How To Stop Shoulder Pain

The shoulder is a non-weight bearing joint (in most cases unless you walk around on your hands doing handstands). Most painful conditions of the shoulder result from direct injury and disuse of the joint (over stressing the joint acutely or chronically). This monograph will focus on how to stop shoulder pain…the chronic variety.
ACUTE SHOULDER PAIN SHOULD BE IMMEDIATELY EVALUATED BY A QUALIFIED MEDICAL PRACTITIONER.
Chronic shoulder pain is defined as persistent pain that lasts longer than 6 months. Chronic shoulder pain is a common phenomena in certain sports, work environments, age groups, and disease conditions. In the year 2000, direct costs to treating shoulder dysfunction in the U.S. totaled 7 billion dollars.
The key to effective treatment of chronic shoulder pain is an accurate diagnosis. Once established, a focused and effective treatment regimen can be constructed that will relieve the pain, reduce recurrence, and restore normal function to the shoulder. Unlike other joint disorders, the shoulder does not respond well to complete immobilization.
Important Note
A THOROUGH HISTORY AND PHYSICAL BY A QUALIFIED MEDICAL PRACTITIONER IS ESSENTIAL FOR THE ACCURATE DIAGNOSIS OF CHRONIC SHOULDER PAIN. THIS MONOGRAPH IS INFORMATIONAL ONLY AND DOES NOT REPRESENT MEDICAL ADVICE.
Shoulder Anatomy and Physiology
The anatomy and physiology of the shoulder is one of the most complex organizational structures of the skeleton of the human body. The range of motion of the shoulder is the largest of any joint in the human body. Because of this it is particularly vulnerable to injury.
Click edit buttThe shoulder is mostly a “ball in socket” joint (the Gleno-humeral joint) which allows for the large range of motion. It also has the Acromio-clavicular joint (the acromion of the scapula attaches to the “collar bone” or clavicle).on to change this text. Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
The Gleno-humeral joint is where the ball of the humerus (the upper arm bone) inserts into the cup of the Glenoid fossa (attached to the scapula). It is a synovial joint (meaning it has synovial cartilage on the ball of the humerus) and synovial cartilage on the surface of the Glenoid fossa or cup.
This type of cartilage has a very low frictional coefficient which allows for smooth movement with a minimum of heat build-up. The construction of the joint is similar from person to person.
Whereas, the Acromio-clavicular joint (AC joint) can vary from person to person. In the usual arrangement the ends of the clavicle and acromion have synovial cartilage with a fibrous pad between them. However, anatomical studies have shown that the actual structure of the joint varies widely.

It functions to stabilize the shoulder similar to the “tie rod” on an automobile front wheel. The clavicle rotates along its long axis when the arm is raised overhead. The motion of the clavicle with the scapula is in a “tomahawk” fashion with the clavicle the handle and the scapula the blade (hence the colloquialism “shoulder blade” for the scapula).
Some people have only fibrocartilage between the acromion and clavicle. Other people have have synovial cartilage, a fibrous disc between, and tight ligamentous banding. The unique configuration of each person’s AC joint effects the likelihood of injury.
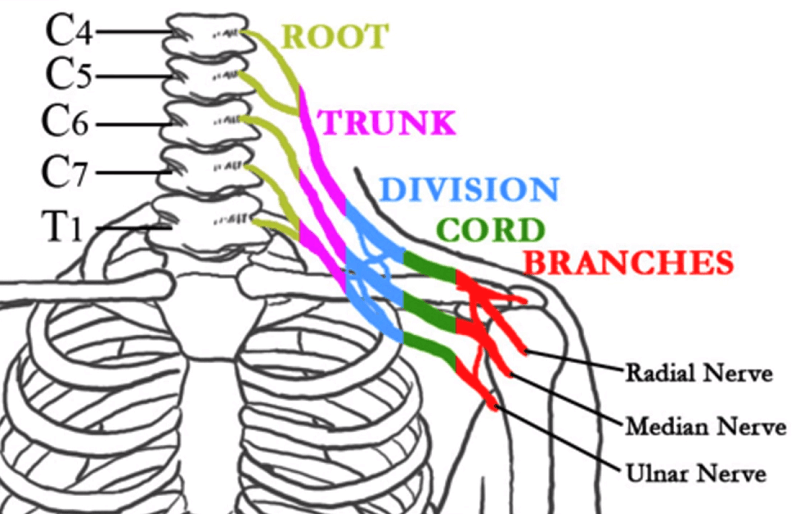
There is a rich neural network that is involved with the shoulder called the Brachial Plexus. It is a grouping of the nerve trunks that come out of the spinal cord and connect in the soft tissue near the shoulder. Emanating from the Brachial Plexus are the major nerves that descend into the arm.
The Brachial Plexus rearranges the contribution that each spinal nerve makes with the nerves going into the arm. Though the arrangement follows a certain order, variability occurs here also. Because of the close proximity to the shoulder, these important nerves are easily injured when the shoulder sustains an injury.
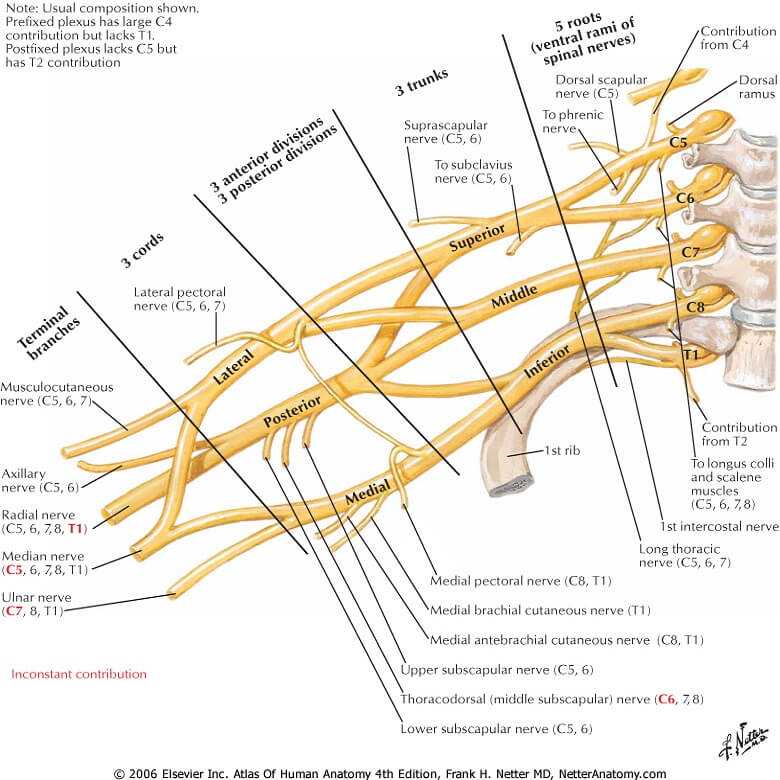
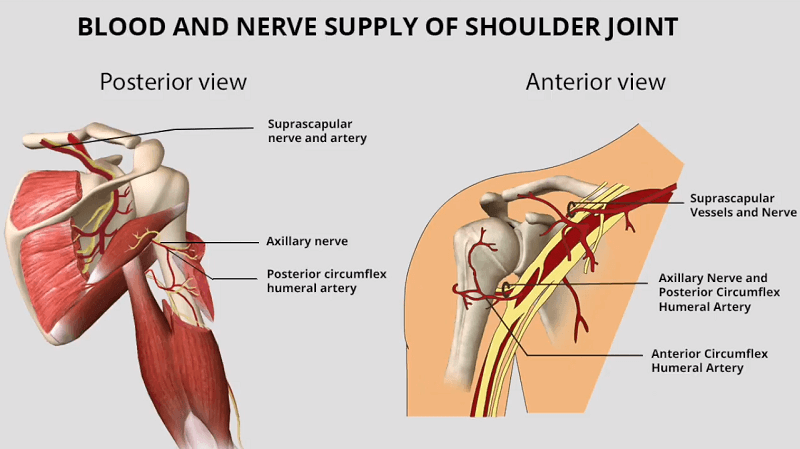
In addition to the nerves, there are large arteries, veins, and lymphatics (a third vascular network that carries a “milky” colored fluid rich in white cells, proteins, and lipids) that traverse the shoulder region en route to the arm. They too are subject to injury when the shoulder is injured
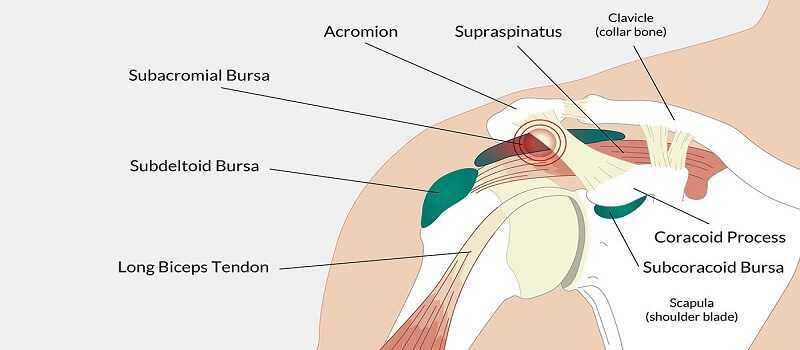
The complex movements of the shoulder require lubricating structures that lower the frictional coefficients of the involved tendons, muscles, and bones of the shoulder. They are called Bursa. A Bursa is a lubricating “pillow” of connective tissue that pads the surfaces of bone edges.
All in all an injury to the shoulder can severely effect the function of the arm and hand as well. A shoulder injury can effect ligaments, tendons, cartilage, bones, muscles, nerves, arteries, veins, and lymphatics that are in close proximity with the shoulder.
At least 9 structures in toto can be effected with a shoulder injury making sorting out the exact cause for shoulder pain challenging. It is rare that only one of these structures are effected with an injury.
Therefore, the cause of shoulder pain usually involves multiple structures. Sorting out the mechanism(s) for shoulder pain is essential for effective treatment.
IF YOU HAVE READ MY OTHER POSTS ON CHRONIC PAIN SYNDROMES YOU WILL HAVE NOTICED THAT IDENTIFYING THE CORRECT MECHANISM FOR THE PAIN IS ESSENTIAL FOR EFFECTIVE TREATMENT. IN MY PREVIOUS PRACTICE OF CHRONIC PAIN MANAGEMENT I FOUND PRACTITIONERS FREQUENTLY ASSIGNED THE WRONG MECHANISM FOR A PERSON’S SHOULDER PAIN. THIS WAS THE MOST COMMON CAUSE FOR TREATMENT FAILURES.
The 7 Best Treatments For Chronic Pain
Causes of Chronic Shoulder Pain
1) Tendonitis:
Any process that causes inflammation of the tendons of the shoulder (the structures that attach bones to muscles) can cause tendonitis. The pain of tendonitis is worsened with contraction of the muscle whose tendon is inflammed. If you have shoulder pain that is worsened when you move your shoulder by will (and less pain with no willful movement) you are more likely to have a tendonitis.
Passive movement of the shoulder (such as by an examiner without willful movement by the patient) will result in less pain than with willful movement. The most common tendon of the shoulder for this malady is the Supraspinatous tendon. It is located on the top of the shoulder and connects to the top of the humerus. There is often point tenderness there also.
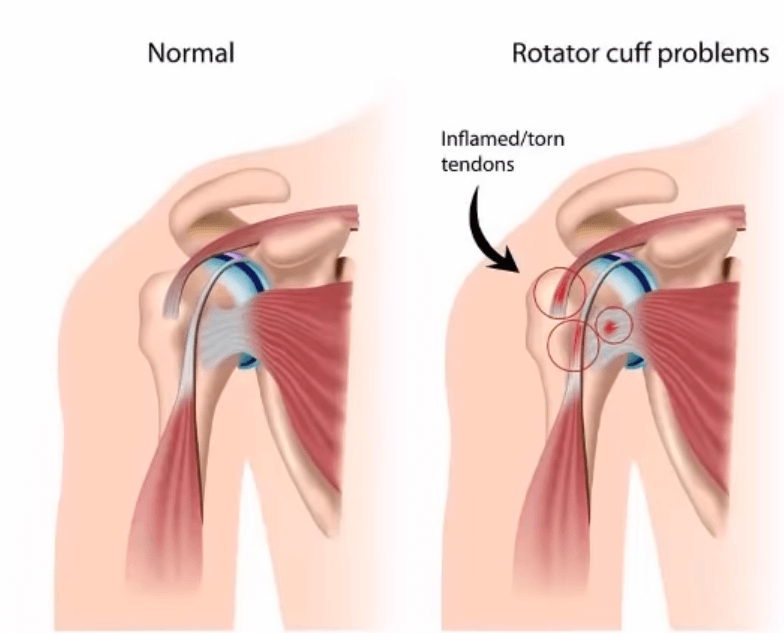
The Supraspinatous tendon is a very small tendon that is easily injured. It accounts for the movement of the arm away from the body laterally from shoulder height to overhead (about 90 degrees). People with this condition will have difficulty and pain extending their arms above shoulder level.
2) Ligamentitis:
Ligaments attach bones to bones. When they are inflammed the pain is usually constant. A stretch applied to the ligaments will increase the pain if they are inflammed. This malady usually occurs when the ligaments have been forcibly stretched (such as in contact sports) or in activities that apply a tractional force to the ligaments of the shoulder.
3) Myofasciitis:
This condition is an inflammation of muscle. This can occur with overuse, improper use, or direct trauma to a muscle. It can also occur in certain autoimmune conditions (such as Dermatomyositis) without any history of trauma. Muscle pain is usually increased with willful movement and often accompanied with visible swelling. Pressing upon the muscle will usually increase pain (as well as contracting the muscle).
4) Arthritis:
Arthritis is a condition that involves damage to the joint surface cartilage. The most common cause in the shoulder is Degenerative Joint Disease where the cartilage “wears away” and becomes pitted. This is usually due to extreme forces being repeatedly applied to the joint surface over time. It is not a rapid or acute process.
Occupations that use tools that vibrate the shoulder are prone to this condition. Heavy weight lifters who specialize in the Bench Press are also susceptible to this type of shoulder arthritis.
The pain of this type of arthritis is worse with movement (active or passive). When the joint is at rest the pain is usually less. An examiner passively moving the shoulder of the patient will result in as much pain as when the person moves the shoulder themselves (or nearly so).
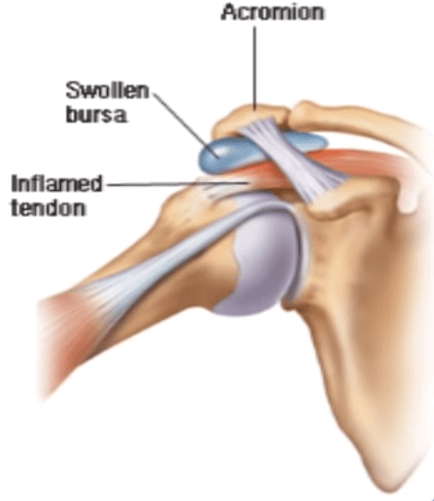
5) Bursitis:
Remember those lubricating “pillows” I spoke about? They can become inflammed for the same reasons as a person would develop any of the conditions I have previously mentioned (direct trauma, stretching, autoimmune diseases, etc.).
The pain of bursitis can occur with active or passive motion. However, the most pain is evoked with direct pressure applied to the bursa. In many cases swelling can also be observed of the skin area that the bursa resides under.
6) Neuritis:
This occurs when a nerve has been irritated. Nerve injury of the shoulder usually occurs when the shoulder has been dislocated (the nerves are stretched). Nerve pain is fairly characteristic.
Nerve pain is usually manifested as a burning type of pain (very distinctive from the other pains experienced with the other shoulder conditions). The pain is usually continuous and is made worse with movement and direct pressure.
7) Capsulitis:
The shoulder has a dense envelope of tissue that surrounds the Gleno-humeral joint that is called the capsule. It is akin to “saran wrap” around the entire joint structure. This structure can be effected for the same reasons as mentioned previously.
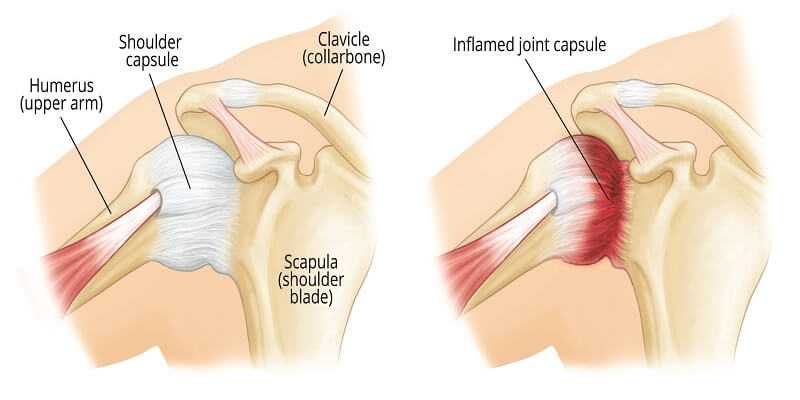
The pain is usually made worse with motion (active or passive) and is less at rest. Squeezing the shoulder joint may increase the pain. There is usually no visible swelling.
AS YOU CAN SEE THE CAUSES OF SHOULDER PAIN HAVE SIMILAR SYMPTOMS AND FINDINGS ON EXAMINATION. THIS MEANS THAT THE PROPER DIAGNOSIS OF CHRONIC SHOULDER PAIN WILL REQUIRE MORE THAN A THOROUGH HISTORY AND PHYSICAL. DIAGNOSTIC TESTING IS ALMOST ALWAYS REQUIRED TO BE ABLE TO ELUCIDATE THE CAUSE(S) FOR CHRONIC SHOULDER PAIN.
Chronic Shoulder Pain Diagnosis
As I remind all my readers, every pain syndrome requires a thorough history and physical to begin the diagnostic workup. However, in the case of chronic shoulder pain, that will not be enough. You will need to consider the following diagnostic studies:
Shoulder X-Rays:
This is the first of the diagnostic studies that must be performed for chronic shoulder pain. Indeed, plain x-rays only disclose bone abnormalities. The other structures of the shoulder are not visualized with this very old but helpful study.
MRI:
This is the most useful of all non-invasive studies for the shoulder. An MRI will disclose bone and soft tissue of the shoulder. Nearly all structures are visualized with this type of study of the shoulder.
However, even an MRI of the shoulder has limitations. Most MRIs are taken with the patient at rest. Some shoulder conditions are provoked with movement (such as a shoulder subluxation or hypermobility). In those cases a diagnostic study that can look at the shoulder while it is moving may be necessary (such as weighted x-rays or cineradiography-motion picture x-ray).
Arthroscopy:
This is a surgical diagnostic procedure (it can be therapeutic too) that allows an Orthopedic Surgeon to actually look inside the shoulder joint with a small scope. It is usually done under anesthesia and yields a direct visualization of many of the structures of the shoulder.
Arthroscopy has its’ limitations too. Some of the structures of the shoulder cannot be visualized with a scope (such as neuritis). Furthermore, the skill of the surgeon is very proportional to the value of the study. Do you know what they call the Doctor that graduates at the bottom of his class…Doctor?
There are other diagnostic procedures that can be performed but they are beyond the scope of this introductory monograph on chronic shoulder pain.
Treatment for Chronic Shoulder Pain
The following therapies have been shown to offer relief:
- Therapeutic Exercises
The best exercise for the shoulder is light weight circumduction. Essentially by taking 1 0r 2 cans of soup in a sock, bend at the waist and dangle the arm of the affected shoulder. Grasping the sock with the 2 cans of soup make small circles with the arm rotating at the shoulder. Proceed to make larger and larger circles then smaller and smaller. Repeat this cycle for 10 minutes 4 times a day.
- Acupuncture (click here to see my article on this topic)
- Shoulder Manipulation (click here to see my article on this topic)
- TENS Therapy (click her to see my article on this topic)
- Cool Laser Therapy
- Cold/Hot packs
Using either hot packs or cold packs, wrap the pack to the shoulder for 20 minutes and repeat this 4-6 times per day. Alternatively, a pack of frozen peas with do following the above instructions.
- Massage Therapy
- Water Exercise
The best way to perform these exercises is in a water therapy class (such as is given at the YMCA). Notify your instructor of your shoulder problem so that you can adjust your activity. The best type of pool for this is one that is on the warm side (90 degrees or higher water temperature).
- Trigger point Injections
These are injections that can be performed in an office setting. The practitioner will inject a local anesthetic agent with an anti-inflammatory agent mixed in. The injection is given into the muscle around the shoulder where the tenderness exists as small, discrete areas called “trigger points”.
- Bio-electric Therapy
- Motrin (click here to see my article on this topic)
- Tylenol (click here to see my article on this topic)
- Cymbalta (click here to see my article on this topic)
- Lyrica (click here to see my article on this topic)
- Australian Dream
- Narcotic Medications
- Natural Supplements (click here to see my article on this topic)
- Ultrasound therapy
Many General Practitioners have small ultrasound units in their office. The sound waves vibrate the deep tissues of the shoulder increasing blood flow, increasing healing, and decreasing inflammation.
- Biofeedback (click here to see my article on this topic)
- Cognitive Behavioral Therapy (click here to see my article on this topic)
- Magnesium Supplementation (click here to see my article on this topic)
- Turmeric Supplementation (click here to see my article on this topic)
- Aromatherapy (click here to see my article on this topic)
- Cervical Traction
- Shoulder Injections
When having a shoulder injection the practitioner will use the same mixture as is used in trigger point injections. However, the mixture will be injected directly into the shoulder joint under sterile conditions.
- Shoulder Arthroscopic Surgery
- Shoulder Micro-incision Surgery
- Open Shoulder Surgery
- Shoulder Joint Replacement Surgery
THE ABOVE LISTING IS NOT ALL THE POSSIBLE TREATMENTS FOR CHRONIC SHOULDER PAIN. THERE ARE MANY OTHER TYPES OF THERAPIES. THE MOST IMPORTANT CONSIDERATION IS TO NOT GIVE UP SEEKING RELIEF. THERE WILL BE A THERAPY OR GROUP OF THERAPIES THAT WILL WORK FOR YOU.
Final Comments on Chronic Shoulder Pain
I have discussed the foibles of treating chronic shoulder pain. As you can see there are many overlapping syndromes that will require an accurate diagnosis and multiple therapies.
The issue is that much of this therapy can be done by yourself. It is only a matter of you working through the different therapies until you find the combination that works for you.
I hope you have found this monograph helpful. If you have any questions or comments please leave it below. I would love to hear from you.
Wishing you joy and healing.
Facebook
Google+
Twitter
Pinterest
Reddit
StumbleUpon