.The severity of spinal stenosis and instability is what determines the best approach. (click here for a link to endoscopically assisted spinal decompression)
Nearly all the procedures in this category do something that none of the non-invasive therapies can…there is an absolute removal of the compression tissue with spinal canal enlargement.
Since spinal stenosis is a “crowding” of the spinal canal, it stands to reason that compression tissue would need to be removed and the spinal canal enlarged for permanent relief of spinal stenosis.
Obviously, open surgical procedures carry much more risk than the closed or conservative measures. The most dramatic improvement with an open surgical procedure will occur in people who had reversible neurological impairment related to their spinal stenosis.
Relief of pain, as the sole reason for an open procedure in spinal stenosis, is usually disappointing. I have seen many times that the patient wants the surgery for one reason (pain relief) and the surgeon is doing the surgery for a different reason (preserve neurological function and spinal stability).
If you or your loved one is contemplating an open procedure, make sure your surgeon is experienced, his location for the surgery is reputable, and you are on the same page as to what is a reasonable expected outcome. It is a good idea to obtain at least 2 opinions from 2 different spinal surgeons before proceeding with surgery.
Summary
I have reviewed the history, physical, diagnostics, and treatments for Lumbar Spinal Stenosis. This is a very difficult chronic pain syndrome to treat conservatively. However, the conservative measures are what usually work the best over time (given the limited benefits of other modalities).
Invasive surgical procedures should be reserved for the most serious of cases. These would be cases of neurological impairment or spinal instability.
The best outcomes for chronic spinal stenosis are generally achieved by way of a graded exercise program. Spinal exercises are effective, inexpensive, and can be followed up with surgery if necessary. Your greatest hope for you or your loved one suffering with chronic lumbar spinal stenosis resides in exercise.
Exercise is the best of all the options for chronic lumbar spinal stenosis.
If I may be of service to you or you just want to leave a comment please do so below. I would love to hear from you.
Wishing you joy and healing.