Stem Cell Therapy: The Ultimate Answer?
It will be years before nanoparticle therapy is available to people with Crohn’s disease, because the research is just beginning. Treatment of Crohn’s is constantly evolving, however, and several new treatments are being tested by researchers around the world.
At the University of Chicago, physician David T. Rubin says, “We are extremely optimistic about new treatments that are coming and look forward to more effective and safe therapies in the near future.” In 2010 Rubin said that there were at least twenty new drugs being investigated and tested as improved treatments for Crohn’s disease. Still, these medicines are treatments, not cures, and finding a cure is the ultimate goal for Crohn’s. Many scientists do believe that a cure is possible. One idea for a cure that is being explored by researchers involves the use of stem cells.
Stem cells are the body’s master cells from which all other cells are formed. They are unique cells that are unspecialized—they do not perform a specific function like heart cells or immune system cells.
However, they are able to differentiate—to become specialized cells—and then to divide and multiply. Stem cells are the way that the body repairs itself, replaces injured or dead cells, and generates new functioning cells. In the bone marrow, in the centers of bones, are stem cells named hematopoietic stem cells. They generate, or give rise to, eight different kinds of new blood cells, including the white blood cells of the immune system. Most stem cells are in a resting state most of the time, but hematopoietic stem cells are turned on and active. This is true because the blood cells are short-lived and must be continually replaced. It is these hematopoietic stem cells that gastroenterologist Christopher Hawkey of Nottingham University in Great Britain is using to try to cure Crohn’s disease.

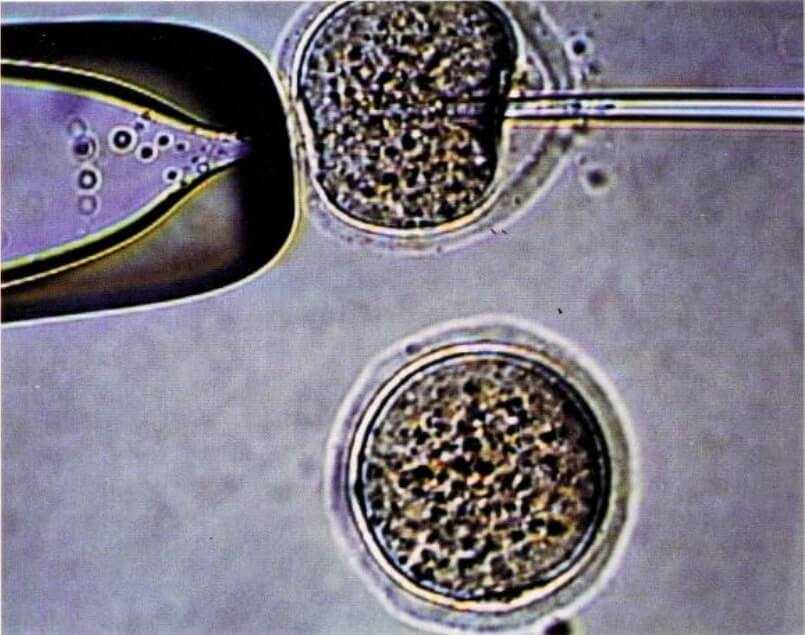
In 2007 Hawkey and his research team began a long-term trial, using stem cells to treat volunteers throughout Europe who have severe Crohn’s disease. The researchers are trying to “reboot” the immune system in these people using stem cell transplants. The treatment involves extracting bone marrow stem cells and preserving them in the laboratory. Then the patient’s own active immune system cells are killed—poisoned in the same way that doctors kill cancer cells with chemotherapy. Finally, the preserved stem cells from the patient’s body are transplanted back into the patient’s body, where they specialize into new immune system cells.
The theory behind this treatment is that the Crohn’s patient’s immune cells, already genetically coded to respond to an environmental trigger, have been “taught” to overreact and cause an inflammatory autoimmune disease. The stem cells from the bone marrow, still urispecialized and undifferentiated, have not “learned” to cause autoimmune disease because they have never been exposed to the environmental trigger. The transplant is a way to let the person start over, with an immune system in the state it was before the environmental trigger happened. Hawkey says, “People with severe Crohn’s have very poor quality of life and at the moment there is no cure for them. So what we are attempting to achieve with this trial is something really quite radical and ambitious—and [that] could make a major difference to the lives of a lot of patients.”
Hawkey’s team has named their study the Autologous Stem Cell Transplant International Crohn’s Disease Trial (ASTIC). (“Autologous” refers to using the person’s own stem cells instead of a donor’s for the stem cell transplant.) By the end of 2010, ASTIC had treated only about seventeen patients with transplants, and it is still enrolling volunteers for the trial. Undergoing the treatment is not easy. The process is painful and difficult and takes about two years. Even when the trial is completed, the results will have to be analyzed, and patients will have to be followed for a long time to be sure that the stem cells have done their jobs. However, says, Hawkey, “I’m hopeful that, half or more of the patients who undergo stem cell transplantation may either be cured or have a long-term remission.”
Toward a Bright, Hopeful Future
Stem cell treatment for Crohn’s is very new, but efforts to develop different stem cell treatments for the disease are ongoing around the world. Many scientists and medical researchers believe that research such as Hawkey’s will lead to cures or vastly improved therapies in just a few years. Wherever the answers come from, most Crohn’s experts believe that new breakthroughs in treatments and therapies are near. Say Warner and Barto, “The past 10 to 15 years have witnessed great strides in understanding the basic immunology of IBD and dramatic advances in the treatment of IBD. With this strong foundation to grow upon, the future for individuals with IBD is both bright and hopeful.”





