Parkinson’s and Depression

Coping with Depression
As many as half of all Parkinsonian patients suffer from depression, compared to only 10 percent of the general population. Although the depression that Parkinsonian patients suffer is typically mild, a significant number report moderate to severe depression.
Some investigators have argued that the depression suffered by Parkinsonian patients is a reaction to the chronic impairment in motor functioning; that is, depression is secondary to the discomfort and inconvenience of the disease. However, several studies have found Parkinsonian patients to be significantly more depressed than other groups of patients who suffer from the chronic and irreversible motor impairment such as that brought on by arthritis. Also, there does not appear to be a relationship between the severity of the depression and the duration or severity of Parkinson’s disease, which runs counter to the hypothesis that the depression is primarily a reaction to the debilitating effect of the disease.

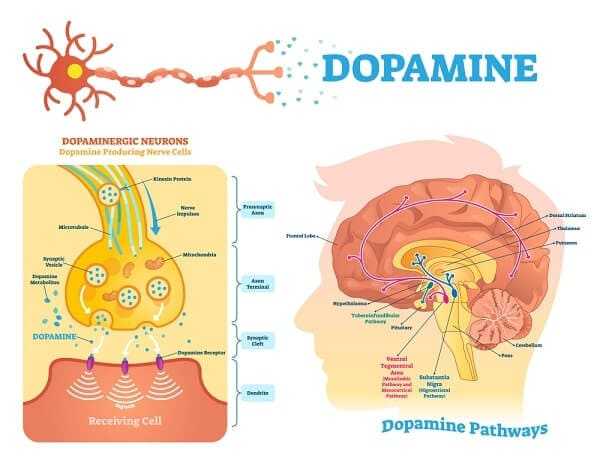
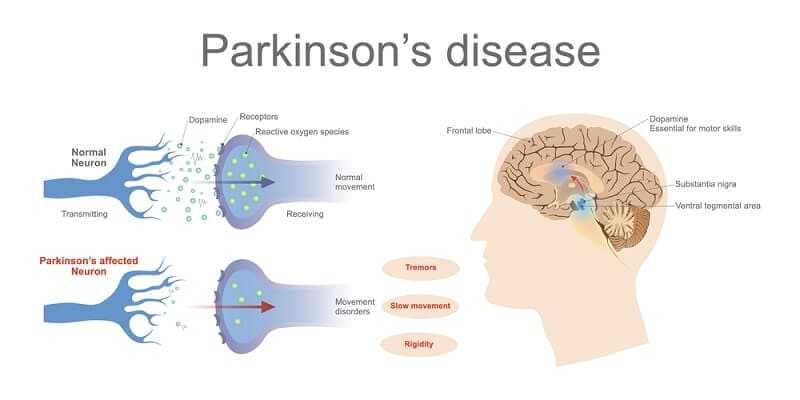
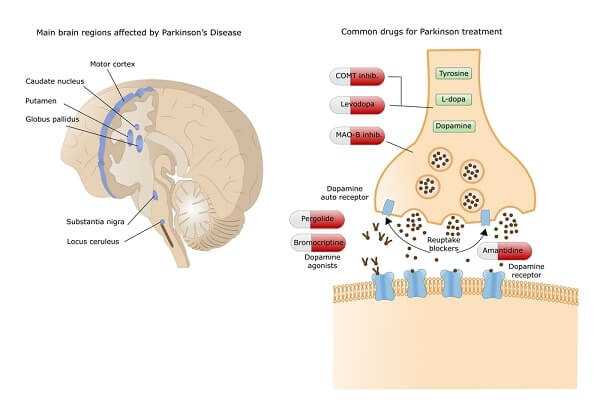
The increased prevalence of depression in Parkinsonian patients is most likely a result of reduced levels of brain monoamines, also called neurotransmitters. Neurotransmitters are the chemicals that allow nerve cells in the brain to communicate with one another and to send signals to muscles or sensory organs. Neurotransmitters are also important in the regulation of moods. The four major kinds of neurotransmitters include dopamine, norepinephrine, serotonin, and acetylcholine. Parkinson’s disease is associated with a depletion of dopamine. Norepinephrine and serotonin are also somewhat depleted in the brains of Parkinson’s victims, and these monoamines are also known to be depleted in the brains of depressed individuals. In fact, antidepressant medication acts to increase brain monoamines.
There are many other factors that may contribute to the development of depression. Many individuals with Parkinson’s disease are greatly frustrated by the rigidity, akinesia, and the tremor that interferes with their ability to complete even the most simple task, whether it be buttoning a shirt or writing a check. When the ability to move from place to place is made difficult, individuals may restrict their social activity, thereby intensifying feelings of loneliness and isolation. Parkinsonian patients report embarrassment at their tremor, their shuffling gait, and their poor posture. A friend of mine who has the disease disclosed that he no longer goes to church because people stare at him.
The frustration that Parkinsonian patients feel may express itself as the appearance of being irritable, demanding, or excessively dependent. These behaviors put stress on marital and family relationships. The guilt associated with placing extra burdens on family members tends to lower the patients’ self-esteem. If the patients’ activities are severely restricted, they may necessitate early retirement along with its accompanying financial worries. New activities must be developed to prevent the onset of boredom. The fear experienced when contemplating an unknown future or personal mortality must be faced head on. Given that Parkinsonian patients may have a biological propensity toward the development of depression, besides the stressors just discussed, it is very important that the physician, the nurse, the psychologist, or a family member recognize signs of depression and act to treat the disorder.
Diagnosis of Depression
Depression may not be readily apparent. Elderly depressed patients often do not present the same complaints witnessed in depressed younger adults. Elderly patients may not describe themselves as depressed, preferring instead to suffer quietly in a strong, stoic manner, perhaps fearful of being even more of a burden to their families. The depressed elderly may be less likely than younger persons to discuss openly feelings of despair, poor self-esteem, and worthlessness; older persons may be less inclined to complain of guilt.

The elderly are more likely to complain about feeling tired, loss of energy, sleeplessness, poor appetite, or a vague array of physical problems. It is often difficult to determine if these complaints are solely due to the Parkinsonism, or if depression has intensified their severity. The depressed elderly are less prone to tears than are younger depressed patients, and may be more likely to expess their depression by appearing irritable, on edge, or quick to anger. Those elderly who are suffering from depression frequently complain of memory problems or mental confusion.
It is important to identify depressed Parkinsonian patients and to treat the depression quickly and completely. Depression can be a fatal disorder: the risk of suicide in the elderly is many times greater than for younger people experiencing depression, and it may be four times greater for a depressed male than for a depressed female. Widowed and divorced individuals are also at considerable risk. Parkinsonian patients are at greater risk than most groups: the presence of a physical illness greatly increases the likelihood of suicide in the elderly. These losses are a real tragedy, because depression is an illness that can be treated with good results in most cases.
If a Parkinsonian patient discusses thoughts of suicide, take these statements seriously. Don’t fall victim to the popular myth that if an individual talks about suicide, then he will be less likely to follow through. In most cases the victim does make an effort to let others know how much pain he is experiencing. Empathizing with those who suffer depression, taking their suicidal threats seriously, and acting immediately to find suitable treatment will go a long way toward saving lives.
Although Parkinsonian patients may run a greater risk of depression, occasionally the caregiver may also fall victim to depression. The increased stress of a changed lifestyle, resentment about assuming added responsibilities, and the guilt fostered by resentment toward the increased dependency of a loved one, may at times be more than caregivers can bear by themselves. Fear of hurting a spouse or family member often leads to silent suffering, and ultimately to depression. If this occurs, it is important that the caregiver receive treatment.
Treatment for Depression
Traditional methods of treating depression are recommended for Parkinsonian patients: antidepressants have generally been found to diminish the symptoms. The combined treatment of levodopa and antidepressants is generally well tolerated by Parkinsonian patients. These antidepressants are often started at low dosages and increased slowly. As with most medication prescribed for the elderly, lower dosages may be used than for younger adults and serious consideration must be given to the effects of combining various drugs. Monoamine oxidase inhibitors, another type of antidepressant, are not considered safe when taken in conjunction with levodopa. Electroconvulsive therapy (shock treatment) is sometimes useful in treating severe cases of depression that do not respond to other forms of therapy.
In addition to drug therapy, depressed Parkinsonian patients may need counseling. Mental health assistance may aid victims of Parkinson’s disease in their efforts at adjusting to this progressively debilitating illness; it is particularly important when the patient is also suffering from depression.
Let me stress that severely disturbed behavior need not be present for counseling to be either warranted or helpful. Clinical psychologists and other mental health professionals are trained to help patients and caregivers discuss openly fears and feelings that may be difficult to share with others.
Strategies to Combat Depression
Many things can be done to prevent feelings of depression or to diminish such debilitating feelings if they occur. When depression sets in, simple tasks and activities become difficult if not insurmountable. To combat these obstacles, start with small goals and gradually increase expectations in a slow, progressive manner. Do not invite failure by setting goals that cannot be reached.

Parkinsonian patients should be very specific in describing their goals; effective means should be provided to evaluate whether these goals have actually been accomplished. If stated goals have not been accomplished, patients should review the reasons for this and, if need be, modify their goals or develop new strategies for obtaining them. Everyone needs goals for their growth and development. When depression emerges, it is especially important to identify goals if feelings of helplessness and hopelessness are to be overcome.
Possible Goals
* Meet a new friend this month.
* Exercise twenty minutes, three times a week.
* Read a new book in an unfamiliar subject area this week.
* Practice listening to someone’s concerns and then ask for feedback regarding listening
effectiveness.
* Organize and label photos by the end of the month.
* Call an old friend.
* Dictate stories of your own childhood so that your children (and possibly their children)
can gain a sense of family history.
* Write a poem.
Notice that well-formed goals often include a time frame for completion. We sometimes work better with deadlines, and these also provide specific time to review accomplishments and to reevaluate progress toward emotional and physical health. Patients might consider establishing the following ritual: every Sunday morning (or at some other established time) weekly goals are determined and those of the past week are evaluated. What a special way to share one’s self with family or friends.
When Parkinsonian patients establish their goals, the following considerations are recommended:
1. Make goals realistically obtainable. Set small goals.
2. They should feel good about themselves when a goal has been successfully accomplished; an appropriate reward could be enjoyed.
3. When goals are not accomplished, develop new strategies or alter the goals to make them more attainable.
4. Do not belittle or trivialize goals or successes. Do not exaggerate failures!
5. Be expressive and creative in developing goals! Patients should consider doing things they have never done before. Be daring and playful!
To fight depression and promote good self-esteem and life satisfaction, goals should address the following areas:
Exercise
* walking
* stretching
* posture exercises
* speech exercises
* (if necessary) passive exercises like isometrics
* swimming
Structural Activities
* crafts
* gardening
* volunteer work
* reading
* writing
* movies
Social Interaction
* church
* volunteer work
* out-of-town visits
* entertaining
* shopping or lunching with a friend
* support group meetings
Improved Communication (with spouse, family, and friends) Discuss the following feelings:
* fear
* loneliness
* embarrassment
* anger
* frustration
* hope(lessness)
* helplessness
* joy
* love
(Write or dictate letters that examine feelings and relationships. There is no need to mail them.)
Rewards
Many people are stingy when it comes to rewarding themselves for their hard work and effort. Depressed individuals frequently feel they do not deserve rewards. These people need to find ways to feel special and important. The reward need not be elaborate or expensive: treating oneself to a shopping trip, a meal at a new restaurant, or just buying some flowers to brighten a room; calling a special friend or visiting a relative; enjoying a bubble bath or a relaxing day at the park. It is vital that Parkinsonian patients realize that they have value as human beings and they deserve all the good things in life.

Negative Self-Talk
It is also important for patients to reduce self-critical statements such as “Em no good to anybody,” “I can’t do anything,” “Em too slow, ” etc. Caregivers may find it useful to count every negative self-statement and display the tally in a conspicious place. Patients will be surprised at how often they focus on what they cannot do rather than what they can do! Instead of focusing on failures, patients should review their positive accomplishments. Individuals should attempt to be as generous with self-evaluation as they are when assessing the accomplishments of others. For example, a patient might review his life and make the following list:
* I raised two wonderful children.
* I was a solid, dependable employee.
* I have a loving relationship with my spouse.
* I walked around the block today.
* I finished my library book.
* I helped my wife/husband (fill in with a special task) today.
If the patient is unable to determine positive accomplishments, then the depression may be well entrenched; a mental health professional may need to be consulted.
What is a Clinical Psychologist?
Clinical psychologists have an undeserved reputation for being the mental health professionals to whom “crazy” people go for help. Actually, the vast majority of work performed by psychologists focuses on quite ordinary individuals who find themselves confronting special problems in their lives. Generally, counseling is brief in duration and much less expensive than commonly believed.

There is often confusion regarding the distinction between different types of mental health practitioners. Psychiatrists, for example, have earned a medical degree and have completed a residency program in psychiatry. They provide counseling and are licensed to prescribe medication.
Psychologists have completed a doctoral program (Ph.D., Psy.D., or Ed.D.), which typically includes three to four years of course work and practical experiences, and a year of clinical internship. Before being licensed to practice independently, the psychologist must hold a doctoral degree, have one or more years of postdoctoral experience under the supervison of a licensed psychologist, and pass a state-administered examination. In most cases, individuals with master’s degrees in psychology are referred to as psychological associates and must practice under the supervision of a licensed psychologist.
What Psychologists Do ?
Psychologists offer a wide variety of services to the public. Only a few of the available services will be discussed here.
Psychological Testing
One of the most valuable skills that a psychologist develops in training is the administration and interpretation of psychological tests. There are many kinds of tests, but some of the most commonly used are those designed to measure intelligence, personality variables, and neuropsychological functioning.
Intelligence testing and neuropsychological testing are often requested to assess possible brain impairment. Neuropsychological testing assesses the patient’s cognitive functioning. These tests measure an individual’s ability to remember, to calculate, to use language, and to think abstractly. Such testing is particularly important if there is some question of brain impairments due to stroke or to a neurological disorder such as Alzheimer’s disease.

Some Parkinsonian patients also suffer from cognitive impairment. If there is reason to suspect that the patient is showing cognitive decline, it is often helpful to undergo neuropsychological testing to measure areas of weakness and strength. The results of such testing may suggest adjustments that the family should make to ensure the patient’s safety and to protect the patient from unreasonable expectations or demands.
It is often difficult to determine if mental confusion and forgetfulness are due to brain impairment or depression, since many depressed individuals complain of difficulty with memory and concentration. Neuropsychological testing and personality testing may be useful in locating the problem and indicating what form of treatment will be most appropriate.
A psychologist conducts personality testing to gather information regarding a patient’s current emotional state and the personality variables that influence behavior. Personality assessment is particularly useful in diagnosing depression and in assessing the risks of suicide. It is also useful for suggesting what factors might be modified to enhance life satisfaction. Common personality tests include:
1. Minnesota Multiphasic Personality Inventory (MMPI). This is a pencil and paper test with over four hundred questions regarding likes and dislikes, past and present emotional experiences, and physical symptoms.
2. Rorschach Inkblot Test. This famous projective test has no right or wrong answers. The subject “projects” internal experiences onto a neutral stimulus (the inkblot). This is a very useful tool for understanding how an individual perceives the world.
3. Thematic Apperception Test (TAT). This is another projective test in which subjects are asked to tell a story suggested by several drawings.
4. Depression Inventories. These are composed of several questionnaires specifically designed to assess depression.
Individual Psychotherapy
Therapists differ as to style and approach toward treatment, and each client presents different issues and needs. Based on test results or an initial interview, individual therapy may be recommended to help clients work through issues that may be creating stress, dissatisfaction with life, or depression.
Therapy may be very brief, lasting one to eight sessions, or it may last for several years, depending on the client’s needs. The average length of therapy is probably between six and twelve months. The expected duration of therapy should be discussed with the psychologist during the first couple of sessions. Problem-solving sessions may prove adequate when seeking solutions to obvious situational obstacles (e.g., loss of income, or lack of interesting daily activities). Alternatively, the therapist and the client may agree that the therapy sessions should focus on internal experiences, such as feelings of poor self-esteem and guilt.

Psychotherapy is a very personal process that relies heavily on a strong relationship between therapist and client. Trust is essential to a positive outcome. If for some reason the match does not “feel” right, and the client is dissatisfied with the therapist, these concerns should be addressed at the next session. If the client’s dissatisfaction continues, another therapist may be the solution. The best security against an unsatisfactory experience is to seek counseling from individuals who have had extensive training and experience, and who have the proper credentials. Clients have every right to verify the credentials of prospective counselors.
Marital Therapy
Occasionally, the best arena to tackle the client’s problems is in the presence of the entire family, or in the presence of the spouse. If the husband and wife are having difficulty communicating their experiences or feelings to one another, or find that they argue constantly, a therapist may be able to intervene gently in such a way that a clearer understanding of issues is possible.

When an individual develops Parkinson’s disease, the entire family system changes: Husbands and wives who have always gotten along well together may suddenly find themselves arguing or, perhaps worse, not talking to one another. Real issues may be masked by arguments over inconsequential matters. Through therapy, the family may begin to explore their fears regarding changes in roles, increased dependencies, fears of losing a family member, as well as anger over having to assume extra responsibilities or over an inability to follow through with a responsibility that had been diligently carried out for years. Once the real issues are identified, constructive work can be done to improve the relationship and to confront the fears.
Family Therapy
Parkinson’s disease generally afflicts individuals who are older. Aging spouses or family members may also have health concerns that inhibit their ability to care for the Parkinsonian patient. Increased demands may be placed on the patient’s children or members of the extended family. Many sons and daughters will want to help as much as possible, but demands of work and their own young families may limit the resources and the time they can devote to their loved one who suffers with Parkinson’s disease.

Family therapy can be a valuable forum for reviewing the family’s problems and needs, discussing possible solutions, and clarifying the expectations of each family member. Better communication will help prevent the resentment that pulls many families apart in times of stress.
Conclusion
If professional counseling is sought, a physician may be able to suggest a well-respected mental health practitioner. The psychology department of the nearest medical school, university, or major hospital may be able to recommend psychologists in the immediate vicinity who have received specialized training in aging. These specialists are referred to as geropsychologists. Most health or medical insurance policies provide reimbursement for mental health services, but a careful inquiry to an insurance agent will clarify the services, restrictions, or limitations imposed by the carrier.
Medicare allows reimbursement for psychological services, but with certain restrictions. Medicaid coverage of psychological services is typically more generous. An interdisciplinary team approach to the treatment of Parkinson’s disease can prove helpful. Each discipline has unique viewpoints and specialized skills, which together can focus on the whole person.