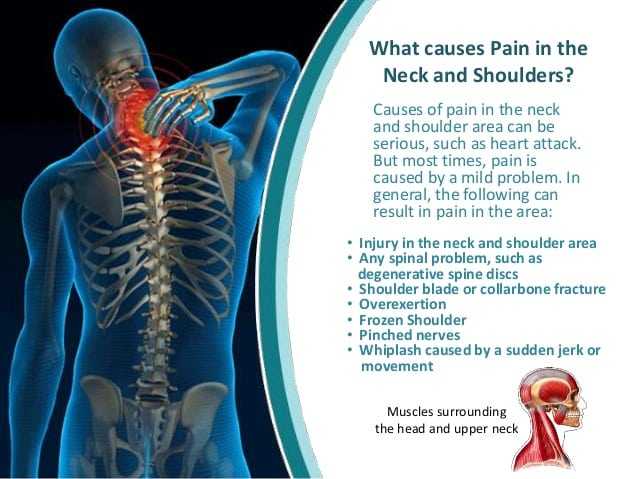
Pain in the Neck

Pain in the neck is common and is the cause of considerable morbidity. This clinical syndrome has various causes:
- Infection: pyogenic, tuberculosis, meningitis
- Inflammation: seronegative spondarthritides, rheumatoid arthritis
- Degenerative: osteoarthritis, degenerative disc disease
- Structural: cervical rib, cervical canal stenosis
- Metabolic: osteopenia, osteomalacia
- Trauma: fracture, non-articular strain, “whiplash injury”
- Non-specific pain: soft tissue rheumatism, postural, “psychogenic”
- Referred pain: retropharyngeal pathology
- Neoplastic: secondary, primary (intra- or extramedullar lesion)
The cervical spine of all mammals, including even the giraffe, has seven vertebrae. Like the lumbar spine, it has a protective and supportive role. The cervical spine, however, is very mobile, allowing movement in six planes. Apart from the central articulations (the secondary cartilaginous joints or symphyses, which are devoid of synovium), there are two diarthrodial joints between each spinal segment. The facet joints are set at an angle of 45° which permits a compromise between movement and stability, and in addition the neurocentral joints at the margins of the disc are synovial lined. The vertebrae protect the spinal cord and the vertebral arteries ascending through the intervertebral foramina.
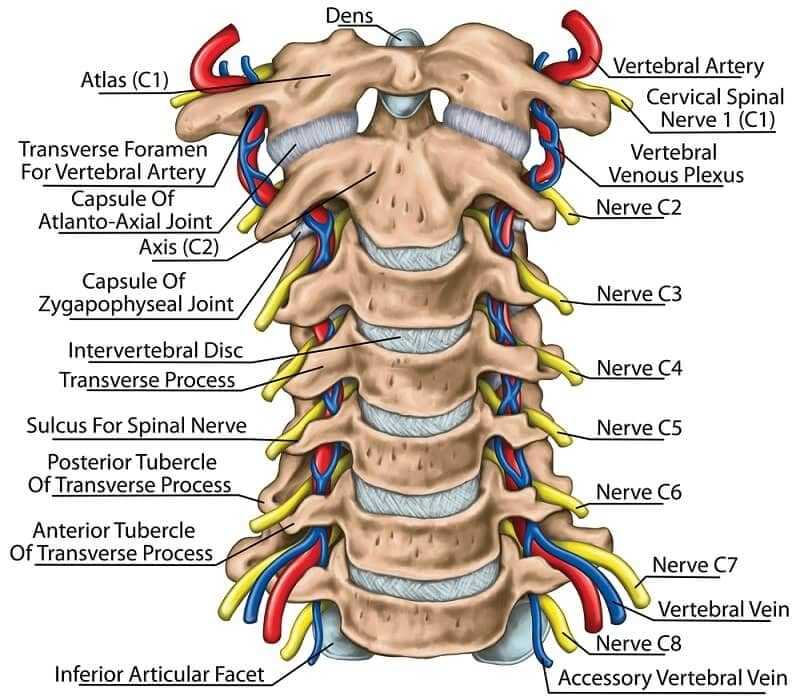
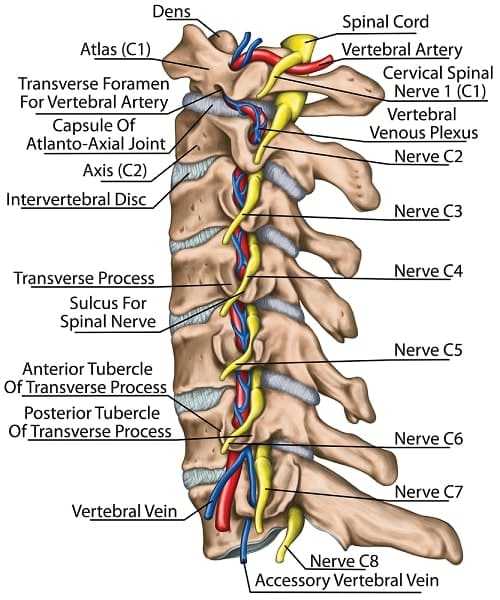
The skull rests upon the atlas and both rotational and flexion/extension movements occur here. The atlas has no vertebral body but instead the odontoid process of the axis is held between the anterior face of the bone and the transverse ligament. Synovial bursae separate the process from the ligament and this is an area of considerable importance in inflammatory diseases such as rheumatoid arthritis or ankylosing spondylitis.
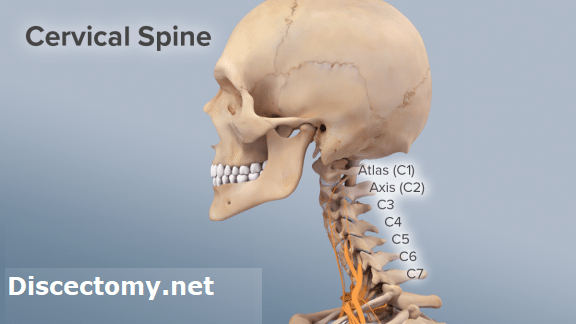
The term “cervical spondylosis” is used to include the process involved in both disc degeneration and osteoarthritis of the spine, expressing the close relationship between these two diseases. Each alone or together is responsible for a large proportion of episodes of neck pain. The pain is usually described as dull or aching, may be exacerbated by movement (sometimes in a particular direction) and is usually worse in the evenings or at night. Sleep may be impaired and often the patient will complain of pain on awakening. A characteristic feature of cervical spine disease is pain which begins at the occiput then radiates over the vertex and settles in the frontal area. This indicates involvement of the cervical nerve roots. It is obviously important to consider in the differential diagnosis all other causes of headache, the more so when one recognises the insecurity of finding changes on radiological examination of the cervical spine.
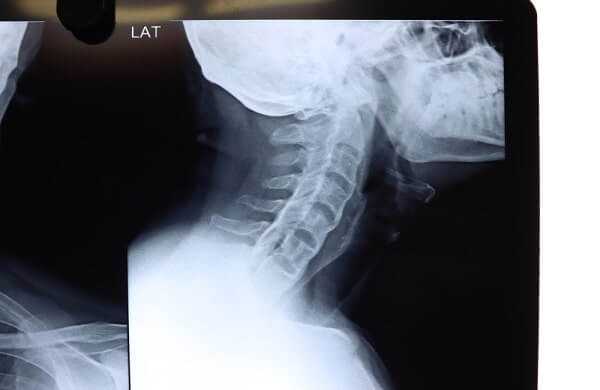
Many symptomless patients have X-ray changes and the most dangerous trap is to ascribe the clinical symptoms wrongly to osteoarthritis in the presence of much more serious pathology. It is worth stating the obvious: when changes in the cervical spine become radiologically apparent they have already been present for a considerable time and caution should be exercised before ascribing recent symptoms to them. It is also important to remember iatrogenesis. The very drugs prescribed for headache and neck pain themselves may produce these symptoms and all that is required is to remove the offending agent. Indomethacin is the best recognised in this context but most other NSAIDs may also produce this side-effect.
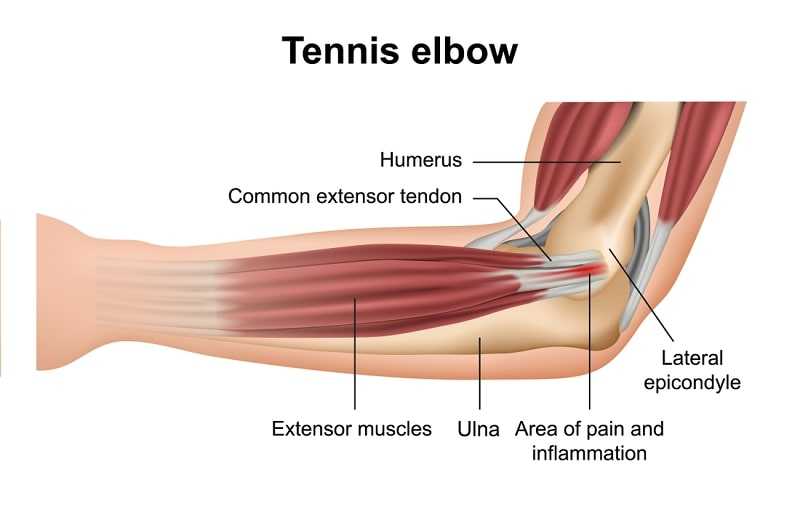
Well-known clues indicating the possibility of disc protrusion, such as exacerbation of symptoms with coughing, sneezing or straining at stool, require little emphasis, but simple useful clinical tests are often neglected. Production or exacerbation of symptoms by positional change such as flexion (which suggests disc protrusion), extension (which suggests facet joint disease) or tilting to one or other side (which suggests osteophytic or disc encroachment) is often omitted, as is a search for local paravertebral muscle spasm. The value of these tests is enhanced considerably when the manoeuvre also produces distinct dysaesthesia along the territory of a particular nerve or root. The dermatome and peripheral nerve distributions are illustrated in Image 1 and 2. It is too often stated that the clinical picture may be confused by multiple level involvement and by vascular involvement and this is often true. More often, however, it is an excuse for careless clinical practice. The importance of attempting to localise the lesion is underlined by the all-too-common patient who presents for cervical fusion with the scars of unsuccessful surgical intervention at the wrist and elbow clearly evident. There are better ways to localise the level of involvement than multiple surgical exploration.


A common clinical problem is the patient who presents with pain in the shoulder but whose symptoms owe their genesis to disease in the cervical spine. This is the counterpart of the similar problem of referred pain discussed above in the context of the lower limb. The first clue arises during the clinical examination, when the symptoms are exacerbated by rotation or tilting of the head. The second is simply to ask the patient to place his or her hand over the pain. If the hand is placed over the clavicle or above, then the source of the problem is in the neck. If the hand is placed over the deltoid insertion, then it is likely that the pain does indeed stem from the shoulder itself. Confirmation may be obtained by finding clinical clues to the presence of disease in or around the shoulder. A further clinical clue of inestimable value is the presence of distinct and prolonged stiffness in the morning and after inactivity, indicating the presence of one of the inflammatory arthritides.
The first step in the management of a patient with pain in the neck, therefore, is precision in diagnosis and assessment. Thereafter all of the general principles discussed above with reference to peripheral joint disease find equally important application. Reassurance, removal of treatable complications and co-diseases, and non-specific general measures are again more important than the selection of an antirheumatic drug. With particular reference to the neck, advice to alter inappropriate sleeping positions and the correct use of pillows may suffice; the following guidelines are given:
- Maintain a good posture, with your head, neck and chest in a straight line
- At night use only one pillow
- Avoid carrying heavy weights by hand
- Support arms on a chair rest when sitting
- Avoid the stooping posture
- Perform exercises three or four times daily to mobilise the neck and to strengthen the neck and shoulder muscles
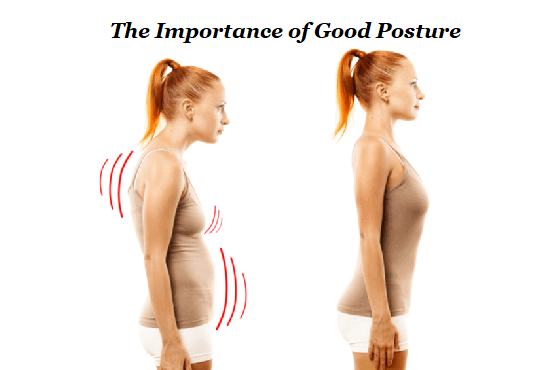
The balance between rest and exercise is again important, and the general rule is that the only thing which will relieve acute pain is rest and time. Thereafter as soon as the pain is relieved the patient should be encouraged to commence a graduated, carefully supervised exercise programme directed both generally and locally. Swimming is one of the simplest and best therapeutic modalities. The purpose of the programme is secondary prevention and this must be explained to the patient. It is worth emphasising that activity, involvement and the attainment and maintenance of the patient’s maximum physical fitness and mobility are the cornerstones of management. The practice of simply dismissing the patient with an inappropriate and ill-fitting cervical collar is to be deprecated. If a collar is indicated because of persisting pain, it must be properly fitted to achieve the dual role of comfort for the patient and partial immobilisation of the neck. As soon as the acute episode is over, the collar should be discarded, except in a few elderly addicted patients or in those patients who derive benefit and in particular achieve an otherwise impossible night’s sleep from this measure. Unnecessary long-term use of collars should be discouraged since it interferes with a mobilisation programme, encourages the patient in invalidism and dependency and predisposes to vertebral osteopenia and loss of muscle tone.
There remains a numerically small but clinically important group of patients who do not respond to these measures. In the presence of unremitting pain or in particular of advancing neurological symptoms and signs, continuous cervical traction may be required. It hardly requires stating that this carries a potential morbidity and extreme caution is required. These patients require admission and the availability of a fully trained and interested nursing staff is essential. In this situation and in that further group of less acute but nevertheless non-responding patients, close consultation with the surgeon is again mandatory. The most unequivocal indication for surgical intervention is the surgical emergency of a central disc prolapse with local pain, neurological signs and sphincter disturbance. In the other group of more chronic patients the indications are less clear and individual judgement is critical. The surgeon likes to see a situation where there is a clear-cut local and focal lesion, and it is in such cases that the best results are obtained from operation. The further the clinical situation departs from this, the worse become the results. The most serious error is in failure of assessment, and here an evaluation of the patient’s personality and previous response to adversity and pain must be included.
It is conspicuous that little mention has been made of drug therapy. In fact antirheumatic drugs are often very disappointing in such patients. Pure analgesics may be preferred by the patient but the general principles of selection and prescription apply. Every attempt should be made to raise the pain threshhold and to minimise the need for drug therapy. The patient should be encouraged to select a single preparation on the basis of patient preference and both daily and total dosage should again be kept to a minimum.