Coping With Crohn’s
Staying Positive With Crohns
Your mental game is one of the most important aspects of your fight with any disease. Keeping an optimistic outlook on your life will go a long way in your battle with this monster.
The main thing that helps me to stay positive throughout all my struggles is that having Crohn’s has helped me not to take things for granted as much. I wake up every day and I’m glad to be alive. That doesn’t mean I’m glad I have to wake up so early, mind you! But at least I still have the ability to stand up out of bed and go live my life.
Be thankful for all the things you do have that are good; the things you enjoy doing, the material possessions you’ve been blessed with, and the people in your life you find comfort in.
Be thankful for all the things you don’t have that you could; Crohn’s is one disease among millions, and personally if I had to choose a chronic condition I’d choose Crohn’s over lots of others that come to mind.

Concentrate on making time for yourself. Sit back and relax. Get some sleep. Stay in bed for longer than you should; the world will still be spinning when you get up.
Dealing With Your Stomach Noises
For me, the noises my stomach makes are almost worse than the actual fact that I have to use the bathroom more often than most people.
I’m in my 20′s and while I usually stay in relatively safe places where I can find a moment to saunter off and do my business, it’s a lot more embarrassing to be alone with, say, a member of the opposite sex, and be getting into a deep conversation in an otherwise quiet room when all of a sudden, “SQUEEEEEEEEEEEEEEEE!”
I’m like, “sorry, my stomach is loud,” or “my stomach makes a lot of noises.” Then I’m just like, “so, wanna make out?” Only kidding.

It’s worse when I’ve just come back from dinner or having eaten in the presence of a date, because it’s harder to use the “I’m hungry” excuse when your innards decide to act up then. Sometimes the sound is really gross though and I’ve got to start talking loudly when I know it’s about to happen, or make noise with something else as a distraction, so you can’t hear my guts doing a drum solo.
The only real way to deal with stomach noises is to watch what you eat, expel your noxious fumes before you go out, and stay away from the foods you know will put up a fuss. This can be different for everyone – for me the worst ones are lettuce, chocolate, bread, and potatoes. When people offer me chocolate potato sandwiches, I always say no thanks.
I think food choices can really do a lot to quell or cause stomach noise, so pay close attention to how your body reacts from the different things you eat. Over time you can get a pretty good idea of what to expect from the chocolate monster and other terrible abominations.
Bathroom Habits
Too often, timing is everything when you’re living with Crohns disease. I hate to admit it but a lot of times it comes down to how long I can hold it – or how long I care to hold it before I just give in and use a public bathroom.
I start thinking, “okay, if I wait until I get home it’ll be [X] minutes, but if I just get it over with now I’ll be fine for the next [X] hours.” It’s a sad existence, but you have to make do with what you’ve got.
If you’re in a place where you’re using the bathroom more than half a dozen times a day, or however much it takes to become a serious inconvenience for you, tell your doctor. I am by no means a proponent of taking more meds than you need to, but sometimes it’s better to bite the bullet and take something if a problem gets out of hand.

A lot of your symptoms can be controlled just by what you eat, but that’s a different topic for a different page. Check out my Diet and Nutrition.
Weight Gain And Loss
I have literally had some of my closest friends tell me I looked like a skeleton. You want red, rosy cheeks? How about that for calling someone out in front of a crowd of people?
That was back when I weighed almost fifty pounds less than I do now. I was in my absolute worst state ever since I’ve had Crohn’s. I heard things like that all the time; people told me I looked like I was on drugs, like I had just escaped from a concentration camp – you name it, they said it.
The hilarious thing is, they were right! It would’ve been funny if it had been anyone else but me.
Pain, cramping, bloating and other internal symptoms associated with Crohn’s are things that no one else knows unless you make it apparent to them; your weight is an entirely different matter.
As you go through flares and remissions your weight will most likely fluctuate, and often there isn’t a whole lot you can do to control that. If you’re like me, you might have a couple different sizes of pants.
I’ve got my skinny jeans and my healthy jeans. Right now my biggest jeans are tight around my thighs, but when I’ve been my thinnest even my smallest pairs of pants were falling off, my t-shirts mere drapes over my torso.

Hopefully losing weight won’t be your major problem if you have Crohn’s – more likely, it’ll be keeping weight on and gaining back the weight you’ve lost. I find that during flares, when I don’t want to eat a lot because my stomach is in bad shape, drinking high-calorie liquids like whole milk and pure grape juice (by pure, I mean No Sugar Added) helps because they’re easier to absorb and digest than food is.
Diet And Nutrition
I’m surprised with how little the medical world seems to think diet affects bowel disorders like Crohn’s disease. Quite frankly, it’s mind-boggling that doctors don’t see diet as one of the major factors that affects people who have this condition. It’s a digestive disease, for crying out loud!
I wholeheartedly endorse and practice the Specific Carbohydrate Diet as outlined in the book Breaking The Vicious Cycle by Elaine Gottschall. The diet is extremely strict, and eliminates tons of foods from your diet in order to clear up symptoms.
The simple fact about the SCD is that it works, but it is very rigorous and difficult to stick to without a lifestyle change. You have to be willing and committed, and in fact it wasn’t until I had spiraled down into the worst condition I’d ever been in that I decided to try it.
If you want to try the SCD, more power to you – I highly recommend it. But if you believe that diet does have more to do with how a Crohn’s patient feels than many doctors would like to admit, then just try this: don’t eat as much bread. Read the ingredient labels of foods you eat. If anything lists Corn Syrup, High Fructose Corn Syrup, or Sugar, don’t eat or drink it.

You’re likely to find that there are tons of things you never would’ve guessed have corn syrup and other processed sugars in them. These ingredients aren’t good for anybody, and they’re especially bad for Crohn’s patients who might have difficulty digesting these foods.
Whether you want to try this or not, it’s very important for a Crohn’s patient to get a healthy dose of vitamins, minerals, and other nutrients.
Flares And Remission
Crohn’s is a cyclic condition, meaning it goes through wave-like periods where it may get better or worse. Periods where the disease is at its worst are called flares or flare-ups, while periods where symptoms are minimal are called states of remission.
Since I’ve had Crohn’s, I can never truly say I have been in total remission. If experiencing the bowel habits of a normal person and having no symptoms of disease whatsoever is true remission, then I believe there’s no such thing.
I have, however, been in states where I had no pain, no bleeding, and no uncomfortable gas or cramping. But even in these situations I still had to use the bathroom more often than the normal person would.

So for me, a flare is when my symptoms are so bad they effect my ability to work and enjoy time with friends. A flare is when I don’t get out of bed – not because I don’t want to, but because I can’t.
Many times a period of remissive behavior in this disease requires several things to be in place – the ‘stars aligning,’ as it were. The stress levels in your life are low, the medicine(s) you’re taking are doing their job, and your body is reacting well to the food and drink you are consuming.
To arrange these vital components is a feat that requires some luck and some discipline. Certain things you can control and others you can’t, but everyone goes through stormy seas in their lifetime and everybody sees sunshine.
Dealing with your flares and getting through them makes times of remission that much more enjoyable, but the temptation becomes the “oh, I’m perfectly fine” mentality.
What I mean is that, as far as my personal struggle goes, the times when I’m feeling good are the times when I push myself further than I should go. I wear myself out and stretch myself thin so that I think sometimes I almost bring myself back into flare-ups.
I eat too much of things I know I shouldn’t. I stay up too late and miss out on sleep. I start dating multiple women and don’t commit myself to anything, in relationships or otherwise. Okay, so that last part might be something personal that has nothing to do with having Crohn’s, but you get the idea. Just take it easy; if you feel good, be happy that you feel good but don’t use that as an excuse to go crazy.
Pace yourself and take each day as it comes. Unless they develop a cure or you get miraculously healed, you have this thing for the long haul, so it’s like being married to it – you have to respect its wishes, too.
Visiting Your Doctor
Your doctor should be consulted before you make any moves that will affect your disease. Whether it’s in the medication you’re taking, any tests you’re scheduled to undergo, or other lifestyle alterations including a diet change, your GI doctor at least deserves to know your feelings on the matter, whether you decide to listen to everything he says or not.
I dislike going to the doctor as much as anybody – no, actually I hate it – but when you have Crohn’s you shouldn’t just go when you don’t feel well. Conditions inside your body can change pretty rapidly, and keeping track of them periodically with your doctor’s help can save you from a lot of trouble in the long run.
Take my story, for example. I decided to go on a Crohn’s-oriented diet, stop taking all my medication, and not visit the doctor for over a year. I felt great, and I didn’t think I needed medical advice anymore because I’d found something that worked.

When I suddenly started having abdominal pain that built up over the course of a couple weeks, I was bewildered. It finally got to the point where I couldn’t ignore it any longer, so I went to the doctor. He ordered a colonoscopy and found a stricture in my sigmoid colon so tightly closed that he couldn’t finish the procedure.
A couple of years and a colon resection surgery later, I’m now regretting every minute of my decision to throw modern medicine out the window. The diet I use definitely works, but staying on maintenance drugs balances out any slip-ups I might make and does all the more to keep my body in remission.
As a general rule of thumb, if six months have gone by and you’ve felt good enough that you haven’t scheduled a doctor’s appointment, do so now. If you’re in tip-top shape, checking in with the doctor will make you feel better about what you’re doing to combat your disease. If you aren’t, you’ll hopefully have caught any problems early enough to do something about them in the least invasive way possible.
Crohns Disease And Hospitalization
Battling Crohn’s disease sometimes might get to be too much for you to handle on your own. If you’ve had this condition for any stretch of time you’re probably used to the spasms of pain, discomfort in your abdomen, and feelings of nausea on an almost daily basis.
Knowing when something’s seriously wrong – a bowel obstruction, an infection such as diverticulitis, or even cancer – is important. So let this be your little cheat sheet of information for when to hold and when to fold, so to speak.
If you’ve never had to be hospitalized for a condition stemming from your Crohn’s, good on ya mate! That’s excellent, and I hope you never do. But there are times in life when we all have to bite the bullet and give in; realize we aren’t powerful enough to do everything by ourselves.
I’ve been to the hospital for Crohn’s-related garbage probably around half a dozen times. Most of these times were in the weeks and months leading up to my resection surgery, when I was too stubborn to give in and just let them do the operation.
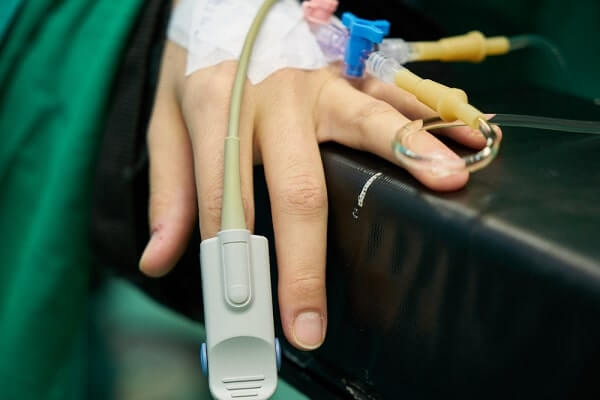
My typical hospital visit goes something like this.
Pain. More pain. It gets to be too much for me to ignore, and then it finally gets to be too much for me to handle. It’s such intense pain that I can barely keep myself from vomiting because it hurts so much.
I drive myself to the emergency room. Sign myself in. Plastic wristband. Wait. Wait some more. Triage. IV with a saline bag on a rolling pole. They shoot me up with some morphine for the pain, a little phenergan for the nausea.
I’m a light-weight, so they give me half a dose of each and I’m still out like a light. In Lala land. I wait some more, get taken into the ER. They put me on a bed and stick me into a room If the hospital’s busy, they put me in the hallway.
Wait. And some more waiting.
The first test they always run is the CT Scan with contrast. I’ve got a page about CT Scans and a page about contrast, check them out on the left navigational menu if you don’t know how these things work.
I drink a radioactive cocktail of ginger ale and contrast. Two big 12- or 16-ounce cups, with ice to keep it cold. The ginger ale’s just there to disguise the taste of the contrast, but I’m so out of from the morphine and phenergan they keep giving me I could be drinking liquid poo and not know it.
The contrast goes down easy; I’m used to it by now. It’s working its way through my system now. Wait for it.
They take me in for the CT. Hey, what do you know? A blockage! Something isn’t working right down there. You don’t say. It hurts doc, gimme more meds.
I get admitted and taken to a hospital room I’m sharing with what seems to always be some old guy.
Wait some more. Drift in and out. Eyes opening and closing, people coming into the room and talking at me. I nod to them, no matter what they say.
You have an intestinal obstruction. We need to put in an NG tube. A tube that goes through your nose into your stomach. Ever had one of those before?
I nod. Yeah. Unfortunately I have.
They do the deed. It hurts going down, feels awful, uncomfortable. They turn on the suction.
Fast forward twenty-four to seventy-two hours. I feel much better! I can’t wait to get out of this hellhole! What did I ever come here for in the first place? I’m perfectly fine…
Okay people, back to reality. My hospital dramatization is over. The fact is, with any kind of obstruction, rupturing, or hemorrhage, you need to get to the ER fast. If the pain hurts too much to sleep, like you literally can barely stand it, that’s a good indicator. Never just try to ignore it and hope it goes away.
At the same time, don’t jump at the first sign of trouble either. Give it some time to see if the pain stays there. If it stays or gets worse, you need to get on the road.
Stomas
I’m so scared of having to get a stoma one day I can’t even describe the fear that courses through my veins every time I think about it. It’s gut-wrenching when I consider the possibility.
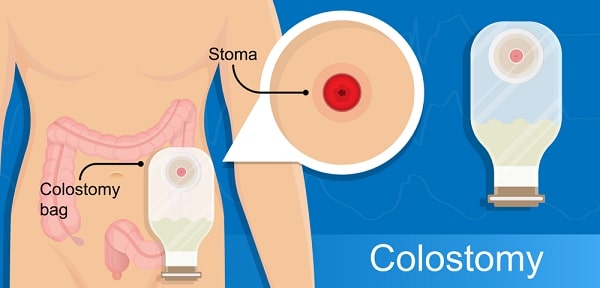
A stoma is an external outlet for your intestines. In other words, they re-route your digestive tract through surgical means so that it empties through a hole in your lower abdomen instead of through your rectum.
To catch the waste you produce, you have to wear what’s called a colostomy bag. It has a little nozzle that fits over the stoma pretty snugly, and you can attach it to the waistband of your pants.
I guess most of my fear comes from the fact that if I ever had to get a stoma, I wouldn’t be able to take my shirt off to go swimming or mess around with a girl without having some [awkward and disgusting] explaining to do.
Some people say that wearing a bag is freeing, because for someone with Crohn’s who’s always had to worry about their next bathroom visit, once you have a bag all that worrying is over. That’s probably the only upside of the whole deal.
The most common types of stomas resulting from Crohn’s disease are created during either an ileostomy or a colostomy surgery. In the former case, the ileum (the end of the small intestine) is re-routed, whereas with the latter the colon is used to create the stoma.
Nutrients And Crohn’s Disease
Because of the digestive system’s reduced efficiency in the Crohn’s patient, we tend to develop several imbalances in the amount of certain nutrients our bodies carry.
Many of these deficiencies have close cause-and-effect relationships with one another. Vitamin B12 deficiency, for example, is quite common in the Crohn’s patient and appears due to malabsorption and the body’s inability to harvest this and other important nutrients, such as iron, from the food we eat.
Bleeding caused by inflammation of the gastrointestinal tract leads to low levels of red blood cells, and because of a lack of vitamin B12 and iron, both of which assist in the production of new cells, these levels are not easily replenished.
When the body is unable to maintain a healthy rate of red blood cell production, anemia occurs and can become worse over time.
Deficiencies of B12 and iron are often treated with B12 injections and iron supplements, although iron in pill form may exacerbate intestinal inflammation and be counter-productive for achieving its goal.
The best way to combat nutrient deficiency is always to consume foods high in the nutrient in question, but in cases where the body is simply not absorbing enough of these important elements in the diet, nutritional supplements may become necessary for the Crohn’s patient.
Recipes For Crohn’s Disease
This page will eventually become a database of recipes for the Specific Carbohydrate Diet, a diet which has done wonders for me and many others with Crohn’s. I have tried and experimented with several dozen of my own recipes which I’m hoping to eventually be able to get the time to add here, so they may even warrant a completely new section of the site being made. For now, check out these great SCD Recipes, which has hundreds of healthy recipes posted already.