Reiter’s Syndrome

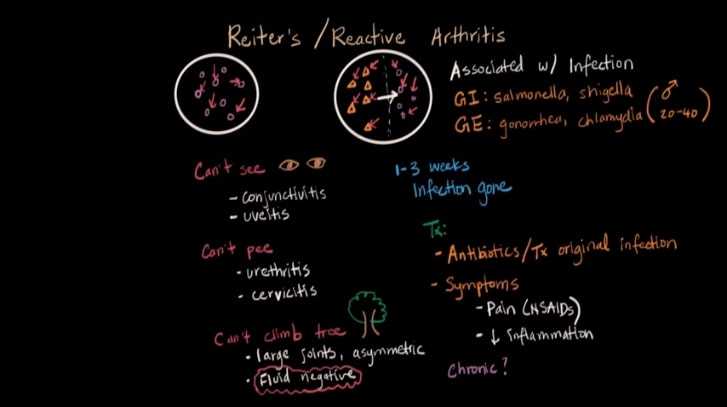
Reiter’s Syndrome, also called Reiter’s Disease, is a form of arthritis that follows several kinds of infectious diseases. It is named after Dr. Hans Reiter, who described the major features of the syndrome in a German soldier who developed it after having dysentery during World War I. Along with arthritis, Reiter’s Syndrome usually includes at least one of the following problems:
•Urethritis—an inflammation of the urethra (the small duct through which urine passes out of the body from the bladder). In men, this inflammation results in a discharge from the penis. In women, it may not cause any symptoms at all.
• Painless ulcers in the mouth.
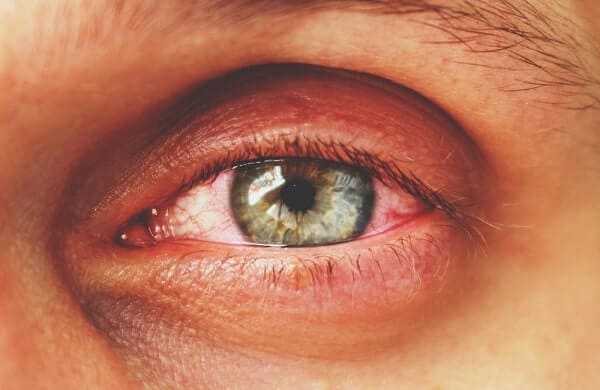
• Conjunctivitis—an inflammation of the eyelids and the eyeball (“pinkeye”).
• Keratodermie blennorrhagica—a chronic skin rash characterized by scaly, reddish patches that can occur on any part of the body, especially the penis.
Reiter’s Syndrome occurs in people with a genetic tendency to develop the disease and is frequently triggered either by some sexually transmitted infections or by certain bowel infections. However, the microbes are not found in the joints; the inflammation seems to be a reaction to the triggering infection. In some people, the disease develops, remains for several months, and then goes away completely. Others have repeated episodes over a period of many years. The disease is usually not as serious as some other rheumatic diseases, such as rheumatoid arthritis, since it does not often produce permanent deformity.
Affected Population
Reiter’s Syndrome primarily affects young men between the ages of twenty and forty, although it may affect anyone at any age. The disease is diagnosed in fewer women than men perhaps because its symptoms are very often not obvious in women.
Physical Effects
Reiter’s Syndrome begins with different symptoms in different people. These depend partly on what type of infection was present before the syndrome began. If the disease is preceded by a bowel infection, the early symptoms will include diarrhea, nausea, and vomiting. If it follows urethritis, the symptoms may be either mild or acute and obvious. In such a case the symptoms include pain or burning on urination and, in males, a discharge from the penis or urethra.
Several days or weeks after the symptoms of infection begin, pain occurs in one or more joints. The knees and the joints inside the balls of the feet are the most likely to be affected, but any joint may become painful. There may also be pain under the heels, in the lower back, and in the ribs. The affected joints are usually swollen and warm. Although the joints usually begin to improve after two or three weeks, many people continue to experience pain, especially in their backs and heels, even after their other symptoms have gone away.
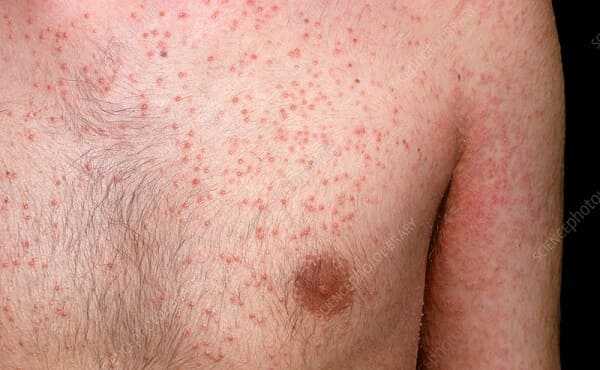
Most people with Reiter’s Syndrome develop the conjunctivitis with redness and irritation of their eyes. This complication usually appears during the first two weeks of a flare-up, if at all. It usually disappears of its own accord, without treatment, and leaves no permanent damage. Another symptom of Reiter’s Syndrome is a type of skin rash that occurs in ten to thirty percent of people with the disease. It is a reddish rash that may appear on the soles of the feet, the palms, and other areas of the body.
Usually, it is not painful or serious, and goes away in a few weeks. There may also be small red spots on the end of the penis, on the roof of the mouth, or on the tongue. Besides this, most people with Reiter’s Syndrome have a slight fever, and some lose weight. Some people have only a few of these symptoms and are said to have incomplete Reiter’s Syndrome. For example, they may have arthritis alone, with no other features.
Possible Causes
The cause or causes of Reiter’s Syndrome are unknown, but medical scientists have found some clues they are studying further. Most people who develop Reiter’s Syndrome have had infections of their genitourinary system or enteritis, infection of the bowels. Why some people who develop these infections develop Reiter’s Syndrome, whereas the majority do not, is probably related to a genetic susceptibility.
Genetic Markers
The HLA-B27 genetic marker, which is found in about eight percent of the general population, occurs in seventy percent or more of people with Reiter’s Syndrome. It is the same genetic marker that is associated with an increased susceptibility to ankylosing spondylitis. Having the HLA-B27 marker does not necessarily mean that a person will get Reiter’s Syndrome; it simply means he or she has a higher chance of developing it than do people without this marker. In fact, very few of all people with the HLA-B27 marker actually develop the Syndrome.

Infections
Although certain infections do seem to trigger Reiter’s Syndrome, not all of the agents causing these infections have been identified. They are not found in the joints, which makes them more difficult to pinpoint as the culprits in the disease. Sometimes the disease seems to be triggered by certain bowel infections, particularly those due to certain species of bacteria, shigella, salmonella, and yersinia.
Scientists have been able to recognize that some of the microbes known to cause genitourinary infections can trigger Reiter’s Syndrome in some people. They do know that such infections can be caused by several kinds of organism that are passed from one person to another by sexual contact; small microbes related to bacteria called chlamydia and ureaplasma have been linked to Reiter’s Syndrome, but their role has not yet been fully understood.
Diagnosis
The diagnosis of Reiter’s Syndrome is based on the overall pattern of symptoms and on the results of a physical examination. The doctor will ask detailed questions about the joint pain and other symptoms a person is experiencing. During the physical examination, the doctor will pay close attention to the joints, eyes, and skin, and will look for other evidence of infection.
Although no blood or urine tests can prove whether or not a person has Reiter’s Syndrome, such tests help to rule out similar diseases and to determine if an infection is present. The doctor may also remove some fluid from the affected joints to see if another kind of arthritis is present. Testing for HLA-B27 is sometimes helpful in making the diagnosis.
Treatment
Because there is no known cure for Reiter’s Syndrome, treatment is aimed at controlling the inflammation caused by the disease and preventing or reducing joint damage. The goal is to keep the person with the disease comfortable so that he or she can continue normal activities.
The drugs most commonly used in treating Reiter’s Syndrome are the nonsteroidal antiinflammatory drugs. These help to reduce the pain and inflammation associated with the syndrome. Indomethacin is probably the drug used most often at first, although some other non steroidal anti-inflamatory drugs are probably equally effective. Although they can have side effects, as can all drugs, they often provide considerable relief in fairly low doses, so that side effects can be minimized or avoided.
For some people, a drug that did not seem to help at first may turn out to be effective several months later. For this reason, the doctor may need a trial period to find the best drug. In those few people who do not improve on treatment with non steroidal antiinflamatory drugs, cytotoxic drugs such as methotrexate have been tried.
Mild skin rashes caused by Reiter’s Syndrome are usually not treated with medication, since they are likely to go away on their own. Conjunctivitis may be treated with steroid drops if it does not disappear by itself.
Even though Reiter’s Syndrome seems to be caused by infections, antibiotics have not proven to be predictably effective in treating it. This is because the microbes which caused the infections are not found at the sites of inflammation. Nonetheless, antibiotics are sometimes used, especially if the triggereny infection is known, in the hope that they will do some good.
Because of the close relationship between sexual activity and Reiter’s Syndrome, doctors strongly recommend that men who have had this disease use a condom regularly, especially with a new sexual partner.
Emotional Aspects
Because of the probable connection of Reiter’s Syndrome to sexual activity, some people who develop the syndrome are embarrassed by it. Some people even delay seeking treatment because they are hesitant about discussing their problems with a physician. Such people need not worry; the doctor will be concerned about the medical aspects of the disease, and will not judge their lifestyle.
Intimate personal relationships may also be harmed by Reiter’s Syndrome. Communication between sexual partners will be awkward if either partner is embarrassed about discussing the condition. Part of this embarrassment may come from a changing body image. Such symptoms as a body rash or, in men, a discharge from the penis sometimes keep people from feeling good about their bodies. The person with a lowered self-image may well need some emotional support to restore his or her confidence. Patience and understanding are important ingredients in any couple’s relationship, but may be even more important when one of the partners has Reiter’s Syndrome.
Because no consistently effective treatment for Reiter’s Syndrome has been found, some people may lose faith in their treatment and go “doctor-shopping” in an attempt to get well. But since each new doctor must start anew in seeking the best treatment for such people, the result is a loss of valuable time. People with Reiter’s Syndrome need to understand their illness so that they will have realistic expectations of themselves and their physicians. The more they understand it, the better they can work with their physicians in finding the best treatment.
Some people who carry the HLA-B27 genetic marker are concerned about passing the tendency for Reiter’s Syndrome on to their children. Genetic counseling may be helpful to those people who are considering having a family. However, it is very rare for two people in the same family to have the disease.
The Future
Some people have only a single episode of Reiter’s Syndrome, after which the symptoms may disappear, never to return. Others may have repeated episodes with symptom-free periods in between. It is, however, fairly common for people with Reiter’s Syndrome to have continuing problems, such as back pain or pain in the heels.
Researchers are getting closer to identifying the causes of this disease, with the hope of eventually developing effective prevention and treatment.