What is a Herniated Disc?
What is Disc Herniation?
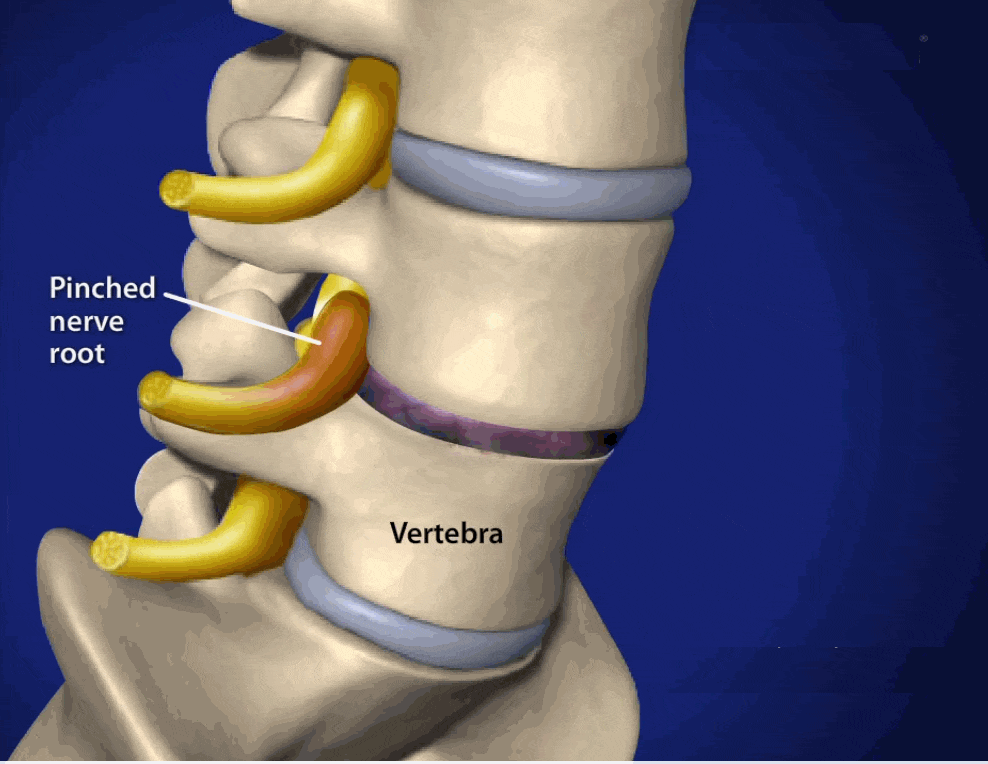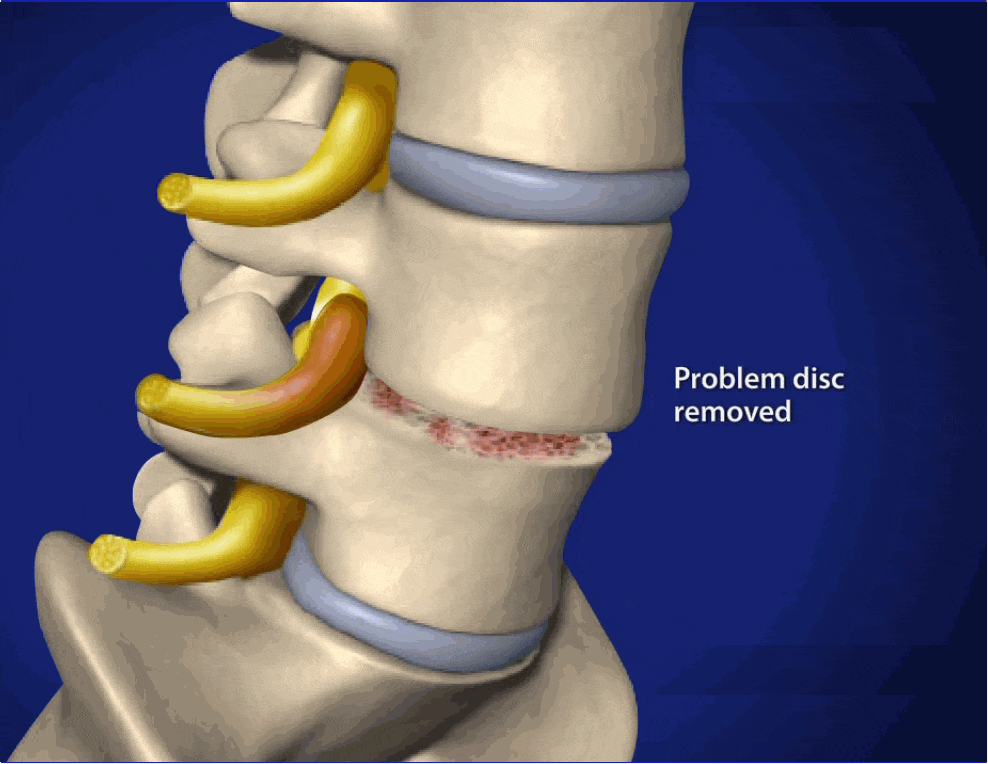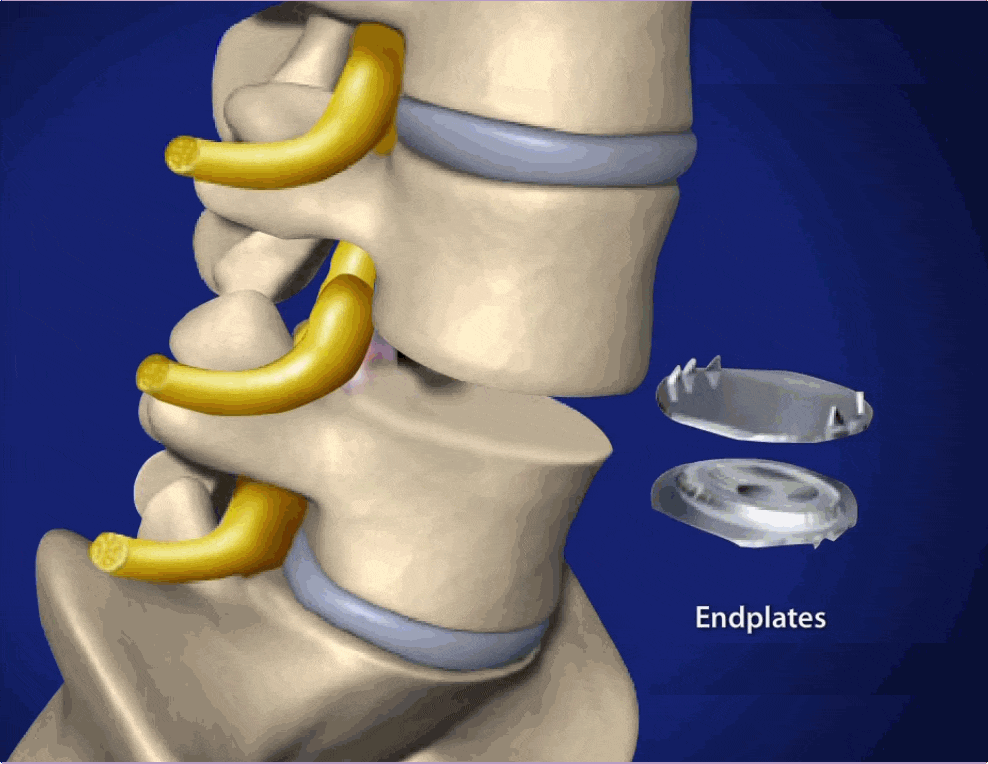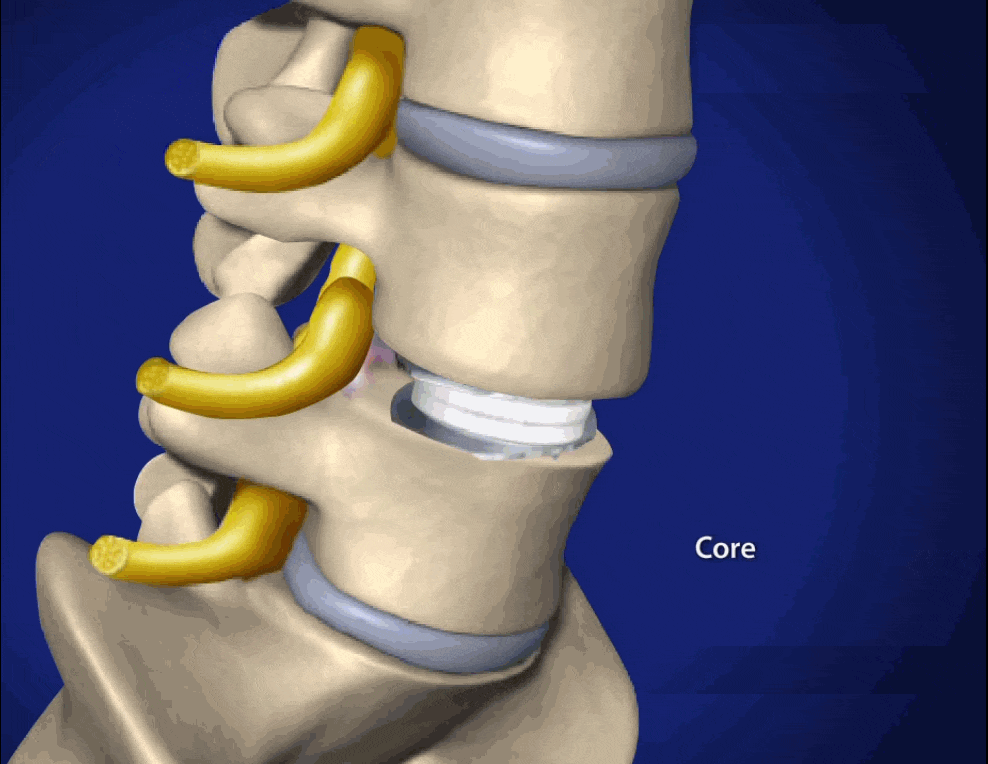
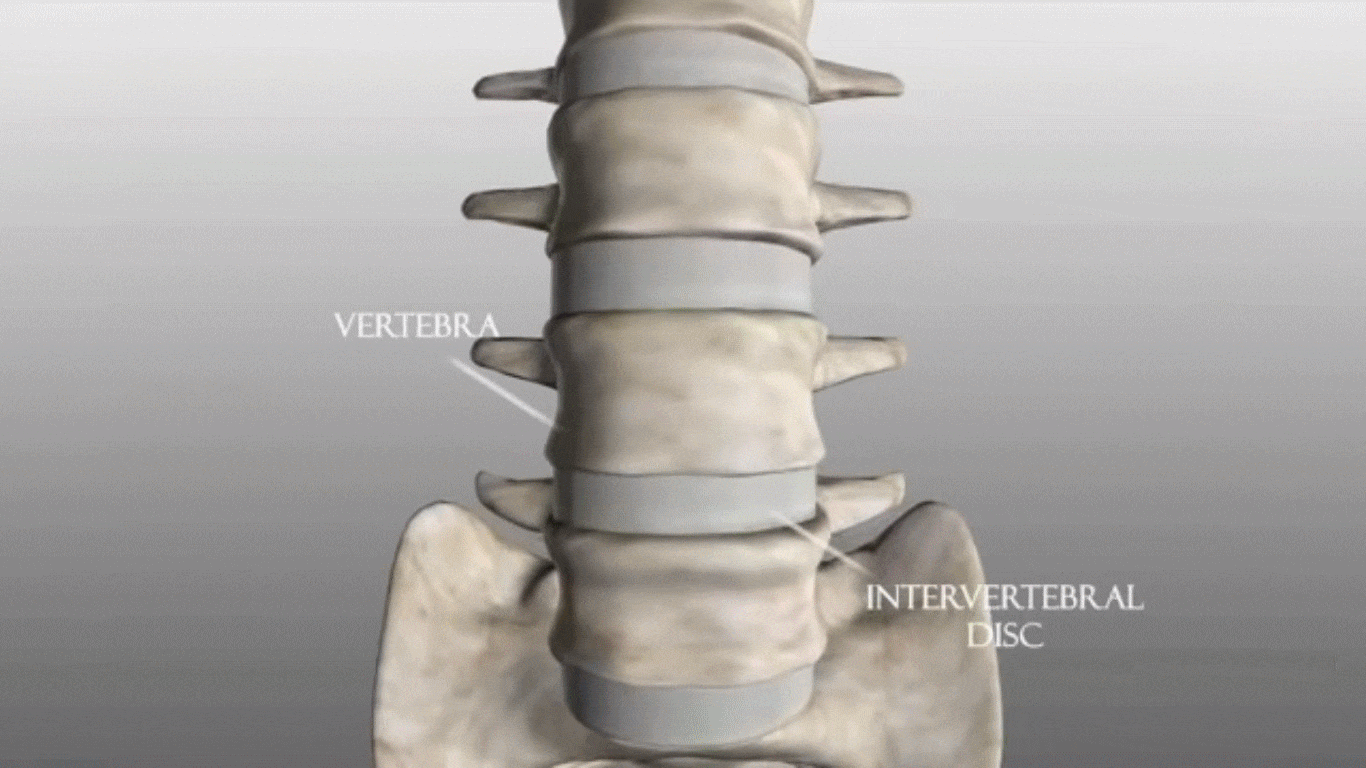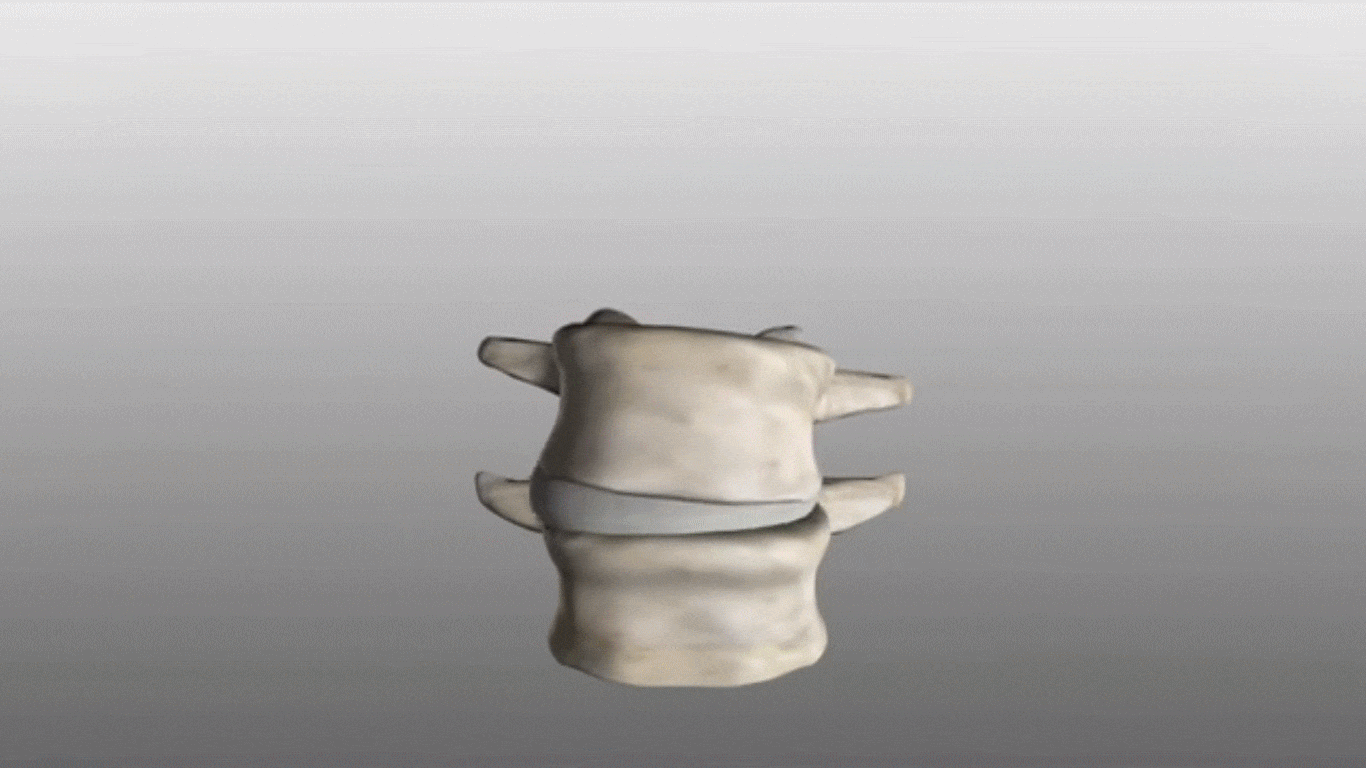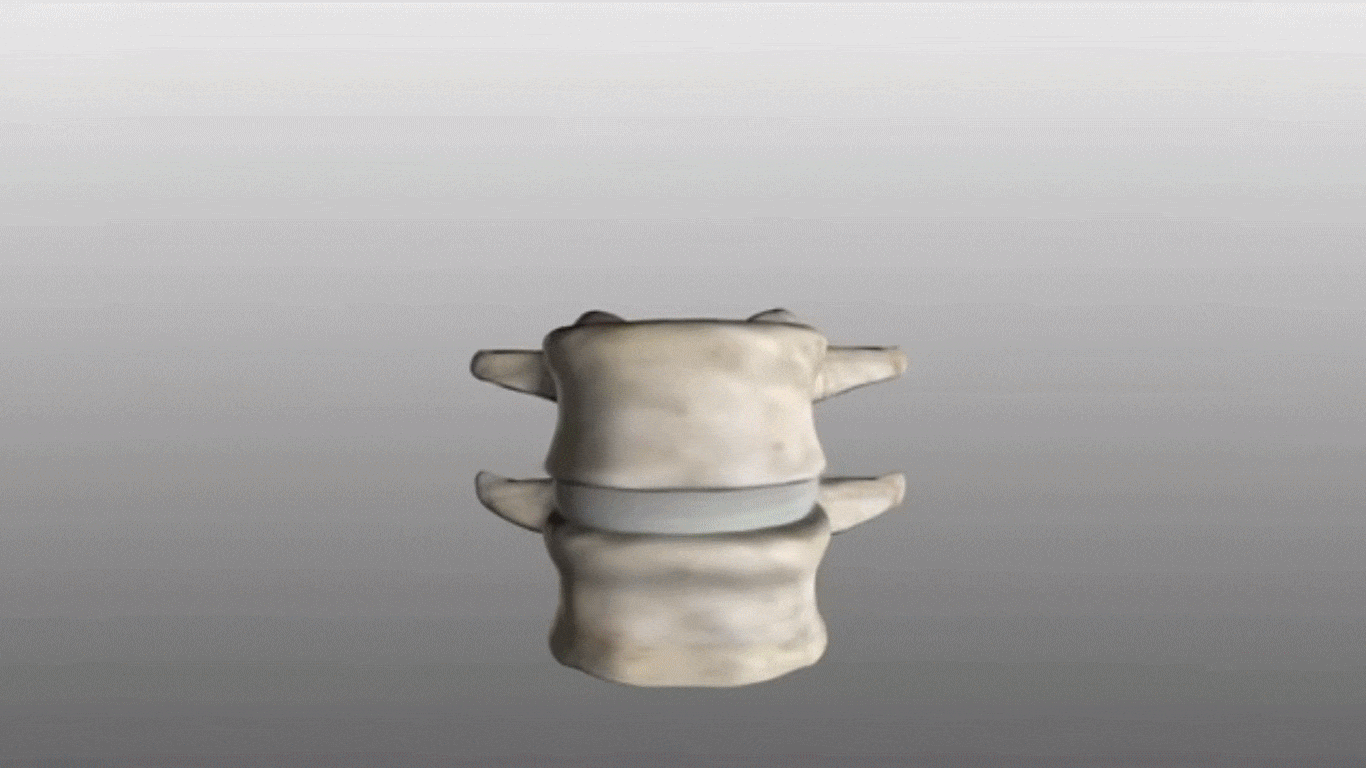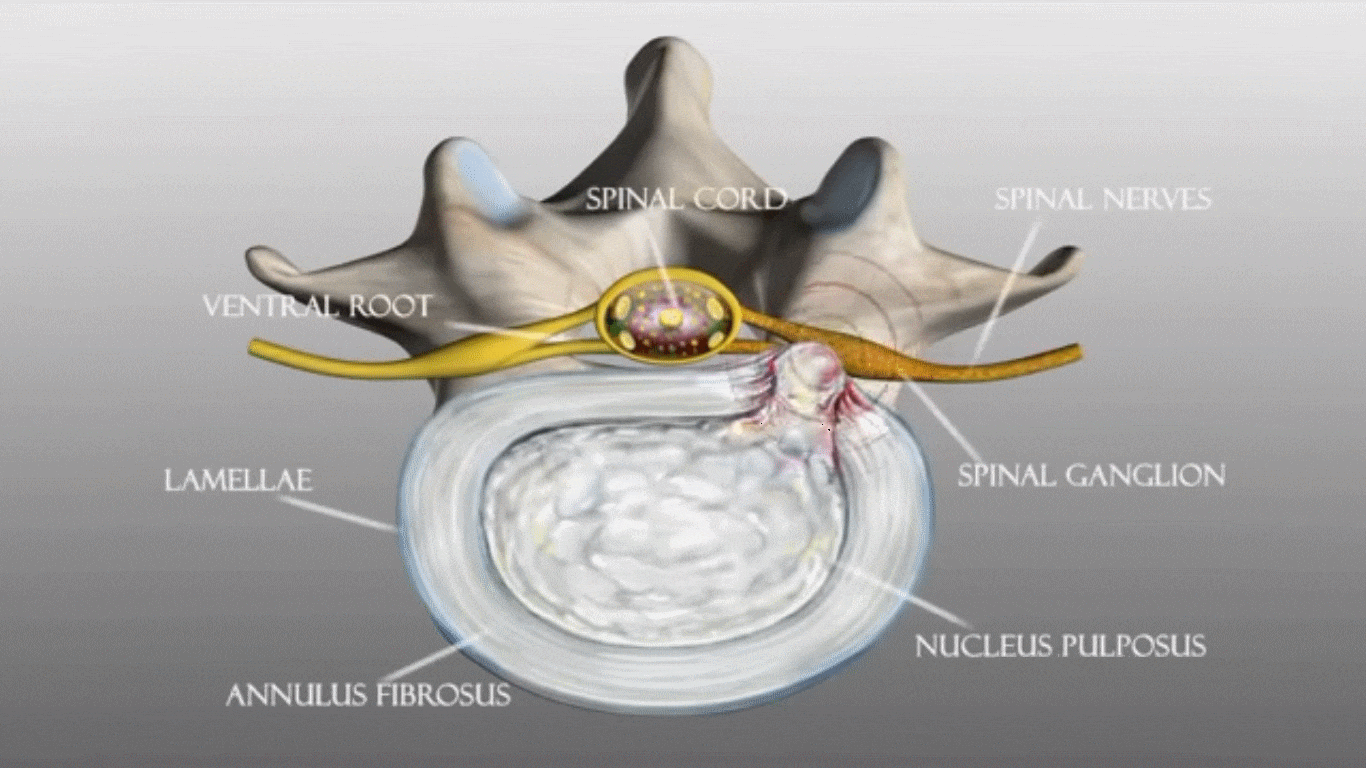
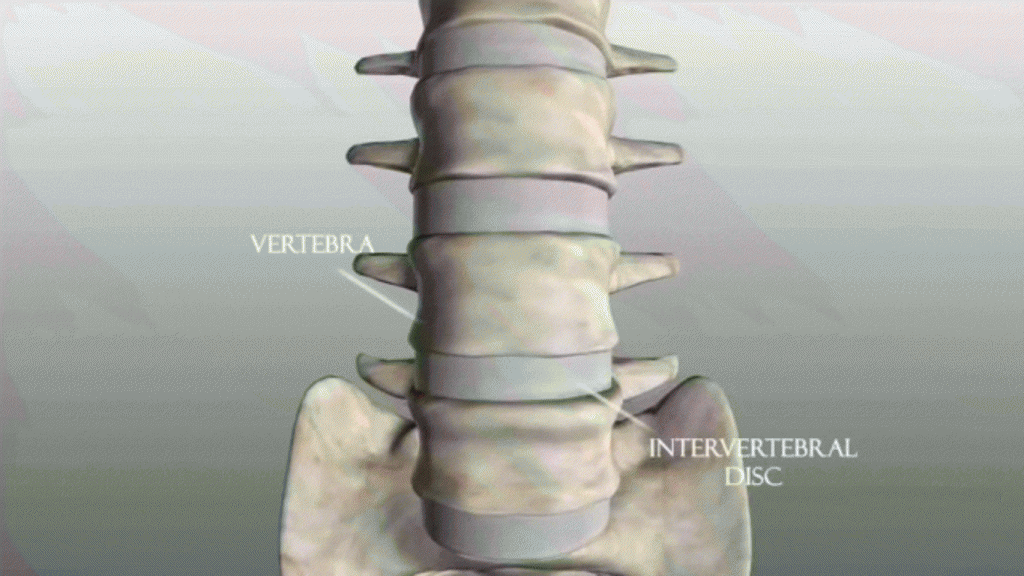
The most common cause of sciatica and other back, hip and leg pain is a herniated disc. This occurs when a disc, the soft, cushion-like tissues that act as shock absorbers to the vertebrae, either ruptures or is partially pushed out of alignment. The term, ‘slipped disc‘ has been commonly used to describe a herniated disc. The spinal nerves lie very close to the spine and so any change in the alignment of the parts of the spinal column can cause pressure or irritation to these major nerves.
Like many other tissues of the body, spinal discs lose their elasticity as we age and this makes them much more susceptible to damage and injury. Deterioration of the spinal discs can start as early as 30 years of age in about one third of the population and so disc herniation becomes more common as we get older.
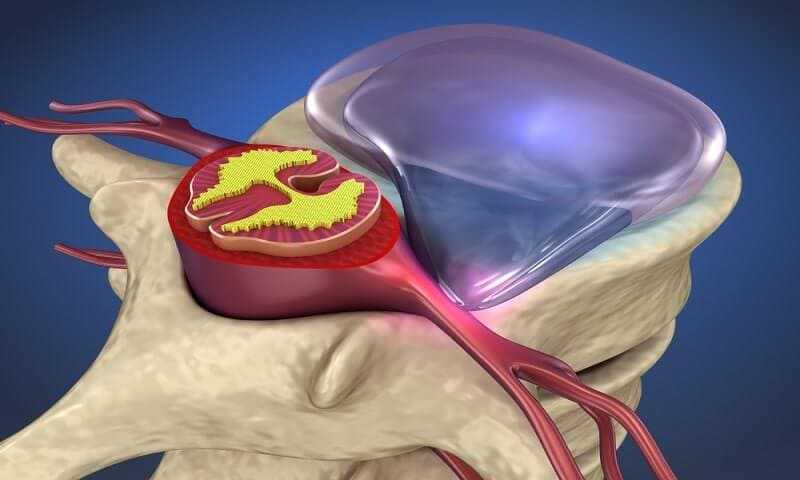
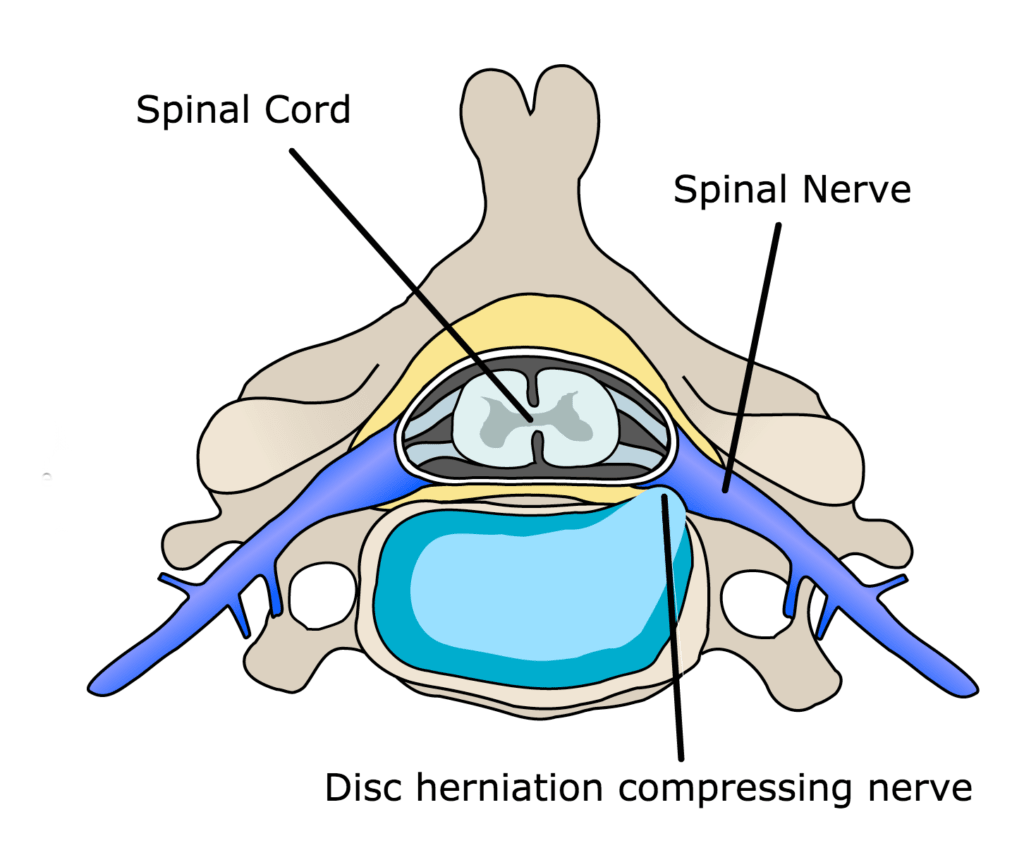
A herniated disc occurs when a piece is pushed out , having ruptured or bulged between the vertebrae. Because there is little space around the spinal cord and spinal nerves, the bulging or ruptured disc often impacts on the nerves, causing irritation or compression to the nerve.
What are the Symptoms of a Herniated Disc?
The most common symptom of disc herniation is pain; where the pain is felt depends on the location of the affected disc in the spine. Other symptoms include muscle cramps or spasms, difficulty moving the affected area, muscle weakness, increased pain when trying to move, loss of feeling in the area, pain in the skin surrounding it, a pins and needles sensation down the limb.
These symptoms do not represent a medical emergency but if bladder or bowel problems occur, immediate medical advice must be sought. The pain, sometimes called nerve pain or neuralgia may be a dull ache, a burning sensation, a sharp pain often likened to an electric shock or a pain that radiates down the arm or leg.
What causes a Herniated Disc?
Sometimes the cause of a herniated disc cannot be determined but it is usually due to either an accident or sudden injury or it develops gradually as the result of repetitive strain being placed on an area of the spine. Poor posture when sitting, standing, carrying or lifting will place undue strain on the spine which in time will cause a disc herniation.

How is a Disc Herniation diagnosed?
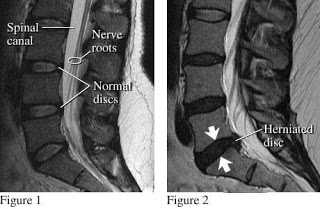
Disc herniation can be diagnosed by a doctor through a physical examination and collecting a medical history. A firm diagnosis can be reached with muscle strength, sensation and reflex tests although CT scan, x-ray, ultrasound or MRI may also be used to locate the exact cause and location of the problem.
Once a correct diagnosis has been made the most appropriate treatment plan can be established. The treatment will be based on certain individual factors such as the age and general health of the patient, the symptoms and their severity, how active the patient’s lifestyle is and whether the symptoms have been getting worse over time.
What is the Treatment for a Herniated Disc?
Treatment usually starts conservatively with rest recommended to allow the irritation and inflammation to subside. Activities that aggravate the symptoms are usually curtailed in the short term. Some disc herniations resolve themselves given time and rest.
To get relief from the pain, the application of heat packs and cold compresses are very effective. Heat and cold, applied to the affected area, relax the muscles, relieve spasms and reduce pain significantly. After the initial intensity of the pain subsides, physical therapy may be used to strengthen the muscles of the torso to correct posture and support the spine more strongly. This can lessen the likelihood of repeated pain from the disc herniation.


Pain medication also helps with the pain associated with a herniated disc, NSAIDS or non-steroidal anti-inflammatory drugs reduce inflammation and pressure at the site of the disc which is a contributor to the pain and muscle relaxants reduce cramping and muscle spasms.
Oral steroid drugs are powerful anti-inflammatory medications which reduce inflammation and relieve symptoms. Some of these have significant side effects so be sure to ask your doctor about this. Cortisone injections into the site of the herniated disc relieve the pressure on the compressed nerve in severe cases; this type of treatment is faster acting than oral medication.
If these conservative and moderate treatment measures are not successful at controlling disc herniation symptoms or the patient is experiencing on-going problems, surgery may be considered. During surgery, bone may be removed around the herniated disc to allow the nerves more space or the part of the disc that is protruding outside the vertebrae may be removed. In severe cases, especially after trauma, the disc may be removed completely.
How can I Prevent further problems from a Disc Herniation?
To help prevent pain in the future, there are several things you can do. To keep your back strong and healthy you need to watch your posture when you lift heavy things, when you sit or stand for long periods and when you bend forward from the waist. Regularly do exercises which strengthen the core muscles, maintain a healthy weight, get regular exercise and don’t smoke. With a few lifestyle changes, you can protect your back and avoid the pain from disc herniation.